In a perfect world, after the extraction of a tooth, there would be complete preservation and restoration of the original ridge volume via the natural process of tissue modeling, which is ideal for future implant placement. Commonly, and unfortunately, this is not the case. Regardless of whether tooth removal is atraumatic or not, healing of the extraction socket can be expected to result in significant osseous deformity; without further treatment, socket modeling can lead to ridge dimensional changes resulting in vertical bone loss of 1.5 to 2 mm, and horizontal ridge width loss of 40% to 50% over a six to twelve months healing period 1, with the dimensional changes primarily occurring in the first three months. We are aware that such ridge reductions can result in a residual ridge anatomy that decreases aesthetics, compromises the ideal localization of an implant or precludes placement altogether without the aid of adjunctive guided bone regeneration procedures. It is imperative that socket preservation–or more accurately–ridge preservation, be considered and excavated.
Commonly, grafting is a knee-jerk panacea that compromises both patient time and monetary resources. Whether a socket graft is required or not depends on a number of factors. Factors include (a) labial/buccal plate thickness, (b) smile line, (c) anterior or posterior location, and (d) pre-extraction bucco-lingual ridge width. As responsible surgeons we must weigh these factors to accurately formulate a socket-grafting algorithm that dictates grafting on a case-by-case basis, and not just a technique we use in a vacuum. Traditionally, assuming a socket graft was necessary, the use of ridge preservation techniques at the time of extraction required intact socket walls with at most only minor fenestrations or dehiscences (Case 1: Figs. 1-10). Sockets that were more greatly compromised were left to heal until soft tissue closure of the socket entrance was achieved six to eight weeks later (Case 2: Figs. 11-21). The idea behind this traditional method was that without intact socket walls, a bone graft procedure required employing the four principles of guided bone regeneration 2: (1) exclusion of epithelium and connective tissue, (2) space maintenance, (3) stability of the fibrin clot, and (4) primary wound closure. It was attainment of the fourth principle–primary closure–that dictated the delay in bone grafting until soft tissue had grown over the socket entrance. Of course, closure could be achieved at time of extraction by coronally advancing the labial/buccal tissue but this was not an aesthetic solution because it resulted in the coronal re-positioning of the muco-gingival junction, and necessitated an additional surgical procedure to reset the junction to its original location.
Case 1
Figure 1 Figure 2
#11 presents with vertical root failure. Detection of labial plate dehiscence.
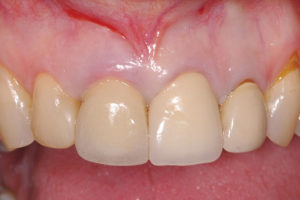

Figure 3 Figure 4
Visual of dehiscence. Resorbable membrane placed in socket.


Figure 5 Figure 6
Membrane folded over bone graft. One-week post-op.


Figure 7 Figure 8
Four-months later ready for implant. Maintenance of papilla height.


Figure 9
Implant placement with thick labial plate.

Figure 10
Final restoration by referring dentist.

Figure 11 Figure 12
Pre-extraction of #11. Loss of labial plate.

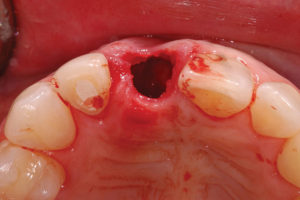
Figure 13
Preservation of labial contour with collagen plugs.

Figure 14
Soft tissue closure after six weeks.

Figure 15 Figure 16
Labial plate loss. Labial plate fenestration.


Figure 17
Ti-reinforced membrane tacked over graft.

Figure 18
Adequate ridge height of mature graft.

Figure 19
Adequate B-L ridge width for ideal implant placement.

Figure 20
Implant has been placed and the soft tissue sculpted with temporary crown for the restoring dentist.

Figure 21
Implant uncovering.

Recently I have been revisiting my rationale for immediate versus delayed ridge preservation. By examining the technique I use to preserve ridges and how that method relates to normal socket healing physiology, I have developed (caveat: perhaps other periodontists have considered similar ideas) approaches for more complex procedures that would allow for immediate grafting – even immediate implant placement, notwithstanding significant compromise in the integrity of the labial/buccal cortical plate.
The common technique for socket grafting involves the placement of a bone graft material, followed by closure of the socket entrance by a barrier, such as a collagen plug, resorbable/non-resorbable membrane, or autogenous/allograft soft tissue. The key for me was the realization that the graft does not maintain the integrity of the labial plate; the physiology of healing determined the fate of the labial plate and was related to extraction trauma, pre-existing damage, and most importantly, to the thickness of the labial plate as it related to cortical and medullary bone presence. In fact, it has been shown that even with immediate socket grafting in an intact socket we should expect 1.5 mm of horizontal and vertical ridge resorption.3,4 It follows from this that whether or not the labial plate is present should not dictate the timing (delayed or immediate) of the ridge graft. It also follows that since the continued integrity of the labial plate is not guaranteed, even in a completely intact socket, then primary closure (which is not a goal in these simple cases) is not critical in extraction socket cases. Without the pre-conditions of primary closure or the presence of a labial cortical plate, I can engage in immediate ridge preservation – even in the most compromised cases.
The following case study or series of images illustrates the progression of my thinking and the success achieved thus far with these more advanced socket-grafting techniques. (Case 3: Figs. 22-31) shows the use of a ti-reinforced membrane for space maintenance and soft-tissue exclusion. Stability of the fibrin clot is achieved by affixing the membrane with titanium tacks. This achieves three of the four principles of guided bone regeneration. Further, because the fourth principle–primary closure–is no longer a pre-requisite, I may be confident that this procedure will be successful, because it is based on a sound biological reasoning.
Figure 22
Large fenestration and very thin labial plate.

Figure 23
Ti-reinforced membrane for space maintenance.

Figure 24
Internal Mattress suturing over socket at papilla.

Figure 25
Socket entrance closed with collagen plug.

Figure 26
Two-week post-op.

Figure 27
Preservation of B-L ridge width after six months.

Figure 28
Adequate ridge for implant placement after six months.

Figure 29
Implant uncovering.
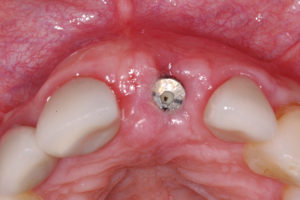
Figure 30 Figure 31
Final restoration. Final restoration.
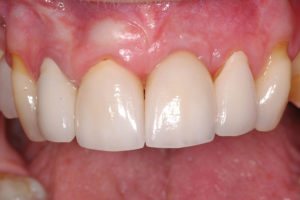

The next series of figures (Case 4: Figs. 32-43) show how this concept can be applied to a more greatly compromised labial plate. In this case, a resorbable membrane was used for comparison purposes; a ti-reinforced membrane would provide better space maintenance, but also requires removal, and thus a more complicated implant placement surgery (since the membrane would have to be removed). This case study treatment is not complete but as with the previous case, the biological reasoning is sound, and I expect the result will be an adequate ridge for implant placement.
Figure 32
Previous root end surgery and apical radioleucency.

Figure 33 Figure 34
Initial sulcular incision. Preparing to access osseous defects.


Figure 35
Loss of labial plate, large fenestration and thin remaining labial plate.

Figure 36
Resorbable membrane secured with tack.

Figure 37
Bone graft with membrane for soft tissue exclusion.

Figure 38
Socket entrance closed with collagen plug and internal mattress sutures at papilla.

Figure 39
Vertical incisions closed only with internal mattress sutures.

Figure 40
Two-week post-op.

Figure 41
Incision lines can hardly be seen due to mattress sutures.

Figure 42 Figure 43
Six-week post-op. Six-week post-op.


Based on the foregoing discussion, it is important to consider how we are trained, and how we approach treatment planning. As general dentists we are trained to think like engineers. By contrast, periodontal surgery, and its conjunctive techniques, is not mechanically based; rather, they are based on an understanding of human biology – the mechanical aspects of our work serve only to take advantage of nature to achieve our ends. OH
Dr. Raman Kohli is certified as a Periodontal surgeon and is a diplomat of both the Canadian and American Boards of Periodontology. Dr. Kohli received his Doctor of Dental Surgery in 1990 from the University of Toronto. He practiced dentistry for thirteen years before switching gears to attend the renowned Boston University Goldman School of Dental Medicine, where he received his Masters in Oral Biology and Periodontology. During his studies, Boston University awarded Dr. Kohli the recognition of the top graduating resident in Periodontology. As an alumni of BU, he visits the Goldman School to lecture periodontal residents. Dr. Kohli has also been a guest lecturer for the specialty programs at the Universities of British Columbia, Manitoba and Toronto for the purpose of delivering his suturing program.
Oral Health welcomes this original article.
References:
1. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 2003; 23(4):313–23.
2. Wang HL, Boyapati L. “PASS” principles for predictable bone regeneration. Implant Dent 2006; 15(1):8-17.
3. Horváth A, Mardas N, Mezzomo LA, Needleman I, Donos N. Alveolar ridge preservation: A systematic review. Clin Oral Investig. 2013 Mar;17(2):341-63.









