Introduction:
December 31, 2019: Chinese medical authorities announced a cluster of pneumonia cases of unknown etiology.
January 9, 2020: The Chinese Center for Disease Control reported that a novel coronavirus was the causative agent.
February 10, 2020: The virus and the disease were named SARS-CoV-2 and COVID-19.
Since its origin, the disease has spread globally, a dangerous pandemic. The novel (new) nature of the virus means no “herd immunity” and virtually universal susceptibility. Symptomatic patients are the main means of transmission, but asymptomatic infected patients can also communicate the disease. It is believed that transmission occurs mainly via respiratory droplets and contact transmission. Additionally, there may be a risk of fecal-oral transmission. These realities have changed the way that we all live and work. Social distancing has become the norm, and major metropolitan centers are virtually empty.
Dentists work at the oral end of the airway which is the SARS-CoV-2 path of entry to the human body. The virus enters host cells via ACE2 (angiotensin-converting enzyme 2) receptors which are abundant in respiratory system cells. The virus can be found in the oral cavity, saliva and conjunctival secretions. Dentists, otolaryngologists and ophthalmologists do most of their work in these danger zones.
Transmission of SARS-CoV-2 in the dental clinic:
SARS-CoV-2 can be passed directly from person to person by respiratory droplets, and/or transmitted through contact with fomites. Dental clinics invariably carry the risk of COVID-19 infection due to routine procedures that involve face to face patient communication and frequent exposure to body fluids.
Airborne spread: Handpieces and ultrasonic scalers generate aerosols and droplets that may be contaminated. Aerosolized virus particles may remain suspended for up to an hour.
Contaminated surface spread: SARS-CoV-2 may persist on hard surfaces (metal, glass or plastic) in the operatory are potential sources of virus transmission. After treatment, the operatory must be thoroughly disinfected according to current protocols.
PPE: All dental procedures must be performed with personal protection equipment that meets the currently established protocols.
The COVID-19 pandemic poses an existential threat to the way we practice dentistry. As this hazard may last for some time, it is essential to find treatment modalities for patients who need urgent assistance. Protocols that delay the spread of dental disease with minimal handpiece use are a crucial focus. The objective is to save and stabilize teeth until all conventional treatment options are safe.
ART: Atraumatic Restorative Technique (modified for the COVID-19 pandemic): or ITR (Interim Therapeutic Restoration)
These two techniques are very similar; in fact, they are the same. Dentists require protocols that allow conservative treatment of dental disease while minimizing viral transmission. ART is a strategy for caries management that does not utilize a handpiece, an ideal strategy for pandemic dental treatment. In fact, the term ITR should be discontinued as it is redundant and confusing.
ART Goals
- Remove diseased tooth structure without a dental handpiece
- Preserve tooth structure
- Save teeth
- Reduce the chance of odontogenic infection
- Manage odontogenic pain (particularly reversible pulpitis)
- During the COVID-19 pandemic, buy time for teeth that can be saved
ART Disadvantages
- Glass ionomers and IRM have low wear resistance
- These materials have a typical longevity of 2 years.
Overcoming disadvantages of ART (during COVID-19 pandemic)
- Use local anesthetic
- After adequate caries excavation, use a restorative material that seals effectively and has wear resistance.
- Biodentine (Septodont Canada, Cambridge, ON.) is a tricalcium silicate material designed as a permanent dentin substitute with a bactericidal pH of 12 that arrests active carious lesions.
Biodentine is biocompatible and not cytotoxic to pulpal cells. It is bioactive, creating dentinal bridges over pulp exposures and precipitates into dentinal tubules during the setting reaction, creating restoration “tags” that seal the margins and create retention. Biodentine can be the ideal restorative to overcome the disadvantages of ART.
Silver Diamine Fluoride:
- Indications: Interim treatment for patients who are not eligible for traditional restorative treatments (uncooperative, special needs, post-radiation with osteoradionecrosis, delayed treatment, etc.)
- Contraindications:
a. Silver allergy
b. Pulpally involved or symptomatic teeth
c. Stomatitis or ulcerative gingival conditions - Silver: Antibacterial
- Fluoride: Fluoroapatite
- Can be effective in arresting active carious lesions
- Causes dark staining in caries arrested areas.
Professional judgement is paramount; lesions must be treated when necessary, with minimally invasive dental techniques. Significantly cavitated lesions, depending on whether the teeth are symptomatic or asymptomatic, must be saved when possible. ART is most successful with appropriate case selection. Cavitated carious lesions with reversible pulpitis have the best prognosis when treated with ART.
Modified ART strategy for COVID-19 pandemic treatment without a handpiece:
1. Emergency patient contact by phone or email.
2. Essential triage questions:
- Do you have uncontrolled bleeding from your mouth?
- Do you have swelling in your mouth, upper or lower jaw or under your tongue?
- Do you have difficulty breathing from the swelling in your mouth, neck or jaw?
- Are you unable to eat or drink due to oral pain to the point where you are ill and physically weak?
- Do you have new difficulty opening your mouth due to pain and swelling?
- If no to the above, what is your chief complaint? Dental pain from a cavity
3. If the patient should be seen, further COVID-19 screening questions:
- Have you been in contact with someone who is confirmed or suspected to have COVID-19 In the past month?
- Do you have any of the following symptoms?
o Fever or chills?
o Dry cough?
o Shortness of breath?
o Rash? - Have you traveled domestically or internationally in the last month?
o If yes, Where? When?
4. If the patient has answered yes to any screening questions, they should be referred to their primary care MD. If answers are all “no”, and the dentist is prepared to see the patient (appropriate PPE and operatory protocols), the appointment is set.
5. Review the screening questions upon arrival; if all answers are “no”, the patient is seated in the operatory which should be completely set up to avoid the PPE waste of moving in and out.
6. Conduct a problem-focused examination (including necessary radiographs). (Fig. 1) If the tooth is restorable (cavitated lesion with reversible pulpitis), an ART can be considered.
Fig. 1
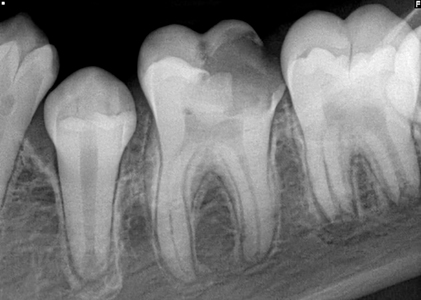
7. Have the patient rinse with an anti-viral mouthwash to kill the virus/reduce the oral viral load.
8. Administer local anesthesia as necessary.
9. Place rubber dam for isolation.
10. If direct access to the lesion exist, excavate the caries with surgical curettes or spoon excavators. Remove as much of the lesion as is clinically appropriate. (Fig. 2) Position the restorative matrix.
Fig. 2

11. Mix Biodentine according to manufacturer’s instruction (Fig. 3) and bulk fill the cavity. The initial set time will be 9-12 minutes, adequate working time. Leave the restoration out of the occlusion to avoid occlusal adjustment with a handpiece.
Fig. 3

12. The completely set Biodentine exhibits the hardness of natural dentin and hydroxyapatite deposition at the restorative interface seals the margins. These eliminate some ART shortcomings.
13. Remove the rubber dam and verify occlusion. (Fig. 4)
Fig. 4
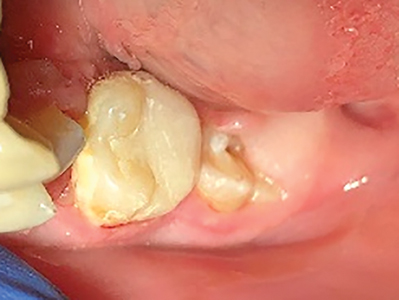
14. Dismiss the patient with chewing, homecare and maintenance instructions.
15. Set up a phone or email follow-up.
Oral Health welcomes this original article.
References
- Coronavirus Disease 2019 (COVID-19): Emerging and Future Challenges for Dental and Oral Medicine L. Meng, F. Hua, Z. BianFirst Published March 12, 2020 Research Article https://doi.org/10.1177/0022034520914246
- E. Kim et al.,Microneedle array delivered recombinant coronavirus vaccines: Immugenicity and rapid translational development, EBioMedicine (2020) http://doi.org/10.1016/j.ebiom.2020.102743
- Xian, P et al., Transmission routes of 2019-nCoV and controls in dental practice. International Journal of Oral Science. http://doi.org/10.1038/s41368-020-0075-9
- Frencken JE, et al., Atraumatic Restorative Treatment (ART): rationale, technique and development. J Public Health Dent. 1996;56: 135-40.
- Frencken JE, Atraumatic restorative treatment and minimal intervention dentistry. BDJ 2017 223; (3) August 183-189
- Poorandokht Refaei, Maryam Zare Jahromi, and Abbas ali Khademi Moughan. Dent Res J (Isfahan). 2020 Jan-Feb; 17(1): 66–72., Comparison of the microleakage of mineral trioxide aggregate, calcium-enriched mixture cement, and Biodentine orthograde apical plug. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7001563/
- Afnan M. Saber 1 , Azza A. El-Housseiny 1,2 and Najlaa M. Alamoudi 1,* Atraumatic Restorative Treatment and Interim Therapeutic Restoration: A Review of the Literature Dent. J. 2019, 7, 28; http://doi:10.3390/dj7010028
About the Author
 Mark Roettger is Chief of Dentistry at University of Minnesota Medical Center, and Associate Professor at the University of Minnesota. He is Director of the University of Minnesota Physicians Dental Clinic University of Minnesota Medical Center; Transplant Clearance Clinic, Head and Neck Cancer Clinic; Clinical research; Dental management of head and neck cancer patients. Medical Director for the Dental clinic within the M Health Clinics and Surgery Center (CSC) designed to integrate dentistry and medicine within a clinical setting. Dr. Roettger is the author of “Modern Sports Dentistry”, published by Springer Nature.
Mark Roettger is Chief of Dentistry at University of Minnesota Medical Center, and Associate Professor at the University of Minnesota. He is Director of the University of Minnesota Physicians Dental Clinic University of Minnesota Medical Center; Transplant Clearance Clinic, Head and Neck Cancer Clinic; Clinical research; Dental management of head and neck cancer patients. Medical Director for the Dental clinic within the M Health Clinics and Surgery Center (CSC) designed to integrate dentistry and medicine within a clinical setting. Dr. Roettger is the author of “Modern Sports Dentistry”, published by Springer Nature.
To see more articles from the July/August 2020 issue, please click here!












