Dental clinicians are primary oral care providers, focused on optimal health outcomes for their patients. The progression of oral disease is multifactorial and can present a downward spiral if left unchecked. This is not inevitable, however, if there is a conscious effort to proactively intervene, to slow or completely interrupt the process. All dental procedures must be performed with this in mind – through the practice of Proactive Intervention Dentistry.
Bioactive dental materials are the ideal candidates for the restoration of form and function of dental patients’ carious and/or damaged dentition using a proactive approach. Bioactivity is defined as having “any effect on, interaction with, or response from living tissue”. Bioactive materials are “active”, not “passive” participants in the restorative process.1 They provide proactive benefits for the patient that continue after they are placed, without any additional intervention on the part of the clinician.
For a material to be tried and successfully incorporated into a dentist’s practice, it must exhibit superior physical and esthetic properties and be user-friendly. Dental manufacturers work hard, creating these products. Some products have superior properties, or are user-friendly, while the best have both attributes. Effective, successful, bioactive materials must provide the same superior properties, be user-friendly and of course, add the healing aspect of bioactivity.
Bioactivity in dental materials can be displayed by:1
- The ability to remineralize and strengthen tooth structure through fluoride release and/or release of other minerals
- The formation of an apatite-like layer on their surfaces when immersed in body fluids
- The regeneration of live tissue to promote vitality in the restored tooth
This article focuses on bioactive materials that heal by remineralizing to strengthen remaining tooth structure, and other bioactive materials that regenerate live tissue to heal the pulp and keep the tooth alive. These are everyday restorative materials that are essential to the general dental practice.
Remineralization: The natural repair process for non-cavitated lesions
Oral saliva is a miraculous solution that bathes the dentition with minerals that keep teeth strong and resistant to acid challenges. There is a constant state of demineralization and remineralization occurring which fluctuates depending on food consumption, oral hygiene, oral pH, and other factors unique to each individual patient. Remineralization is the natural repair process for tooth structure before it becomes cavitated. When remineralization outperforms demineralization, the tooth retains its mineral content and integrity. When this balance is disrupted, demineralization prevails, minerals are lost, and with time, cavitation occurs.
Oral hygiene products and techniques may improve the initial situation, while today’s restorative materials are able to bioactively tip the balance to encourage remineralization, and to accomplish this in vulnerable, previously damaged areas, which now require restoration or repair.
Everyday Bioactive Clinical Dentistry
As mentioned, the ideal everyday “go-to” restorative material must exhibit superior physical and esthetic properties and easy handling. The addition of bioactive properties should in no way diminish these attributes.
Giomers (Shofu Dental, San Marcos, CA) were developed to do just that – be the everyday “go-to” bioactive restorative solution. This is the family of Beautifil and Beautifil Flow Plus materials.
Giomer materials have been clinically evaluated in a series of long-term clinical trials. A study of Beautifil restorations placed at the University of Florida found no post-operative sensitivity, no secondary decay or marginal deterioration, 100% retention and maintenance of anatomic form with 95% of lustre retained after 8 years.2 A thirteen-year recall study demonstrated 95% of the restorations with no secondary decay.3
What about bioactivity? Studies show dentin remineralization occurs at the preparation surface adjacent to the giomer.4 Giomers are based on a proprietary filler particle that contains ions that have distinct biological effects. These are: fluoride (remineralization, acid resistance, anti-bacterial), strontium (acid resistance, decreased sensitivity, anti-bacterial), aluminum (decreased sensitivity, radiopacity), silicate (calcification), borate (anti-bacterial), and sodium (radiopacity) (Fig. 1).
Fig. 1
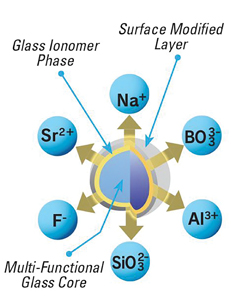
Giomers take up additional fluoride (after fluoride toothpaste, rinse, or varnish applications) and then act as a reservoir until the fluoride is needed. This can be best described as a “fluoride bank” where fluoride is released on demand during cariogenic challenges (to decrease demineralization and enhance remineralization) and then recharged during fluoride application of toothpaste, varnish, etc.5,6 (Fig. 2).
Fig. 2
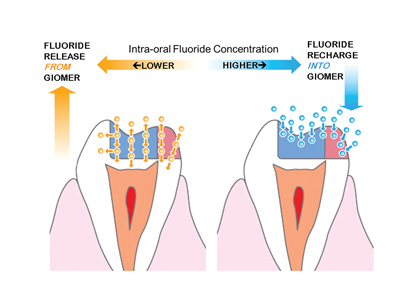
The ion release around the giomer restoration creates a bioactive envelope (protective film layer) which inhibits bacterial adhesion and plaque formation, thereby decreasing the risk of secondary decay and promoting periodontal health (Fig. 3). The ions in the protective film layer neutralize oral acids, in effect creating an acid-free zone around the restoration. The full range of bioactive actions of giomers thereby strengthens surrounding tooth structure and increases the longevity of the restoration.
Fig. 3A

Fig. 3B

Most recently Shofu has introduced Fit SA, a self-adhesive, flowable, bioactive giomer restorative material – thereby eliminating the bonding layer, which may be a barrier to full ion transfer between the restoration and the tooth. There is no bonding layer to block the beneficial action of giomer ions on the tooth. The bonding agent is within the material itself. This is chemical as well as micro-mechanical (through resin tag infiltration) bonding (Fig. 4).
Fig. 4

Fit SA is designed to be used as a liner and as a restorative material, in small Class I, Class III, and Class V
restorations, and any other non load-bearing indications. It is ideal in pediatric and geriatric cases where speed and efficiency are of the essence. No etching, no rinsing, no mess. Defects and secondary decay around old crowns are speedily repaired with a material that delivers bioactive benefits for many years after placement.
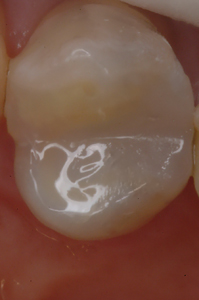
Perimeter preparation – Time and function may break down the margins of a restoration, at the interface between tooth structure and composite resin. In many cases, while the margin exhibits localized or “perimeter” breakdown and secondary decay, the rest of the restoration remains intact. The dentist is then faced with the decision of replacing or repairing the restoration. This is not the time to “watch and wait” until the restoration becomes unsalvageable. A “perimeter preparation” is a proactive treatment performed at an early stage before more extensive treatment is required. All stain and secondary decay around the defective margin must be removed. The ideal replacement material should integrate with the original restoration and the remaining tooth structure, be plaque resistant and have remineralizing properties, to prevent future perimeter breakdown (Fig. 5).7 Fit SA is this material.
Fig. 5A

Fig. 5B
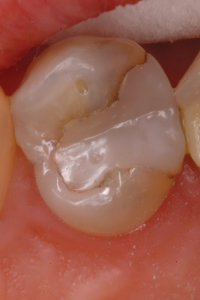
Fig. 5C
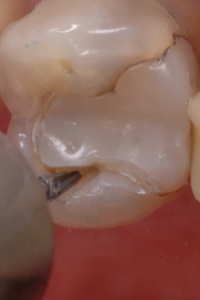
Fig. 5D
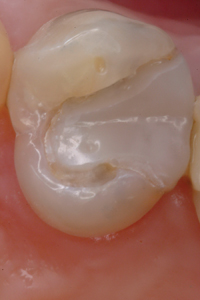
Fig. 5E
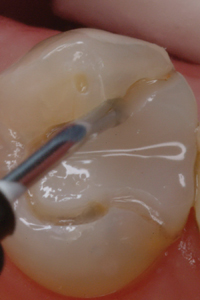
Fig. 5F

Fig. 5G
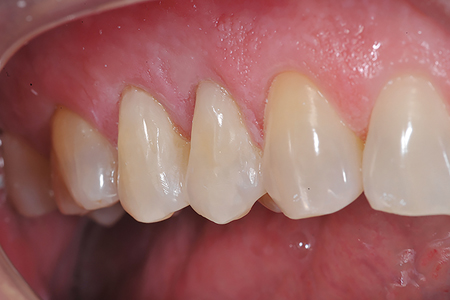
Over the life of a restoration, the bonding layer may eventually create a stain line at the margin. With no bonding layer, no stain line will develop. This is particularly beneficial in Class III and Class V restorations (Fig. 6). The Fit SA restoration also blends easily with the surrounding dentition due to its unique filler structure that combines the light transmission and diffusion properties of dentin and enamel.
Fig. 6A
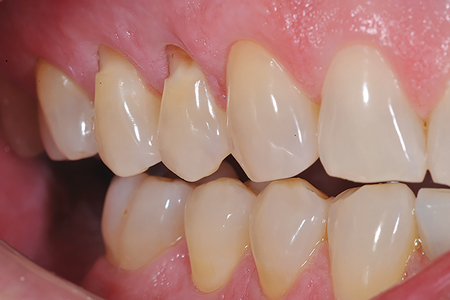
Fig. 6B
Glass ionomers, the original bioactive materials, should be used in challenging restorative areas, where it is difficult to achieve a dry field. They are also indicated as protective sealants against caries during tooth eruption and development.8
Bioactive Regeneration of pulpal tissue: Saving tooth vitality
What is the protocol in cases of deep decay where a remineralizing resin liner is just not enough to protect pulp vitality? Where decay reaches dangerously close to the pulp, or even slightly into it? Biodentine (Septodont, Lancaster, PA) is a calcium silicate material developed to protect the pulp and to assist in regenerating pulpal tissue, without the physical limitations and handling challenges of earlier MTA products. Biodentine provides a hermetic seal that protects the pulp from bacterial infiltration and provides an ideal environment for healing to take place. This seal is formed by Biodentine’s micromechanical retention into the dentinal tubules as well as by its stimulation of odontoblasts to deposit dentin.9 Upon mixing, Biodentine produces calcium hydroxide, a known pulp regenerating agent.10 Calcium hydroxide on its own does not have long term stability and with time turns into what can best be described as “cottage cheese”. The Biodentine formulation produces a gel-like material envelope around the calcium hydroxide that is strong and not porous. This harnesses the regenerative powers of calcium hydroxide without its physical disadvantages.
Biodentine, through the action of calcium hydroxide in this enhanced physical state, boosts the deposition of reparatory dentin by odontoblasts, creating a dense dentin barrier11,12 that allows for isolation and healing of pulpal tissue.13
It should be noted that non-resin based materials (Biodentine) and ProRoot MTA (Dentsply Sirona, York, PA) were more effective than a resin based material (TheraCal, Bisco, Schaumburg,IL) in a partial pulpotomy study.14 In another study, TheraCal was shown to increase inflammatory cells and to decrease the regenerative processes of the pulp while Biodentine did not increase inflammation and supported pulpal regeneration.15 These studies suggest caution in using resin-based materials for vital pulp therapy.1
Biodentine can be used as a base in deep carious lesions, a pulp capping agent in vital pulp therapy (both direct pulp capping and pulpotomy), for root repair (perforations, resorptions, apexifications, etc) – and anywhere pulpal regeneration and tissue healing is needed.1
What about handling? Biodentine has been underused in clinical practice due to the suggestion that complete set of the material is necessary prior to finishing the restoration with composite resin. Is this because the material does not completely set under the composite resin? Is the bond inadequate between the unset Biodentine and the overlying composite resin?
Instructions recommend bulk-filling of Biodentine completely and using it as a temporary restoration while evaluating pulpal response. The patient then returns in 3-6 months to replace the external layers with composite resin. A second option is to wait chairside for 12 long minutes for the material to set completely before placement of the composite resin.
The author undertook a simple counter-top experiment to test whether Biodentine would achieve total set after being sealed with composite resin within a minute after placement, and whether the two materials would achieve a good bond.
The Experiment
Biodentine was mixed and inserted into 2 cut straws which were placed on a flat surface (Figs. 7A,B). Shofu BeautiBond was applied and light cured. (A 7th generation no-etch bonding agent is preferred as it eliminates the possibility that etching or rinsing could interfere with the set or bond of the materials). Beautifil Flow Plus 03 was then applied (Fig. 7C) and light cured (Fig. 7D). The straws with the 2 restorative materials and bonding agent were left for 24 hours.
Fig 7A

Fig. 7B

Fig. 7C

Fig. 7D

After 24 hours the straw matrix was removed, and it was observed that the Biodentine had set rock hard (Fig. 7E). An attempt was made to break the bond between the 2 materials (Fig. 7F). The result was a cohesive fracture (Fig. 7G) within Biodentine (a therapeutic, regenerative material, not designed to withstand shearing forces). This was not a bonding failure between the 2 materials.
Fig. 7E

Fig. 7F
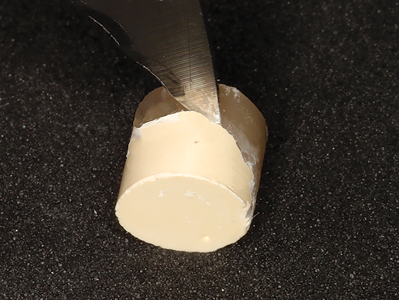
Fig. 7G

The take-away: There is no reason to wait 12 minutes for the complete set of Biodentine before finishing the restoration with composite resin. Biodentine sets completely underneath composite resin, and the bond between them is strong.
Conclusion
The answer to our original question “bioactivity: why should I care?” is clear. Whether it is the everyday “go-to” restorative giomer, or glass ionomer for challenging locations, or calcium silicate to save pulps – bioactive materials can help stop and reverse disease. They are better for the patient. They enhance clinical outcomes. They are easy to use. The time has come for bioactive dentistry!
Oral Health welcomes this original article.
References
- Goldstep F, Bioactivity in Restorative Dentistry: A User’s Guide. Oral Health; 2017 December: 6-18.
- Gordan V et al, A Clinical Evaluation of a Self-etching Primer and a Giomer Restorative Material: Results at Eight Years. J Am Dent Assoc. 2007 May;138(5): 621-7.
- Gordon V et al, A Clinical Evaluation of a Giomer Restorative System Containing Surface Pre-reacted Glass Ionomer Filler: Results From a 13-year Recall Examination. J Am Dent Assoc. 2014 Oct;145(10):1036-43.
- Miyauchi T et al, The effect of Giomer restorative materials on demineralized dentin, 2010, IADR Abstract 135006.
- Dhull KS, Nandlal B, Comparative evaluation of fluoride release from PRG-composites and compomer on application of topical fluoride, Journal of Indian Society of Pedodontics and Preventive Dentistry, 2009:27:1:27-32.
- Okuyama K, et al, Fluoride release and uptake by various dental materials after fluoride application, Am J Dent, 2006:19:123-127.
- Goldstep F, The Perimeter Preparation. Oral Health; 2012 July: 18-21.
- Goldstep F, Delios C, Glass Ionomer for Proactive Intervention. Oral Health; 2018 December: 42-48.
- About I, Biodentine: from Biochemical and Bioactive Properties to Clinical Applications. Giornale Italiano di Endodonzia. 2016;30: 81-88.
- Camilleri J, Laurent P, About I, Hydration of Biodentine, Theracal LC, and a Prototype Tricalcium Silicate-based Dentin Replacement Material after Pulp Capping in Entire Tooth Cultures. JOE. 2014; 1-9.
- About I, Coiffage pulpaire direct de RD94 a l’aide du modele de culture de dent entiere, Report RD EN RA EXT-RD94/096, 2007.
- Shayegan A, RD 94 Etude #PC08-001, Etude de RD 94 comme agent pulpaire dans le cadre de pulpotomie et coiffage direct sur les dents lacteales de cochon, Report RD RA DEV 94-006, 2009.
- About I, Effects des materiaux bioactifs Biodentine™ et Calcipulpe® sure les etapes preoces de la regeneration dentaire, Report RD RA DEV 94-013, 2009.
- Bakhtiar H, Nekoofar MH, Aminishakib P, et al. Human Pulp Responses to Partial Pulpotomy Treatment with TheraCal as Compared with Biodentine and ProRoot MTA: A Clinical Trial. JOE. 2017; 1-6.
- Giraud T, Rufas P, Chmilewsky F, et al. Complement Activation by Pulp Capping Materials Plays a Significant Role in Both Inflammatory and Pulp Stem Cells’ Recruitment. JOE. 2017;43(7): 1104-1110.
About the Author
 Dr Fay Goldstep has lectured extensively on Proactive/Minimal Intervention Dentistry, Soft-Tissue Lasers and Bioactive Dental Materials. She has been a contributing author to four textbooks and has published more than 100 articles. Dr Goldstep sits on the editorial boards of Oral Health Journal, Dental Tribune US Edition, Dental Asia and REALITY. She has been listed as one of the leaders in continuing education by Dentistry Today since 2002. Dr. Goldstep is a consultant to a number of dental companies and maintains a private practice in Richmond Hill, Ontario. She can be reached at goldstep@epdot.com.
Dr Fay Goldstep has lectured extensively on Proactive/Minimal Intervention Dentistry, Soft-Tissue Lasers and Bioactive Dental Materials. She has been a contributing author to four textbooks and has published more than 100 articles. Dr Goldstep sits on the editorial boards of Oral Health Journal, Dental Tribune US Edition, Dental Asia and REALITY. She has been listed as one of the leaders in continuing education by Dentistry Today since 2002. Dr. Goldstep is a consultant to a number of dental companies and maintains a private practice in Richmond Hill, Ontario. She can be reached at goldstep@epdot.com.
To see more articles from the July/August 2020 issue, please click here!












