Toxic biofilm is enemy number one when it comes to dental diseases. It lurks in a patient’s mouth above and below the gum line. It clings to natural teeth, restorative work, gingival tissue and the tongue, implants and orthodontic appliances. It is very challenging to remove or debride all of the biofilm from the oral cavity. But with a repurposed technology in air polishing, we have a fighting chance as clinicians to thwart it’s destructive path.
What we used to consider to be planktonic bacteria floating in crevicular fluid has become a much more complex entity know as biofilm. Bacteria colonize and replicate within their safe environment of a community, held together by a sticky protein matrix known as glycocalyx. The bacteria communicate within this “biome” for their replication and survival. As this biofilm matures and spreads, it can lead to inflammatory processes that manifest as periodontal or caries diseases. Due to the challenging anatomy of teeth and roots, this becomes very difficult to remove with traditional instruments as in the past.
Traditional air polishing as done in the past was a cosmetic procedure concentrating on removing stain above the gum line. The powder most often used was Sodium Bicarbonate and most clinicians experienced difficulty in using the devices due to discomfort for the patient, messiness and grittiness of the powder, and lack of control of the particle and bacteria laden aerosol. I like to joke that it was like a day at the beach: water washing over you, gritty sand getting in every part of your body and tasting like saltwater!
Today a paradigm shift is occurring within air polishing as we now use it to “pressure wash” the patient’s mouth for more complete and quicker removal of the biofilm. This is now considered to be therapeutic, not cosmetic as in the past.1 The secret is in the smaller particle size and type of powder used today and in the devices designed to accommodate this powder efficiently with the proper air pressure.
Traditional sodium bicarbonate or aluminum trihydroxide particles are 75-microns and up in size, whereas the newer entrants on the market, glycine or erythritol powders, are 14-25 microns. I compare this size difference to getting sprayed with kosher salt (larger particle) or cornstarch (smaller particle). Larger particles would sting and be more aggressive at removing or harming oral structures. Smaller particles can be used on any surface supra or subgingivally, as they are very gentle to structures.
Glycine is a nonessential amino acid and is naturally sweet flavored and 25 microns in size. Erythritol is a natural plant sugar and is 14 microns in size. Either powder can be used successfully subgingivally without harming any natural or restorative oral structures. Glycine may have some therapeutic properties as it has been shown to interfere with cytokines produced by the inflammatory process. This cytokine byproduct interferes with collagen production.2 Erythritol, though a smaller particle, is harder and is somewhat more effective at removing stain without harming any of the tooth structures.3
There are several units that can accept this smaller size particle successfully. Acteon has a portable handheld unit called the Air and Go (Fig. 1) that has interchangeable powder chambers that will accept both large or small size particles. They also have a perio nozzle that is designed to go subgingivally but is made of inflexible metal. Coltene has a tabletop combo unit with an air polisher that will accept the smaller particle but their perio nozzle is also metal.
Fig. 1

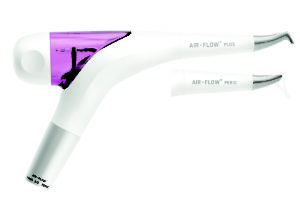
I am most familiar with the EMS-Hu-Friedy units. Their table top unit has removable chambers so switching powders becomes very easy. Their handheld Handy 3.0 Premium (Fig. 2) has both the standard handpiece that can be used around all oral structures supra and subgingivally, as well as a perio handpiece that accepts a disposable flexible nozzle that can be inserted into a sulcus up to 10mm. The handheld unit is very portable and is a good starting point for a lot of practices. I consider it another tool in my toolbox that can be shared when the implant or ortho patient comes in.
Fig. 2
If the device is not intended for smaller particle use it should not be used as it could clog the device and invalidate the warranty. For those who utilize the Dentsply Prophyjet, this is especially true, since the air pressure in that unit is set higher to impel the bigger size particle recommended for use in that device. Thus, PSI is too aggressive for tender tissues and restorative materials even if glycine could be used.
While biofilm gets disrupted with any manipulation within the pocket and on the tooth surface with hand or power inserts, research is showing that the most efficient way to disrupt the biofilm is via what is called Air Flow Therapy, or Guided Biofilm Therapy.4 As a clinician, I debride the soft deposits/biofilm/loosely adherent stain from all oral surfaces I can access with glycine powder Airflow therapy first. This saves me time, approximately five to ten minutes, as I then follow with my ultrasonic scaler and am not wasting effort scaling soft deposits or invisible biofilm. Research backs up my claim of time savings.5,6
Any remaining stain is usually mixed in with calculus and as Airflow does not remove hard deposits I need to scale that off anyhow. I suggest that clinicians utilize disclosing solution when learning how to effectively use Airflow Therapy. Disclose half the mouth so the biofilm is visible and practice removing it thoroughly. Then, do the other half of the mouth and disclose to see what you left. This will soon have you more rapidly and efficiently using the device. I use both a stationary saliva ejector resting in the posterior vestibule to gather up excess water, and a HVE suction device in my non-dominant hand (Fig. 3). I follow the Airflow handpiece around the mouth to suction up the aerosol created by the procedure. This is definitely not a “day at the beach” as very little aerosol/powder gets outside the mouth.
Fig. 3

Utilizing Airflow Therapy in your practice will not only save you time that can be spent on other procedures or patient education, it will benefit the patient’s overall health. Research shows GBT removes biofilm more completely and in less time.5,6
Being the practice that offers cutting edge technology is a benefit to patients via value added services, as well as being a marketing tool. The ability to safely and effectively remove biofilm from root surfaces, gingivae, implants, restorative material and orthodontic appliances is definitely a benefit to any practice. Today’s Guided Biofilm Therapy using Airflow Therapy is definitely not your grandmother’s air polishing as in the past!
References
1. A Paradigm Shift in Mechanical Biofilm Management. Bastendorf KD et al, Quintessence International 2013 July/August; 44(7): 475-477
2. Potential Immune Modularity Role of Glycine in Oral Gingival Inflammation. Schaumann, Teresa et al. Clin Dev Immunol. 2013; 2013: 808367.
3. Davis, K. Erythritol Powder: Its broad implications for oral health. RDHMag 2018 Aug; p 26
4. Graumann S, Sensat M, Stoltenberg J Air Polishing: A Review of Current Literature. J Dental Hygiene 2013; 87:173-180
5. Wennstrom JL, et al. Subgingival debridement of periodontal pockets by air polishing in comparison with ultrasonic instrumentation during maintenance therapy. J Clin Periodontol 2011; 38: 820-827
6. Moene R et al. Subgingival plaque removal using a new air polishing device. J Periodontol 2010; 81: 79-88
About The Author
 Nancy has been a Jameson advisor since 1998. Her area of expertise is in clinical procedures, periodontal therapy and instrumentation. She promotes the concept of the entire team being involved in periodontal treatment and continuous care of their patient family. Nancy has provided extensive knowledge and expertise to the profession through writing, lecturing, and coaching of dental teams nationwide. For more information on Nancy and the entire spectrum of Jameson services, visit www.jmsn.com.
Nancy has been a Jameson advisor since 1998. Her area of expertise is in clinical procedures, periodontal therapy and instrumentation. She promotes the concept of the entire team being involved in periodontal treatment and continuous care of their patient family. Nancy has provided extensive knowledge and expertise to the profession through writing, lecturing, and coaching of dental teams nationwide. For more information on Nancy and the entire spectrum of Jameson services, visit www.jmsn.com.
RELATED ARTICLE: Is Your Tongue Causing Your Health Problems?












