I first began using silver diamine fluoride (SDF) in my private pediatric dental practice in 2015. Minimally Invasive Dentistry is a topic near and dear to my heart as a mother and advocate for improving children’s oral health and safety. My own daughter having surgery under general anesthesia at just nine months coupled with experiencing a medical emergency with a patient with Autism undergoing IV sedation in my office led me to question what I could do differently and better for my patients and their families. That began my journey to silver diamine fluoride (SDF) and silver modified atraumatic restorative treatment (SMART). By incorporating these new options, I have reduced the number of sedations done in my practice by 67% since 2014. I hope to help spread the word about this versatile minimally invasive treatment option to my colleagues.
SDF is a topical antimicrobial and remineralizing agent cleared by Health Canada in 2017 for caries arrest. While its precursor, silver nitrate, dates back to the mid 1800’s, silver diamine fluoride was developed in Japan in the 1960’s, approved and sold as Saforide beginning in 1970. SDF first came to the Canadian market as Advantage Arrest Silver Diamine Fluoride 38% from Oral Science. Its chemical composition is 25% silver, which is antimicrobial, 8% ammonia, which acts as a solvent, and 5% fluoride, for remineralization. There is an abundance of scientific evidence demonstrating the efficacy of SDF including 12 randomized clinical trials. 1-12 A recent systemic review and meta-analysis found that the use of SDF is 89% more effective in controlling/arresting caries than other treatments or placebos, and the quality of evidence was graded as high.
Silver Diamine Fluoride is fast becoming a staple of many dentists’ armamentarium. This article will illustrate some of the many clinical uses for Silver Diamine fluoride. I now use SDF every day in my private pediatric practice, but I didn’t jump in over my head right out the gate. The more I used it, and particularly the more I read and studied about it, the more confident I became. My suggestion is to start small and cautiously, with careful case selection. As you get more comfortable and confident with this treatment option, you’ll find yourself using it more and finding more clinical uses for it. To be perfectly honest, I was initially nervous about what the perception of SDF would be from my patients’ parents. I was pleasantly surprised by the warm reception of parents and patients to this treatment. Some of the comments included, “I’m so glad you’re on the cutting edge,” “I’m glad you think outside the box,” and “I wish my dentist did this, do you take adults?”
The following list will highlight just a few of the valuable clinical uses for SDF. It is not an exhaustive list, but rather some suggestions for my fellow dental professionals to see the potential this new treatment option may have for their patients and practices.
Clinical Uses for Silver Diamine Fluoride
1. Delay or Avoid the Need for Sedation to Treat Pediatric Patients
In 2016, the FDA released a black box warning that the repeated or lengthy use of general anesthetic and sedation drugs during surgeries or procedures in children younger than three years may affect the development of children’s brains. This coupled with a number of recent, highly-publicized dental anesthesia related adverse outcomes, has increased the interest and demand from parents for minimally invasive treatment options for their children. In just one minute, with little more than a microbrush, SDF can be painlessly brushed on a carious tooth and arrest 80% of lesions. There will always be patients with advanced caries with pulpal involvement and infection that will not be candidates for SDF treatment, who may still require sedation or general anesthesia. However, there are many young patients that can benefit from SDF treatment as a stop-gap until they are older and/or more cooperative for traditional restorations and/or until the teeth exfoliate without the need for surgical intervention (Case 1).
Case 1
SDF application is easy and painless for pediatric patients, building trust and positive dental experiences for a lifetime of good oral health.
Fig. 1

Fig. 2

2. Caries Arrest for Special Needs and Medically Frail Patients
There are many patients who can benefit from SDF treatment who are unable to have traditional restorative dentistry due to special needs or complex medical problems. This includes patients undergoing chemotherapy, suffering from chronic diseases, salivary dysfunction or polypharmacy, or immunocompromised patients. Special needs patients also benefit from the simple and non-invasive nature of SDF treatment. As a pediatric dentist, I have been able to help many patients with special needs, such as sensory processing disorder, Down Syndrome and Autism receive care in my practice, helping them avoid the added cost and risk of hospital dentistry.
3. Caries Control in Patients with Extensive Treatment Needs
Sadly, many patients suffer from extensive dental disease, the cost of which may be beyond their financial means. Rather than letting everything get worse, spiraling deeper into a hole that is even more difficult to recover from, SDF can help bridge the gap until an individual has the financial means for restorative care. This can build goodwill in the practice, where a patient may have financial pressures at home or insurance limitations necessitating a prioritization of care. This can also translate into public health and outreach. Earlier in my career, my missionary and volunteer work were characterized by addressing the worst tooth or quadrant with surgical intervention. Now, armed with SDF and glass ionomer cement, I can treat an entire mouth of disease.
4. Silver Modified Atraumatic Restorative Treatment (SMART)
SDF does not restore form or function, so cavitated lesions would still benefit from a restoration. Lesions arrested by SDF can be restored in an efficient and effective manner using glass ionomer cement restorative materials, an approach known as SMART. The material of choice for SMART is high viscosity glass ionomer cement (HVGIC), such as Fuji EQUIA Forte (GC America) (Case 2).
HVGIC is a self-curing, bulk-fill restorative material. It is superior to resin composite in some instances because it is the more biocompatible restorative material. It produces significantly lower shrinkage stress, bonds via chemical and micro-mechanical adhesion, and releases and recharges with fluoride (thereby reducing both s. mutans levels in the biofilm and recurrent caries). The SDF treated lesion is prepared with an atraumatic approach (hand instruments or slow speed round bur), and a glass ionomer restoration is placed.
Carious root surfaces are clinically challenging, particularly in the geriatric population. A recent systematic review with meta-analysis published in the Journal of the American Dental Association found that “Yearly 38% SDF applications to exposed root surfaces of older adults are a simple, inexpensive, and effective way of preventing caries initiation and progression.” 2 Having this option will benefit dentists and their patients in private practice, but also has the advantage of increasing access to care via teledentistry, since SDF can be applied by dental hygienists in nursing homes and assisted living facilities.
Case 2
A carious occlusal lesion in a mandibular primary first molar is arrested with Advantage Arrest Silver Diamine Fluoride 38%. 2 weeks later, the lesion is restored using the SMART technique (Silver Modified Atraumatic Restorative Treatment) with a high viscosity glass ionomer cement restorative, Fuji EQUIA Forte, to avoid sedation in a 5- year-old patient. The restoration masks the black scar, providing a pain-free, efficient, durable and aesthetic restoration. 6-month follow-up, looking good.
Fig. 1

Fig. 2
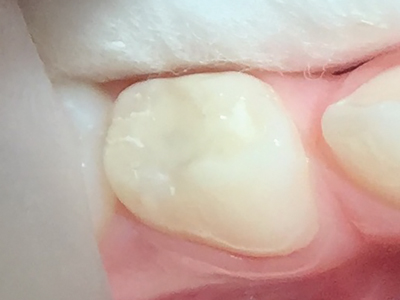
Fig. 3

6. Hypersensitivity
SDF acts as a powerful desensitizer by occluding dentinal tubules, producing preferential fluorohydroxyapatite and increasing mineral density and hardness. 1,2 Hypersensitivity symptoms should improve within 24 hours following SDF application, though anecdotally, some patients have reported same-day improvement of their symptoms. SDF will not stain healthy tooth structure, so it is an excellent option for patients suffering from hypersensitivity who have found little to no relief with typical over-the-counter treatments such as potassium nitrate containing toothpastes for sensitivity. Anecdotally, some patients have reported relief of long-term hypersensitivity symptoms after just one SDF application. If symptoms return, the quick, simple, and affordable application can be repeated.
7. Treatment of Molar Incisor Hypomineralization (MIH)
Molar Incisor Hypomineralization (MIH) is a clinically challenging condition seen in as many as 20-40% of permanent first molars. 3 These teeth are notoriously hypersensitive, difficult, if not impossible to adequately anesthetize, and have a 10-fold higher risk of developing caries. Historically, restoration of MIH affected molars has involved invasive, expensive, and generally unpleasant procedures which leave much to be desired for both the patient and practitioner. Depending on the severity, earlier in my career, I treated MIH affected molars with resin- based sealants and fillings, stainless steel crowns, or even oral surgeon and orthodontic referrals for extraction and second molar substitution. A game changing new treatment option for these teeth is SDF to desensitize the teeth, and HVGIC as a minimally invasive restoration. A recent study from the University of Brasilia, Brazil, found a 98% survival rate of restorations on first permanent molars affected by MIH after 12 months using a glass ionomer restorative system (Fuji EQUIA Forte, GC America) placed with the ART technique. 2 I have been achieving similar, successful outcomes in my practice treating MIH molars with SDF and Fuji EQUIA Forte.
8. Recurrent Caries at Restoration Margins
Caries is a chronic biofilm disease for which there is no cure, and restorations have a finite longevity. As a result, we’ve all faced the clinical scenario where a patient develops recurrent caries at a restoration margin. Whether it is a filling or a crown, SDF treatment is a simple and effective way to prolong the life of an existing restoration. The simplicity and low cost of the treatment is particularly appealing to patients, especially when faced with frequency issues from insurance companies. Offering SDF as a time buyer builds good will and loyalty between the dental provider and the patient.
9. Incipient Interproximal Lesions
Incipient interproximal lesions present a challenge clinically since accessing the lesion involves removal of a considerable amount of sound tooth structure. Since fillings have a finite longevity, once you cut a tooth, you are beginning the life-long cycle of “redo-dentistry”. Many lesions, in particular those lesions confined to enamel, are capable of arresting and remineralizing. SDF can be applied interproximally using puffy floss, such as Superfloss from Oral-B or GUM Expanding Floss from Sunstar. Simply clean, isolate, and dry the affected area, then place the floss into the contact. Apply SDF to the floss using a microbrush, saturating it with the solution and allowing it to soak in the interproximal space for one to three minutes. This approach can conserve natural tooth structure and postpone or even prevent the need for a surgical intervention (Case 3).
Case 3
SDF applied with puffy floss to arrest incipient interproximal lesions in a teenager. Notice how very little stain shows clinically and natural tooth structure is conserved and remineralized.
Fig. 1

Fig. 2

Fig. 3

Conclusion
The list of potential clinical uses for SDF goes on and on. The low-cost, low-tech (minimal equipment, no electricity required), and low-technique sensitivity of the treatment offers versatility which can translate into virtually any clinical setting. Whether you are in private practice or public health, treating patients that are young, old, and everything in between, you are bound to find a use for this exceptional oral medicine.
You can start small and proceed cautiously as you incorporate silver diamine fluoride into your clinical practice. Before you know it, you might just find yourself using SDF every day and, like me, you may never want to practice without it again.
For more information on silver diamine fluoride, including free downloads of my forms, links to YouTube tutorials, and webinars, please visit www.kidsteethandbraces.com. OH
Oral Health welcomes this original article.
References
- Chu CH, Lo ECM, Lin HC. Effectiveness of silver diamine fluoride and sodium fluoride varnish in arresting dentin caries in Chinese preschool children. J Dent Res 2002;81(11):767-770.
- Zhi QH, Lo ECM, Lin HC. Randomized clinical trial on effectiveness of silver diamine fluoride and glass ionomer in arresting dentine caries in preschool children. J Dent 2012;40(11):962-967.
- Yee R, Holmgren C, Mulder J, Lama D, Walker D, van Palenstein Helderman W. Efficacy of silver diamine fluoride for arresting caries treatment. J Dent Res 2009;88(7):644-647.
- Santos Dos VE, de Vasconcelos FMN, Ribeiro AG, Rosenblatt A. Paradigm shift in the effective treatment of caries in schoolchildren at risk. Int Dent J 2012;62(1):47-51.
- Llodra JC, Rodriguez A, Ferrer B, Menardia V, Ramos T, Morato M. Efficacy of silver diamine fluoride for caries reduction in primary teeth and first permanent molars of schoolchildren: 36-month clinical trial. J Dent Res 2005;84(8):721-724.
- Zhang W, McGrath C, Lo ECM, Li JY. Silver diamine fluoride and education to prevent and arrest root caries among community- dwelling elders. Caries Res 2013;47(4):284-290.
- Liu BY, Lo ECM, Chu CH, Lin HC. Randomized trial on fluorides and sealants for fissure caries prevention J Dent Res 2012;91(8):753-758.
- Tan HP, Lo ECM, Dyson JE, Luo Y, Corbet EF. A randomized trial on root caries prevention in elders. J Dent Res 2010;89(10):1086-1090
- Monse B, Heinrich-Weltzien R, Mulder J, Holmgren C, van Palenstein Helderman WH. Caries preventive efficacy of silver diamine fluoride (SDF) and ART sealants in a school-based daily fluoride toothbrushing program in the Philippines. BMC Oral Health 2012;12(1):52.
- Braga MM, et al. Effect of silver diamine fluoride for arresting caries treatment. J Dent Res 2009;88:644-7.
- Duangthip D, et al. A randomized clinical trial on arresting dentin caries in preschool children by topical fluorides, 18 month results. J Dent 2015;444:57-63.
- Fung MHT, et al. Arresting dentin caries with different concentration and periodicity of silver diamine fluoride. JDR Clin Trans Res 2016;1:143-52.
- Chibinski A, et al. Silver diamine fluoride has efficacy in controlling caries progression in primary teeth: A systemic review and meta-analysis. Caries Res 2017;51:527-54.
- Oliveira, Controlling caries in exposed root surfaces with silver diamine fluoride: A systematic review with meta-analysis JADA 2018
- Mei ML, et al. Formation of Fluorohydroxyapatite with Silver Diamine Fluoride. J Dent Res. 2017 Sep;96(10):1122-1128.
- Grossi J, et al. Glass hybrid restorations as an alternative for restoring hypomineralized molars in the ART model. BMC Oral Health 2018; 18(65).
About the Author
 Dr. Jeanette MacLean is a Diplomate of the American Board of Pediatric Dentistry, Fellow of the American Academy of Pediatric Dentistry, owner of Affiliated Children’s Dental Specialists in Glendale, Arizona, and mother of two. She received her dental degree, with honors, from the University of Southern California in 2003 and completed her specialty training in pediatric dentistry in 2005 at Sunrise Children’s Hospital through the University of Nevada School of Medicine. Dr. MacLean has become an internationally recognized advocate and expert on minimally invasive dentistry, appearing in newspapers, magazines, television, and continuing education lectures on this hot topic. Most notably, she was featured in the July 2016 New York Times article, A Cavity Fighting Liquid Helps Kids Avoid Dentists’ Drills, which brought national attention to the option of treating cavities non-invasively with silver diamine fluoride.
Dr. Jeanette MacLean is a Diplomate of the American Board of Pediatric Dentistry, Fellow of the American Academy of Pediatric Dentistry, owner of Affiliated Children’s Dental Specialists in Glendale, Arizona, and mother of two. She received her dental degree, with honors, from the University of Southern California in 2003 and completed her specialty training in pediatric dentistry in 2005 at Sunrise Children’s Hospital through the University of Nevada School of Medicine. Dr. MacLean has become an internationally recognized advocate and expert on minimally invasive dentistry, appearing in newspapers, magazines, television, and continuing education lectures on this hot topic. Most notably, she was featured in the July 2016 New York Times article, A Cavity Fighting Liquid Helps Kids Avoid Dentists’ Drills, which brought national attention to the option of treating cavities non-invasively with silver diamine fluoride.
RELATED ARTICLE: Silver Diamine Fluoride Unstained and Liberated












