Abstract
The existence and preservation of attached keratinized gingiva around natural teeth and dental implants plays an important role in periodontal1 and peri-implant health.46,47 This paper describes a novel surgical technique that addresses multiple adjacent Miller class II and III recession defects5 in a predictable one staged surgical procedure. The goal of treatment is to improve esthetic outcomes, gain clinical attachment and keratinized tissue levels in addition to possible root coverage. A combination of traditional periodontal plastic procedures are utilized with sound evidence based techniques. To date, over 100 surgical cases have been completed. Surgical steps and rationale for this new technique are detailed and representative cases will be shown.
Introduction
As many epidemiological reports suggest, gingival recession affects the majority of the adult population.2,3 Gingival recession is defined as the apical migration of the soft tissue margin around teeth leading to exposure of the cementoenamel junction (CEJ) and the dentinal root surface4 and is classically categorized by Miller.5,6 The philosophy for increasing the zone of keratinized tissue for teeth is for attachment stability, facilitation of plaque control and to prevent further gingival recession from frenal/muscle pulls.6,7 Periodontal plastic procedure articles in the literature evidentially demonstrate very predictable and esthetic root coverage in the majority of Miller class I & II single or adjacent tooth sites with and without the adjunct of a subcutaneous connective tissue graft (SCTG)3,7 irrespective of the surgical technique/s utilized (ie pedicles, tunnels, coronally positioned flaps (CPF), guided tissue regeneration (GTR) etc); provided that biologic principles for obtaining root coverage are satisfied (ie interproximal papillary height and interseptal bone height). In addition, the results of long term clinical retrospective studies in private practice demonstrate that not only is there effective root coverage but indeed mean root coverage tends to improve over time after initial surgery.8 In acellular dermal matrix and GTR studies over the short and long term, neither showed a statistically significant increase in root coverage as opposed to the use of autogenous tissues.9,10 The literature also shows clinical cases of inexplicable root resorption in SCTG cases performed in a traditional manner more recently.47,48 In contrast, the presence of multiple recessed sites in a posterior sextant which have advanced recession beyond Miller class I/II presents a clinical conundrum which, in the literature and clinical periodontal practice of periodontics, has not been addressed until just recently.3,11,12 Nevertheless the goal of periodontal therapy should be to address the needs and wishes of each patient, and treatment options should be made available to them.13
Recession in multiple adjacent teeth can occur for a variety of reasons: the patient’s iatrogenic habits, history and/or treatment of chronic periodontal disease by traditional flap therapy, anatomy/malpositioned teeth in the alveolar ridge corridor compromising attachment apparatus, muscle/frenal attachment levels at or beyond the mucogingival junction (MGJ) and secondary parafunctional habits in addition to the obvious long standing results of a history of chronic untreated periodontal disease.
A two staged surgical a) free gingival graft (FGG) + b) surgical repositioning coronally positioned flap (CPF)12,14 procedure can aid individual sites in some Miller II, III recessed areas. These surgical sites which have experienced two surgeries are prone to double the postoperative surgical shrinkage, fibrotic scar tissues and morbidity.30 Patients also report discontent with this treatment option as a result of the need for two surgeries due to increased costs, healing time, work absences and scheduling issues. In difficult economic times, the dental profession must streamline treatment options for patients but still continue to deliver excellent surgical skills to our patients along with the subsequent clinical benefit.
In posterior sextants where there are multiple recessed Miller class II/III sites accompanied by a lack of adequate keratinized and attached gingiva where the adjacent papillae may or may not be affected: no treatment options are available. As such, an effort has been made to fill this void with a corrective surgical procedure able to stabilize progressive recession with the added benefit of some root coverage in Miller III recessions.11
CASE 1
Figure 1

Lower right sextant presurgical photo.
Figure 2

Lower right sextant preop X-ray.
Figure 3

Post-op photo.
Inclusion Criteria For Single Stage Cpf/Fgg
Patients eligible for the one stage CPF/FGG procedure included those with: 1) no health issues as a contraindication for periodontal surgery 2) presence of at least two to three adjacent teeth with Miller II/III facial recession with a frenal/ligamental attachments deemed to be playing a role in creating a stable gingival margin 3) chief complaint of impaired esthetics associated with the recession 4) absence of anatomical defects, caries or restorations needed in the site 5) no periodontal surgical treatment of the involved sites during the previous 24 months 6) adequate oral hygiene 7) non smokers.
Procedure
Patients chosen, exhibited posterior sextants of recession with interproximal bone loss (Miller II or III) and encroachment of gingival recession on the MGJ, commonly found with frenal pulls and muscle attachments, which may or may not have played a role in the etiology of attachment loss; but will play a role on the success and stability of surgical treatment to resolve progressive recession.15,49
A modified one staged FGG + CPF12,14 surgical approach is suggested: implementing Sumner’s full thickness envelope16 and Sorrentino and Tarnow’s17 semilunar procedure augmented with a traditional FGG18 apical to the coronally positioned semilunar flap is suggested. This combination procedure proposes to inhibit the coronal reattachment of the musculature and freni which can play havoc with graft stability in the long-term,49 in addition to increasing the zone of keratinized and attached tissues. Results showed that most class III recessed cases even showed significantly improved root coverage in addition to an ample gain in keratinized and attached tissues.11,12
The first incision was performed by the Er,Cr:YSGG laser (with appropriate soft tissue settings due to its known properties of hemostasis, due to energy penetration). The T4 laser tip incises precisely at the MGJ in a contact/non contact manner depending on the extent of fibrous and ligamentous frenal attachment to make a split thickness incision release of all musculature/fibres prior to reaching the periosteum. All elastomeric fibres are thus incised and denatured at the MGJ. This allows the mucosa to apically relax, laying passively extending the vestibular region without causing any tension on the future graft’s recipient surgical site. Rarely was vestibular suturing needed for hemostasis in the region unlike with a traditional blade incision. Resorbable 4-0 gut sutures are used in the vestibule for this purpose.
Dentinal root preparation is done in a conservative manner if the anatomy is deemed to be inhibitory to coronal flap positioning and stability (ie in root abrasion, horizontal grooving, caries cases, etc). The root surfaces are traditionally modified with root planing to remove calculus, plaque, debris and to create a flat/convex architecture and etched with the hard tissue setting with the Er,Cr:YSGG at the coronal gingival margins prior to suturing of the coronal flap.
The second incision (Fig. 5) is the release of the coronally attached keratinized tissues incised as an envelope flap19 from the sulcus in a full thickness manner20 with microsurgical blades, without the use of vertical incisions on the facial aspect and split thickness in the papillary regions. The flap is coronally positioned with vertical mattress interrupted sutures using 6-0 non-resorbable monofilament microsurgical sutures. Once the coronally placed flap is secure, then the soft tissue laser setting of the Er,Cr:YSGG allows gingivoplasty/gingivectomy via microplastiying of the marginal tissue outline and adaptation of the marginal papillary regions of the gingival margins. An ideal scalloping in the manner of a “paintbrush” stroke of the laser tip allows the coronal architecture of the free gingival margin (FGM) adjacent to the teeth to adapt the marginal tissues precisely. This gingivoplasty allows the whole site to have a more finessed marginal gingival adaptation and contoured appearance against the dentition. The whole coronally positioned tissue is still attached with its mesial and distal blood (Fig. 6) supplies intact and is now fixed with interproximal sutures gaining blood supply from the split thickness papillae and the alveolar bone beneath it. The coronally positioned tissue is immobile and well adapted interproximally to have the best chance of blood vessel anastomoses, but at the apical aspect it lays passively on the periosteal bed.
The donor FGG is then placed apical to the coronally positioned flap onto the periosteum and alveolar bone which has been cleared of any elastomeric fibres and sutured with resorbable interrupted 6-0 sutures engaging the periosteum and the apical aspect of the CPF binding the coronal aspect of the donor FGG down to create immobility and no dead space to ensure the best blood supply. The Er:YSGG laser is used at appropriate settings to actually “weld” and plasty the donor FGG with paintbrush strokes to the CPF at the junction of the new augmented KT/AT to create a more esthetic result and strengthen tissue junction. Pressure on the whole surgical site aids in hemostasis and immobility if needed prior to pack placement, avoiding any dead space or blood clots which may hinder a healthy blood supply for vascularity of the newly placed graft and tissue. Surgical glue is used if necessary for additional stabilization minding any subtissue leakage, which will impede healing. Thus the whole site is tension free with an increased vestibular depth and an increased zone of AT/KT without frenal/muscle hinderance in addition to the potential of root coverage.
Traditional postoperative instructions, analgesics/antiinflammatories are prescribed and patients are followed at one (pak removal), three (suture removal) and six-week intervals for followup as with traditional periodontal plastic procedures. Patients were asked to refrain from any mechanical hygiene techniques in the treated area for the three weeks following surgery and were prescribed 0.12% chlorhexidine mouthwash three to four times per day during the three weeks after the procedure.
CASE 2
Figure 4

UL sextant pre-op photo.
Figure 5

Surgery–flap elevation.
Figure 6

Surgery–coronally positioned flap.
Figure 7

Postop surgery UL sextant–four weeks post-op.
Figure 8

Post-op surgery UL sextant–six weeks post-op.
Results
All patients demonstrated surgical results that had an improved and stable zone of attached and keratinized tissues with no evidence of muscle or frenal reattachment compromising the zone of KT. Most often there was evidence of partial root coverage in class III Miller recessions. The typical white “scar” line evidenced at the MGJ discussed in Sorrentino & Tarnow’s17 original paper can be seen seldomly in this one staged procedure. Patients also found the procedure no more arduous then any other periodontal plastic procedure and more often then not, the treatment was more comfortable then expected using the Er,Cr:YSGG laser for the initial incision. The author has done this procedure in over 100 cases with no untoward results and with great patient satisfaction.
CASE 3
Figure 8A

Pre-op surgery UL sextant.
Figure 8B
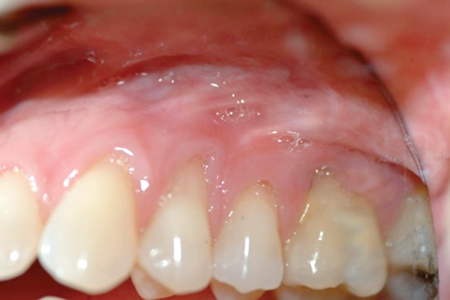
Post-op surgery UL sextant.
Discussion
In recession studies available to review, Miller I and II recessions are the majority found in the literature. In one such study21 coronally advanced flaps were used for multiple teeth in the esthetic zone for root coverage and were noted to be stable at one-year’s time with a statistically significant increase in the amounts of KT. Yet in another study by Gurgan49 after five years, 50% of these cases receded to the presurgical levels as surmised by using alveolar connective tissue as donor as opposed to gingival tissue as donor. Baldi22 concluded that coronally advancing tissues in the treatment of multiple gingival recessions irrespective of the number of recessions or the minimal amount of keratinized tissue apical to the defects, is a successful method in which to achieve root coverage; but that a CPF thickness of >0.8mm was associated with 100% root coverage and that there is a direct relationship between flap thickness and recession reduction. Animal & human papers demonstrate that altered gingival circulation and vitality as determined by fluorescein angiography show that more vascularity is associated with greater graft survival.23 Hwang and Wang24 also indicated that a positive association exists between weighted flap thickness and mean and complete root coverage.
Langer & Langer’s25 technique utilized partial thickness flap elevation to enhance revascularization of the graft, which was then stabilized on the recipient site using periosteal sutures. Raetszke, however,19 advocated the use of the split thickness envelope in isolated areas only, reporting difficulty in obtaining sufficient tissue for use in more extensive areas of recession. However surgically, the elevation of a partial thickness flap can be arduous to perform, particularly in patients with a thin gingival biotype. A partial thickness flap also reduces the KT tissue thickness, and mucosal flaps less than 1 mm thick have been correlated with a reduction in the percentage of root coverage in defects treated using coronally advanced flaps.22,27 Since bilaminar vascularity is required ONLY to provide blood supply to a SCTG, a full thickness CPF was used in this procedure.
Any chance of fenestration or dehiscense over the roots26 remaining after a full thickness CPF is compensated for by the FGG placed over these denuded sites and has proven to be historically not an issue28,29 when grafts were placed straight onto the alveolar bone. No issues were observed due to coronally positioning a full thickness flap versus a partial thickness flap26,29 and yet the benefit of maintaining the full buccal lingual thickness of KT remains a huge asset.20 Also the elevation of a full or partial thickness flap did not appear to influence the amount of KT or the percentage of root coverage achieved postsurgically.20
Literature comparing the CPF vs semilunar flaps showed that both designs were effective in obtaining and maintaining a coronal displacement of the gingival margin. The CPF resulted in clinical improvements significantly better than semilunar flaps for percentage of root coverage, frequency of complete root coverage and gain in clinical attachment level.27
A recent review50 points out that aberrant frenal pulls are a contraindication to the traditional CPF/SCTG as aberrant freni cannot be corrected at the time of surgery because incisions would compromise the blood supply available to the graft. When indicated, a frenectomy is scheduled four to six weeks prior to grafting.15,50 The beauty of the single stage laser CPF/FGG is that all aberrant frenal attachments are dealt with immediately in order not to compromise graft stability, microvasculatature from the recipient bed and graft longevity and thus future recession of the new donor tissue.
CASE 3
Figure 9A

Pre-op surgery.
Figure 9B
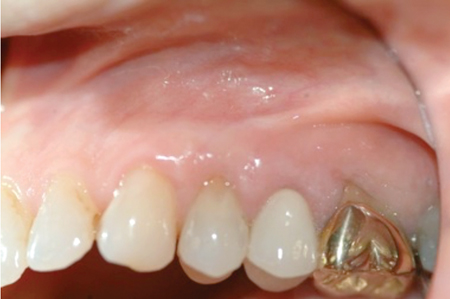
Pre-op surgery.
Figure 9C

Post-op surgery.
In another paper, Harris10 treated 266 defects with connective tissue grafts associated with a coronally advanced or a double papilla flap and reported that the average results of deep recessions (≥ 5 mm) were less favorable (87% versus 95%), when connective tissue grafts were associated with a coronally advanced flap. Although these results were for Miller I and II recessions and showed better results then seen in the Miller III laser CPF/FGG procedure, they confirm limitations when recessions reach 5 mm.30 In the traditional SCTG + CPF without vertical releasing incisions, results in Miller III root coverage, ranging from 1 to 3 mm (mean 1.0 ± 1.5); and Miller IV recessions ranged from 2 to 10 mm (mean 1.86 ± 0.14) the number of Class III and IV recessions were fewer than class I and II recessions. Nevertheless the authors noted that these type III/IV clinical situations could be improved with this procedure.12
It has also been shown that when CPF plus CTG versus CPF procedures for root coverage are compared, the two surgical procedures resulted in similar degree of root coverage but the CPF’s alone reverted to presurgical positions of the MGJ.31 In addition, other long-term papers evaluating CPF with CTG all show that an apical rebound of the MGJ occurs, resulting in unstable root coverage and increased recession.31,45,52 These findings may be explained by Ainamo et al51 who reported that the MGJ will regain its original apical position over time resulting in unstable root coverage while this paper has reestablished a brand new MGJ by adding keratinized FGG apical to the MCJ.
A study comparing CPF techniques with and without the use of vertical releasing incisions both showed to be effective in reducing recession depth, but the envelope type of CAF was associated with an increased probability of achieving complete root coverage and with a better postoperative course. Keloid formation along the vertical releasing incisions was responsible for a poor esthetic outcome along with a longer healing period and a more uncomfortable postoperative course.32
Complete root coverage has been shown to be more likely in Miller I and II type recessions, when marginal tissue recessions are shallower: 66% for an average attachment level of 3.81 mm, in comparison to 50% and 33.3% for mean attachment levels of 5.23 and 5.5 mm, respectively.33,34 Glise and Monnet-Corti also reported that percentage of root coverage was inversely proportional to the width and height of the initial recession dimensions.35 Thus, even though the literature indicates that Miller III and IV recessions have little probability of 100% root coverage, increasing the KT and AT can increase the longevity of a patient’s dentition. Even if only some slight root coverage (based on individual anatomy and physiology) is possible, this may be a significant improvement for the patient esthetically. It will also increase the chances of root coverage as a result of creeping attachment for the patient.36
The Er,Cr:YSGG laser is used here for the first time in surgical grafting procedures as it allows a precision not possible with a surgical blade. Erbium lasers also have the unique ability to vaporize water-containing tissue because of its
wavelength and a hemostatic effect to cauterize blood vessels.
What is clearly observed is that the Er:YSGG laser allows the operator a “microsurgical approach” to finesse the marginal tissue adaptation at the coronal edges along with “laser welding” the FGG donor portion to the CPF portion of the surgical site and control the hemostasis without additional suturing. Pini Prato37 showed that the gingival marginal position at the end of plastic surgery allowed for complete root coverage in Class I and Class II gingival recession defects, and applying this philosophy of treatment to the laser CPF/FGG will only enhance any probability of root coverage in Miller III/IV recession defects.
The elevation of a full thickness versus partial thickness flap does not appear to influence either the amount of keratinized tissue or the percentage of root coverage achieved post-surgically.20 In fact, the thicker coronal tissue, allows an increase in blood supply, surgical anchorage and less tissue trauma with better potential root coverage.38 Pedicle and envelope flaps are successful if the grafted tissues remain vital on the exposed dental avascular root surface and soft tissue healing is critically controlled by this vascularity.28,29 Most reaffirming was that Romanos et al43 showing that the lateral bridging flap technique designed similar to this paper’s CPF, exhibited the most stable location of the repositioned MGJ which was 2-3 mm coronally over five to eight years with stable root coverage and gingival margins.
Of further interest is that treatment success is more predictable with limited interproximal bone loss and undamaged interproximal soft tissue.5,39 Gurgan commented that tooth location, vestibular depth, muscular and frenum insertions may affect wound stability once a flap is advanced.50 Fombellida analyzed the significance of the “vascular supply” as a critical factor on the prediction of root coverage success; a positive balance between the vascularized and nonvascularized areas of the surgical field yields better results in terms of root coverage, even in those less favorable cases, such as Miller Class III recessions.40
Conclusions
Clinicians have all too often are faced with the request “can you not do something to cover these teeth?” Many times the concern is not related to sensitivity but rather that of esthetics due to recession increasing over a period of time for a patient on a stable maintenance schedule. Once the periodontal health was assessed to be stable, the remaining compromised zone of KT/AT and the location of the muscle/frenal attachment often appeared to play a role in progressive recession. Thus the single staged laser CPF/FGG was developed and completed in over 100 patients and was reported to be a comfortable procedure with an esthetic improvement. There are even documented areas of root coverage in Miller III and IV situations and over the years some “creeping attachment” has been documented.36 More investigation in a prospective clinical study, with volumetric methodology44 needs to be done in order to assess the statistical significance of increases in KT and root coverage this new procedure with the adjunct of tissue engineering and biological adjuncts such as enamel matrix derivative, PRP (platelet rich plasma) or PRF (platelet rich fibrin).41
The CAF procedure is effective in the treatment of gingival recessions. However, recession relapse and reduction of KT occurred during follow up periods without any FGG adjunct.42 The baseline width of KT is a predictive factor for recession reduction when using the CAF technique. Thus the new single staged laser CPF/FGG is an effective and predictable method to increase the zone of KT and AT width. The technique can also be shown to increase root coverage in Miller III and IV cases and fulfills the need of the patient, while at the same time reducing the number of appointments and patient costs. OH
Oral Health welcomes this original article.
Disclaimer: Dr. Desai has no financial interests or received any materialistic or financial benefit from corporations with respect to this article.
References:
- Bowers GM. A study of the width of the attached gingiva. J Periodontol 1963;34: 201–209.
- Susin C, Haas AN, Oppermann RV, Huaghjorden O, Albandar JM. Gingival Recession: Epidemiology and risk indicators in a representative urban Brazilian population. JP 2004;75:1377-1386.
- Chambrone L et al. Root-Coverage Procedures for the Treatment of Localized Recession-Type Defects: A Cochrane Systematic Review. JP April 2010, Vol. 81, No. 4, Pages 452-478.
- Wennström J. Mucogingival surgery. In: Lang NP, Karring T (eds). Proceedings of the 1st European Workshop on Periodontology. London: Quintessence, 1994: 193–209.
- Miller PD Jr. Classification of marginal tissue recession. Int J Periodontics Restorative Dent 1985;5:8–13.
- Miller PD Jr. Regenerative and reconstructive periodontal plastic surgery. Mucogingival surgery. DCNA 1988;32:287–306.
- The American Academy of Periodontology. Consensus report: Mucogingival therapy. Ann Periodontol 1996;1:702–706.
- Cortellini, Tonetti, Baldi et al. JCP 2009;36(1):68-79. Multi center Randomized Double Blind Trial … Does the CTG improve Coronally Advanced Flaps for single Tooth Recessions of Maxillary anterior Teeth?
- Harris RJ. Root Coverage with Connective Tissue Grafts: An Evaluation of Short and Long Term Results. JP 2002;73:1054-1059.
- Harris RJ. Acellular dermal matrix used for root coverage: 18mo followup observation. IJPRD 2002;22:156-163.
- Esteibar JRV et al. Root Coverage of Miller Class III Recessions. IJPRD 2011;31:e1–e8.
- Vergara JA and Caffesse RG. Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients. J Periodontol 2004;75:1397-1403.
- Caffesse RG, Mota LF, Morrison EC. The rationale for periodontal therapy. Perio 2000 1995;9:7-13
- Bernimoulin JP, Luscher B, Muhlemann HR, Coronally repositioned periodontal flap. Clinical evaluation after one year. J Clin Periodontol 1975;2:1-13
- Allen AL. Use of the supraperiosteal envelope in soft tissue grafting for root coverage. II. Clinical results. Int J Periodontics Restorative Dent 1994;14:302–315.
- Sumner CF 3rd. Surgical repair of recession on the maxillary cuspid. Incisally repositioning the gingival tissues. J Periodontol 1969;40:119-121.
- Sorrentino JM, Tarnow DP. The semilunar coronally repositioned flap combined with a frenectomy to obtain root coverage over the maxillary central incisors. J Periodontol. 2009 Jun;80(6):1013-7.
- Björn, H.: Free transplantation of gingiva propria. Sven Tandlak Tidskr 22: 684, 1963.
- Raetzke P. Covering Localized Areas of Root Exposure Employing the “Envelope” Technique. JP Jul 1985, Vol. 56, No. 7, Pages 397-402
- Mazzocco F, Comuzzi L, Stefani R, Milan Y, Favero G and Stellini E. Coronally Advanced Flap Combined With a Subepithelial Connective Tissue Graft Using Full- or Partial-Thickness Flap Reflection. J Periodontol 2011;82:1524-1529.
- Zuchelli G & de Santis M. Treatment of Multiple Recession type Defects in patients with Esthetic Demands JP 2000; 71:1506-1514.
- Baldi C et al. Coronally Advanced Flap Procedure for Root Coverage. Is Flap thickness a relevant predictor to Achieve Root Coverage? A 19 Case series. JP 1999;70:1077-1084 (3mos followup for the 0.8mm)
- Burkhardt R, Lang NP. Coverage of localized gingival recessions: comparison of micro- and macrosurgical techniques. JCP Vol 32(3) p287–293, March 2005
- Hwang D, Wang HL. Flap thickness as a predictor of root coverage: A systematic review. J Periodontol 2006;77:1625-1634.
- Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol 1985;56:715–720.
- Haghiahat Modified semilunar coronally advanced flap. J Periodontol. 2006 Jul;77(7):1274-9.
- Santana RB et al. A clinical comparison of two flap designs for coronal advancement of the gingival margin: semilunar versus coronally advanced flap. JCP 2010 Jul;37(7):651-8.
- Dordick B, Coslet JG, Seibert JS. Clinical Evaluation of Free Autogenous Gingival Grafts Placed on Alveolar Bone. Part I. Clinical Predictability. JP Oct 1976, Vol. 47, No. 10, Pages 559-567
- Dordick B, Coslet JG, Seibert JS. Clinical Evaluation of Free Autogenous Gingival Grafts Placed on Alveolar Bone. Part II. Coverage of Nonpathologic Dehiscences and Fenestrations. JP Oct 1976, Vol. 47, No. 10, Pages 568-573
- Miller PD, Allen EP. The Development of Periodontal Plastic Surgery. Perio 2000 1996;11: 7-17.
- Wennström JL, Zucchelli G. Increased gingival dimensions. A significant factor for successful outcome of root coverage procedures? A 2-year prospective clinical study. J Clin Periodontol 1996;23:770–777.
- Zucchelli G, Mele M, Mazzotti C, Marzadori M, Montebugnoli L, De Sanctis M. Coronally advanced flap with and without vertical releasing incisions for the treatment of multiple gingival recessions: A comparative controlled randomized clinical trial. J Periodontol 2009;80:1083-1094.
- Pini Prato GP, Tinti C, Vincenzi G, Magnani C, Cortellini P, Clauser C. Guided tissue regeneration versus mucogingival surgery in the treatment of human buccal gingival recession. J Periodontol 1992;63:919–928.
- Pini Prato GP, Franceschi D, Cairo F, Rotundo R. Prognostic factors in the treat- ment of gingival recessions. J Parodontol 2006;25:175–190.
- Glise J-M, Monnet-Corti V. La greffe de conjonctif par la technique de l’enveloppe. In: Borghetti A, Monnet-Corti V (eds CdP Groupe Liasons SA). Chirurgie Plastique Parodontale. Rueil-Malmaison, France: CDP, 2000:233–241.
- Matter J. Creeping Attachment of free gingival grafts. A five year followup study. JP 1980;51:681-685
- Pini Prato GP, Baldi C, Nieri M, et al. Coronally advanced flap: The postsurgical position of the gingival margin is an important factor for achieving complete root coverage. J Periodontol 2005;76:713–722.
- Cairo F, Pagliaro U, Nieri M. Treatment of gingival recession with coronally advanced flap porcedures: A systematic review. JCP 2008; 35(suppl 8):136-162.
- Fombellida F. El pronóstico del cu- brimiento radicular en el autoinjerto de encía queratinizado. Estudio de las diferentes variables anatómicas. Periodoncia y Osteointegración 2002;12:121–132.
- Fombellida Cortázar F, Martos Molino F, Sáez Domínguez JR, Esparza Muñoz H, Goiriena de Gandarias FJ. Estudio com- parativo de la eficacia clínica de auto- injerto libre de encía en la recesión del tejido blando marginal clase III de Miller. Av Periodoncia 1996;8:147–152.
- McGuire MK, Scheyer T, Nevins M, Schupbach P. Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Purified Recombinant Human Platelet-Derived Growth Factor-BB with Beta Tricalcium Phosphate or Connective Tissue: A Histologic and Microcomputed Tomographic Examination. Int J Periodontics Restorative Dent 2009;29:7–21.
- Pini-Prato G et al. Long-Term 8-Year Outcomes of Coronally Advanced Flap for Root Coverage. JP Posted online on 20 October 2011.
- Romanos GE et al. The double lateral bridging flap for coverage of denuded root surface:Longitudinal study and clinical evaluation after 5 to 8 years. JP 1993;64:683-688
- Lehmann KM et al. A New Method for Volumetric Evaluation of Gingival Recessions: A Feasibility Study. JP Jan 2012, Vol. 83, No. 1, Pages 50-54
- Pini Prato GP, Baldi C, Nieri m et al. Coronally advanced flap: the post-surgical position of the gingival margin is an important factor for achieving complete root coverage. JP 2005;76:713-722.
- Lin GH, Chan HL and Wang HL. The Significance of Keratinized Mucosa on Implant Health: A Systematic Review. JP 2013;84:1755-1767
- Hokett SD et al. Lin GH, Chan HL and Wang HL. The Significance of Keratinized Mucosa on Implant Health: A Systematic Review. JP 2013;84:1755-1767. JP 2002; 73:334-339
- Carnio J & Camargo PM, Kenney EB. Root Resorption associated with subepithelial connective tissue graft for root coverage: clinical and histological report of a case. IJPRD 2003 Aug:23(4);391-8
- Gurgan CA et al. Alteration in Location of the Mucogingival Junction 5 years after Coronally Repositioned Flap Surgery. JP 2004;75:893-901.
- Richardson CR, Allen EP et al . Periodontal Soft Tissue Root Coverage Procedures: Practical Applications From the AAP Regeneration Workshop. Clinical Advances in Periodontics February 2015, Vol. 5, No. 1: 2-10.
- Ainamo et al. Location of the mucogingival junction 18 years after apically repositioned flap surgery. JCP 1992;19:49-52.
- Lee Y-M et al. A 3 year longitudinal evaluation of subpedicle free connective tissue graft for gingival recession coverage. JP 2002;73:1412-1418.
 Dr. Desai has been in full time specialty periodontal practice in Kamloops, BC, Canada, since 1997.
Dr. Desai has been in full time specialty periodontal practice in Kamloops, BC, Canada, since 1997.












