In recent years, measures of success in implantology have significantly changed. Due to the fact that we have assumed functionality of implants as a result of improved osseointegration parameters, the main focus now lies on aesthetic and long-term stable rehabilitation. The imitation of ‘natural’ is the biggest concern and the goal in modern implant dentistry.1 All surgical and prosthetic measures should pursue this goal. The following report describes how we try to achieve this by using a provisional restoration with a modified surgical and prosthetic protocol. The aims are: aesthetic outcome, functional long-term success achieved by a short treatment time while minimizing surgical trauma. This goal can be achieved by trying to obtain maximum control over changes in bone and gingiva. Therefore, the concept of immediate loading was applied in order to affect the maturation of the gingiva and minimize resorption of bone.2
Initial Presentation And Treatment Plan
A female patient with PFM crowns on teeth 11 and 21 presented for assessment to the Department of Periodontics at the Faculty of Dentistry, University of Toronto. Her chief complaint was the recurrent decementation of crown 11, which caused her discomfort in social situations due to the constant fear of losing the crown. The history of the chief complaint was that the crown had come off multiple times in recent months and was always recemented with no better success. The medical history was unremarkable and the patient was under regular and quality dental care. Her periodontal condition was healthy and no other restorative needs were identified. Four dental implants had been placed in Quadrant 1 and 4 but were not restored yet as the patient wanted to allot her finances to the problem she considered to be a priority. Healing was uneventful after past intra-oral surgical procedures and the patient had tolerated the procedures well. Upon clinical examination, it was discovered that the crown on tooth 11 had an open margin on the palatal aspect and the remaining clinical crown was inadequate in height to support a restoration (Figs. 1-3). Prosthodontic and endodontic consultations revealed limited predictability for alternative treatments such as forced eruption or endodontic retreatment due to the limited remaining root length and the aesthetic concerns. Therefore, after a lengthy discussion with the patient about risks and benefits of implant therapy in the aesthetic zone, the patient agreed to the following treatment plan: extraction of tooth 11 and immediate placement of a dental implant with immediate temporization. The possible need for further corrective soft tissue surgery was discussed and understood by the patient as well as the possible need for a new crown on the adjacent tooth 21.
Figure 1

Initial presentation, note the slight soft tissue discrepancy between 11 and 21.
Figure 2

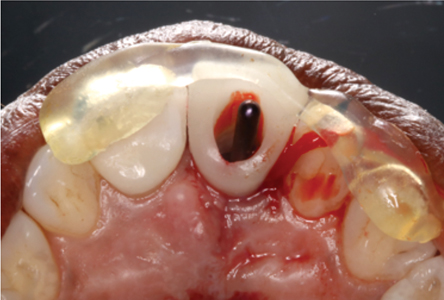
Initial presentation, note the open margin on the palatal aspect of crown 11.
Figure 3
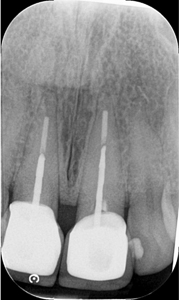
Initial periapical radiograph.
Presurgical Workflow
The clinical examination of the surgical site revealed adequate bucco-lingual and mesio-distal space for the proposed implant treatment. A minimal loss of soft tissue on the buccal aspect was noted. An alginate impression and clinical photographs were taken to document the pre-surgical situation as well as a panoramic – and a periapical radiograph. Bone sounding revealed the full presence of the buccal bone. The patient was referred to the laboratory together with her clinical records for a custom shading of the temporary restoration. The technician was advised to prepare an acrylic hollow crown for pick up on a temporary abutment matching the existing tooth in shape and dimension. A jig was created over the temporary crown in order to use it as a surgical guide and to help with the pickup.
Surgical Treatment
After obtaining a written consent and updating the medical history, the patient was prepared in the usual manner for surgery. Antibiotic prophylaxis was dispensed (2g Amoxicillin), local anaesthesia was applied and great care was taken in order to minimize the distortion of the soft tissue. The crown on tooth 11 was carefully removed, the periodontal ligament was loosened with appropriate instruments and the tooth was retrieved with forceps (Fig. 4). The jig was inserted and the implant bed was prepared (Figs. 5 & 6). In order to gain better control over the drilling direction, the Lindemann bur was used instead of the twist drill to break the palatal cortical bone in the extraction alveolus. A periapical radiograph was taken to control the direction and the implant bed was prepared to 4×15 mm.3 A platform switching implant 4/3.4 x 15 mm (Zimmer Biomet 3i, Mississauga, ON) was inserted with an initial insertion torque of 25 Ncm. The buccal gap was filled with Freeze Dried Bone Allograft (Straumann, Burlington, ON). No suture was applied but hemostasis was achieved.
Figure 4

Careful extraction of tooth 11 with minimal soft tissue trauma.
Figure 5

Direction indicator in place without jig.
Figure 6
Direction indicator and jig with temporary crown in place to control angulation and insertion axis.
Immediate Temporization
A temporary abutment cylinder (Zimmer Biomet 3i, Mississauga, ON) was inserted into the implant and the temporary crown was positioned with the jig. The temporary cylinder was marked and shortened accordingly outside of the mouth. The temporary crown was picked up with light curing composite, the jig removed and an emergence profile was formed. Contacts, occlusion and laterotrusion were carefully evaluated to obviate all potential loading to the implant. The crown was then inserted with 15N cm insertion torque and the access hole was sealed with Temp-It. The patient was instructed postoperatively regarding precautions and homecare (Figs. 7-11).
Figure 7

Temporary crown in place after removal of jig and adjustment of temporary cylinder.
Figure 8

Temporary crown prepared for pickup.
Figure 9

Final post-operative result after insertion.
Figure 10

Final post-operative result after insertion (occlusal view).
Figure 11

Post-operative radiographic control.
Post-Operative Phase And Final Restoration
One and two-week post-operative appointments showed uneventful healing with no signs of inflammation or infection. Gentle tapping on the temporary crown produced a high-pitched percussive sound and all other parameters indicated healing without complications (Fig. 12). The patient was asked to come for a pre-prosthetic check about three and a half months after surgery. On inspection, a fracture of the acrylic crown was noted, consistent with recent history of biting in a nut. There were no associated symptoms. The fracture on the palatal aspect led to a slight discrepancy in the occlusal edge of the two incisors (Figs. 13 & 14). Nonetheless, all other clinical parameters indicated successful osseointegration and the patient was referred for final restoration (Figs. 15 & 16).
Figure 12

Healing after two weeks, note the complete retention of the interdental papillae.
Figure 13

Healing after three and a half months, note the slight discrepancy in the incised edge of 11 and 21.
Figure 14

Palatal aspect of acrylic temp fractured due to occlusal forces.
Figure 15

Final restoration at insertion.
Figure 16

Radiographic control of final restoration, note the excellent periimplant bone levels.
Follow-Up and Conclusion
One year follow up shows excellent soft and hard tissue conditions around the implant 11 with even minimal creeping attachment on 21 (Fig. 17). Currently the patient was advised to monitor the area for further changes. Overall the patient is very happy with the aesthetic appearance and the treatment outcome, the short treatment time and that there was no need to wear a removable partial denture following the surgery.
Figure 17

One year follow up, note the harmonious gingival profile.
This case shows that the meticulous planning and a subsequent careful surgical approach can preserve the ‘natural’ appearance as much as possible. Nonetheless, such cases demand a highly skilled team in order to create results that please patient and clinician alike.4 OH
Oral Health welcomes this original article.
Disclosure: There are no financial interests in companies manufacturing or distributing products or services mentioned here.
Acknowledgment: The author would like to thank Mr. Al Lino, RDT (Shaw Lab Group, Toronto, ON) and Dr. Michel Kelada
(Faculty of Dentistry, University of Toronto, Toronto, ON) for their valuable contributions to this case. Also Dr. Peter Birek for his help and guidance with this manuscript.
References
- Cosyn J, Thoma DS, Hammerle CH, De Bruyn H. Esthetic assessments in implant dentistry: objective and subjective criteria for clinicians and patients. Periodontol 2000. 2017;73(1):193-202.
- Stanley M, Braga FC, Jordao BM. Immediate Loading of Single Implants in the Anterior Maxilla: A 1-Year Prospective Clinical Study on 34 Patients. Int J Dent. 2017;2017:8346496.
- Rosa AC, da Rosa JC, Dias Pereira LA, Francischone CE, Sotto-Maior BS. Guidelines for Selecting the Implant Diameter During Immediate Implant Placement of a Fresh Extraction Socket: A Case Series. The International journal of periodontics & restorative dentistry. 2016;36(3):401-7.
- Harel N, Meirowitz A, Block J, Palti A, Matalon S, Ormianer Z. Collaboration Patterns and Processes Between Dentists and Dental Laboratories When Planning and Fabricating Implant-Supported Restorations. Implant Dent. 2017;26(3):475-9.
 Dr. Hendrik Doering recently graduated from the specialty program in Periodontics at the Faculty of Dentistry, University of Toronto, Toronto, ON and is set to start working in private practice in the GTA.
Dr. Hendrik Doering recently graduated from the specialty program in Periodontics at the Faculty of Dentistry, University of Toronto, Toronto, ON and is set to start working in private practice in the GTA.
RELATED ARTICLE: Aesthetic Crown Lengthening
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












