Treatment planning for highly esthetic implant restorations can be a difficult challenge even for the most experienced implant surgeon and restorative dentist. This article will attempt to highlight many of the treatment planning considerations and the requisite conditions to create highly esthetic implant restorations.
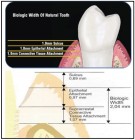
Among the most important requirements in esthetic dentistry is the presence and shape of the interdental papillae. In a recent article in the European Journal of Prosthodontics and Restorative Dentistry1, absence of interdental papillae (“black triangles”) was rated, as the third most disliked esthetic problem behind only visible anterior caries and visible anterior black crown margins. To understand how papillae get their shape and volume, we need to review the concept of the Biologic Width (BW) first described by Gargiulo, Wentz and Orban2 and later refined by Vacek3 and Choquet4 (Fig.1).5
The BW is the term used to describe the sum of the connective tissue attachment height (approximately 1.0 mm) and the epithelial attachment height (approximately 1.0 mm) around a natural tooth (averages 2.04 mm). The third component not part of the BW but related to tissue height is the gingival sulcus. A healthy sulcus measures approximately 1.0 mm midfacial and 2.0 – 3.0 mm interproximally. The sum of the BW and sulcus determines the tissue height above the osseous crest (bone). This averages 3.0 mm mid-facially and 4.5 – 5.0 mm interproximally but may vary from individual to individual and from tooth to tooth.
The extra 1.5 – 2.0 mm of tissue height interproximally is due to the interproximal contact factor and is a direct result of compression of interproximal tissue between adjacent teeth which effectively ‘squeezes’ 1.5 to 2.0 mm of tissue height beyond the midfacial height, giving rise to the 5.0 mm papillae criterion as referenced by Salama/Garber6, Tarnow7 and Choquet4. It is this interdental tissue height of 4.5 to 5.0 mm above the osseous crest that we refer to as the interdental papillae. Recently Hae-Sung Cho8 et al reviewed the effects of root on the existence of interdental papilla and found that root proximity has a direct effect on the presence of papilla.
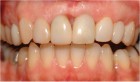
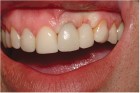
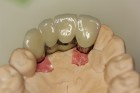
Manipulating this interproximal tissue with the restoration is the strategy behind papillae development and maintenance. Simply put, the fuller the interproximal tooth/restoration contour the more incisal and pointed the papilla will be, and the thinner the interproximal tooth/restoration contour, the more apical and blunted the papilla will be9. If the papilla is non-
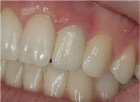
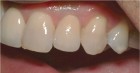
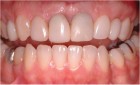
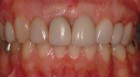
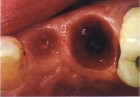
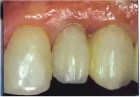
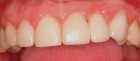
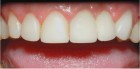
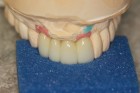
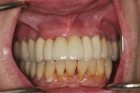
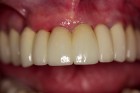
epithelialized during healing, the contour is too full (Fig. 2). If the papilla is healthy but blunted during healing, the contour is too thin (Fig 3.). The ideal interproximal profile places the free gingival margin at the desired location and produces a pointed papilla that is inflammation free10 (Figs. 4, 5 & 6).
When ideal hard and soft tissue conditions exist the papilla will spontaneously develop without intervention (Figs. 7-12).
There is a limit however, to the amount of tissue that can be supported between two adjacent teeth, (or two implants, two pontics or any combination thereof).4 According to Salama/Garber the maximum amount of tissue height that can be augmented between two adjacent implants is only 3.5 mm.2 Where does this magic number come from and why is it less than the 5.0 mm quoted around natural teeth? The answer lies in the BW location around an implant compared to a natural tooth. In the case of a natural tooth the BW is supra-crestal but around implants it is sub-crestal.
Since the BW is approximately 2.0 mm sub-crestal on an implant, the resultant tissue height will also be 2.0 mm apical compared to that of a natural where the BW is supra-crestal. This explains the 3.5 mm maximum papillae height around adjacent implants and a 4.5 – 5.0 mm papillae height around adjacent natural teeth.
This is significant since both hard and soft tissue tend to resorb immediately after extractions.10-13 Without careful planning and controlling for this resorption during the healing stages, papillae will blunt resulting in the dreaded ‘black triangles’. This is compounded when managing the healing around multiple adjacent extractions.
This information is essential when trying to create esthetic restorations predictably when there are multiple missing adjacent teeth. Garber and Salama compared the amount of soft tissue that can be AUGMENTED above the bony housing between teeth, pontics, implants and every combination thereof.6 Their results demonstrated that it was possible to augment tissue 6.5 mm around a tooth adjacent to a pontic, 5.5 mm around an implant adjacent to a pontic, 6.0 mm around two adjacent pontics, 4.5 mm around a tooth adjacent to an implant, 5.0 mm around a two adjacent teeth, but only 3.5 mm around two adjacent implants (because of the sub-crestal nature of the BW around implants as discussed above).
Knowing that we can support 5.5 mm between an implant and a pontic and only 3.5 mm between two adjacent implants, it follows that we can create better papilla form (shape and height) and therefore better esthetics around an implant adjacent to a pontic than we can around two adjacent implants. In fact as a general rule, never place implants side by side if you can avoid it.
Consider the following case:14
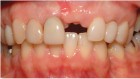
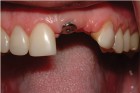
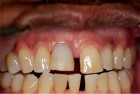
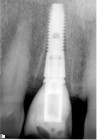
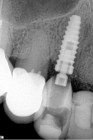
Saad A et al Nonsurgical management of interdental papilla associated with multiple maxillary implants. Journal Prosth, 2005; 93: 212-215. The patient had received two adjacent implants in the #22 and #23 position. Predictably the final result was an esthetic failure. Maximum tissue height between two implants is only 3.5 mm. Result was predictably an esthetic failure.
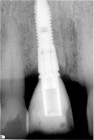
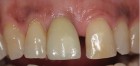
The patient had received two adjacent implants in the #22 and #23 position. Predictably the final result was an esthetic failure. Why? Firstly, interdental bone requires blood supply and adjacent implants compromise blood supply.13 Secondly, the BW; that minimum amount of soft tissue (vertical and horizontal) whose primary function is to insulate the underlying bone both, from the outside environment is sub-crestal around implants, reducing the ultimate height of the papilla. Bone will be lost in both dimensions until this criterion is met.11,12,13,15,16 The author recognized this and buried the #22 implant to create a pontic instead and allow soft tissue to granulate into the site as a means of BW enhancement (increased insulation) around the remaining exposed implant.
The final result was a marked improvement over the initial result.
A better option when confronting adjacent missing teeth in the esthetic zone is to alternate between implant and pontic. The maximum tissue height here is potentially 5.5 mm similar to adjacent natural teeth4 (Figs. 18, 19, 20-25).
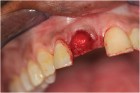
When it is necessary to extract a tooth in the esthetic zone, immediate implant placement and delayed implant placement options exist. Immediate implant placement provides for shorter treatment time and improved patient acceptance (one surgery versus two) but the risks are significant and include increased risk of perforation, bone loss, or failure of osseointegration and loss of implant. However, when ideal conditions do exist, it may be more desirable and more predictable to place implant immediately after extraction.16, 19,20,21,22,23,24. Ideal conditions exist when soft tissue and hard tissue, (both labial and palatal), are present after extraction. The implants should be placed slightly palatal; implants in a more labial position are more prone to resorb the labial plate.17 Ideally 2.0 mm of bone labial is necessary to prevent recession.17 Moreover, when primary stability of implant is possible (50 Ncm), and when the restoration can be kept out of function the implant should be immediately be restored with provisional. The immediate provisional restoration should be screw retained and not removed for six weeks.18
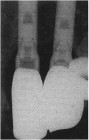
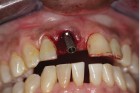
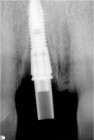
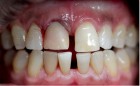
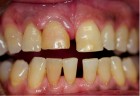
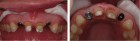
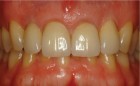
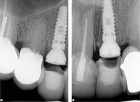
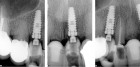
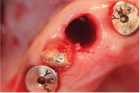
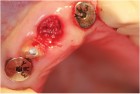
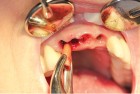
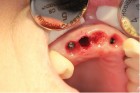
The next case demonstrates the steps taken in the treatment of a failing right maxillary central incisor with an immediate implant and immediate provisional. All options were discussed with patient prior to treatment. (Note the 12-month post extraction response of the bone around the implant).
The next case demonstrates extraction of #52 and 62, immediate implant and delayed provisional.
Patient was referred for implants to replace missing #12 and 22 (Figs. 37, 38). The margins of pre-existing crowns revealed unesthetic short clinical crown lengths, (Figs. 40, 41). Pre-op length-width ratios were almost 1:1 instead of a more desirable 1.6:1.0 ratio. With proper treatment planning, it was agreed that crown-lengthening procedures simultaneous with implant placement would achieve a more esthetic final result, (Figs. 42, 43).
The last case will demonstrate how to apply the above concepts to restore a patient back to her original condition after Xerostomia and caries ravaged her natural anterior crown restorations.
Patient presented for loose front left central incisor. Examination revealed drug-induced Xerostomia, moderate to severe caries in teeth #13, 12, 11 and 21 (Figs. 44, 45). Treatment option included attempts to salvage teeth with root canal therapy, crown lengthening procedures and new post core and crown restorations. This option would involve either orthodontic forced eruption procedures or esthetic mutilation of free gingival tissues. Prognosis would still carry high risk for future caries, (Xerostomia) and create poor esthetics or permanent BW violations and inflamed unesthetic crown margins.
Option 2 would involve extraction of #13, 12, 11 and 21 and placement of only two implants. The use of four implants would create serious esthetic complications, including poor papillae form, potential for significant bone loss and difficulties with provisionalization. Furthermore would be almost twice the cost to the patient! Knowing that we can support more tissue around an implant adjacent to a pontic we proposed the following. Extract #13, and 21 with immediately implants in those sites.
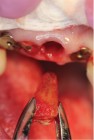
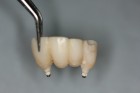
Use #12 and 11 as abutments for metal reinforced cantilevered provisional (Figs. 46 and 47). After allowing six months for healing, transition provisional from tooth supported to implant supported, extract #21 and graft socket with non-resorbable biomaterial (Bio Oss) and develop ovate form for future pontic (Figs. 48, 49 & 50-56). It was decided to delay extraction of #12 for two months to allow soft tissue healing and restore blood supply to region and minimize risk of tissue collapse during the healing of the adjacent sockets. Tooth #12 was extracted two months later and grafted with non-resorbable biomaterial (Bio Oss, Fig. 57).
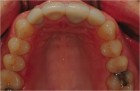
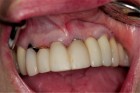
After two additional months of healing, the provisional was removed and impressions taken for final restoration. (Lab work up, final restoration and insert shown below).OH
To see images for this article, please view below references.
Dr. Dr. Domenic Belcastro; BSc, Biochemistry University of Toronto, 1982. DDS University of Toronto, 1986. MSc Department of Oral and Maxillofacial Implant Surgery at Lille University Medical School, France 2010. Associate Clinical Director University of Toronto Mini Residency Cosmetic Dentistry for General Practitioner. Clinical Instructor at The University of Toronto Department of Restorative Dentistry 2012 – 2014. Served on the committee of the RCDSO PLP program. He is an alumnus of the Pankey Institute (Key Biscayne FL.) and author of several scientific articles. Dr. Belcastro has lectured in Canada, the US and UK. He is a member in good standing with numerous academies and associations and maintains a private practice in Toronto, Canada.
Oral Health welcomes this original article.
References:
1. Patients’ Ranking of Interdental “Black Triangles” Against other common aesthetic problems Eu J Prosth and Rest Dent Dec 2009
2. Gargiulo, Wentz, Orban, J. periodontal 1961; 32: 261-267. Dimensions and relations of the dento-gingival junction in humans.
3. Vacek J.S. et al, Intl Journal of Prosthodontics and Restorative Dentistry, Vol. 14, #2, 1994
4. Choquet V, et al J. Perio. 2001; 72: 1364-71.
5. Biologic Width IJDA 2, (4) October – December 2010: 338
6. Salama/Garber et al, Practical Periodontics Aesthetic Dentistry 1998: 10: 1131-1141
7. Tarnow, D. P., et al J Clin Perio 1992: Dec 63 (12): 995-60).
8. Hae-Sung Cho et al J Perio. Oct. 2006; 77: 1651-1657.
9. Kois JC Periodontology 2000, 1996; 11:29-38. The restorative-periodontal interface: Biologic parameters.
10. Chen et al 2009 J Perio and Botticelli J Clin Perio. 2004 Oct. 31(10): 820-8.
11. Schroppe et al J Perio Rest 2003
12. Canula and Maeda Int J Oral Maxillofacial Implants. 2013 Jan-Feb; 28(1): 143-7.
13. De Rouck JOMI 2008 23: 897-904
14. Saad A et al Journal Prosth, 2005; 93: 212-215
15. Evans CD and Chan ST Clin Oral Implants Res. 2008 Jan;19(1):73-80. E pub 2007 Oct 22
16. Glauser R et al 2004, JOMI
17. Sennerby et al 1988 J Clin Perio
18. Wennstrom 2005 J Clin Perio
19. Botticelli et al 2004 J Clin Periodontol. 2008 Clin Oral Implants
20. Sanz et al Clin Oral Implants Res. 2012
21. Van der Welds 2008
22. Paoloantonini J Craniofacial Surg. 2013 May; 24(3): 841-4
23. Van Brakel Clin Oral Impl 2011
24. Tarnow et al: Comp CE Dent. 2012 Jul-Aug; 33(7): 524-32, 534 Dual zone therapeutic concept of managing immediate implant placement and provisional in anterior extraction sockets.