To view figures, click on figure mentions throughout the article.
Your patient in the chair has confirmed that their lips and tongue are numb from your block local anesthesia. As you are beginning to start the clinical procedure, your patient jumps to report that you are hurting them and they still feel pain. Feeling apologetic, you provide additional local anesthesia hoping that the patient will become more comfortable. You are feeling an increased amount of pressure as you are uncertain as to whether you have sufficiently provided profound anesthesia that will last throughout the dental procedure. If you recognize this experience, or have had this happen to you, you are not alone. Unfortunately, this happens to clinicians from time to time.
A common reason that patients report not enjoying dental visits is that they fear pain during procedures (Table 1). Studies have shown that that the conventional Inferior Alveolar Nerve Block may be missed or ineffective 15-54% of the time. There are multiple reasons why patients experience pain during dental procedures after being reported numb. For instance, numbing patients who have active infections can be difficult. The site of an active infection is acidic, which can deactivate local anesthetics that function best in a slightly basic environment. Additionally, anatomical variability may contribute to missed mandibular blocks. Mandibular molars have been reported innervated by up to four different nerves which means that a conventional block may be present, inhibiting the ability to provide profound anesthesia (Table 2).
Table 1
Top Reasons Patients don’t like going to the Dentist
1) They don’t like the pain during or after the clinical procedures
2) They worry about being lectured or made to feel guilty of oral health neglect
3) They worry about the unexpected expenses
4) They are too busy and don’t value oral health care
5) They dislike waiting and anxious about the procedure
6) They worry about the bad news or discovery of a serious underlying problem
7) They had a bad painful past experience at the previous dentist
8) They dislike the sounds and smells at the dental office
Table 2
Possible reasons why patients are hurting during dentistry when they are already numb
1) Patients present with a site with acute active infection
2) Patients moved during the injection which resulted in deposit of local anesthetics away from the nerve trunks
3) Vasoconstrictors were not used within the local anesthetics which resulted in shorter duration and possible decreased numbness
4) Anatomical variability from conventional text book positions
As clinicians, our ideal local anesthesia should be Painless, Predictable, Profound, Precise, Immediate and without collateral numbness. Furthermore, the parameters described above may be possible through utilizing the intraosseous local anesthesia techniques. The intraosseous injection allows placement of a local anesthetic solution directly into the cancellous bone adjacent to the tooth of interest. There are a few intraosseous systems available on the market; the Stabident, X-tip, IntraFlow and Quick Sleeper 5.
The Stabident system is comprised of a slow speed handpick driven perforator, which is a solid 27-gauge wire with a beveled end that when activated, drills a small hole through the cortical plate. The anesthetic solution is then delivered to the cancellous bone through the 27-gauge ultra-short injector needle and placed into the hole made by the perforator. It is important to note the precise locations of the perforated holes that will engage the 27-gauge needle.
The X-tip anesthesia delivery system consists of an X-tip that separates into two parts; the drill and guide sleeve component. The drill leads the guide sleeve through the cortical plate whereupon it is separated and withdrawn. Therefore, the guide sleeve provides the exact location of the perforation and injection site into the cancellous bone. The remaining guide sleeve is removed after the intraosseous injection is compete.
The QuickSleeper 5 is an electronic pen that efficiently and comfortably performs the intraosseous dental anesthesia (Fig. 1: QuickSleeper 5.). Since this intraosseous anesthesia technique aims for the apices of the teeth to be treated, profound and immediate anesthesia can be predictability achieved. The electronically controlled injection rate provides maximal comfort for patients. The QuickSleeper 5 has three injection modes for slow, fast and intraosseous rate of flow of local anesthetics. Additionally, needles can be rotated using a foot pedal, enabling easy penetration of the cortical plate to simply and quickly access osteocentral anesthesia. The patented double bevel needle ensures painless anesthesia of the attached soft tissues and easy cortical perforation (Fig. 2: QuickSleeper 5 patented double bevel needle.). There are three steps to perform the osteocentral/transcortical anesthesia. Step 1 involves attached gum anesthesia with the double bevel needle. Step 2 involves perforation of the cortical plate and subsequent penetration into the cancellous bone to the appropriate depth. Step 3 involves injection into the cancellous bone and needle withdrawal.
Fig. 1
QuickSleeper 5.
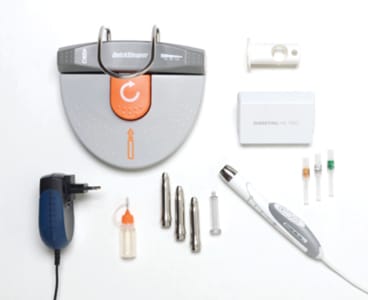
Fig. 2
QuickSleeper 5 patented double bevel needle.

The diffusion of local anesthetics in the maxilla moves distally and medially. When choosing the injection site for the maxillary arch, the point selection aims to provide the easiest access and operator position. The mandible diffusion is mainly mesial direction. Therefore, when choosing the injection point for the mandibular arch, we aim for the point distal to the tooth to be treated, especially for the teeth devoid of pulp circulation or inflammatory tissues. For asymptomatic teeth, mesial intraosseous injection will also provide sufficient local anesthesia for the tooth just distal of the injection site.
The principle of intraosseous anesthesia consists of placing the anesthetic solution directly into the cancellous bone adjacent to the apices of the roots or anatomy. The number of teeth, length of duration, and effectiveness depends on several factors. The site of interest with volume of bone dictates the volume of local anesthetic required. The local anesthetic product with higher concentration of vasoconstrictor will yield more effective and longer lasting anesthesia. Finally, the quantity of anesthetic injected should be adapted to the volume of cancellous bone to the number of teeth to anesthetize and the length of the procedure with required. These factors will usually result in anesthetizing two to eight teeth, with one cartridge having a lasting effect of 45-60 minutes.
There are some contraindications and limitations to using intraosseous local anesthetic techniques. Access to maxillary wisdom teeth may be limited. Thus, conventional infiltration anesthesia is indicated. Additionally, sites where the bone may be infected or when there is very small interdental space between the roots, it may be difficult to locate perforation points. Therefore, choosing a distal site to the affected area or perform another conventional technique may be indicated. As with any new technical advances, using intraosseous local anesthetic techniques will require a minor learning curve. Once practiced and experienced, the adjunctive intraosseous local anesthetic offers an invaluable pain free experience for our patients and practice.
Clinical procedures and applications to be used with intra-osseous local anesthetic techniques can range from restorative, endodontics, cosmetic, pedodontics, prosthodontics, oral
surgery and implantology (Table 3).
Table 3
Clinical Applications with Intraosseous Local Anesthetic Techniques
1) Basic restorative procedures without collateral numbness to lip and tongue
2) Pedodontics
3) Endodontics
4) Prosthodontics, crown and bridge preparations
5) Anterior cosmetic procedures without collateral lip numbness
6) Implantology for osteotomy preparations
7) Extractions
At the time of publication, the author of this article will have been using the QuickSleeper 5 for over six months. Several procedures have been performed using this electronic pen including procedures done on dental professionals, hygienists, dentists, and patients, resulting in a great deal of positive feedback. Dentists are often as nervous as the average patient and they know exactly what is being done, so having them in the chair and hearing their feedback elevates the standard. The feedback was very positive from dental professionals as they reported profound, painless anesthesia with no collateral soft tissue numbness.
In conclusion, intraosseous local anesthesia should be revisited by all clinicians to be implemented as a supplemental technique to provide, immediate, profound, painless and precise delivery of local anesthetics. Any new technology or techniques that decreases pain for our patients and improves our reputation for delivering comfortable dentistry should be evaluated for its validity.
For further information regarding the QuickSleeper 5, the readers can contact: 1-877-237-3233 and www.rwrdentalcom. OH
Oral Health welcomes this original article.
Disclaimer
Dr. Mark Lin is an instructor and key opinion leader for the QuickSleeper 5 unit.
About the Author
 Dr. Mark H. E. Lin graduated from the University of Detroit Mercy for his dental program. He them completed a one-year General Practice Residency program at the Miami Valley Hospital in Dayton, Ohio. He practiced general dentistry for 13 years and then returned to complete his post-graduate training in the specialty of prosthodontics at the University of Toronto. He maintains a full-time specialty practice as a prosthodontist at Dr. Mark Lin Prosthodontic Centre.
Dr. Mark H. E. Lin graduated from the University of Detroit Mercy for his dental program. He them completed a one-year General Practice Residency program at the Miami Valley Hospital in Dayton, Ohio. He practiced general dentistry for 13 years and then returned to complete his post-graduate training in the specialty of prosthodontics at the University of Toronto. He maintains a full-time specialty practice as a prosthodontist at Dr. Mark Lin Prosthodontic Centre.













