Despite numerous advances in dentistry over the past few decades, dental caries remains one of the most widespread diseases worldwide.1 Children from lower socio-economic classes or those with special needs are often affected and generally lack access to conventional restorative dental care.2 The caries management ideology has thus shifted from typical restorative treatment to arresting dental decay using fluoride therapies to provide more inclusive care. Silver diamine fluoride (SDF) has recently gained significant popularity in the dental community after being approved for use by Health Canada in 2017 as a dental sensitivity agent under the name Advantage Arrest (Fig. 1). Due to its new introduction, dental practitioners should be informed regarding its clinical efficacy, indications, benefits and risks prior to routinely implementing it as a viable treatment option in their offices.
Figure 1
SDF 38% bottle and applicator, marketed as Advantage Arrest.
Clinical studies have shown that 38% SDF can arrest dental caries and halt further progression of the disease whereby applying it once annually arrests 65.9% of dentin carious lesions.2,3 The silver component provides an anti-bacterial effect while the fluoride promotes remineralization of tooth structure. More specifically, several studies have confirmed that 38% SDF inhibits cariogenic biofilm formation and prevents further tooth demineralization.3-5 In addition, this product has been shown to protect against dentin collagen destruction by suppressing matrix metalloproteinases and cysteine cathepsins.6 Although its mechanism of action has been well researched, there has been much debate with regards to the optimal concentration of SDF to be used. Fung et al. found that the chances of arresting active dental decay significantly increased with 38% SDF compared to 12% SDF, and if the treatment was applied biannually rather than once a year.7
Using this information, dental clinicians must be able to evaluate which patients will benefit from SDF treatment and provide it only when indicated. This treatment has been recommended for high caries-risk patients and for those with behavioural and/or medical challenges.8 Many of these patients can only receive traditional dental treatment under general anesthesia, some of which are ineligible for sedation due to their medical complexity. Furthermore, patients presenting with a large number of carious lesions that cannot otherwise be treated in one visit can benefit from SDF application to halt the carious process until treatment can be provided over multiple appointments. Contraindications include an allergy to silver and gingival stomatitis as mucosal staining is possible if the epithelial layer is compromised.9
Since dentists started to incorporate SDF in their practices, practical strategies have been investigated to create an efficient and optimized clinical protocol for its application. So far, the consensus is to use standard universal precautions, isolate and dry the affected tooth and place one drop of 38% SDF on the carious lesion using a microbrush.8 Allow the SDF to be absorbed for one minute and remove the excess with gauze or cotton rolls to reduce systemic absorption. All equipment that comes into contact with SDF should be carefully disposed of in a plastic waste bag, as it will stain items black. It is also recommended that the patient does not eat or drink for thirty to sixty minutes following application for best results, which most patients should be accustomed to with typical in-office fluoride treatment9. It is well known that SDF must be re-applied to sustain caries arrest as 50% of lesions that received a one-time application became active once again within 24 months.10 Studies have shown that applying SDF three times per year demonstrated higher caries arrest rates compared to twice or once per year.11 Further investigations are required to establish an ideal protocol, outlining proper re-application intervals and standardizing the methodology.
Although SDF has been clinically proven to arrest dental caries, dental practitioners must understand and communicate all benefits and risks to their patients prior to its use. It represents a quick, non-invasive and painless procedure in which local anesthetic is not required. Studies have confirmed that no pulp damage is caused by SDF, but that it should not be used on teeth with exposed pulps12. In addition, its low cost and simple application make it an attractive option for both the dentist and patient. However, there are a few risks and disadvantages to using SDF. Firstly, the classic presentation of SDF after application is dark black staining of the affected teeth (Figs. 2 & 3), which is permanent unless restored with glass ionomer or composite resin.9 There are also reports of temporary dark staining of any contacted skin, typically resolving within 2 to 14 days.8 Moreover, patients complain of a metallic or bitter taste after application, which typically dissipates soon after.2
Figure 2

Primary teeth with carious lesions before 38% SDF application.14
Figure 3
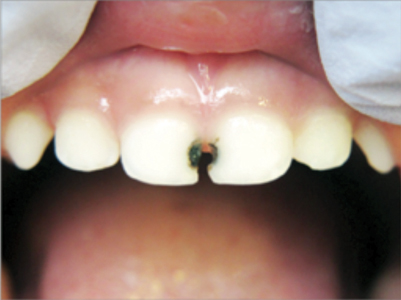
Primary teeth after 38% SDF application.14
As with any other dental procedure, the parents of the child must weigh the benefits and risks of this treatment option in order to provide informed consent prior to proceeding. A recent study by Crystal et al. investigated parental acceptance of SDF in relation to its esthetic concerns. They found that parents were more agreeable to the dark staining in posterior teeth compared to anterior teeth.13 When questioned regarding choosing SDF on anterior teeth versus general anesthesia for comprehensive dental treatment, the majority of parents preferred SDF.13 Dental clinicians should therefore be cognizant of these parental perceptions towards SDF treatment and plan the caries management of the child accordingly.
In conclusion, the current scientific literature suggests that 38% SDF applied two or three times per year is effective in arresting active carious lesions. It can be used for high caries-risk patients to arrest decay and prevent serious infection until traditional restorative treatment can be completed. Furthermore, for medically compromised patients or those with special needs, SDF should be considered in situations where restorative treatment cannot be safely managed in the dental chair and when general anesthesia is contraindicated. However, further research is needed to establish if and when formal restorative treatment should be undertaken to remove the carious lesion. Studies with long-term follow-up should also be initiated to determine survival rate of treated teeth and presence of recurrent decay despite re-application. Although there are still unanswered questions with regards to its long-term application, SDF can provide a feasible option to dental clinicians when tailoring caries management plans. This is especially true for children with complex medical conditions and special needs, as they are more vulnerable to serious consequences of untreated caries. OH
Oral Health welcomes this original article.
References
- Frencken JE, Sharma P, Stenhouse L, Green D, Laverty D, Dietrich T. Global epidemiology of dental caries and severe periodontitis–a comprehensive review. J Clin Periodontol. 2017;44 Suppl 18:S94-S105.
- Chu CH, Lo EC. Promoting caries arrest in children with silver diamine fluoride: A review. Oral Health Prev Dent. 2008;6(4):315-321.
- Gao SS, Zhang S, Mei ML, Lo EC, Chu CH. Caries remineralisation and arresting effect in children by professionally applied fluoride treatment–a systematic review. BMC Oral Health. 2016;16:12-016-0171-6.
- Mei ML, Li QL, Chu CH, Lo EC, Samaranayake LP. Antibacterial effects of silver diamine fluoride on multi-species cariogenic biofilm on caries. Ann Clin Microbiol Antimicrob. 2013;12:4-0711-12-4.
- Mei ML, Chu CH, Low KH, Che CM, Lo EC. Caries arresting effect of silver diamine fluoride on dentine carious lesion with S. mutans and L. acidophilus dual-species cariogenic biofilm. Med Oral Patol Oral Cir Bucal. 2013;18(6):e824-31.
- Zhao IS, Gao SS, Hiraishi N, et al. Mechanisms of silver diamine fluoride on arresting caries: A literature review. Int Dent J. 2017.
- Fung MHT, Duangthip D, Wong MCM, Lo ECM, Chu CH. Arresting dentine caries with different concentration and periodicity of silver diamine fluoride. JDR Clin Trans Res. 2016;1(2):143-152.
- Horst JA, Ellenikiotis H, Milgrom PL. UCSF protocol for caries arrest using silver diamine fluoride: Rationale, indications and consent. J Calif Dent Assoc. 2016;44(1):16-28.
- Crystal YO, Marghalani AA, Ureles SD, et al. Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent. 2017;39(5):135-145.
- Yee R, Holmgren C, Mulder J, Lama D, Walker D, van Palenstein Helderman W. Efficacy of silver diamine fluoride for arresting caries treatment. J Dent Res. 2009;88(7):644-647.
- Duangthip D, Chu CH, Lo EC. A randomized clinical trial on
arresting dentine caries in preschool children by topical fluorides – 18 month results. J Dent. 2016;44:57-63. - Korwar A, Sharma S, Logani A, Shah N. Pulp response to high fluoride releasing glass ionomer, silver diamine fluoride, and calcium hydroxide used for indirect pulp treatment: An in-vivo comparative study. Contemp Clin Dent. 2015;6(3):288-292.
- Crystal YO, Janal MN, Hamilton DS, Niederman R. Parental perceptions and acceptance of silver diamine fluoride staining. J Am Dent Assoc. 2017;148(7):510-518.e4.
- Nelson T, Scott JM, Crystal YO, Berg JH, Milgrom P. Silver diamine fluoride in pediatric dentistry training programs: Survey of graduate program directors. Pediatr Dent. 2016;38(3):212-217.
 Dr. William Nicola is a dental resident in the Department of Dentistry at Hospital for Sick Children in Toronto, Ontario.
Dr. William Nicola is a dental resident in the Department of Dentistry at Hospital for Sick Children in Toronto, Ontario.
RELATED ARTICLE: Clinical Uses for Silver Diamine Fluoride
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












