The concept of using amputation to treat an infectious disease was last used by the medical profession to treat gangrene in the late 1800s.
The pharmacological management of dental caries aims to leave most caries in situ, killing the bacteria and enabling infected dentin to heal as arrested caries. A way of achieving this is by the use of Silver Diamine Fluoride (SDF) that has been available to dentists for over 50 years. Whilst SDF it is currently receiving a resurgence in interest, this procedure has never gained real traction in general dentistry, due to the staining associated with it.
Riva Star (SDI, Australia) combines the application of SDF followed by potassium iodide (KI) to dental caries that prevents staining by scavenging free silver ions. This prevents silver fluocculation (clumping) onto dentin and forms silver iodide, a creamy white precipitate. Figure 1 shows the difference between two self-cure glass ionomer cement (GIC) restorations treated with SDF and Riva Star stored in water for 6 weeks in direct sunlight.
As with any dental procedure, an established protocol exists to maximize the benefits of this technique. This will prevent staining that can occur if established protocols are not closely followed.
Fig. 1

Mechanism of Caries Management
Electron probe micro analysis (EPMA) shows that it is the fluoride and not silver that penetrates deeply into demineralized dentin (Fig. 2).
Silver and iodine do not penetrate more than 100 microns beneath the surface of the lesion, and while this may provide a lethal barrier against further bacterial infection, it is the fluoride ions that pass deeply into demineralized dentin at maximum concentrations of almost two percent (10,000 ppm), well beyond the lethal dose of 2000 ppm required to kill strep mutans bacteria.
After application of the SDF/KI, best outcomes are achieved by placing a self-cure glass ionomer cement over the cavity to seal the lesion from the external environment. This enables remineralization of the caries to occur and prevents incorporation of sulphur ions from the saliva that will stain the remineralizing caries. (All sulphur salts are black).
In an asymptomatic carious lesion, calcium and phosphate ions from the odontoblastic processes combine with fluoride from SDF and strontium and fluoride ions from the GIC to form a caries resistant base beneath the GIC. Infected dentin will form as fluoride rich arrested caries as the collagen matrix within the dentin has been destroyed. Affected caries, with an intact collagen matrix will form as a fluoride enhanced fluorapatite. Figure 3 shows a previously carious lesion three years after treatment with Riva Star and GIC. The GIC restoration has been removed showing a hard base of unstained arrested caries beneath.
Fig. 2

Fig. 3

Treatment Protocol
Riva Star is suitable for application to any asymptomatic carious lesion in both deciduous and permanent teeth. If used in conjunction with a self-cure GIC (providing the correct treatment protocol is followed), it will arrest caries and assist with the remineralization of the lesion to become a caries resistant base under the restoration. Applied correctly, it will neither stain surrounding tooth structures or the restoration.
As a precaution however, clinicians are advised to avoid restorations within the aesthetic zone until they have mastered this treatment protocol.
The higher the pH of an SDF solution the further it may penetrate into carious dentin and precipitate out more dissolved tooth mineral within the caries. Application of KI to the SDF reduces the pH in the dentinal tubules to around pH 9.
Caries Access
Accessing caries is required, especially proximally, for the correct application of Riva Star. Depending upon patient compliance, local anaesthetic is usually unnecessary. Occlusal caries requires minimal tooth removal. Proximal caries may require using an ultra conservative “tunnel preparation” for permanent teeth or for deciduous teeth, a small proximal slot preparation.
Surface Preparation
Once access has been achieved, prepare the surface by first removing any loose grossly carious dentin, followed by a 15 second etch with 37% phosphoric acid. Rinse and dry the preparation.
A 15 second etching time removes debris from the cavity surface and most importantly removes bio-load within the non-vital dentinal tubules to facilitate penetration of the Riva Star deeply into the caries. Figure 4 compares two demineralized dentin surfaces treated with Riva Star. The polyacrylic acid, conditioner, treated surface does not facilitate penetration of Riva Star whereas the etched surface enables Riva Star to penetrate deeply into the demineralized dentin.
Figure 5 compares the difference between two samples of light activated carious teeth, previously treated with Riva Star. One sample was etched for 15 seconds, the other sample unetched. The etched sample shows no sign of SDF staining whereas the unetched sample is heavily stained on both the enamel and dentin. This may be due to the strong organic bonds between AgI and collagen protein that is exposed on the etched surfaces and resists breakdown of the AgI to free silver ions when subjected to the intensity of the curing light. On the non-etched surfaces where these bonds are absent, staining occurs.
Fig. 4

Fig. 5

Riva Star Application
Any clinician who has used SDF from a multiple dose bottle will be aware of the problems of staining on operatory surfaces associated with this delivery system. Furthermore, ammonia continually leaks from the container every time the cap is removed reducing the clinical effectiveness of the SDF.
A single dose delivery system reduces cross contamination, and minimizes staining of operatory surfaces.
Clinical Steps to Riva Star
- Isolate the preparation
- Etch the preparation for 15 seconds, wash and dry
- Take the SDF (grey) vial and break the seal with the hard end of the brush applicator
- Apply the SDF with the brush over the caries
- Immediately following this, similarly apply the KI (green) vial over the SDF
- A white precipitate will appear
- Continue applying the KI solution until the white precipitate completely disappears
- Wash away the reactant with water and dry the preparation
This will remove free silver ions and any residual AgI that may break down and potentially stain the surface. Remaining AgI, seen as a white film on the caries, is bound to collagen protein that is extremely stable and unlikely to break down over time (Fig. 6).
Fig. 6

GIC and Composite Placement
A self-cure GIC restoration is indicated immediately after SDF/KI treatment. If the restoration encroaches upon undermined cusps in the tooth or has a large load bearing area, a GIC and composite resin “co-cure” sandwich restoration is indicated. See *.
Clinical Cases
Three clinical cases are shown that demonstrate the healing effects of Riva Star on large asymptomatic carious lesions.
Case Study 1
This patient presented seeking a second opinion to a treatment plan involving the extraction of a carious asymptomatic upper right second molar and replacing it with a dental implant.
Minimal access “tunnel” cavities, without local anaesthesia, were prepared on the mesial of the second molar and distal of the first molar. The preparations were etched for 15 seconds washed and dried. SDF was applied immediately followed by KI until the reactant went clear. The cavities were washed and dried and proximal matrices applied and wedged. Self-cure GIC restorations were placed into each cavity.
Figure 7 shows a radiograph of several large asymptomatic carious lesions prior to treatment. Figure 8 shows a radiograph immediately after placement of Riva Star and self-cure glass ionomer cement, Riva SC (SDI, Australia). The increase in radiopacity was caused by the precipitation of tooth mineral within the carious lesion due to the initial high pH of Riva Star.
Six weeks later the patient returned to have the remaining cavities restored. Photograph of the restorations (Fig. 9) shows no sign of staining and a radiograph (Fig. 10) shows a further increase in radiopacity beneath the restoration.
Fig. 7

Fig. 8

Fig. 9
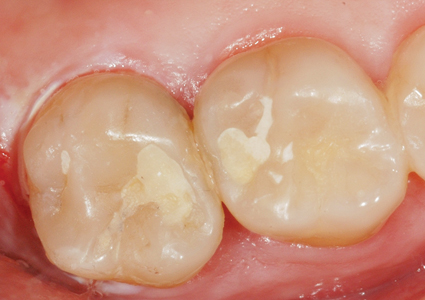
Fig. 10

Case Study 2
This patient presented with a large asymptomatic carious lesion beneath a failed composite resin restoration (Fig. 11).
The composite was removed followed by minimal caries excavation. The preparation was etched for 15 seconds, washed and dried. SDF was applied followed by KI until the reactant cleared. The cavity was then washed and dried.
Following placement of a proximal matrix, a co-cured restoration was placed over the treated surface consisting of a self-cure GIC and composite resin, with Riva Bond at the interface. After occlusal adjustment, the restoration was contoured and polished. A radiograph taken immediately following placement of Riva Star and the restoration shows a marked increase in radiopacity of the caries beneath the restoration (Fig. 12).
The patient was recalled one week later and a further radiograph taken, showing continuing increase in radiopacity (Fig. 13).
Fig. 11

Fig. 12

Fig. 13

Case Study 3
Shows a large asymptomatic carious lesion beneath a failed composite resin restoration (Fig. 14).
The restoration was removed, and following minimal caries excavation, the lesion was etched for 15 seconds followed by Riva Star placement as prescribed and a GIC/ composite resin sandwich (co-cured) restoration placed. An immediate post placement radiograph (Fig. 15) shows a substantial improvement in radiopacity of the remaining caries. A four-week follow up shows no staining of the surrounding tooth structure or restoration (Fig. 16) and a radiograph demonstrates a further increase of radiopacity of the carious dentin (Fig. 17).
Fig. 14

Fig. 15

Fig. 16

Fig. 17

Conclusions
The pharmacological management of dental caries is a new era in the science of restorative dentistry. Patients can expect significant reduction in the time and discomfort associated with a dental visit. Dentists who engage in pharmacological caries management and use biomimetic restorative materials that assist the tooth’s own ability to heal, see dramatic improvements in clinical efficiency and patient acceptance of care.
*The Co-Cure Technique
Back in the 70s, John Mclean (early GIC researcher) was advocating “sandwich restorations”, replacing dentin with biomimetic GIC, and enamel with strong and aesthetic composite resin. The problem was the weak bond between self-cure GIC and composite, about 2.5 MPa. This predisposed the restoration to adhesive failure at the interface between these two materials. The use of Riva Bond LC (SDI, Australia) or Fuji Bond LC (GC Corp, Japan) both RMGIC bonding agents enables higher bond strengths between the GIC and composite resin, equivalent to the cohesive failure of a self-cure GIC, about 7 MPa.
The co-cure technique requires the placement of Riva Bond LC or Fuji Bond LC onto the surface of a self-cure GIC either prior to setting or immediately after the first set of the GIC. This enables a chemical bond between the self-cure GIC and composite to form upon photo initiation of the composite resin. OH
Oral Health welcomes this original article.
Disclaimer
The author is a clinical evaluator for, and non-executive director of SDI.
About the Author
 Geoff Knight is a general dentist from Melbourne, Australia with interests in aesthetic and minimal intervention dentistry. He has introduced a number of innovative clinical techniques and is named on several dental patents. Dr. Knight speaks internationally with a focus on highly efficient, minimally invasive dentistry. He has been State President of his Dental Association and has extensive political and economic experience within the profession. Dr. Knight’s recreational pursuits include mountaineering, an interest that has taken him to a number of the highest peaks on several continents.
Geoff Knight is a general dentist from Melbourne, Australia with interests in aesthetic and minimal intervention dentistry. He has introduced a number of innovative clinical techniques and is named on several dental patents. Dr. Knight speaks internationally with a focus on highly efficient, minimally invasive dentistry. He has been State President of his Dental Association and has extensive political and economic experience within the profession. Dr. Knight’s recreational pursuits include mountaineering, an interest that has taken him to a number of the highest peaks on several continents.
RELATED ARTICLE: Silver Diamine Fluoride: A New Treatment for Caries Management?
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












