Practicing dentistry at a distance, utilizing instantaneous virtual mobile technology, was the stuff of science fiction just a few decades ago. We were taught in dental school that our capacity to diagnose disease and to perform dentistry relied entirely upon our hand instruments and our clinical abilities. Thus, the stereotype of the dentist holding a mirror and explorer, or a handpiece, adjacent to the patient seated in the dental chair, became the norm. And we, as dental professionals, were satisfied with this scenario. (Fig. 1)
Fig. 1

And then, without warning, the COVID-19 pandemic hit. As of March 2020, the majority of a million dentists around the globe were instructed to shut down their practices and stay at home. More importantly, millions of patients had their on-going treatments interrupted, and many more were left without access to routine dental care. It soon became evident that the pandemic would not fade as rapidly as everyone had hoped. The dental profession was challenged to overcome this difficult situation by seeking innovative modalities in order to provide dental diagnosis and care.
One of the primary recommendations to contain the virus is “social distancing”, and the concept of Teledentistry (tele-, prefix. from Greek meaning “far”) has become a very attractive and viable solution for both patients and dentists. Teledentistry has the potential to function not only during the pandemic but also in the future that we refer to as the “new normal”.
Teledentistry: Definition and Background
Teledentistry (a subunit of telehealth and telemedicine) can be defined as the remote facilitation of dental diagnosis, care, guidance, education and/or treatment via the utilization of information technology vs. direct face-to-face contact with a patient.1 This concept can be traced back to 1994, when the US military used teledentistry to serve US troops in the field. The Total Dental Access (TDA) project involved military dentists transferring radiographs and oral photographs to specialists at remote locations, who would then diagnose the problems and recommend treatment plans. Similar projects have been conducted for secluded populations such as prisons, homes for the elderly, and remote rural areas.
In 2015, the American Dental Association adopted a policy on teledentistry that encompassed patients’ rights, quality of care, licensure requirements, insurance reimbursement, the supervision of allied personnel, and technical considerations.2 The American Teledentistry Association (ATDA) was launched (2018) in an effort to shape the practice of teledentistry in the United States.3 Dr. Marc Ackerman, Executive Director of the ATDA indicated “the immediate goal of the ATDA is to educate dental professionals and the public about the benefits of teledentistry.”
In May 2020, as a direct result of the coronavirus pandemic, the American Dental Association (ADA) published interim guidance for coding and billing for virtual dental visits, including recommendations on the format of a virtual consultation.4 Although regulations in other countries are still at an early stage, teledentistry is rapidly being recognized worldwide as a mainstream modality of dental care.
Teledentistry: The Protocol
Teledentistry, according to the ADA, can include patient care and education delivery using, but not limited to, the following modalities:5
Synchronous (live video): live, two-way interaction between a person (patient, caregiver, or provider) and a provider using audiovisual telecommunications technology. (Fig. 2)
Fig. 2

The synchronous modality can be implemented with free, live video platforms (Zoom, Google Meet). A real-time video call may be used for initial triage, diagnosis (or a presumptive diagnosis), patient education, treatment planning, electronic prescription dispatch, and/or referral to specialists. A more sophisticated approach employs specialized platforms (readily available on the digital market) that integrate live virtual consultations into the dental office workflow software.
Asynchronous (store and forward): transmission of recorded health information through secure electronic communication systems to a practitioner, who uses the information to evaluate a patient’s condition and/or to render a service outside of live interaction.
The asynchronous modality offers the dentist access to radiographs, photographs, videos, digital impressions and other clinical data for a more comprehensive evaluation of the patient’s concerns. These specialized platforms can also empower the dentist’s referral network, as the gathered information is readily shared among various specialists both in and out of the dental field. While there are dedicated platforms available, standard email and messaging apps may be utilized effectively.
Benefits for Patients
Teledentistry’s primary patient benefits include convenience and rapid access. Even in the post-COVID world, scheduling a dental appointment may take several days or weeks depending on patient location and dentist availability. Patients living in remote areas may be several hours’ drive from the nearest dental office. Some individuals may seek specific care from a distantly located dentist. When urgent (or routine) care is required, teledentistry provides access to a dentist, from the comfort of the patient’s own home, over a wider range of hours; some websites offer virtual dental appointment 24/7. (Fig. 3)
Fig. 3

Teledentistry offers a thorough anamnesis and evaluation of the patient’s symptomatology. Patients can be instructed to take photographs with their own phones for further evaluation. The dentist is then in a good position to recommend clinical follow-up, counseling, education, and/or to provide OTC or prescription medications for pain/discomfort. The practitioner may also prescribe radiographs and/or other clinical diagnostic tests, referring the patient directly to their dental office. Alternatively, the patient may be referred to a specialist directly.
This is a good opportunity for dentists to begin the discussion of fees with patients, offering some insights into the costs of treatment. Teledentistry also facilitates second opinions, making the patient’s research process easier.
Benefits for Dentists
In the context of the COVID pandemic, teledentistry improves biosafety by reducing the number of face-to-face interactions which can spread infected droplets in the dental operatory. Furthermore, a video consultation allows the patient and doctor to converse freely without the awkward restrictions of face masks. (Fig. 4)
Fig. 4

The comfort and familiar ambience of the home setting may help patients to discuss their dental history and expectations more openly, establishing a preliminary trust relationship with the dentist even prior to the in-person appointment. Increased patient trust translates into increased case acceptance, and ultimately, increased revenue for the dental practice.
Allocating office hours specifically for productive clinical procedures makes chair time more valuable and efficient. Scheduling introductory and educational patient interactions through teledentistry (typically with auxiliary staff) frees up the practitioner’s time for family and leisure. Teledentistry is an excellent triage mechanism, determining if the patient requires immediate attention, greatly reducing non-essential visits. Referrals and more comprehensive interprofessional consultations are also facilitated.
Virtual consultation may broaden the dentist’s practice reach well beyond the office’s physical location. Case presentations can be performed at a distance with multiple participants. For example, a minor’s parents who reside in different locations can both take part in their child’s virtual dental visit.
Challenges of Teledentistry
Integrating teledentistry into the dental practice requires the practitioner and staff to be receptive to technological change. The absence of direct patient contact may seem strange initially, but most dentists and staff will adapt quickly. (Fig. 5)
Fig. 5

Patients may be reluctant to embrace teledentistry at first due to absence of technological competency, lack of interest, and the perception that these new processes are too complex. However, the rapid expansion of telemedicine is quickly making virtual triage, at the very least, the standard of treatment.
Virtual diagnosis and treatment planning may present concerns of accuracy, a problem that can readily be overcome with strict professional criteria and experience over time. The areas that still require definition are legal (licensure across jurisdictions, malpractice coverage, internet information confidentiality) and reimbursement (responsibility, enforceability, taxation).
The future of Teledentistry
In orthodontics, recent advances raise both hope and concerns. Various companies have been offering do-it-yourself treatment for several years. The patient is mailed an impression kit which they then return to a lab for the fabrication of orthodontic aligners. Alternatively, the patient can have digital impressions taken at designated scanning centers, with or without orthodontist supervision.
Dental Monitoring (Paris, France) promotes the “scan box” as the world’s first Artificial Intelligence-powered monitoring solution in dental care. This technology integrates the patient’s own smartphone to a scanner to capture home images of the dentition, which are then sent by an app to the orthodontist for monitoring.
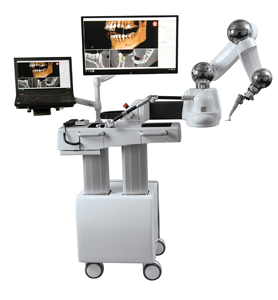
Teledentistry’s future is dependent upon the development of ever newer technologies which allow dentistry to be delivered without the physical presence of a dentist. Could actual clinical dentistry occur outside the dental office? Robotic implant placement (Neocis, Miami FL) has been approved by the FDA. (Fig 6) Other modalities are sure to follow. Quickly.
Fig. 6
Conclusions
Teledentistry is trending in the dental field, offering many benefits for dentists and patients alike. It reduces the need for travel to the dental office, live interaction (when pandemics strike), and enhances workflow, saving time and money for both patients and dentists. It also facilitates access for people in remote and isolated situations. The range and utility of app-based AI services is expected to grow dramatically in the near future. The implementation of teledentistry requires a paradigm shift, but the results are well worth the effort.
Oral Health welcomes this original article.
References
- Khan S.A., Omar H. Teledentistry in practice: literature review. Telemed J e Health. 2013;19:565–567. doi: 10.1089/tmj.2012.0200.
- ADA Statement on Teledentistry. https://www.ada.org/en/about-the-ada/ada-positions-policies-and-statements/statement-on-teledentistry
American Teledentistry Association. https://www.americanteledentistry.org - ADA COVID-19 Coding and Billing Interim Guidance : Virtual
- Visits. https://success.ada.org/~/media/CPS/Files/COVID/ADA_COVID_Coding_and_Billing_Guidance.pdf
- ADA Policy on Teledentistry. https://www.ada.org/en/about-the-ada/ada-positions-policies-and-statements/statement-on-teledentistry
About the Author
 Dr. Paola Ochoa (graduated Cayetano Heredia University 2006) was awarded a degree in Occlusion and Oral Rehabilitation, Universidad Científica del Sur. Co-founder, Infinity Dental Clinic and Infinity Advanced Dental Learning Center, Lima, Peru, Dr. Ochoa is a Diplomate of the American Board of Aesthetic Dentistry and Member, ASDA. Dr. Ochoa employs an interdisciplinary, facially driven, and minimally invasive philosophy, with extensive use of digital tools.
Dr. Paola Ochoa (graduated Cayetano Heredia University 2006) was awarded a degree in Occlusion and Oral Rehabilitation, Universidad Científica del Sur. Co-founder, Infinity Dental Clinic and Infinity Advanced Dental Learning Center, Lima, Peru, Dr. Ochoa is a Diplomate of the American Board of Aesthetic Dentistry and Member, ASDA. Dr. Ochoa employs an interdisciplinary, facially driven, and minimally invasive philosophy, with extensive use of digital tools.
RELATED ARTICLE: Future of Teledentistry in the Post-Pandemic World












