Dental implant therapy has advanced remarkably in the last decade with new innovations on both surgical and prosthetic fronts. New techniques, materials, and modalities have been developed, but the most important development has been the refinement and utilization of digital technology in treatment. Although techniques such as computer guided surgery, immediate implant placement, and immediate loading have been tested and advocated, nothing has been as universal in aiding the progression of the field of oral implantology as digital technology. Classically, much time and effort was needed to plan implant cases properly, with the use of stone models and diagnostic wax-ups. However, with the use of digital technology and workflow, it is now possible to digitally plan both surgical and prosthetic modalities to begin with the end in mind, and provide implant therapy in a more safe, efficient, and accurate manner.
The digital workflow is begun by digitizing the patient prior to any therapy. Classically, cone-beam technology was utilized to evaluate implant patients and was thought of as the best method for analyzing cases prior to treatment. However, in today’s dental implant therapy, the use of cone-beam technology to plan implant surgery is no longer enough. The CBCT scan technology must be united with digital impression technology to not only assess the surgical anatomy, but also to relate this information to the pre-planned contours of the final restoration. The fusion of these two technologies allows for the clinician to accurately plan the dental implant location as well as the position and contours of the final restoration prior to any surgical therapy. Additionally, the detailed design of the final abutment and restoration is selected prior to surgical placement of the implant, and thus directly influences the exact placement of the dental implant.
Digital Implant Planning
Utilizing a planning software that permits the merging of CBCT technology (DICOM) and digital impressions (STL) is imperative. Furthermore, the process of populating the software with this digital information must be simple. It is now possible to take a single CBCT scan of the partially edentulous patient and combine it with a single digital impression. This will allow the clinician to simply plan the implant case digitally (Fig. 1). The digital workflow now progresses by precisely designing the shape of the final restoration (via a digital wax-up) and the mechanical aspects of the final restorative design (screw-retained vs cement-retained). It is only after this 3-D position and design of the final restoration is confirmed, that the corresponding ideal and proper implant position in 4-dimensions1-2 can be determined and planned in the software. This digital “top-down” implant planning allows for the delivery of a very efficient and accurate tooth replacement which begins with the end in mind.
Dental Implant Selection
The optimal implant position can only be achieved when selecting the correct size of implant for the specific size of tooth to be replaced.2 With the influx of platform switching in numerous implant designs today, it is important to appreciate that the emergence profile of the restoration begins from the implant connection width and not the actual width of the implant.3 Therefore if a large mismatch exists between the width of the implant and the width of connection, the fixture may need to be placed more apically to allow for the optimal amount space needed to create the ideal emergence profile. Proper implant placement depth is paramount to long-term implant success, as placing an implant too shallow is an uncorrectable mistake leading to poor emergence profile, food impaction and tissue inflammation.3 Lastly, it is fundamental that the implant connection type utilized in today’s implant therapy lend itself to being restored in numerous ways utilizing new innovations and technologies. Restorative flexibility is an absolute requirement of the implant utilized today (Fig. 2).
Computer Guided Implant Surgery
After the 3D position and contour of the final restoration has been established and approved, the implant position and need for any hard or soft-tissue augmentation can be determined. The planned implant placement must allow for the correct biological result as well as provide the environment needed for the restorative design to become a reality. The planned implant placement in 4-dimensions2 can then be transferred from the virtual world to the real world via guided surgery. This is the key aspect of the digital workflow. It has been established that fully guided implant surgery is the most precise and certain method of transferring the digitally planned implant position to the oral cavity during surgical placement.4,5 The surgical guide is designed in the planning software, and then is printed using a 3D printer (Fig. 3). In partially edentulous cases, these surgical guides can be tooth supported which makes them very simple to seat and stabilize. Furthermore, it allows for many surgeries to be performed utilizing an atraumatic flapless protocol. This precision and predictability in surgical planning makes for fewer surprises during surgery and allows for more accurate treatment results for the patient.
Figure 1

Nobel Clinician SmartfusionTM initial digital planning. Blue is the digital rendering of the desired final tooth position. (Digital Wax-up) Pink is current tissue position. (Model)
Figure 2

NobelParallelTM CC implant utilizing a conical connection and platform switching technology.
Figure 3

Digitally designed surgical guide to be utilized in fully guide surgical protocol. Implant position based solely on final restoration position and contours.
Inmmediate Provisional Restoration
The utilization of an immediate implant restoration provides many benefits, however, developing the ideal emergence profile for the implant restoration is the key purpose of the provisional restoration. This allows for the implant restorative tissue bed to mimic the biological appearance of a natural tooth. An immediate provisional restoration placed on an immediately placed implant also provides the added benefit of maintaining the natural anatomic emergence profile that was provided by the natural tooth root.6,7 However, it is essential that to shape the soft tissue profile, the implant fixture must be placed at the proper depth and the soft tissue thickness must be adequate.8 Provisional restorations may be either screw-retained or cement retained. Ideally, screw-retained provisional restorations are preferred. With the use of digital implant planning, and fully-guided implant surgery, it is now possible to fabricate a screw-retained provisional restoration prior to the surgery and deliver it intra-orally with some slight modifications on the day of surgery.
Tissue Contouring Using New Materials & Modalities
The placement of an implant provisional restoration delivers restorative design to the implant site. One technique that has been utilized as an alternative to a provisional restoration is the use of a customized gingival former. This allows for soft tissues to be contoured without having the risk of a restoration in occlusion. Fabrication of both customized gingival formers and provisional restorations can be technique sensitive and time consuming when done chairside. Furthermore, lab-processed restorations may be delayed and bring added cost to the treatment. Additionally, the common materials utilized for these custom solutions are composite resin and PMMA acrylic which both may not be as kind to the soft tissues.9 One restorative innovation that has been developed is the use of Polyether Ether Ketone (PEEK) as a material to be used for both gingival formers and provisional abutments that have been pre-milled as stock abutments with standardized emergence profiles built into them (Figs. 4-7) This provides much more efficiency in the fabrication of chairside provisional restorations, as well as customized gingival formers. PEEK is a material that has been demonstrated to be favorable to periodontal soft tissues, and is adjustable.10 As a result, through the digital workflow, it is now possible to construct a provisional restoration using PEEK abutments, before implant placement, and then deliver it intraorally (Fig. 6).
Figure 4

NobelParallelTM CC WP implant placed into immediate molar site and utilization of a PEEK anatomical healing abutment (gingival former).
Figure 5

NobelParallelTM CC WP implant with PEEK anatomical healing abutment
(gingival former).
Figure 6

NobelParallelTM CC WP implant with PEEK provisional abutment.
Figure 7

Wide Platform Conical Connection implant with immediate provisional restoration utilizing the PEEK anatomical provisional abutment.
Restorative Design
The digital workflow begins and ends at the same point, the final restoration. Designing the final restoration prior to surgical implant placement allows for focused delivery of a predictable tooth replacement. Final implant restorative designs can be broadly divided into cement-retained and screw-retained types. Documented issues with retained cement around cemented final implant restorations leading to peri-implantitis and other mucositis type issues has made screw-retained final restorations the preferred design.11,12 With new innovations in screw-retained technology such as Angulated Screw Channel (NobelProcera® Angulated Screw Channel) it is now possible to have the vast majority of implant restorations be screw-retained (Figs. 8-9).
Figure 8

NobelProcera® Angulated Screw Channel crown design. Screw angulation is corrected 22.4 degrees.
Figure 9
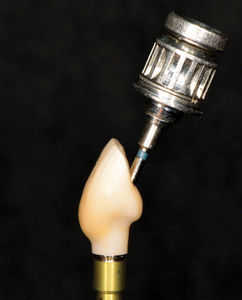
NobelProcera® Angulated Screw Channel crown. Note direction of fixture vs abutment screw.
Figure 10

Four “Screwmentation” Monolithic Zirconia screw-retained crowns.
Cad-Cam Milled Final Restorations
Today the material choice (eg. Zirconia vs Lithium Disilicate) and technical design (monolithic or layered) of the restoration can also be planned digitally prior to surgery. Soft tissues have been shown to react more favorably with the presence of a highly-polished zirconia or titanium surface.13 Therefore it is recommended that the area of the implant restoration that will be sub-gingival be comprised of highly polished zirconia or titanium. Also, sub-gingival extension of ceramic restorative materials may not be as favorable.14 The use of CAD-CAM technology allows for the milling of final restorations in a more accurate and repeatable fashion. Overall, implant restorations should be designed to minimize prosthetic complications such as chipping. Classically, a screw-retained crown was fabricated by baking porcelain onto a metal-based custom abutment. Although this provides an adequate solution that can be very esthetic, it is also imperfect in the fact that porcelain may readily chip or break off these restorations long-term.15 With new innovations in restorative design, materials such as monolithic zirconia have become a reality and offer a very tissue friendly, biocompatible option. A full-contour zirconia crown allows for the esthetics of a tooth-colored material to be utilized with minimal porcelain layering. However, up till now this type of restoration could only be utilized for screw-retained solutions by cementing these CAD/CAM zirconia crowns extra-orally onto a titanium abutment to create a “screwmentation” type of implant restoration. This may result in long-term issues with cement retention and de-bonding of restorations (Fig. 10).
New Cad-Cam Cement-Free Final Restorations
An innovative implant crown design that has developed is the fully mechanical, cement free, full-contour CAD/CAM zirconia crown (NobelProcera® Full Contour Zirconia Implant Crown). This new type of screw-retained crown uses technological innovation in screw-retained technology, namely the Angulated Screw Channel (NobelProcera® Angulated Screw Channel), and delivers a monolithic zirconia screw-retained crown that is free of any cement and just involves engineered CAD/CAM components (Fig. 11).
Historically, the main concern with creating a screw-retained restoration has been the position of the screw access channel, which has restricted the use of screw-retained restorations where the trajectory and location of this access channel is an esthetic concern. Furthermore, when posterior access to the implant site is difficult due to patient factors (e.g. limited opening), screw-retained restorations were also found to be difficult to deliver. The ASCTM technology has allowed clinicians to overcome this by re-angulating the screw access channel up to 25 degrees there by creating screw retained restorations with favorable esthetics and ease of delivery posteriorly. Coupled with this is the technology to mill the restoration from a highly esthetic full contour monolithic zirconia material, which for the posterior molar site fulfills all the functional and esthetics requirements needed (Figs. 12-13).
Figure 11

NobelProcera® Angulated Screw Channel with blue ASCTM Omnigrip screw.
Figure 12

NobelProcera® Full Contour Zirconia crowns. Note blue ASCTM Omnigrip screws.
Figure 13

NobelProcera® Full Contour Zirconia crowns. Frontal view.
New On1TM Concept Perio-Prosthetic Platform
The implant-abutment connection is the most important component of the dental implant system. This is the place where forces concentrate and bacterial colonization can occur. Furthermore, this connection is often sub-gingival and sub-crestal resulting in tissue adherence to components attached to the connection. As a result, it has been proposed and demonstrated that numerous disturbances to the biological equilibrium of the implant-abutment connection can result in tissue trauma, inflammation, and subsequent bone remodeling.16-18 Considering that the removal and switching of components (eg. healing caps, impression copings, abutments) into the implant-abutment connection occurs at least three to four times in each implant case, tissue trauma may readily occur. Furthermore, it has been demonstrated that decreased bone remodeling may occur if a final abutment is delivered into the implant-abutment connection on the day of surgical placement.18 However, this may be restoratively limiting due to tissue resolution and implant position/angulation. As a result, an innovative perio-prosthetic restorative platform has been developed that seals off the implant-abutment connection on the day of surgical placement and still allows for restorative flexibility. The On1TM concept (Nobel Biocare) is a restorative platform that preserves the soft tissue attachment at the implant-abutment connection and allows for restorative workflows to occur without disturbing the implant-abutment connection. Furthermore, it can be completed utilizing a digital workflow (Fig. 14).
Figure 14

Immediate maxillary molar placement of a NobelParallelTM CC WP implant with simultaneous indirect sinus grafting.
Figure 15

Nobel Biocare WP On1TM base.
Figure 16

Nobel Biocare WP On1TM base seated into implant and torqued to 35NCm.
Figure 17

Nobel Biocare WP On1TM IOS healing cap (PEEK) which is also an IOS scan body for intraoral scanning.
Figure 18

Post-Operative Radiograph of immediate implant placement and placement of On1TM abutment and PEEK healing abutment.
Figure 19

Digital workflow and implant positioning based on On1TM IOS healing cap (PEEK).
Figure 20

Digital workflow and On1TM base monolithic zirconia screw-retained final crown design.
Figure 21

Occlusal view of final screw-retained crown on On1TM base.
Figure 23

Lateral view of final screw-retained crown on On1TM base.
Figure 24

Lateral view of final screw-retained crown on On1TM base.
Conclusion
Tooth replacement using dental implants is reaching new levels of success and efficiency today with the utilization of digital technology. By digitizing the patient and utilizing intuitive software to properly plan the cases “top-down”, superior accuracy and predictability can be seen. Fully digital implant treatment using minimally invasive surgical techniques, and pre-manufactured prosthetic delivery utilizing new materials and mechanics may soon become the standard of care. Dentists will need to become familiar with the technology available to truly realize the surgical-prosthetic synergy in oral implantology. Digital perio-prosthetic implant therapy is the future. OH
Oral Health welcomes this original article.
References
- Cooper LF, Objective criteria: guiding and evaluating dental implant esthetics. J Esthet Restor Dent. 2008;20(3):195-205.
- Funato A, Salama MA, Ishikawa T, Garber DA, Salama H. Timing, positioning, and sequential staging in esthetic implant therapy: a four-dimensional perspective. Int J Periodontics Restorative Dent. 2007 Aug;27(4):313-23.
- Cappiello M, Luongo R, Di Iorio D, Bugea C, Cocchetto R, Celletti R. Evaluation of peri-implant bone loss around platform-switched implants. Int J Periodontics Restorative Dent. 2008 Aug;28(4):347-55.
- Ozan O1, Turkyilmaz I, Ersoy AE, McGlumphy EA, Rosenstiel SF., Clinical accuracy of 3 different types of computed tomography-derived stereolithographic surgical guides in implant placement. J Oral Maxillofac Surg 2009 Feb;67(2):394-401.
- Pettersson A, Kero T, Gillot L, Cannas B, Fäldt J, Söderberg R, Näsström K. Accuracy of CAD/CAM-guided surgical template on human cadavers: Part 1. J Prosthet Dent. 2010 Jun;103(6):334-42.
- Rosa AC, da Rosa JC, Dias Pereira LA, et al. Guidelines for selecting the implant diameter during immediate implant placement of a fresh extraction socket: a case series. Int J Periodontics Restorative Dent. 2016;36(3):401-407.
- Kinaia BM, Ambrosio F, Resident P, Lamble M, Resident P, Hope K, Resident P, Shah M, Neely AL. Soft Tissue Changes Around Immediately Placed Implants: A Systematic Review and Meta-analyses With at Least 12 Months Follow up After Functional Loading. J Periodontol. 2017 May 18:1-17.
- Wittneben JG, Brägger U, Buser D, Joda T. Volumetric Calculation of Supraimplant Submergence Profile After Soft Tissue Conditioning with a Provisional Restoration. Int J Periodontics
Restorative Dent. 2016 Nov/Dec;36(6):785-790. - Luchinskaya D, Du R, Owens DM, Tarnow D, Bittner N. Various Surface Treatments to Implant Provisional Restorations and Their Effect on Epithelial Cell Adhesion: A Comparative In Vitro Study. Implant Dent. 2017 Feb;26(1):12-23.
- Rea M, Ricci S, Ghensi P, Lang NP, Botticelli D, Soldini C. Marginal healing using Polyetheretherketone as healing abutments: an experimental study in dogs. Clin Oral Implants Res. 2017 Jul;28(7)
- Korsch M, Walther W. Peri-Implantitis Associated with Type of
Cement: A Retrospective Analysis of Different Types of Cement and Their Clinical Correlation to the Peri-Implant Tissue. Clin Implant Dent Relat Res. 2015 Oct;17 Suppl 2:e434-43. - Korsch M, Robra BP, Walther W. Cement-associated signs of inflammation: retrospective analysis of the effect of excess cement on peri-implant tissue. Int J Prosthodont. 2015 Jan-Feb;28(1):11-8.
- Linkevicius T, Vaitelis J. The effect of zirconia or titanium as abutment material on soft peri-implant tissues: a systematic review and meta-analysis. Clin Oral Implants Res. 2015 Sep;26 Suppl 11:139-47.
- Linkevicius T. The Novel Design of Zirconium Oxide-Based Screw-Retained Restorations, Maximizing Exposure of Zirconia to Soft Peri-implant Tissues: Clinical Report After 3 Years of Follow-up. Int J Periodontics Restorative Dent. 2017 Jan/Feb;37(1):41-47.
- Wittneben JG, Millen C, Brägger U. Clinical performance of screw- versus cement-retained fixed implant-supported reconstructions – a systematic review. Int J Oral Maxillofac Implants. 2014;29 Suppl:84-98.
- Nader N, Aboulhosn M, Berberi A, Manal C, Younes R. Marginal Bone Remodeling around healing Abutment vs Final Abutment Placement at Second Stage Implant Surgery: A 12-month
Randomized Clinical Trial. J Contemp Dent Pract. 2016
Jan 1;17(1):7-15. - Berberi AN, Noujeim ZN, Kanj WH, Mearawi RJ, Salameh ZA. Immediate placement and loading of maxillary single-tooth implants: a 3-year prospective study of marginal bone level. J Contemp Dent Pract. 2014 Mar 1;15(2):202-8.
- Degidi M1, Nardi D, Piattelli A. One abutment at one time: non-removal of an immediate abutment and its effect on bone healing around subcrestal tapered implants. Clin Oral Implants Res. 2011 Nov;22(11):1303-7.
 Dr. Birdi is a certified Periodontist & Prosthodontist. He co-director of the Pacific Institute for Advanced Dental Education as well as co-founder of the Digital Dentistry Institute. He practices at the BC Perio Dental Health & Implant Centres in Vancouver & Coquitlam. His practice focuses on periodontal and prosthetic treatment with a major focus on implant dentistry.
Dr. Birdi is a certified Periodontist & Prosthodontist. He co-director of the Pacific Institute for Advanced Dental Education as well as co-founder of the Digital Dentistry Institute. He practices at the BC Perio Dental Health & Implant Centres in Vancouver & Coquitlam. His practice focuses on periodontal and prosthetic treatment with a major focus on implant dentistry.

Dr. Ron Zokol is a Diplomate of the American board of Oral Implantology/Implant Dentistry and of the International Congress of Oral Implantologists. He has over 30 years of experience in implant dentistry and is the founder and co-director of the Pacific Institute for Advanced Dental Education which is an educational institute for dentists.
 Dr. Sundeep Rawal received his dental degree at the UF College of Dentistry and then completed his training in prosthodontics at the University of California San Francisco. He is co-founder of the Digital Dentistry Institute which is an educational institute for his fellow dentists. His practice out of Orlando, Florida focuses on digital prosthetic treatment and implantology.
Dr. Sundeep Rawal received his dental degree at the UF College of Dentistry and then completed his training in prosthodontics at the University of California San Francisco. He is co-founder of the Digital Dentistry Institute which is an educational institute for his fellow dentists. His practice out of Orlando, Florida focuses on digital prosthetic treatment and implantology.
 Dr. Saj Jivraj earned his DDS at the University of Manchester, and was then accepted at the world-re- nowned Herman Ostrow School of Dentistry at the University of Southern California (USC), where he received his certification in prosthodontics. He is founder of Allon4doctors.com as co-founder of the Digital Dentistry Institute. He has a comprehensive prosthodontic practice in the Los Angeles area.
Dr. Saj Jivraj earned his DDS at the University of Manchester, and was then accepted at the world-re- nowned Herman Ostrow School of Dentistry at the University of Southern California (USC), where he received his certification in prosthodontics. He is founder of Allon4doctors.com as co-founder of the Digital Dentistry Institute. He has a comprehensive prosthodontic practice in the Los Angeles area.
RELATED ARTICLE: Final Molar In One Day: Digital Implant Therapy Utilizing Current Technology









