The task of repairing restorations has historically been an unproductive procedure in the dental practice. Dental professionals have learned through extensive personal experience that repairs, whether intra- or extra-oral, have a very poor prognosis. In fact, no matter how carefully the fractured ceramic or composite surface was roughed, cleaned, dried, primed, and bonded, the repair invariably failed within a short time. Understandably, dentists are reluctant to perform risky repairs because they then assume forward responsibility for the condition of the tooth; patients return with alarming regularity with failed patches, and eventually, practitioners must remake the restoration, often at their own expense.
The easiest (and most profitable) solution is to recommend a new crown, bridge, or restoration. This may be feasible for the patient in many instances. However, the dentist must also consider situations where the patient’s financial position is simply incompatible with the ideal treatment plan. A more affordable alternative must be made available.
There may be circumstances where the fractured restoration is an integral and/or inseparable part of an extensive bridge or rehabilitation, the removal and/or replacement of which is clinically or financially prohibitive for both the patient and the dentist.
The fracture may have occurred on a recently placed restoration. The practitioner prefers a long-term temporary, but highly esthetic, reparative solution until the patient’s oral state has stabilized, and a decision on the necessity for a remake can be made with confidence.
In these cases, “heroic” dentistry is often called for. For the dentist, it may be difficult, out of the ordinary, and out of the box. The specific treatment approach may be beyond the typical indications for the material, and more adventurous than routine practice. However, given the proper scientific foundation, and the backing of research, the extra mile is of great value to the patient, and ultimately to the occupational satisfaction of the dental team.
The three major clinical concerns with earlier repair “systems” were:
1. Low reparative bond strengths to the remaining restorative substrate(s) leading to rapid failure
2. The need to stock a variety of unexpired adhesive systems, one for each category of residual base layer, and each with its own protocol and instructions-for-use
3. Situations where several different substrate layers were exposed by the fracture, each ideally repaired with a different adhesive and technique
Recent advances in adhesive technologies have improved the adhesion of reparative composite (typically flowable resin) to the remaining substrates. These enhanced bonding values make repairs much more predictable and less worrisome to the practitioner.
Given the extensive variability of indirect and direct restorative materials that are available today, it is virtually impossible to keep track of, and have access to, the dedicated reparative products that are indicated for each individual substrate. Furthermore, if the repairing and the original restoring dentists are not the same, there may be no clear record of the actual materials that were used, and must now be adhered to.
Restorative fractures are not orderly; cracks propagate irregularly across and through the various layers of a restoration, often leaving a multitude of substrates that require reparative adhesion. These layers are often thin, barely visible even with magnification, and impossible to treat individually in or out of the oral cavity.
CeraResin Bond Porcelain & Resin Repair System, a bonding system specifically designed for the repair of ceramic, porcelain, acrylic, and crown and bridge materials, was introduced by Shofu Dental USA (San Marcos CA). It was developed to overcome the existing clinical difficulties associated with the repair process. It is simple and intuitive to use (Fig. 1).
Fig. 1

It has been specifically designed as a universal adhesive; it forms an effective and predictable interface between ceramics, direct and indirect composites, cold-curing resins, denture teeth, and light-curing reparative materials (Table 1). The “universal” feature, its adhesion to all restorative materials, is particularly important to the practitioner; one single reparative adhesive (with one single protocol) covers ALL potential clinical eventualities, simplifying techniques and supply management. In cases where multiple materials are exposed by the fracture, the dentist is assured that CeraResin Bond universal adhesive addresses all the substrates.
Table 1

Improved adhesive strengths make the reparative process much more predictable, and thus, much less risky. A repair can now be expected to have a considerable service life. This makes the repair vs. remake decision much easier for the dentist and much more convenient for the patient.
Procedure
Three specific quick steps form the entire CeraResin repair procedure. Pretreatment is consistent with existing techniques: roughen the surface, clean and dry, etch with phosphoric acid (optional for extra-oral repair), and rinse and dry. Then:
(1) Apply one coat of Bond I and leave undisturbed for 10 seconds;
(2) Apply one coat of Bond II and leave undisturbed for 10 seconds;
(3) Light-cure.
Restore the necessary dental anatomy to form and function with any adhesive and composite resin (typically a flowable) that is currently used in the practice.
Chemistry
CeraResin Bond 1 contains ethanol (carrier) and silane (active ingredient). It is the silane that primes the various substrates and couples to all ceramics, including the fillers in composite resins (Fig. 2).
Fig. 2

CeraResin Bond 2 is comprised of acetone (carrier), 4-AET (4-acryloxyethyltrimellitic acid – an adhesive-promoting monomer), UDMA (fast-curing polymer), and a polymerization initiator (Fig. 3).
Fig. 3

CeraResin Bond is extremely resistant to moisture infiltration and to thermal strains, providing a durable, long lasting bond. It is compatible with, and can be used intra- or extra-orally to adhere all ceramics, all composites, and all acrylics. Thus it is useful both chairside and at the laboratory bench.
Clinical Case 1
The patient’s smile was compromised by a single unesthetic tooth (Fig. 4). The left lateral had previously been fractured and restored with resin that had stained and pitted over the years (Fig. 5). The treatment of choice was a full crown. Given the lack of remaining tooth structure, elective endodontics, post-and-core, and crown were recommended. The patient requested treatment that was less aggressive and less costly. The original restorative material was not identifiable. The old restoration was partly removed, leaving some buccal tooth structure and mostly old composite (Fig. 6). The surfaces were roughened with air-abrasion, and the CeraResin Bonds 1 and 2 were applied in sequence and light-cured. Tooth form was restored with Beautifil Flow Plus and Beautifil II hybrid giomer (Shofu Dental USA, San Marcos CA). After polishing, a good color match and esthetics were achieved (Fig. 7). A close-up reveals an esthetic restoration, which should provide years of predictable function (Fig. 8).
Fig. 4

Fig. 5

Fig. 6

Fig. 7

Fig. 8

Clinical Case 2
A porcelain laminate veneer placed some years before had debonded essentially intact (Fig. 9). The highly visible position of the left lateral, and the worn condition of some of the adjacent anteriors, suggested that 6 anterior porcelain veneers would be an ideal treatment. The patient demurred for financial reasons. After examination and microabrasion, it was found that the buccal surface was partially natural tooth structure and partly composite (Fig. 10). The ceramic veneer recementation must take into account multiple substrates, natural tooth, remaining composite restorative, resin cement, and ceramic; it is crucial however that all the components, ceramic, composite, and natural tooth structure adhere to each other through the veneer cement. The natural tooth surface was etched and bonded with BeautiBond 7th generation adhesive. The intaglio of the veneer and the composite on the tooth were treated with CeraResin Bonds 1 and 2 in sequence. The light-cured veneer cement was applied to the veneer, which was then seated. The excess cement was removed and the entire surface light cured (Fig. 11). The patient’s esthetic smile was restored within their financial means (Fig. 12).
Fig. 9

Fig. 10
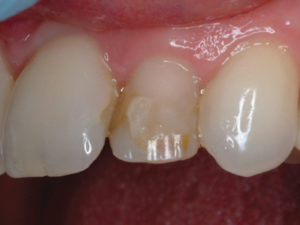
Fig. 11

Fig. 12

Conclusion
The availability of a universal repair adhesive makes heroic dentistry more predictable and less risky. Adhesive to all ceramic, porcelain, acrylics, and direct and indirect composite materials, the repair system is compatible with all resins and composites. It can be used to quickly modify and adapt porcelain and resin restorations instead of remaking them, providing a strong and durable bond. Shofu’s CeraResin Bond System allows dentists to treat patients who require immediate esthetic repairs with confidence and to offer treatment options to those who are unable to afford more comprehensive treatment options. OH
Oral Health welcomes this original article.
About the Author
Dr. George Freedman is a founder and past president of the American Academy of Cosmetic Dentistry, a co-founder of the Canadian Academy for Esthetic Dentistry and the International Academy for Dental Facial Esthetics, and a Diplomate of the American Board of Aesthetic Dentistry. He is Professor and Program Director, BPP University, London, UK, MClinDent programme in Restorative and Cosmetic Dentistry. His most recent textbook is “Contemporary Esthetic Dentistry (Elsevier). He is the author or co-author of 14 textbooks, more than 800 dental articles, and numerous webinars and a Team Member of REALITY. Dr Freedman received the Irwin Smigel Prize in Aesthetic Dentistry (NYU College of Dentistry). He lectures internationally on cement-free implant restoration, dental esthetics, adhesion, composites, implants, 3D printing, and porcelain veneers and crowns. Dr. Freedman is a Regent and Fellow of the International Academy for Dental Facial Esthetics and maintains a private practice limited to Esthetic Dentistry in Toronto, Canada.












