This article is the second in a series for Oral Health. The first article was published in the August 2015 issue, with the title “Surgical Risk Factors in Implant Dentistry: Influence on Failures and Bone Loss”. Table 1 in this article, organizes risk factors in implant dentistry into four categories. These were introduced in the August 2015 article together with the concept of “Evidence Based Dentistry” and a representative case presentation.
This current article will primarily focus on the influence of the first of the four risk factor categories as seen in Table I i.e. “Patient Related Systemic Risk Factors”. This article will also describe the importance of “Patient Informed Consent” as knowledge of risk factors is crucial to successfully providing patient informed consent. Risks that are foreseeable need to be considered at many stages, i.e. at the initial patient interview, in order to formulate the prognosis and treatment plan, during the patient consultation, formulating the treatment plan options and the maintenance plan (see Table 2). This article will also illustrate two similar cases treated by the author and will discuss the influence of risk factors on these cases and in particular the “Patient Related Systemic Risk Factors”. Future articles will cover risk factors in the other three risk factor categories in more detail namely: “Patient Related Local Risk Factors”, “Operator Related Risk factors” and “Biomaterial Related Risk factors” (Table 1).


Patient Related Systemic Risk factors: (Table 1)
This category of risk factors includes but is not limited to patient related: a) complaints, expectations, psychological suitability and limitations (e.g. clinical limitations and financial limitations), b) history of periodontitis (especially aggressive periodontitis) and c) smoking, systemic disease and medications.

• a) Patient Complaints, Expectations, Psychological Suitability and Limitations:
Patient’s complaints, problems, goals, expectations (especially comfort, functional, phonetic and esthetic expectations), psychological suitability and limitations (including clinical and financial limitations), should be investigated in detail at the initial patient interview. In particular the patient’s esthetic requirements and expectations need to be analyzed and a determination made if the patient’s expectations are realistic. These determinations are primarily made at the initial patient interview and diagnostic phases. A thorough esthetic analysis may include the factors as outlined in Table 3.
• b) History of Periodontitis:
A patient’s history of periodontitis and in particular aggressive periodontitis needs to be determined from the information gathered from both the initial patient interview, previous dental records as well as from the diagnostic information gathering phase. There have been several articles studying this issue. Readers are referred to a meta-analysis published in 2014.1 A conclusion can be drawn from this review that a history of aggressive periodontitis poses a negative risk factor for and should be taken into account and included as part of the “informed consent” process and treatment.
• c) Smoking, Systemic Disease and Medications:
The patient’s dental, medical and habit history and in particular current conditions that could impact upon the outcome, need to be questioned and evaluated at the initial patient interview and where indicated investigated in more detail. Outside consultations may be needed to determine if any pre-treatment precautions need to be taken or if treatment is absolutely contra-indicated.
There are certain medical conditions that may be considered to be “absolute contraindications” including but not limited to: unrealistic expectations, psychiatric instability, recent heart attack or stroke, severe immunosuppression, uncontrolled bleeding, current malignancy therapy, high dose radiation, drug abuse-alcoholism, pregnancy, diabetes that is severely uncontrolled, renal failure, severe infection, IV- bisphosphonates, severe liver disease, and non-compliance with critical aspects of the recommended therapy. Non-compliance can include diverse issues such as patient unwillingness to commit to proper maintenance and a patient wanting to determine the treatment plan that is contrary to an appropriate treatment as determined by the dental professionals.
Smoking is considered to be a relative risk factor as there have been numerous studies correlating smoking with increased implant failure rates. As well there is some evidence that the risk may be dose related and that smoking cessation may reduce the risk. Dentists should advise prospective patients of these factors and they may decide to modify their clinical protocols with smokers. There are many medical conditions and medications where there is insufficient evidence to say that they are absolute contraindications to treatment. However, some conditions and medications require medical evaluation and may be considered to be “relative risk factors”. Some of these conditions may include but are not limited to: Parkinson’s Disease, Osteoporosis, Hyperparathyroidism, certain bone disorders e.g. Pagets, certain auto immune diseases e.g. Lupus, smoking (dose dependant), Genotype-IL1 especially combined with smoking, history of periodontitis especially aggressive periodontitis, certain medications e.g. oral bisphosphonates, corticosteroids, immune suppressants, and anticoagulants. Advanced age as a risk factor is of significant interest as it is a very common patient inquiry. The vast majority of studies on this subject however have not linked advanced patient age to higher implant failure!
Many common systemic medications have an effect on bone metabolism and have been postulated to possibly affect osseointegration negatively. A 2016
article2 reviewed this subject and found no convincing human experimental evidence that the reviewed medications should be considered absolute contraindications to implant dentistry. Nevertheless the authors advised readers to cautiously approach these situations and that further human studies were needed. The systemic medications that were reviewed in this article included: Cyclosporine, Glucocorticoids, Selective Serotonin Reuptake Inhibitors, Nonsteroidal Anti-Inflammatory Drugs, Oral Bisphosphonates and Chemotherapeutic Agents. Research is ongoing and medications that can negatively affect osseointegration may come to light in the future. For example a 2016 animal study3 concluded that a common medication used for gastroesophageal reflux and peptic ulcer disease (Omeprazole, marketed by the brand name Prilosec and Losec) “impaired bone healing and implant osseointegration”.
Patient Informed Consent
Successfully achieving “patient informed consent” is a critically important aspect of overall patient care. It is a legal and ethical duty for dentists to make sure that the patient understands the important aspects of treatment. There have been several recent RCDSO Dispatch articles that have addressed this issue, for example “Dental Implant lawsuits”, August/September 2015 issue, “Informed Consent Learning program”, November/December 2015 issue and “Informed Consent From
Material Risks to Material Information”, February/March 2016 issue. Readers are encouraged to reference these RSCDO publications but some of the key points related to patient informed consent are:
1) It is a comprehensive and ongoing process
2) Includes material risks and material information (e.g. alternatives)
3) Patients must appreciate relevant and foreseeable consequences
4) Patient questions need to be encouraged
5) Delegation is allowed but the dentist is ultimately responsible
6) Consent forms are only a part of the overall process
7) Lists of risks and side effects are critical and need to be updated
8) Detailed documentations is the best “evidence”
An integral part of achieving patient informed consent requires a knowledge and application of the significant risk factors and this applies throughout the “sequence of therapy”.
Informed Consent, Risk Factors and Sequence of Therapy: (Tables 1 & 2)
1) Initial patient interview
At the initial interview the patient’s complaints, problems, expectations, goals, limitations, past and present medical and dental history need to be investigated. An assessment needs to be made if the patient is a suitable candidate from a psychological, medical, dental and financial viewpoint. Potential risk factors as outlined in Table 1 need to be identified and evaluated.
2) Data Collection
At the diagnostic gathering phase, a thorough clinical, radiographic examination at the minimum are necessary and as well additional diagnostic aids such as study models and diagnostic wax-ups may be indicated. Potential risk factors as outlined in Table 1 need to be identified and evaluated. In particular, esthetically demanding cases may require a more detailed analysis to anticipate potential esthetic related risks (Table 3).
3) Diagnosis, Prognosis and Treatment Plan
In formulating the diagnosis, prognosis, and treatment plan as well as the treatment plan options, potential risk factors as outlined in Table 1 need to be identified and evaluated. A determination needs to be made of the suitability of various treatment plan options that are reasonable to present to the patient.
4) Patient Consultation
The patient consultation is a critically important phase to start the ongoing process of successfully providing “Patient Informed Consent”. Readers are referred to the recent RCDSO Dispatch publications referred to earlier in this article which goes into detail on the factors that encompass patient informed consent. At the patient consultation, obtaining “informed consent” is a comprehensive process that includes a thorough review of all suitable treatment options including a discussion of the benefits, the advantages and disadvantages of the treatment options, the risks of each treatment option as well as the risks of no treatment. While the clinician can depend on their knowledge and experience to advise the patient on the treatment that they feel is most appropriate, clinician bias should be avoided and suggestions should b e patient centered in order to enable the patient to make an informed decision. While the patient may have a pre-conceived idea of an appropriate treatment plan for themselves, it is incumbent on the dentist to educate the patient and for example explain significant risk factors that the patient would not be aware of that in turn may indicate alternate treatment.
5) Treatment and Maintenance:
With treatment and in particular with maintenance, the patient needs to be made aware of the responsibilities of the patient as well as dental professionals. Where significant risk factors are present, specific additional measures that need to be taken to mitigate the risk need to be explained to the patient. For example in a patient with a history of Aggressive Periodontitis, all parties need to be aware that a more intensive monitoring and maintenance program may be indicated.
Case Presentations: (Figs. 1-20)
A common situation we see in our practice is when patients present with a “terminal dentition”, often characterized by advanced caries and or periodontal disease and missing teeth. These patients may want to have full mouth extractions and full arch implant rehabilitation, and in some cases this treatment may be justified and indicated. Two very similar cases with terminal dentitions and treated in this manner are presented in this article. These two cases are illustrated in Figures 1-20 and are discussed below relative to the sequential diagnosis, treatment planning process, achieving informed consent (Table 1) while considering the associated risk factors and primarily “Patient Related Systemic Risk factors” (Table 2).
Case 1
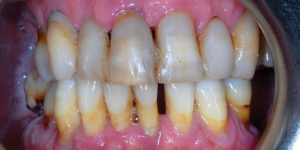
Pre-treatment “smile” view Pre-treatment “retracted” view

Pre-treatment panoramic radiograph Post-treatment “smile” view


Post-treatment “retracted” view Post-treatment panoramic radiograph


Definitive Locator abutments in maxilla

Definitive Locator abutments in mandible

Maxillary definitive Overdenture prosthesis

Mandibular definitive Overdenture prosthesis

Case 2
Pre-treatment “retracted” view Pre-treatment panoramic radiograph


Post-treatment “retracted” view Post-treatment panoramic 1 yr radiograph


Definitive Locator abutments in maxilla

Definitive Locator abutments in mandible

Maxillary definitive Overdenture prosthesis

Mandibular definitive Overdenture prosthesis

Post treatment “smile” view Post-treatment 3 yr panoramic radiograph


Case #1 and Case #2:
It is not within the scope of this article to cover in detail all the risk factors taken into account with these two cases, however, some important factors are outlined below.
Initial patient interview
• Patient Chief Complaints / Problems: Poor esthetics and function, “fed-up” with continuous dental problems, e.g. pain and cost.
• Patient Expectations / Goals: “Good” esthetics and function and phonetics, avoid full palatal coverage, ease of personal and professional maintenance, affordability, stable long-term results
• Limitations: Financial, compliance and dexterity for oral hygiene
• Medical and Dental History: Non-contributory except for poor oral hygiene and a history of aggressive periodontitis.
Diagnosis / Prognosis:
• Diagnosis: Generalized advanced periodontal attachment loss, caries, heavily restored teeth, poor esthetics and function. Good potential bone quantity and quality availability for six or more implants in both arches i.e. very good bone in the mandible and fairly good bone in the maxilla. Existing pre extraction bone and gingival tissue loss with anticipated significant further recession after extractions and extraction socket healing.
• Prognosis for the Natural Teeth: generally poor.
• Prognosis for the Implants: Implant prognosis was anticipated to be excellent in the mandibular anterior area and fairly good in the anterior maxilla. The prognosis was arrived based on factors such as no systemic risk factors other than a history of aggressive periodontitis and less than ideal patient home care compliance. However, despite these risk factors the implant prognosis was anticipated to be good due in part to a prosthesis design that would facilitate maintenance (see below), relatively good bone quality and quantity and the
author’s good long term results achieved with many similar cases (Table 4).
Table 4
“Unsplinted Overdenture Implant Survival”

Treatment Plan:
• Treatment Plan and Options: Definitive prosthetic options would include: Conventional removable partial and or complete dentures, implant removable overdentures (unsplinted or bar splinted) and fixed implant prostheses. After taking into account the risk factors and achieving patient informed consent as outlined in this article, the decision was made to treat with full arch removable implant overdentures with unsplinted attachments. More specifically the choice of this prosthetic design was decided based upon the advantages it offered over the other prosthetic designs relative to: patient preferences, limited finances, bone availability for this option without having to consider bone augmentations, ease of dealing with potential future implant failure, concern for achieving good esthetics and phonetics, ease of home care especially considering the patient history of less than ideal home care and history of periodontitis, and the good long-term results that the author has experienced with the full arch removable unsplinted prosthetic design (Table 4). Over the last 20 years the author has placed over 3,000 implants used for unsplinted overdenture prosthetic designs and has documented an overall survival rate of 96% (97% in the mandible and 91% in the maxilla). To the author’s best knowledge the “prosthetic survival rate” for these designs has been 99% as this design allowed the continual functioning of the prosthesis while any failed implant was replaced and subsequently retrofitted to the original prosthesis.
Patient Consultation:
• Patient Consultation: Informed consent (as described earlier in this article) is achieved to a great extent during the patient consultation. Some specific risk factors pertinent to these two cases have been described above and would include significant loss of hard and soft tissues and a history of Periodontitis which in turn would potentially lead to esthetic, phonetic, hygiene and long-term maintenance issues. All the factors as outlined in the initial patient interview would play a critical role in determining which treatment option would best suit these two particular patients. In addition and in particular the anticipated definitive results can best communicated to the patients with the adjunctive use of accurate representative photographs and especially models demonstrating the different types of prosthetic restorations.
Treatment:
• Treatment Sequence:
1) Preparation of immediate interim dentures.
2) Full mouth extractions with anticipated immediate placement of four implants in the mandible and four to six implants in the maxilla, with a one stage surgical protocol assuming 40 Ncm or more of initial implant stability is achieved.
3) Insertion of the immediate interim dentures with relief, soft relining and adjustments to avoid excessive transmucosal loading on the implants.
4) Verification of successful osseointegration several months (two to six) or more after placement.
5) Definitive prosthetic restoration.
6) Prosthetic and biological maintenance.
Maintenance:
• Maintenance: Home care was greatly facilitated with the unsplinted removable prosthetic design. With the history of less than ideal home care in the past, this could be a significant design factor to facilitate patients efforts to carry out adequate oral hygiene and increase the chances of good home care compliance. A relatively short three-month professional maintenance interval for monitoring and professional cleaning as needed was suggested primarily based on the patient’s history of significant periondontitis.
Summary:
This article has discussed the influence of risk factors and primarily the category of “Patient Related Systemic Risk Factors” as they apply throughout the sequence of therapy and their crucial importance in successfully achieving “Patient Informed Consent”. This article also illustrated two similar cases that incorporated some of the principles and the risk factors discussed in this article. Future articles will illustrate other cases and cover additional risk factors highlighting the other categories as outlined in Table 1.
References:
1. “Generalized aggressive periodontitis as a risk factor for dental implant failure: A meta-analysis”. J. Periodontology 2014; 85: 1398-1407. Monje A, Flores-de-Jacoby L.
2. “The Influence of Systemic Medications on Osseointegration of Dental Implants”, J Can Dent Assoc 2016;82:g7, by Aviv Ouanounou, Siavash Hassanpour and Michael Glougauer
3. “Systemic Administration of Omeprazole interferes with bone healing and implant osseointegration. An in vivo study in the rat tibia”, J. Clin. Perio, 2016, 2:43(2), pgs 193-203, by Al Subaie, A, Emami, E, Tamimi, I, Laurenti, M., Elmar, H., Abdallah, MN and Tamimi, E.
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!









