Bullet points:
1. Definition-orthopedic/functional breathing
2. Comorbidity of orthopedic and facial pain and breathing
3. Answers to our questions
4. Method or technique-paradigm shift
5. Integrating myofunctional techniques
This article defines “Airway Centered Dentistry”, explains the mechanism of chronic face/jaw pain and dysfunction, reviews the technique and triage systems that have been successful in the standardized approach currently utilized in 45 TMJ and Sleep Therapy Centres in seven countries.
Treating chronic pain is a lot like emergency medicine. There is a triage process where structural (orthopedic/dental), metabolic, breathing (functional and obstructive apnea), infectious, and genetic mechanisms are evaluated. When patients are unconscious in the ER the airway, breathing and circulation are evaluated. In the treatment of chronic head pain, we do the same.
I have practiced “Airway Centered Dentistry” (recently defined by Dr. Michael Gelb) for over 25 years in various levels of understanding. Essentially it is defined as a mandibular relationship that produces the optimal orthopedic function of the TM joints and prevents or reduces airway collapse (oropharyngeal) in the unconscious state (sleep). To date, I believe I am the only person to produce peer-reviewed research on those two points.


It is important to define physiologic functional breathing from obstructive sleep apnea (OSA). Proper or physiologic functional breathing is through the nose. Noses are for breathing and mouths are for eating. Breathing through the nose allows for filtering, warming and adding moisture to the inspired air. Every nasal breath mixes Nitric Oxide (NO) gas from the maxillary sinuses and is carried into the lungs. NO is necessary for cilia movement in the sinuses to carry out debris, it is anti-fungal, anti-bacterial, and anti-viral, also is important in peripheral vasodilation of the blood vessels. 1-11 It has been recommended that the final endpoint in treating OSA is restoration of nasal breathing. Nasal obstruction can result in increased blood pressure. Mouth breathing has none of the physiologic protective mechanisms so people with this condition are more prone to respiratory infections as well as the dental sequela (gum disease, anterior openbite).
Establishing and developing patency of the four points of obstruction (Fig. 1) are necessary to prevent orthodontic relapse, (anterior or posterior openbite). This is most evident in cases that have been retained with bonded anterior archwires (Fig. 2) 2. Harvold in his work with primates was the first to demonstrate craniofacial deformations and skeletal openbite with silicon obstruction of their noses. 3
Fig. 1
4 Points of obstruction.

Fig. 2
Anterior openbite with wire fixation max and mand.

Patients with OSA have been shown to lower their blood pressure by utilizing nasal CPAP by restoring levels of NO. Infants born with hypoxemic respiratory failure associated with pulmonary hypertension are treated with inhaled NO. 4
Sleep-Related Bruxism (SB), the grinding and clenching of teeth, is classified as a Sleep-Related Movement Disorder by the International Classification of Sleep Disorders (diagnosis and coding manual [ICSD-3]). 5 SB is reported by approximately 15 percent in the pediatric population and between 8 percent and 31 percent in the general adult population, without a difference in prevalence between the sexes. 6,7 The characteristic electromyography (EMG) pattern of SB is found in repetitive and recurrent episodes of rhythmic masticatory muscle activity (RMMA) of the masseter and temporalis muscles, which are usually associated with sleep arousals. 8
Bruxism in children is associated with forward head posture.9 Expansion of the maxilla increases nasal volume. A recent study quantified the three dimensional increase of volume of the nose with palatal expansion. It was found that there is a 2.36 percent volume increase with each millimeter of transverse expansion (Fig. 3). Another important finding is that this ratio was constant in the population base from nine to 22 year-old patients. 10 This challenges the belief that expansion is not possible in adults.
Fig. 3
2.36% volumetric increase for each mm of expansion. Reprinted with permission Dr. Melih Motro.

Palatal expansion has been shown to reduce apnea, increase nasal volume, correct skeletal deformities related to breathing dysfunction, improve sleep related symptoms such as fatigue, nocturnal enuresis, conductive hearing loss, restore proper functional nasal breathing and up righting head posture. 11-17
OSA is defined as obstruction of the velo or oropharynx (collapse of the muscular walls) in the unconscious state that results in cessation of breathing for 10 seconds (apnea) or a blood oxygen desaturation of 3-4% (hypopnea).
My entry to this field came by treating people with chronic head, neck and facial pain complaints. Disturbed sleep and pain often co-exist and the relationship between the two conditions is complex and reciprocal. A five-year prospective study examined whether disturbed sleep can predict the onset of multi-site pain, and whether non-disturbed sleep can predict the resolution of multi-site pain. There were almost 1,600 people in this study that found individuals with no pain at baseline, had a significantly higher odds ratio for multi-site pain five years later was seen for reporting worst sleep [odds ratio (OR) 4.55; 95% confidence interval. They concluded that sleep could be relevant for predicting both the onset and the resolution of multi-site pain. It seems to be a significant factor to include in research on multi-site pain and when conducting or evaluating intervention programs for pain.18 So pain disturbs sleep and lack of restful sleep increases inflammation and results in greater pain during the day (Fig. 4).
Fig. 4

Twenty years ago, I recognized the need to treat patients with oral appliances for their airway collapse (apnea/hypopnea/OSA) problems. Through review of the literature, clinical practice, and research I have conducted we understand that most facial pain and jaw joint pathology is the result of repetitive micro-trauma. These conditions also prevent complete healing from a macro-trauma to the face or jaw. An underlying pathologic process like an obstruction in proper functional breathing (nasal obstruction) can result in mouth breathing and bruxism. The facial pain is the result of the clenching and grinding and fatigue from holding the mouth open to breathe.
Research has demonstrated that chronic face/jaw pain, and primary headaches (migraine, tension type, and cluster) have a high comorbidity with OSA (obstructive sleep apnea) and functional breathing disorders. 19 Patients with OSA are 3.6 times more likely to have TMD. 20
In a study published in the American Journal of Dentistry 2016, of almost 1,200 patients we found that patients with sleep related fatigue measured by an Epworth scale greater than six were 1.39 times more likely to have jaw locking and primary headaches. This is the first paper to link jaw locking to sleep related fatigue. 21 Sleep related fatigue (excessive daytime sleepiness) is more often the result of nasal obstruction (mouth breathing), than OSA. 22
Patients with OSA often also have a functional breathing problem (nasal obstruction).
The A, B, C’s Of Treatment
It should now be clear that patients who have chronic facial/jaw pain likely have either a functional breathing problem (nasal obstruction) or OSA or both.
The “Pearls” in treating Craniofacial Pain & OSA comorbities is to control:
1. Inflammation
2. Parafunctional Activity (decompression appliance therapy)
3. Prevent Airway Collapse and restore proper functional (nasal) breathing
4. Nutrition
Triage begins with evaluation of the airway (oropharynx/velopharynx), functional breathing (nasal evaluation) as well as the orthopedic TM joints. I authored an overview of this process that was published in the Journal of Orthodontic Practice 2015 (CBCT in the evaluation of airway – minimizing orthodontic relapse). 23
A functional breathing problem can be as simple as a collapsed nasal valve or more complicated with skeletal blockage of concha bullosa (enlarged middle turbinates) and soft tissue hypertrophy (tonsils and adenoids) as shown in Figures 5 to 7.
Fig. 5

Fig. 6

Fig. 7

The definition of craniofacial pain is inclusive of musculoskeletal pain, orthopedic inflammatory disorders of the jaw (TMD), tooth and oral structures, neuropathic disorders and primary headaches (migraine and tension-type).
When treating craniofacial pain it is all about getting the head up.
Forward head posture can also be the result of inflammation (capsulitis) of the TM joints. Proper decompression of the jaw can result in up-righting of the head.
For every inch the head is forward of the shoulders it adds approximately 10 pounds of weight to the cervical and lumbar spine. The compressive load can result in osteoarthritis and nerve entrapment. 24 Craniofacial pain and internal derangement of the TM joints (TMD) manifests in forward head posture. 25 The most common symptom of painful jaw joints is occipital cephalalgia at 94%. 26 The FHP is secondary to painful swallowing a postural adaption to injury. The injury described is in the absence/or in addition to a macro-trauma, and is the result of repetitive jaw compression (bruxism) originated by sympathetic stimulation during sleep. The patient wakes with temporal headaches and facial pain and jaw joint inflammation that now produces postural compensation. The cantilever strain of FHP, the result of extensor muscles of the neck (trapezius, splenius capititus, semispinalis capititus), produces acute inflammation at their tendon insertions on the occiput. Decompressing inflamed jaw joints utilizing oral appliances, produced with a phonetic technique, has found to upright the head 4.43 inches on average of a population of patients aged 13-74. This relates to relief of close to 45 pounds of weight from the cervical and lumbar spine. 27 Uprighting the head can eliminate the need for common therapies for migraine, which include botox injections for the tendon insertions on the occiput of the skull as well as the mouth closing muscles (temporalis and masseter), or severing the greater and lesser occipital nerves (often entrapped by the extensor muscle tendons they pass through).
Fig. 8
Pre-treatment.

Fig. 9
Eight weeks into treatment.

Increasing Oral Volume And Preventing Airway Collapse (Vertical And Phonetic Bite)
In situations where the patient has decreased lower face height and or deep overbite they suffer from a reduced oral volume. These patients often present with canted plane of occlusion, which can predispose the patient to unilateral TM joint pathology (Fig. 10). These conditions require increasing the oral volume in a three-dimensional way. Understanding that increases in volume can require small 3D changes rather than the traditional linear techniques of opening (vertical), protrusive and lateral movements. In reality these movements are not linear and are best described as pitch (AP cant), roll (Lateral cant) and yaw (rotational cant). The coined term “Airway Centered” is a physiological 3D positioning that prevents airway muscle collapse and increases oral volume, while improving orthopedic positioning and function of the TM joints. This technique is known as the Sibliant Phoneme Registration, which has been shown to prevent airway collapse in adults and currently is being researched for pediatric OSA patients. 29 Preventing airway collapse is key in the treatment of obstructive apnea (Fig. 11). 30
Fig. 10
Cant of plane of occlusion in patient with AHI 118.

Fig. 11

Using the Sibilant Phoneme position as a starting point for vertical stabilization corrects medio-lateral cant asymmetries so it is an ideal technique for appliances or materials added to teeth to increase vertical (Planas’ Tracks or development/expansion appliances). 31 The increased vertical is beneficial for inflammatory conditions of the TM joints, which is often comorbid with sleep breathing disorders in children. Uneven loading of the TM joints in these asymmetric conditions may lead to craniofacial deformity. One in six children and adolescents have clinical signs of TMJ disorders.
Myofunctional Therapy For Maxillary Arch Development
Exercises for the tongue and skeletal muscles has been shown to be effective in the treatment of OSA. 32 The tongue must have the ability for proper movement in swallowing, breathing, chewing and speech. Evaluation for tongue-tie is an important step and should be identified as early as possible. Tongue-tie can result in pathology as early as breast feeding and lead to craniofacial deformities and sleep breathing disorders as it fails to develop the palate normally. 33 In a normal swallow the dorsum of the tongue presses against the palate to develop the maxilla.
Case Study
A 24-year-old woman with closed lock (24 mm opening) with chronic facial pain following wisdom tooth extractions two years previous to our evaluation. She had additional complaints of jaw pain, pain when chewing, ear pain, and daytime fatigue. History of bilateral TM joint arthrocentesis, splint therapy, physical therapy. Medications at time of examination: doxycycline (antibiotic), Prioxicam (NSAID), amitriptyline (tricyclic anti-depressant). Anterior open bite developed after extractions (Figs. 11-15). Previous orthodontic therapy showed good resuls as a teenager. The patient had a history of multiple awakenings. A polysomnography was performed and she was negative for OSA, but had a functional (nasal) breathing problem. She was told that
she needed a bilateral total joint replacement for her condition.
Fig. 12

Fig. 13

Fig. 14

Fig. 15

Twelve weeks of treatment with day and night orthotics produced using the sibilant phenome registration technique (Figs. 16 & 17), MLS laser therapy (BioResearch Inc.), prolo injection for the TM joint resolved the facial pain and limited opening (50 mm). The day appliance was weaned away from the patient and she had nasal & tonsil surgery. Fatigue was 90 percent improved after nasal surgery.
Fig. 16

Fig. 17
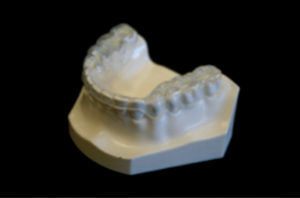
Myofunctional therapy utilizing a Myobrace appliance (TMJ-Mouth Breather Version from Myofunctional Research Co.), was begun after nasal surgery and the anterior open bite was closed in three months without return of symptoms and now can sleep through the night (Figs. 18-21).
Fig. 18

Fig. 19

Fig. 20
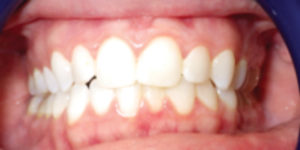
Fig. 21

CBCT imaging (iCat Flex- Imaging Sciences) demonstrates the changes in nasal airway volume and the healing of the osteoarthritis of the left condyle (Figs 22-25).
Fig. 22

Fig. 23

Fig. 24
Post-Surgery with proper nasal channeling.

Fig. 25
Osteoarthritis of the left condyle.

Fig. 26
Regenerated condyle 12 weeks after start of treatment.

I diagnosed this patient at the University of Tennessee Craniofacial Pain & Sleep Clinic & referred to Dr. Daniel Klauer of the TMJ & Sleep Therapy Centre of Northern Indiana. I finished the case with Myofunctional therapy. This case demonstrates an easy transfer of care utilizing a standard protocol developed and taught through the Mini-Residency of the T & S Therapy Centre International. OH
Oral Health welcomes this original article.
References
1. Guilleminault C, Sullivan SS. Towards Restoration of Continuous Nasal Breathing as The Ultimate Treatment Goal in Pediatric Obstructive Sleep Apnea. 2014 Pediatr Neonatol Biol 1(1): 001.
2. 39 Olmos S. CBCT in the evaluation of airway-minizing orthodontic relapse. Journal Orthodontic Practice. 2015; volume 6, number 2.
3. Harvold E, Tomer BS, Vargervik K, Chierici G. Primate experiments on oral respiration. Am J Orthod. 1981;79(4):359-372.
4. Todd Tzanetos DR, Housley JJ, et al. Implementation of an Inhaled Nitric Oxide Protocol Decreases Direct Cost Associated With It’s Use. Respiratory Care • May 2015Vol 60No5
5. Svensson P, Arima T, Lavigne G, et al. Sleep Bruxism: Definition, Prevalence, Classification, Etilology, and Consequences. In: Kryger MH, Roth T, Dement WC. Principles and Practice of Sleep Medicine 6th edition. Philadelphia, PA, Elsevier Saunders. 2017;1423-26.
6. Carra MC, Huynh N, Morton P, et al. Prevalence and risk factors of sleep bruxism and wake-time tooth clenching in a 7- to 17-yr-old population. Eur J Oral Sci 2011;119:386-394.
7. Manfredini D, Winocur E, Guarda-Nardini L, et al. Epidemiology of bruxism in adults: a systematic review of the literature. J Orofac Pain. 2013 Spring;27(2):99-110.
8. Huynh N, Kato T, Rompre PH, et al. Sleep bruxism is associated to micro-arousals and an increase in cardiac sympathetic activity. J Sleep Res 2006;33:1711-1716.
9. Velez AL, Restrepo CC, Pelaez-Vargas A, et al. Head posture and dental wear evaluation of bruxist children with primary dentition. J Oral Rehabil. 2007 Sep;34(9):663-70.
10. Motro M, Schauseil M, Ludwig B, et. al. Rapid-maxillary expansion induced rhinological effects: a retrospective multicenter study. Eur Arch Otorhinolaryngol; online publishing April 2015, Springer.
11. Pirelli P, Saponara M, Guilleminault. Rapid Maxillary Expansion in Children with Obstructive Sleep Apnea Syndrome. SLEEP 2004; 27(4):761-6.
12. Marino A., Ranieri R, Chiarotti F, et. a. Rapid maxillary expansion in children with Obstructive Sleep Apnoea Syndrome (OSAS). European Journal Of Paediatric Dentistry: Official Journal Of European Academy Of Paediatric Dentistry [Eur J Paediatr Dent] 2012 Mar; Vol. 13 (1), pp. 57-63.
13. Usumez S; Işeri H; Orhan M; Basciftci FA. Effect of rapid maxillary expansion on nocturnal enuresis. [Angle Orthod] 2003 Oct; Vol. 73 (5), pp. 532-8.
14. Schütz-Fransson U; Kurol J. Rapid maxillary expansion effects on nocturnal enuresis in children: a follow-up study.The Angle Orthodontist [Angle Orthod], ISSN: 0003-3219, 2008 Mar; Vol. 78 (2), pp. 201-8
15. Eichenberger, M; Baumgartner. The impact of rapid palatal expansion on children’s general health: a literature review S. EUROPEAN JOURNAL OF PAEDIATRIC DENTISTRY; MAR, 2014; 15; 1; p67-p71
16. Cerruto C; Di Vece L; Doldo T; Giovannetti A; Polimeni A; Goracci C. A computerized photographic method to evaluate changes in head posture and scapular position following rapid palatal expansion: a pilot study.The Journal Of Clinical Pediatric Dentistry [J Clin Pediatr Dent], ISSN: 1053-4628, 2012 Winter; Vol. 37 (2), pp. 213-8
17. McGuinness NJ; McDonald JP. Changes in natural head position observed immediately and one year after rapid maxillary expansion. European Journal Of Orthodontics [Eur J Orthod], ISSN: 0141-5387, 2006 Apr; Vol. 28 (2), pp. 126-34
18. Aili K; Nyman T; Svartengren M; Hillert L. Sleep as a predictive factor for the onset and resolution of multi-site pain: a 5-year prospective study. European Journal Of Pain (London, England) [Eur J Pain], ISSN: 1532-2149, 2015 Mar; Vol. 19 (3), pp. 341-9
19. Olmos S. Comorbidities of chronic face pain and obstructive sleep apnea. Current Opinions in Pulmonary Medicine. Volume 22, Number 6, November 2016.
20. Sanders AE, Essick GK, Fillingim R, et al. Sleep apnea symptoms and risk of temporomandibular disorder: OPPERA cohort. J Dent Res 2013; 92:70S-77S
21. Olmos S, Garcia-Godoy F, Hottel T, Tran N. Headache and jaw locking comorbidity with daytime sleepiness. American Journal of Dentistry, Vol. 29, No. 3, June 2016.
22. Hussain SF, Cloonan YK, et al. Association of self-reported nasal blockage with sleep-disordered breathing and excessive daytime sleepiness in Pakistani employed adults. Sleep Breathing (2010) 14:345-351.
23. Olmos S. CBCT in the evaluation of airway – minimizing orthodontic relapse. Journal Orthodontic Practice (2015). Volume 6 Number 2:46-49.
24. Cailliet R. In: Head and Face Pain Syndromes. 1992 F.A. Davis Company.
25. An J, Jeon D, Jung W, et al. Influence of temporomandibular joint disc displacement on craniocervical posture and hyoid bone position. Amer J Ortho & Dentofacial Orthopedics. January 2015;147(1):72-79.
26. Simmons HC, Gibbs SJ. Anterior Repositioning Appliance Therapy for TMJ Disorders: Specific Symptoms Relieved and Relationship to Disk Status on MRI. J Tennessee Dental Association, September 2009, 89(4):22-30
27. Olmos S, Kritz-Silverstein D, et al. The Effect of Condyle Fossa Relationships on Head Posture. Cranio January 2005, 23(1):48-52)
28. Moeller JL, Paskay LC. Gelb M. Myofunctional Therapy: A Novel Treatment of Pediatric Sleep-Disordered Breathing. Sleep Medicine Clinics June 2014.
29. Singh D, Olmos S. Use of the Sibilant Phoneme Registration protocol to prevent upper airway collapse in patients with TMD. Sleep and Breathing Dec 2007.
30. Ng AT, Qian J, Cistulli PA. Orophayrngeal collapse predicts treatment response with oral appliance therapy in obstructive sleep apnea. Sleep. 2006 May 1;29(5):666-71.
31. Rivera-Morales WC, Mohl ND. Anteroposterior and mediolateral variability of the closest speaking space. Int J Prosthodont 3:2, 179-84, Mar-Apr 1990.
32. Guimaraes KC; Drager LF; Genta PR; Marcondes BF; Lorenzi-Filho G. Effects of oropharyngeal exercises on patients with moderate obstructive sleep apnea syndrome. American Journal of Respiratory & Critical Care Medicine, May2009; 179(10): 962-966. (5p)
33. Olivi, G.; Signore, A.; Genovese, M.D.; Olivi, M. Lingual frenectomy: Functional evaluation and new therapeutical approach European Journal of Paediatric Dentistry, 2012, 13(2):101-106
34. Cunali PA; Almeida FR; Santos CD; Valdrichi NY; Nascimento LS; Dal-Fabbro C; Tufik S; Bittencourt LR. Mandibular exercises improve mandibular advancement device therapy for obstructive sleep apnea.
35. Sleep & Breathing = Schlaf & Atmung [Sleep Breath], ISSN: 1522-1709, 2011 Dec; Vol. 15 (4), pp. 717-27
About the Author
 Dr. Steven Olmos has been in private practice for more than 30 years, with the last 20 years devoted to research and treatment of craniofacial pain, temporomandibular disorder (TMD), and sleep-disordered breathing. He obtained his DDS from the University of Southern California
Dr. Steven Olmos has been in private practice for more than 30 years, with the last 20 years devoted to research and treatment of craniofacial pain, temporomandibular disorder (TMD), and sleep-disordered breathing. He obtained his DDS from the University of Southern California
School of Dentistry and and is Board Certified in both chronic pain and Sleep Related Breathing Disorders by the American Board of Crainofacial pain, The American Academy of Pain Management, American Board of Dental Sleep Medicine, and American Board of Craniofacial Pain and Dental Sleep Medicine.
Dr. Olmos is the founder of TMJ & Sleep Therapy Centres International, with over 40 licensed locations in seven countries dedicated exclusively to the diagnosis and treatment of craniofacial pain and sleep disorders. Dr. Olmos is an adjunct professor at the University of Tennessee School of Dentistry, where his system of diagnosis and treatment is utilized at the school’s Sleep Breathing & Craniofacial Pain Center. He is currently the president of the American Academy of Craniofacial Pain.












