Abstract
This case report demonstrates the importance of careful diagnosis and treatment planning to effectively treat a worn dentition in a conservative manner while maximizing the long-term prognosis. The patient presented having completed orthodontic treatment with a significantly worn dentition seeking an aesthetic improvement. A comprehensive evaluation of the patient occurs to determine the etiology of the moderately worn dentition. The treatment plan was driven by the dominant risk factors of aesthetics and function. Treatment goals included lengthening maxillary teeth, leveling the posterior occlusal planes, opening the vertical dimension of occlusion, and establishing equal intensity bilateral simultaneous posterior occlusion. Aesthetic parameters were established with the maxillary arch, enabling the functional goals to be addressed with treatment in the mandibular arch.
Introduction
Tooth structure loss is a multifactorial phenomenon. When evaluating a worn dentition, the first question the clinician should ask is: how did this happen? That is to say, what is the etiology of the worn dentition the patient presents with? Pathological tooth wear can be thought of as the loss of tooth structure from causes other than mastication. However, not all tooth structure loss should be considered pathological requiring intervention. 1 Occlusal attrition occurs resulting in the vertical loss of enamel at a rate of approximately 10.7 um per year. 2 To put this into perspective, we should expect patients to wear approximately 1 mm of enamel every 100 years due to normal function. Tooth wear can be lumped into one of two categories; physical or chemical. Physical causes would include attrition (loss of tooth structure resulting from tooth to tooth contact) and abrasion (loss of tooth structure resulting from friction between a tooth and some type of exogenous material, i.e. toothbrush, toothpick, smokers pipe, etc.). Chemical causes include erosion (wear from corrosion due to acid exposure from an endogenous or exogenous source), and perimolysis (demineralization from acid followed by abrasion). 3
Managing and restoring the worn dentition becomes challenging for most dentists for a multitude of reasons. Treating such patients takes many dentists out of their comfort zone. The complexity of the treatment required is quite high involving a significant number of teeth. Many times there is inadequate tooth structure to restore or little space for the restorations in the patients’ current vertical dimension of occlusion. This creates the need to alter the vertical or create an interdisciplinary treatment plan involving an orthodontist or surgeon to aid in the overall execution of the treatment. As well, the long-term prognosis of such cases comes into question. The fear of fractured porcelain, fractured teeth, and other prosthetic complications can make it very intimidating to begin treating these patients. Tooth wear becomes extremely troubling to see when it presents itself in a young patient, as the stakes are much higher. When significant tooth structure loss occurs in a young patient, the long-term prognosis of that patient’s dentition becomes dubious at best.
In order to restore a worn dentition to ideal aesthetics and function, full coverage crowns have traditionally been recommended. Crown preparations increase the risk of an irreversible pulpitis or pulpal necrosis and necessity for endodontic therapy. 4 As well, the preparations themselves can leave the dentition at greater biomechanical risk of fracture. 5 This necessitates the replacement of the crowns over time creating a domino effect that can eventually lead to partial edentulism. All dental interventions have a limited lifespan whereby its replacement typically removes more tooth structure, leaving the patient at an even greater biomechanical risk. It stands to reason that the less tooth structure that is removed in order to restore a patient, the greater the long-term prognosis of the dentition. In essence, the goal of treatment should be to minimize the risk of tooth loss by transferring the risk from the tooth to the restorative material.
The purpose of this article is to present a case study in which a young patient with a worn dentition was treated in a conservative fashion using a combination of porcelain restorations on the first molars, porcelain veneers for the maxillary incisors and composite restorations in order to create occlusal harmony by distributing occlusal forces. This will satisfy the patient’s aesthetic wishes as well as the author’s goal of a functional reconstruction while minimizing tooth structure removal.
Clinical Case Overview
A 24-year-old male presents stating aesthetics as his chief concern. He especially disliked his aged appearing worn dentition (Figs. 1, 2). His medical history was non-contributory. A complete examination was performed including periodontal, functional, biomechanical and aesthetic evaluation. His dental history included regular recall visits with minor restorative therapy. As well he underwent orthodontic therapy on two separate occasions to correct his Angel class 3 malocclusion. He was first treated as a teenager with fixed orthodontic appliances. Due to continued growth and development and possibly a slight amount relapse, he required a second orthodontic intervention but was unwilling to go through traditional fixed appliances. As such, his orthodontist prescribed and completed Invisalign therapy.
His periodontal status was healthy, stable and could be considered low risk with an excellent prognosis. All probing depths were 3 mm or less and no bone loss could be visualized radiographically.
Biomechanically, no active carious lesions were noted. However, he displayed moderate risk due to the erosive nature of the tooth wear present with a guarded prognosis.
Functionally it was difficult to determine an exact occlusal diagnosis. The orthodontic tooth movement made it difficult to determine the exact nature of his tooth structure loss (frictional vs. chemical) as the wear facets on opposing teeth no longer coincided. There was a definite erosive component to his tooth structure loss as evidenced by the cupped appearance on the occlusal surfaces of his posterior dentition. There was also noticeable generalized wear in both the anterior and posterior dentition. He was considered to have a non-physiological occlusion, more specifically occlusal dysfunction with a history of a constricted envelope of function that was corrected through the orthodontic interventions. His temporomandibular joints were examined and determined to be healthy. He exhibited a normal range of motion and his maximum opening was within normal limits. His joints also accepted load without eliciting any pain. The patient did not have nocturnal parafunction or a neurologic disorder and as such is considered to have a moderate functional risk with a guarded prognosis. The patient understood based on our discussions, as well as those with his orthodontist, that traditional fixed appliances possibly in conjunction with orthognathic surgery to correct his Angle class 3 would potentially be an ideal option. However, he was unwilling to undergo a third orthodontic intervention and would not entertain jaw surgery as his profile was overall pleasing. This allowed for a treatment plan that would involve opening the vertical dimension of occlusion (VDO) in order to create the required restorative space in the anterior while replacing the lost tooth structure in the posterior dentition.
Aesthetically, he is high risk to treat as this was his chief concern. As well, he displays high lip dynamics fully exposing the periodontium in a full smile (Figs. 1, 2). The aesthetics prognosis is good. With lips in repose, very little of his maxillary incisors are displayed due to the severe nature of his wear (Fig. 3). His maxillary central incisors were approximately 8 mm in length (Fig. 4) while the average length of a maxillary central incisor is 10-10.5 mm.
Fig. 1

Fig. 2

Fig. 3

Fig. 4

When treating a patient by altering the VDO it is necessary to create a therapeutic occlusion that can predictably function in harmony with a healthy musculature and TMJ’s. In order to achieve this, the author’s bias is to restore the patient to the orthopaedic jaw position of centric relation (CR) at the appropriate vertical. The rationale for using centric relation is as follows. Centric relation is a reference position, unrelated to tooth position that provides a reproducible hinge position, which can be recorded with a high degree of accuracy. There are many methods of accurately recording CR including the use of an anterior deprogrammer. An anterior deprogrammer discludes the posterior teeth creating an environment in which the elevator muscles relax allowing a healthy TMJ to settle into centric relation. In order to determine CR, initial treatment began by fabricating an anterior deprogrammer. A chairside fabricated anterior deprogrammer was added to the lingual of a composite mock-up used to determine if average length central incisors would satisfy the aesthetic goals of the patient (Fig. 5). With lips in repose, the patient displayed an appropriate amount of his central incisor. This was pleasing to the patient. After allowing some time to elapse to ensure the patient was in fact in CR by noting a consistent contact point on the anterior step (Fig. 6) when the patient is asked to close unassisted. This provided confidence that the patient’s condyles were, in fact, rotating along the hinge axis without translation. It should be stressed that at this point in treatment planning we have established our proposed maxillary incisal edge position, we are confident we have the patient in a CR position, we have created increased the VDO enough to accommodate the restorative space required. All that is left is to create records that will communicate this information to the dental laboratory in order to mount casts onto a semi-adjustable articulator. The Kois Dento-Facial Analyzer was used to record the position of the maxillary arch in relation to an arbitrary hinge position while parallel to the plane of occlusion. This record will be used to mount the maxillary cast onto a Panadent© articulator. An interocclusal record was made with a quick setting bite PVS material to capture the relationship of the maxillary and mandibular arch in CR at the proposed VDO. This interocclusal record is used to mount the mandibular cast to the maxillary cast on the articulator with the pin set to zero. Once the worn cusps in the posterior dentition are restored, sufficient restorative space will be established to provide the patient with conservative porcelain veneers to restore the maxillary incisors (Figs. 7, 8). The laboratory was instructed to provide an aesthetic functional wax-up by adding the worn tooth structure in wax without preparing any teeth on the mandibular cast nor any teeth distal to the maxillary lateral incisors as well as to idealize the aesthetics of the maxillary incisors (Fig. 9) and fabricate clear matrices. The clear matrix enclosed with the completed wax-up was utilized by loading bis-GMA temporary resin material into it and seating it over the maxillary dentition allowing it to polymerize fully for an esthetic evaluation. After the overall shape and length of the proposed teeth were approved, the bis-GMA mock-up was removed and the patient was scheduled to begin treatment.
Fig. 5

Fig. 6

Fig. 7

Fig. 8

Fig. 9

Although there are plenty of ways to sequence a treatment plan to achieve the desired result, I will outline the sequence chosen to treat this specific patient once a diagnosis and treatment plan was established. In one appointment the VDO was increased by the desired amount to create adequate restorative space for average-sized maxillary central incisors. To facilitate this, a clear matrix (clearly affinity – Clinicians choice) of the wax up provided by the laboratory was used as a guide for a direct bonding (Figs. 10-12). Prior to final polishing of the composite restorations, the patient was equilibrated ensuring bilateral equal intensity simultaneous contacts in CO. This left the patient with an anterior open bite (Fig. 13). Another set of alginate impressions, as well as an interocclusal record, was made in MIP which is currently coincident with CO was sent to the lab in order to wax maxillary incisors to ideal contours. The lab was asked to provide a matrix to aid in the fabrication of provisional veneers as well as a preparation guide to minimize the amount of tooth structure removed. The patient was appointed the following week to start treatment of his maxillary incisors. At the next appointment, the patient had an opportunity to communicate with us how he was adapting with his new occlusal configuration. As he was completely asymptomatic and comfortable with his new bite we were confident to proceed to treat his maxillary anterior teeth. After providing profound local anaesthesia a provisional matrix loaded with bisacryl was used in order to visualize the desired contours of the final result. To be as conservative as possible, the preparation was started through the bisacryl allowing us to minimize the reduction necessary while satisfying the minimum dimensions required for material thickness (Fig. 14). An algorithm discussed in a previous article was used to determine the most appropriate prep design.5 Thin gingival retraction cord allowed for predictable impressions (Fig. 15) with a light and heavy body PVS material (3M Imprint) in a stock plastic tray. This process is repeated a second time and both final impressions of the preparations are evaluated. The impression deemed most accurate is sent to the laboratory for fabrication of the final porcelain restorations. The other less accurate impression is poured up with quick setting stone. Once set, a separating medium is painted over the stone cast and the provisionals were fabricated and polished indirectly ready for insertion. An appropriate shaded flowable resin is utilized to lock the temporary in place. If retention is questionable spot etching and adhesive application of the teeth can be considered. The provisional phase gives the patient a preview of the final result and provided the clinician an opportunity to make any necessary modifications. At the insertion appointment, the provisional is removed, and the preparations are cleaned with pumice. The restorations are tried in with water to verify marginal fit and shade. The veneers are bonded using an adhesive system (3M Universal Bond) with a light activated resin cement (3M RelyX Veneer) (Fig. 16). Excess cement is removed, and bilateral equal intensity simultaneous contacts in centric are confirmed. A follow-up appointment is made in one-week to again confirm occlusal harmony and to ensure the patient is pleased with the final aesthetic result (Fig. 17, 18). In order to minimize the risk of frictional wear of the composite itself, it is stressed that the patient has all four first molars restored in porcelain to act as functional occlusal stops. After four years, the patient did indeed have his first molars restored with porcelain and has experienced no breakdown to date.
Fig. 10

Fig. 11

Fig. 12

Fig. 13
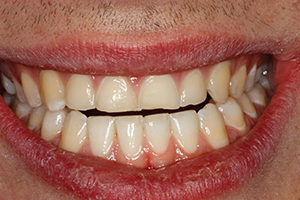
Fig. 14

Fig. 15

Fig. 16

Fig. 17

Fig. 18

Fig. 19

Discussion
All reconstructive cases must begin with the end in mind. To be able to visualize the end result prior to embarking upon the treatment of a patient is as important than the execution of the treatment plan. The most challenging aspect of this particular case was in the occlusal diagnosis itself. Once the patient has undergone orthodontics the etiology of wear becomes difficult to diagnose. Existing wear facets that would have provided vital clues were in a sense covered up. The other issue is that it is difficult to determine if the wear occurred solely in the pre-orthodontic occlusal configuration or if the wear is in fact actively occurring. In this particular case, it was not as relevant as the patient required a restorative intervention due to his displeasure with aesthetics. Prior to restoring a worn anterior dentition with porcelain veneers, a non-destructive therapeutic occlusion should be considered a prerequisite. Occlusal stability is necessary in order to have confidence that the aesthetic rehabilitation will have a good long-term prognosis. A predictable way to achieve occlusal stability is to equilibrate a patient in centric relation. This creates a situation where maximum intercuspation is coincident with centric occlusion, in a mutually protective occlusal scheme. Equilibrations can be additive, subtractive, or a combination of both approaches. In order to conserve as much tooth structure as possible, an additive occlusal equilibration can be provided using composite resin to achieve occlusal stability. Once the occlusion is stable at the minimally increased vertical the patient is at relatively low risk of further occlusal breakdown in the short term. As the posterior composites begin to wear over time, the envelope of function begins to constrict putting the anterior porcelain restorations at risk of chipping and breakdown. In order to minimize this occurrence, it is suggested that the first molars are restored with porcelain. This can be accomplished with full coverage cohesively retained crowns or with adhesively retained porcelain onlays.
Conclusion
While bonding with composite material is a relatively new concept to restore a worn dentition in North America it is a technique that has been used successfully and with good long term success in many Scandinavian countries as a permanent solution to the worn dentition. The goal of this case study is to have the reader consider using bonding with composite resin to transition through an oral reconstruction in a relatively conservative and cost effective manner. OH
Dr. Joseph Fava earned his DDS, MSc. and prosthodontics specialty certificate at the University of Toronto. His MSc focused on dental implants in the aesthetic zone. He currently instructs at the IPU at the University of Toronto and is actively involved in clinical research. He maintains a speciality practice in Yorkville, whose scope includes cosmetic dentistry, surgical and prosthetic components of dental implants as well as advanced restorative and reconstructive full-mouth therapies. He is a distinguished Kois Mentor and co-director of the University of Toronto’s Implant Residency Program.
Oral Health welcomes this original article.
References
1. Kaidonis JA. Tooth wear: the view of the anthropologist. Clinical oral investigations. 2008 Mar 1;12(1):21-6.
2. Pintado MR, Anderson GC, DeLong R, Douglas WH. Variation in Tooth Wear in Young Adults Over a Two-Year Period, mally peutee via skill that is l J Prosthet Dent 1997;77:313-320
3. Lussi, Adrian, ed. Dental erosion: from diagnosis to therapy. Vol. 20. Karger Medical and Scientific Publishers, 2006.
4. Whitworth JM, Walls AW, Wassell RW, Crowns and extra-coronal restorations: endodontic considerations: the pulp, the root-treated tooth and the crown. Br Dent J, 2002 Mar 23; 192(6): 315-20, 323-7
5. Fava, J. Porcelain Therapy: Veneers vs Jacket Crowns, the ALARA Principle for Prosthodontics. Oral Health Nov 2015
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












