To ensure long-term success, a greater understanding of occlusal concepts needs to be incorporated into the restorations we provide our patients. We must ensure that the beautiful smiles we create today will hold up to the rigors of mastication and occlusal forces well into the future.
Fixed restorations have come a long way since the early days of cast gold restorations with pyroplast (acrylic) facings. New materials are being developed and techniques are simplified to make these material advances more economical and viable to the dental community. Beautiful, lifelike reproductions of teeth (Fig. 1) can be created with a variety of different materials, such as:
- porcelain fused to metal
- porcelain layered onto zirconia
- full contour zirconia
- lithium disilicate glass-ceramic
- polymer glass
As well, restorations can be fabricated in many forms, i.e. being cemented onto natural teeth or implant abutments. They can also be designed as one-piece, screw-retained implant restorations with occlusal access holes. But what about function?
Fig. 1
Central Incisor Aesthetic Restorations.

Improper occlusal relationships can be a major cause of failure, not just to the teeth, but to the entire oral maxillofacial complex. When teeth do not function in harmony with each other, more is at stake than just the teeth or the restorations that are fabricated to replace them. Yes, teeth and crowns can break or chip to avoid the interferences created, however, greater problems can manifest over time. Many of today’s restorations are being fabricated out of harder and stronger materials that resist fracture. Occlusal forces are being directed away from the teeth to other areas of the system. The muscles of mastication can be put under stress, leading to clenching and grinding, which can further exasperate the situation. Temporal mandibular joints can be diverted from their optimal movements causing pain and discomfort. As well, with prolonged muscle strain, skeletal changes can occur, which puts further strain on the entire neuromuscular system.
Teeth need to work and function in harmony with each other. 1 They must provide for maximum interdigitation in function and working contacts. 2 At the same time, they must allow for the free range of motion provided by the reduction of interferences in excursive movements. 3,4 This means providing restorations that require minimal occlusal adjustments.
Through discussions with dentists for almost thirty years, we found the number one complaint with fixed restorations, regardless of the material selected, is the excessive time loss associated with adjusting the occlusion or even having to grind in the bites. But why does this occur? Can we not capture a proper occlusal relationship?
To overcome the need to make excessive occlusal adjustments, some clinicians have requested that their restorations be fabricated with varying thicknesses of metal foil placed on the opposing teeth to the restoration being fabricated (Fig. 2). 5 This will create a space, and depending on the cause of the interference, may provide enough relief to keep the restoration out of occlusion and prevent the need to adjust the restoration. However, it does not address the root cause of the issue and results will vary. This can leave the restoration either in hypo-occlusion or too far out of occlusion, and allow the undesirable consequence of tooth over eruption. 6
The vast majority of fixed restorations are still being fabricated on casts mounted on some type of articulator to allow the simulation of movement of the mandible. These casts have generally been made of low expansion, resin-reinforced, dental gypsum products; however, as dentistry progresses into the digital age, these models can now be printed out of resins (Fig. 3).
Fig. 2
Foil On Opposing Teeth.

Fig. 3
Poured Stone Model Over Resin Printed Model.

To capture the relationship between the maxillary and mandibular arches, an intra oral bite registration is taken. Once again, depending on whether the clinician is taking physical impressions or digital scans of the arches, a physical or digital bite registration will be acquired.
There are a number of bite registration techniques that can be utilized for the fabrication of fixed restorations, which are based on a variety of different philosophies such as Centric Occlusion, Centric Relation, Neuromuscular-Based Occlusion, or Joint-Based Occlusion. Depending on the philosophy that is being followed and the technique provided, today’s dental laboratories need to be able to mount the supplied models, using the various bite registrations, on a variety of different types of articulators.
This new millennium has brought together more precise articulators (Fig. 4), so that in conjunction with simpler face bow procedures (Fig. 5), function can now be achieved with greater accuracy and consistency. 7 Lateral and protrusive interferences can be taken into consideration during restoration fabrication. Still, the vast majority of restorations are fabricated on simple metal fixed hinge axis articulators (Fig. 6) or plastic disposable hinges, with only centric occlusion measurements provided. These simple articulators do nothing to relate the dentition to the patient’s condyles or to the base of the skull, and thus provide none of the information needed to create free function. They are simple and inexpensive, and they lack the necessary information that is needed to ensure interferences are not inadvertently built into our restorations. Be it fully adjustable or simple articulators, neither address the concern of pre-maturities in occlusion, which hold the casts apart once they are mounted.
Fig. 4
Kavo Protar Articulator.

Fig. 5
Kavo Arcus Face Bow.

Fig. 6
Standard Hinge Articulator.

With all mounted models, regardless of the method with which the arches are captured and regardless of the articulating instrument that relates these models to each other, interferences in the occlusion will most likely occur. These interferences can take the form intraorally, as natural high spots in occlusion, where a tooth or several teeth contact prematurely in occlusion. Usually due to the periodontal ligaments, these teeth with premature contacts can depress into their sockets or move laterally out of the way.
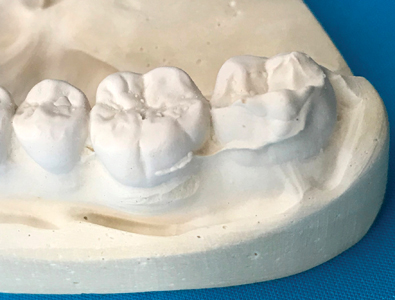
Sometimes these interferences are the result of inaccuracies with the impressions provided (Fig. 7) and can take the form of positive bubbles on the occlusal surfaces of the casts or outright distortions to the natural shape and contours of the teeth (Fig. 8). Regardless of what causes these interferences, they all produce the same result; they do not allow the teeth of the casts to occlude into maximum interdigitation. They, in fact, hold the models apart and create an open bite. If these interferences are not noticed and eliminated, the final restoration, regardless of material or design, will be high in occlusion when placed intraorally.
Fig. 7
Inaccurate Impression.

Fig. 8
Distorted 2nd Molar Tooth Shape.
Unfortunately, corrections of occlusion are left to the restorative dentists to waste valuable chair time with adjustments and re-polishing of restorations, or in worse case situations, the restoration will need to be returned to the laboratory for re-contouring and re-glazing. “We start our treatment with beautifully carved occlusal surfaces and how do we end? We grind until most of those beautifully carved cusps are cut away.” 8 These words, spoken by Dr. Frederick S. Meyer almost 80 years ago, are still sadly the usual routine in many dental oral rehabilitation cases today.
In our laboratory, we have found a solution to this re-occurring problem that has proven itself over time, with what we’ve named our Exclusive Bite Equilibration Technique. Most clinicians are familiar with the concepts of Intraoral Occlusal Equilibration,9-11 from the concepts derived from the teachings of Dr. Lindsey D. Pankey. 12
We have taken these concepts and related them to the stone and/or resin articulated casts. The technique consists of first eliminating all bubbles and noticeable irregularities from the occluding surfaces of the casts (Fig. 9). Secondly, with fine articulating paper (Bausch Arti-Foil, 8 micron, black, double-sided) we look for high spots in occlusion (Fig. 10). These could be naturally occurring high spots, distortions in the impression technique, or errors in the model fabrication technique. Thirdly, we then eliminate these high spots, with a #8 round bur (HP8 Jet Carbide) at low speed, until more stable contact markings appear (Fig. 11). These stable contact areas are similar to the Clayton Centric Stops (Fig. 12) developed by Dr. JA Clayton. 13
Fig. 9
Bite Equilibration Technique Step 1.

Fig. 10
Bite Equilibration Technique Step 2.

Fig. 11
Bite Equilibration Technique Step 3.

Fig. 12
Clayton Centric Stop – Lower 2nd Bicuspid.

It may take several attempts of marking and eliminating interferences, until the mounted models show more stable occlusal markings and more accurately represent the patient’s true occlusal contacts. Since implementing this technique over 17 years ago, we’ve surmised that we have been able to successfully eliminate approximately 95 per cent of all chair-side occlusal adjustments to our restorations.
Today’s dentists and dental technologists are constantly striving to enhance the patient experience. At the same time, as we are working to develop better materials, creating advanced designs, and engineering newer techniques, we can be applying clinical techniques in the laboratory setting to create restorations that reduce the need for adjustments and provide longevity. By ensuring that we do not inadvertently create pre-maturities in occlusion, we can be confident that we are helping to build a more sustainable system that can function with ease for the patient’s lifetime. OH
Oral Health welcomes this original article.
Disclaimer
The author wishes to express that he has no financial interest in any of the products or devises mentioned in the article.
Acknowledgement
The author wishes to gratefully acknowledge the help, support, and guidance of Dr. Stephen Abrams and Dr. Jordan Soll in the writing of this article.
References
- Racich, M. J., “Orofacial pain and occlusion: Is there a link? An overview of current concepts and the clinical implications”, J Prosthet Dent., 2005; 93: 189–196
- Davies, S. J., Gray, R. M. J., Whitehead, S. A., “Good occlusal practice in advanced restorative dentistry”, BDJ, 2001; 191: 421–434
- Brill, N., Schubeler, S., Tryde, G.,“Influence of occlusal patterns on movements of the mandible”, J. Prosthet. Dent, 1962; 12: 255–261
- Davies, S. J., Gray, R. M. J., “What is Occlusion?” BDJ, 2001; 191: 235 – 245
- Schoenrock, Gary A., “How to improve the accuracy of your double-arch impressions 10 secrets to success when processing a double-arch impression”, Parkell Inc., 2011
- Craddock, Helen L., “Consequences of Tooth Loss: 2. Dentist Considerations – Restorative Problems and Implications”, Restorative Dentistry, 2010.
- Becker, C. M., Kaiser, D. A., “Evolution of Occlusion and Occlusal Instruments”, J Prosthodontics, 1993; 2: 33 – 43
- Meyer, FS Cast bridgework in functional occlusion JADA 30: 1015-1030, 1933
- Fleming, Mark, “The Three Goals of Equilibration”, Spear Education, June 2012. http://www.speareducation.com/spear-review/2012/06/the-three-goals-of-equilibration.
- Greany, Thomas J., “What is Equilibration”,Tooth IQ, July 2015. https://www.toothiq.com/dental-procedure/equilibration.
- DeWood, Gary M. “Gnathology and Pankey-Mann-Schuyler: fulfilling the requirements of occlusion in oral rehabilitation”, in The University of Toledo Digital Repository, April 2004: 65-67.
- Mann, A.W., Pankey, L.D. Concepts of occlusion: the PM philosophy of occlusal rehabilitation. Dent Clin North Am. 1963;9:621–639.
- Clayton JA. Centrics: Factors to consider in their use. Aust Dent 1986; 16:41-49.
About the Author
 Ronald Klausz, R.D.T., is owner of Klausz Dental Laboratories, located in Toronto, Ontario. He has written numerous articles on restorative and implant dentistry and has lectured in both Canada and the United States. He keeps with the family traditions of producing advanced, high quality restorations and appliances while developing unique client and patient care services. He has modernized a company, which is celebrating 50 years of serving the dental community, whose focus is still based on fulfilling client needs. “Working harder and smarter for your practice!” is their mantra.
Ronald Klausz, R.D.T., is owner of Klausz Dental Laboratories, located in Toronto, Ontario. He has written numerous articles on restorative and implant dentistry and has lectured in both Canada and the United States. He keeps with the family traditions of producing advanced, high quality restorations and appliances while developing unique client and patient care services. He has modernized a company, which is celebrating 50 years of serving the dental community, whose focus is still based on fulfilling client needs. “Working harder and smarter for your practice!” is their mantra.












