Introduction & Background
Bisphosphonates are a class of medications that prevent the loss of bone mass. Not only are they used extensively in the treatment of metabolic bone disease such as osteoporosis, but they have been shown to decrease risk of fracture and bone pain in lung, breast, and other metastatic cancer. They are grouped mainly based on their route of administration, and fundamental differences exist between those administered orally and intravenously. Bisphosphonates indicated in the treatment of osteoporosis are taken orally, and as such, have a bioavailability near 1-2%. Bisphosphonates administered intravenously are typically indicated for the treatment of malignancy-associated hypercalcemia as well as for prevention of lytic lesions associated with multiple myeloma and various solid cancers. 1 When administered at physiologic doses, bisphosphonates are taken up primarily by the skeleton via adsorption to mineral surfaces. Because of this preferential affinity to bone, prolonged exposure to most other cell types is prevented. Bisphosphonate use is common among older adults and is likely to increase due to prolonged life expectancy. 2
The high prevalence of tooth loss in the older adult population has social as well as health consequences. The use of dental implants has become the standard of care in the replacement of missing teeth and the implementation of this treatment strategy is increasing greatly. Despite the benefits of bisphosphonate therapy, jaw osteonecrosis has emerged as a serious complication in a small subset of patients who have been treated with these medications and who have undergone invasive dental procedures such as tooth extractions and dental implant placement. 3 Although several theories have been proposed to explain the pathophysiology of jaw osteonecrosis associated with bisphosphonate use, a true cause and effect relationship has yet to be established. The leading theory suggests that interruption in bone remodeling by the fundamental osteoclast-inhibiting effect of bisphosphonates is the culprit. 4 However, the incidence of the complications as well as mitigating and aggravating factors are not well understood. The purpose of this paper is to explore the issues of prevention, diagnosis, and treatment of osteonecrosis of the jaw (ONJ) in the patient with a history of bisphosphonate use who has had implant therapy.
Effect of Bisphosphonates on Dental Implant Success
There is controversy within the dental and medical communities regarding development of osteonecrosis and implant failure in patients that are subjected to bisphosphonate therapy. 5 Giovannacci et al retrospectively looked at patients who have had dental implants placed and who were also on either oral or IV bisphosphonate therapy to determine if and when they developed osteonecrosis of the jaw. The authors of the study found that of the nine patients who developed ONJ from one to fifteen years after dental implant placement, 8 patients received intravenous bisphosphonate therapy for malignant disease for an average of 28 months. Of the six patients who developed ONJ two to ten months after dental implant placement, five patients were treated with oral bisphosphonates for osteoporosis and one was treated with intravenous bisphosphonates for malignant disease. The mean length of treatment in the second group was 84 months. They concluded that not only the surgical insertion of the implant, but the mere presence of the implant in bone is associated with ONJ. Although the risk of ONJ is lower among those patients taking bisphosphonates orally rather than intravenously, the risk exists and should not be underestimated. 6
Fig. 1
Patient presents for consult. Panoramic radiograph of ONJ patient with restored implants.

Fig. 2
Initial frontal clinical view in occlusion with shifted midline, maloccluding posterior teeth.

Fig. 2a
Preoperative clinical presentation. Implants on lower right side and temporary on lower left side were not in occlusion.

Fig. 2b

Fig. 2c

Fig. 2d

Fig. 3
Maxillary occlusal view with recession on palatal of first molars, rotation, diastema and extrusion.

In another study, Tallarico et al examined three-year data on success rates of fixed implant-supported dental prostheses in individuals who were previously on oral bisphosphonate therapy. They found that after three years, the implant survival rate was 99%. The group proposed that implant therapy is a viable option for single tooth replacement among those patients taking oral bisphosphonates. The results of this particular study should be interpreted with caution because the follow-up period is merely three years, whereas the latent period for osteonecrosis of the jaw may be much longer. 7 Grant et al looked whether dental implant treatment can be successful in a cohort of patients who have been on bisphosphonate therapy, and whether osteonecrosis of the jaw occurred following dental implant therapy. The investigators determined that oral bisphosphonate therapy did not play a significant role in the development of ONJ, and that ONJ is a relatively rare complication following dental implant surgery in patients who are on oral bisphosphonates. 8 Future studies must be conducted to look at implant success or failure in individuals who are on bisphosphonate therapy versus those who are not.
Fig. 4
Mandibular occlusal view with composite splint LL, three implants LR restored with two composite crowns.

Fig. 5
Mandibular front lingual view with lingual anterior composite splint and supraginigval calculus bridge.
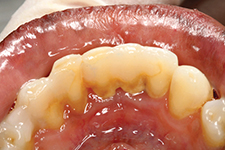
Fig. 6
Periapical radiograph (PA) of restored implants lower right side. Implant #44 has ONJ.

Fig. 7
Opposing dentition PA – #16 has severe radiographic bone loss with vertical osseous defect on mesial. Tooth #16 is extruded and is displaying mobility and pathologic migration with diastema presentation and distalization due to attachment loss. Subgingival etiology present.

Fig. 8
Buccal view at implant removal. Composite restorations were removed and tissue degranulated. Osseous defect displayed.

Fig. 9
Occlusal surgical view of ONJ site. Mobile implants were removed.

Fig. 10
Intrasurgical clinical view of implant removal.

How to Diagnose Clinical Osteonecrosis of the Jaw (ONJ)
A patient with osteonecrosis may remain asymptomatic for months. It is usually recognized by its unique presentation of exposed bone in the maxillofacial region. The lesions usually become symptomatic when exposed areas are secondarily infected. In addition to exposed bone, individuals may present with localized pain and swelling, loosening of teeth, or purulent drainage. Although symptoms may occur spontaneously, they often arise at the site of previous tissue manipulation such as during surgery or tooth extraction. If osteonecrosis of the jaw is suspected, panoramic radiography may help rule out cysts or metastatic disease. Plain film radiographic changes can be seen in patients with osteonecrosis, although earlier stages of disease may be difficult to visualize. 9 More recently, Kolokythas et al looked at whether biomarkers of bone resorption can be found in saliva and whether or not there is a difference between the levels of these biomarkers in patients with and without osteonecrosis of the jaw. The authors reported that there was a statistically significant difference in levels of salivary N-telopeptide of type I collagen between the osteonecrosis group and the control. Further investigation is warranted into saliva as a diagnostic fluid medium for the detection of biomarkers that might aid in the diagnosis of osteonecrosis of the jaw. 10
How to Prevent Clinical Osteonecrosis of the Jaw (ONJ)
To decrease the incidence of osteonecrosis of the jaw, it is well recognized in clinical practice that a thorough intraoral and maxillofacial exam must be performed on all patients prior to initiating bisphosphonate therapy. 11 Individuals taking bisphosphonates should be under the close care of a dentist who is familiar with osteoporosis and oncologic therapy. The main goal is to eliminate oral infection, pathology, and risk factors for osteonecrosis. In order to achieve the optimal oral health environment, invasive dental procedures should be performed before starting bisphosphonates. Several authors have suggested a drug holiday before surgical procedures, but there isn’t enough evidence to support the interruption of medical treatment of patients with osteoporosis. 12 Patients should always be made aware of the risk of developing osteonecrosis of the jaw, especially if treatment with bisphosphonates exceeds four years. 13 The importance of daily home oral health care should be underscored, as well as periodic clinical follow-up that includes radiographic examinations. As outlined in the previous section, dental implant therapy is a viable option in patients who are taking bisphosphonates, but a cautious approach is recommended.
Fig. 11
Implant after removal with attached necrotic peri-implant tissue and bone.

Fig. 12

Fig. 13
Contralateral side after removal of composite splint. The soft tissue on the adjacent abutment teeth is receded, edematous and inflamed. The roots are exposed.

Fig. 14
One-week post-op after removal of implant #44. Poor ONJ healing.

Fig. 15

Fig. 16
Buccal clinical view after additional implant removal region 46 three months later.

Protocol (Dr. J.B.Suzuki):
Bisphosphonate ONJ Prevention Patient Management
Who is at Risk? Patients Receiving Bisphosphonate Therapy
1. Patients having a history of receiving IV Bisphosphonates (Aredia, Zometa and others) represent an absolute contraindication for jaw bone related surgery of any kind.
2. Patients with a history of Oral Bisphosphonate (Fosamax, Actonel, Boniva and others) use for more than three years are considered at greater risk for BRONJ (Bisphosphonate Related Osteonecrosis of the jaws).
3. This is especially true for patients with co-morbidities such as smokers and patients on steroid therapy.
4. Patients who have taken Oral Bisphosphonates for less than three years have a relatively low risk for BRONJ.
Fig.17
PA post implant removal displaying diffuse radiolucency.

Fig. 18
Occlusal clinical view of LR ridge with granulomatous tissue.

Fig. 19
One-month post-op after removal of second implant.

Fig. 20

Bisphosphonate Patient Treatment Protocol
1. Patient should have a consultation with MD provider to be given basic information regarding Bisphosphonate risk.
2. Patients should be scheduled for a prophylaxis/periodontal maintenance (PMT) with the hygienist at least one week prior to scheduled surgery.
3. Patients should be placed on an oral rinse containing Chlorhexidine (such as Peridex), one week prior to scheduled surgery.
4. Assuming no Penicillin allergy, the patient should start on Augmentin 500 mg (four times per day) starting 48 hours prior to scheduled surgery.
How to Treat Clinical Osteonecrosis of the Jaw (ONJ)
There is an abundance of literature on the management of osteonecrosis of the jaw related to bisphosphonate use, and includes everything from surgical debridement to oxygen therapy. 14 Garcia et al describe an interesting treatment modality for refractory cases that involves autologous bone marrow stem cells, beta tricalcium phosphate, platelet-rich plasma (PRP), and demineralized bone matrix (DBM). 15 However, the standard of care in the treatment of osteonecrosis of the jaw remains dependent on the clinical staging system that was developed in 2006 and subsequently updated, with the latest update in 2014. 16 Lozano et al looked at various treatments that have been recommended for osteonecrosis of the jaw and examined the effects of each treatment based on their success rates. Conservative management was one treatment option examined by the group, and included oral hygiene instructions, clinical follow-up, chlorhexidine rinses, antibiotics, ozone therapy, hyperbaric oxygen therapy, and low-power laser therapy. For those patients who were refractory to conservative therapy, sequestrectomy or extensive segmental surgeries were viable options. The authors found that conservative management was reserved for those patients who are at risk for ONJ or who are asymptomatic (stage 1), and surgical management was reserved for stage II or III ONJ patients, or those who were refractory to non-surgical therapeutic modalities. They concluded that whereas currently, surgical management is the preferred option for the treatment of stage II and III ONJ, minimally invasive procedures that afford patient health and comfort are the future treatments of choice. 17
Case Report
A 48-year-old female patient with history of double mastectomy, radical wide neck irradiation, allograft reconstruction of the left arm, radiation to the head and neck, chemotherapy and prolonged use of oral (Fosamax) and high dose IV (Zometa) bisphosphonates on remission for stage IV breast carcinoma.
Patient had implant placement and iatrogenic restorative work performed in Dominican Republic in 2008–2009 without premedication or post-operative antibiotic therapy.
First seen for consultation and removal of defective restorations in 2010.
Necrosis of the right posterior mandible likely due to IV bisphosphonate use and poor tissue management with no possibility of oral hygiene of the implants due to poor placement and defective composite restoration over the implants.
Treatment consisted of removal of the defective restorations, initial periodontal therapy, removal of the loose implants with bone sequestrum and subsequent debridement of the necrotic area alongside hyperbaric oxygen therapy.
The patient was referred to the oral maxillofacial surgery department for further treatment of necrosis (ONJ) of the right mandible. OH
Oral Health welcomes this original article.
Acknowledgements
Enrique Muller, DMD, MSD
References
1. Saldanha, Sharon, Vidya K. Shenoy, Prashanti Eachampati, and Nakul Uppal. “Dental Implications of Bisphophonate-related Osteonecrosis.” Gerodontology 29.3 (2012): 177-87.
2. Rogers, Michael J., Julie C. Crockett, Fraser P. Coxon, and Jukka Mönkkönen. “Biochemical and Molecular Mechanisms of Action of Bisphosphonates.” Bone 49.1 (2011): 34-41
3. Marx, Robert E., Yoh Sawatari, Michel Fortin, and Vishtasb Broumand. “Bisphosphonate-Induced Exposed Bone (Osteonecrosis/Osteopetrosis) of the Jaws: Risk Factors, Recognition, Prevention, and Treatment.” Journal of Oral and Maxillofacial Surgery 63.11 (2005): 1567-575
4. Budtz-Jørgensen, Ejvlnd, Jean-Pierre Chung, and Philippe Mojon. “Successful Aging?the Case for Prosthetic Therapy.” Journal of Public Health Dentistry J Public Health Dent 60.4 (2000): 308-12
5. Albandar, Jasim M. “Oral Bisphosphonate Therapy May Not Significantly Compromise Dental Implants Success.” Journal of Evidence Based Dental Practice 8.4 (2008): 229-31
6. Giovannacci, Ilaria, Marco Meleti, Maddalena Manfredi, Carmen Mortellaro, Alberta Greco Lucchina, Mauro Bonanini, and Paolo Vescovi. “Medication-Related Osteonecrosis of the Jaw Around Dental Implants.” Journal of Craniofacial Surgery (2016): 1
7. Tallarico, Marco, Luigi Canullo, Erta Xhanari, and Silvio Mario Meloni. “Dental Implants Treatment Outcomes in Patient under Active Therapy with Alendronate: 3-year Follow-up Results of a Multicenter Prospective Observational Study.” Clinical Oral Implants Research Clin. Oral Impl. Res. 27.8 (2015): 943-49
8. Grant, Bao-Thy, Christopher Amenedo, Katherine Freeman, and Richard A. Kraut. “Outcomes of Placing Dental Implants in Patients Taking Oral Bisphosphonates: A Review of 115 Cases.” Journal of Oral and Maxillofacial Surgery 66.2 (2008): 223-30
9. Ruggiero, S., J. Gralow, R. E. Marx, A. O. Hoff, M. M. Schubert, J. M. Huryn, B. Toth, K. Damato, and V. Valero. “Practical Guidelines for the Prevention, Diagnosis, and Treatment of Osteonecrosis of the Jaw in Patients With Cancer.” Journal of Oncology Practice 2.1 (2006): 7-14
10. Kolokythas, Antonia, Maria Karras, Edward Collins, William Flick, Michael Miloro, and Guy Adami. “Salivary Biomarkers Associated With Bone Deterioration in Patients With Medication-Related Osteonecrosis of the Jaws.” Journal of Oral and Maxillofacial Surgery 73.9 (2015): 1741-747
11. Ripamonti, Carla I., Maurizio Lucchesi, and Raffaele Giusti. “Prevention and Management of Osteonecrosis of the Jaw Secondary to Bone-targeted Therapy in Patients with Kidney Cancer.” Current Opinion in Supportive and Palliative Care 10.3 (2016): 273-80
12. Papi, Piero, Daniele Rosella, Rita Giardino, Emauele Cicalini, Luca Piccoli, and Giorgio Pompa. “Medication-related Osteonecrosis of the Jaw: Clinical and Practical Guidelines.” J Int Soc Prevent Communit Dent Journal of International Society of Preventive and Community Dentistry 6.2 (2016): 97
13. O’ryan, Felice S., and Joan C. Lo. “Bisphosphonate-Related Osteonecrosis of the Jaw in Patients With Oral Bisphosphonate Exposure: Clinical Course and Outcomes.” Journal of Oral and Maxillofacial Surgery 70.8 (2012): 1844-853
14. Rupel, Katia, Giulia Ottaviani, Margherita Gobbo, Luca Contardo, Giancarlo Tirelli, Paolo Vescovi, Roberto Di Lenarda, and Matteo Biasotto. “A Systematic Review of Therapeutical Approaches in Bisphosphonates-related Osteonecrosis of the Jaw (BRONJ).” Oral Oncology 50.11 (2014): 1049-057
15. Gonzálvez-García, Mar, Francisco Javier Rodríguez-Lozano, Victor Villanueva, Daniel Segarra-Fenoll, Maria Angeles Rodríguez-González, Ricardo Oñate-Sánchez, Miguel Blanquer, and José María Moraleda. “Cell Therapy in Bisphosphonate-Related Osteonecrosis of the Jaw.” Journal of Craniofacial Surgery 24.3 (2013)
16. Ruggiero, Salvatore L., Thomas B. Dodson, John Fantasia, Reginald Goodday, Tara Aghaloo, Bhoomi Mehrotra, and Felice O’ryan. “American Association of Oral and Maxillofacial Surgeons Position Paper on Medication-Related Osteonecrosis of the Jaw—2014 Update.” Journal of Oral and Maxillofacial Surgery 72.10 (2014): 1938-956
17. Rodriguez-Lozano, Fj, and Re Oñate-Sanchez. “Treatment of Osteonecrosis of the Jaw Related to Bisphosphonates and Other Antiresorptive Agents.” Med Oral Medicina Oral Patología Oral Y Cirugia Bucal (2016): 0
RELATED ARTICLE: Safer Implant Treatment
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












