Background
Amelogenesis imperfecta (AI) is a rare genetically determined defect in enamel mineralization with a prevalence between 1:14,000 and 1:70.1,2 AI is caused by mutations in the genes AMELX, ENAM, or MMP20. These genes are responsible for making the proteins needed for normal formation of enamel. A mutation in any one of these genes can prevent it from making the correct protein, leading to defective enamel that is thin or soft. The mutated genes can be passed on from parents to their children, or the mutation can develop in people with no family history.1,2
Several types of AI exist based on clinical, radiographic, genetic, and histological findings. The most widely accepted classification of AI includes four main types:1-4
Type I: Hypoplastic
In this form, there is a defect in the amount of enamel created. The teeth are small and may be white, yellow, or brown, and the enamel is quite thin. The teeth also have pits and grooves. This type represents the majority of all cases of AI.3
Type II: Hypomaturation
In this type, there is a defect in the final growth and maturation of enamel. The teeth are a creamy opaque to yellow or brown with sensitivity. The enamel has a normal thickness, but it’s too soft, so the teeth appear mottled and may wear away and break. Hypomaturation represents between 20-40% of all cases of AI.3
Type III: Hypocalcification
In this type, a defect occurs in the initial stages of enamel formation. The enamel may have a normal thickness, but it’s too soft. Teeth may be white, yellow, or brown, and the enamel may be rough. The teeth may also be extremely sensitive to hot and cold. This is the least common type of AI.3,4
Type IV: Hypomaturation-hypoplasia with taurodontism
Here, the enamel has a variation in appearance, with mixed features from Type I and Type III AI. All Type IV AI has taurodontism in common. This condition is of autosomal dominant pattern. Other common features may include an anterior open bite and sensitivity of teeth.2,4
Impaired esthetics, tooth hypersensitivity, wide pulp chamber, higher risk of dental caries, and decreased occlusal vertical dimension are among the challenges faced in the management of AI. Dental anomalies associated with AI include enamel disorders, anterior open bite, pulpal calcifications, delayed eruption of teeth, pathological root and crown resorption, and taurodontism.4,5
Management of AI requires a comprehensive treatment plan and a multidisciplinary approach involving most of the time a pediatric dentist, an orthodontist, a maxillofacial surgeon, and a prosthodontist. The four main treatment options available to correct anterior open bite when present include surgery, prosthetic crowns, composite or ceramic veneers (for cases with mild open bite), and veneering or crown placement combined with surgery; the latter option is often considered as an ideal treatment for anterior open bite.3-5
A multidisciplinary approach is described for two patients with AI.
Case 1
An 18-year-old healthy patient diagnosed with Type I AI returned to our office after completing orthodontic treatment in 2016. There was no family history of AI. She had been in orthodontic treatment since she was 13 years of age (Figs. 1A & 1B). She wanted to improve her smile before going to University.
Fig. 1A

Fig. 1B

Intraoral examination showed a well-preserved dentition. Her teeth had proper width to length proportions and she had a proper tooth display when smiling (Figs. 2A & 2B). Her teeth had rough and pitted surfaces on the occlusal surfaces of all her mandibular and maxillary teeth (Figs. 3A & 3B). No sensitivity was experienced. Oral hygiene was excellent. No caries lesions or periodontal disease was found clinically. She had been treated with composite restorations for anterior maxillary teeth while she had orthodontic treatment.6 Radiographic examination showed acceptable crown to root ratio and no periapical pathologies were seen. No other radiographic abnormalities were noted. We had discussed different treatment options such as: new composite restorations, laminate veneers and full coverage restorations.6-10 After discussing all advantages and disadvantages, she decided to proceed with first whitening of her teeth, followed by bonded laminate veneers for teeth #15 to #25.9 Since she never had any carious lesions, it was decided to not treat any of her maxillary molars or mandibular teeth at this point. She decided that she would address these teeth if they presented with problems in the future.
Fig. 2A

Fig. 2B

Fig. 3A
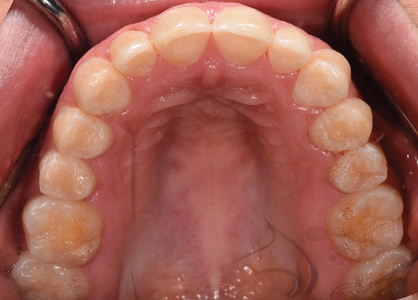
Fig. 3B

Enough reduction was performed in all 10 teeth to receive e-max empress veneers. Final impressions were obtained using an intraoral scanner. Temporaries veneers were fabricated using a template which was fabricated from a wax up. Imported data from the scanner was interpreted and used in conjunction with laboratory design software to create a digital representation of the final product.
A digital scan of the patient’s provisionals veneers was imported and superimposed over a scan of the patients prepared teeth. Digitally designed 3D-printed models of both the maxillary and mandibular arches were milled. It was established that the material choice for all veneers was to be lithium disilicate.
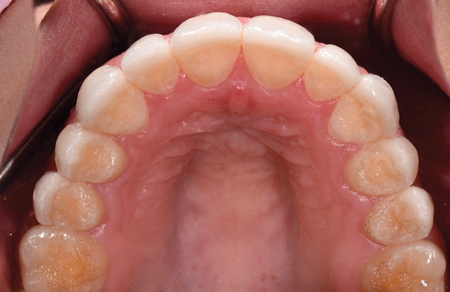
The laminate veneers were luted using resin cement (Figs. 4A & 4B).11 There was excellent marginal adaptation for all restorations. Occlusal contacts were maintained on natural tooth structure (Fig. 5).
Fig. 4A

Fig. 4B

Fig. 5
Case 2
A 17-year-old healthy patient who had been diagnosed with Type III AI was referred to the office by his orthodontist. He had a family history for AI. Both his sister and mother had been diagnosed with AI. He started orthodontic treatment when he was 14 years old (Fig. 6) and completed treatment four years later. Intraoral exam showed dark yellow teeth with brittle enamel that was easy to remove with a scaler. All his teeth had short clinical crowns. Proper gingival levels were noted. There was no tooth display when the patient’s lips were at rest. There was some sensitivity to cold in most of his teeth. Oral hygiene was poor and there were a few carious lesions and gingival inflammation at the end of his orthodontic treatment (Figs. 7A and 7B). Prosthodontic treatement was started when he was 19 years old.
Fig. 6
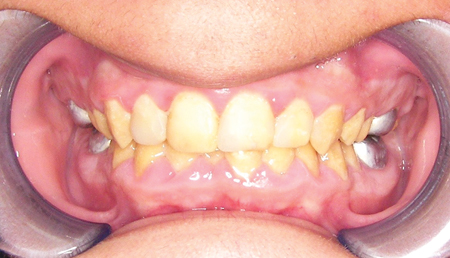
Fig. 7A

Fig. 7B

Radiographic examination revealed good bone levels around all teeth. No signs of periapical infection was noted. Scaling and root planning were carried out by a periodontist and he was put on a three-month recall visits due to his gingival inflammation. When ideal periodontal status was achieved, we proceeded with restorations. As opposed to the first patient, this patient had less options to restore aesthetics and function. After discussing treatment and long-term maintenance, it was decided that all teeth would be prepared for full coverage restorations and that the material of choice was to be monolithic full contour zirconia. All teeth were properly prepared for such restorations and provisional crowns were fabricated based on our diagnostic wax up. Since there was not a favourable width to length ratio for his clinical crowns, his teeth were lengthened incisally and vertical dimension of occlusion was increased by 2 mm. The patient used his temporary crowns for a period of two months. When he was satisfied with aesthetics, phonetics, function, and teeth had not shown any sensitivity, we proceeded to fabricate final crowns.
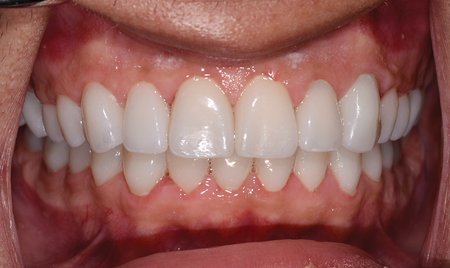
All crowns were designed using a dental modelling software and then prepared for milling. An important variable was the selection of a zirconia material that would exhibit the ability to mask the underlying discolouration of the tooth preparation, yet offer the same translucency to maintain a natural appearance.12,13 Protocol for multiple crown cementation was done carried out and crowns were luted using resin cement.12,13 An occlusal therapy appliance was fabricated for him at the end of treatment. He was very pleased with the outcome of his treatment (Figs. 8A & 8B).
Fig. 8A

Fig. 8B
Discussion
Early recognition followed by preventive and restorative care is paramount in the successful management of AI. A multidisciplinary approach with careful planning from early childhood will
maximize the treatment options available for the permanent dentition and optimize the final outcome. In these two cases, a team consisting of paediatric dentists, orthodontists, and prosthodontist were involved in the management of the patients.14
Treatment included preventive advice, periodontal monitoring, interim composite restorations and stainless-steel crowns, orthodontic treatment and placement of final restorations. The patients were extremely satisfied with the results. They stated that their confidence was greatly improved after final restorations were completed. They were educated to the importance of regular dental appointments and the use of an occlusal appliance to wear at night. Both patients were about to start post-secondary education, so the completion of treatment meant a significant improvement in their quality of lives.14,15
Oral Health welcomes this original article.
Acknowledgement: Many thanks to Mr. Chris Kalopsis DT of Dental Design Centre for his insightful technical support in these and many other cases. His dental laboratory is located in London, Ontario. dentaldesigncentre@yahoo.ca
References
- Witkop CJ Jr, Kuhlman W, Sauk J. Autosomal recessive pigmented hypomaturation amelogenesis imperfecta. Oral Surg Oral Med Oral Path Oral Radiol. 1973;36(3):367-382.
- Sundell S, Koch G. Hereditary amelogenesis imperfecta. I. Epidemiology and clinical classification in a Swedish child population. Swed Dent J. 1985;9:157-169.
- Bäckman B, Holm A-K. Amelogenesis imperfecta: prevalence and incidence in a northern Swedish county. Community Dent Oral Epidemiol. 1986;14:43-47.
- Rowley R, Hill FJ, Winter GB. An investigation of the association between anterior open bite and amelogenesis imperfecta. Am J Orthod. 1982;81(3):229-235.
- Ramos AL, Pascotto RC, Filho LI, Hayacibara RM, Boselli G. Interdisciplinary treatment for a patient with open-bite malocclusion and amelogenesis imperfecta. Am J Orthod Dentofacial Orthop. 2011;139:145-153.
- Ayers KM, Drummond BK, Harding WJ, et al. Amelogenesis imperfecta – multidisciplinary management from eruption to adulthood. Review and case report. N Z Dent J. 2004;100:101-104.
- Seow WK, Amaratunge FA. The effect of acid etching on enamel from different clinical variants of Amelogenesis imperfecta an SEM study. Pediatr Dent. 1998;20(1):37-42.
- Ranganath V, Nichani SA, Soumva V. Amelogenesis Imperfecta: a challenge to restoring esthetic and function. J Indian Soc Peridontol. 2010;14:195-197.
- Nathwani NS, Kelleher M. Minimally destructive management of amelogenesis imperfecta and hypodontia with bleaching and bonding. Dent Update. 2010;37(3): 170-172, 175-6, 179.
- Bouvier D, Duprez JP, Pire LC et al. Amelogenesis imperfecta – a prosthetic rehabilitation: a clinical report. J ProsthetDent. 1999;82:130-131.
- Krunić N, Tonić G. Impact of various luting cements on the fixed dentures bonding strength. Vojnosanit Pregl. 2006;63(3):293-296.
- Chamarthi V, Varma BR, Jayanthi M. Amelogenesis imperfecta: A clinician’s challenge. J Indian Soc Pedod Prev Dent. 2012;30:70-73.
- Wright JT. The diagnosis and treatment of dentinogenesis imperfecta and Amelogenesis imperfecta. Hellenic Dent J. 1992;2:17-24.
- Poulsen S, Gjorup H, Haubek D, et al. Amelogenesis imperfecta – a systemic literature review of associated dental and oro-facial abnormalities and their impact on patients. Acta Odontol Scand. 2008;66(4):193-199.
- Akin H, Tasveren S, Yeler DY. Interdisciplinary approach to treating a patient with Amelogenesis imperfecta: a clinical report. J Esthet Restor Dent. 2007;19(3):131-136.
About the Author
 Dr. Aragon is a Prosthodontist who maintains a full-time private practice in London, Canada. She is an Adjunct Clinical Professor at the Schulich School of Dentistry. She holds clinical privileges at the London Health Science Centre and is also a Staff member at the Thames Valley Children’s Centre. E-mail: doctor@aragonprosthodontics.com/www.aragonprosthodontics.com.
Dr. Aragon is a Prosthodontist who maintains a full-time private practice in London, Canada. She is an Adjunct Clinical Professor at the Schulich School of Dentistry. She holds clinical privileges at the London Health Science Centre and is also a Staff member at the Thames Valley Children’s Centre. E-mail: doctor@aragonprosthodontics.com/www.aragonprosthodontics.com.












