Tremendous strides have been made in both the construction and the placement of modern dental implants compared to earlier iterations. Yet, the prevalence of peri-implant disease continues at an alarming rate. In a meta-analysis of 110 clinical studies examining the extent of peri-implant disease affecting more than 12,000 active dental implants, it was shown that almost half of all those implants had peri-implant disease involvement1,2,3,4 (see Table 1).
Table 1
| Prevalence of Peri-Implant Disease | |
| % of implants | |
| Peri-implant mucositis | Average: 35.6% |
| Peri-implantitis | Average: 13.1% |
| Peri-implantitis & Peri-implant mucositis | Total: 48.7% |
So, what else can be done to avoid these degenerative implant conditions from becoming implant failures in your patients? Guidance can be drawn from a recent workshop of the European Federation of Periodontology where they point out that “As with periodontitis, peri-implant mucositis and peri-implantitis develop as a result of the accumulation of bacterial plaque. So, the treatment for peri-implant disease adopts the same principles of therapy as those used in treating gingivitis and periodontitis.”5
While the causes of implant failure can be multi-factorial, the fact remains that the accumulation of bacterial plaque is far and away the most important cause of peri-implant disease.6
Knowing that bacterial plaque is at the heart of both periodontal disease and also peri-implant disease is still a long way from controlling it. For decades, both dental patients and dental professionals have been fighting dental plaque accumulation and yet periodontal disease has now reached epidemic levels.7 Could it be that our efforts have been ineffective or only poorly effective?
Most dental professionals teach their patients that it is imperative to brush and floss daily as key elements in an effective daily home oral hygiene regimen. But how really effective is brushing and flossing in reducing the accumulation of dental plaque? Are there other patient-friendly ways to achieve much greater plaque reduction than with brushing and flossing? These are important questions to be answered because patients can do more at home to achieve optimal oral health than we can do for them in our offices. Periodontal and peri-implant destruction occurs daily, so a truly effective daily home oral hygiene regimen that actually prevents pathogenic bacterial infection is the best defense against both periodontal disease and also peri-implant disease.8
Table 2 shows the effectiveness of brushing and flossing each day at home in reducing dental plaque compared to brushing and rinsing at home. Both of these studies were controlled, randomized, evaluator-blinded, six-month studies. Each had over 300 patients enrolled. The results may challenge your long-held beliefs. The first study showed that brushing and rinsing was 18 times more effective than brushing and flossing and the second study showed that brushing and rinsing was 6 times more effective than brushing and flossing in reducing dental plaque.9
Table 2
| Effectiveness of Flossing vs Rinsing | ||
| % plaque reduction | ||
| Study #1 | Study #2 | |
| Rinsing & Brushing | 37.5% 18x better plaque reduction | 20.0% 6x better plaque reduction |
| Flossing & Brushing | 2.1% | 3.4% |
An additional six-month study with 160 patients also showed that brushing and rinsing was far more effective in reducing plaque and inflammation (as measured by the Plaque Index, the Modified Gingival Index and the Bleeding Index) than was brushing and flossing.10 We don’t need to “toss the floss.” Flossing still provides important adjunctive benefits, but a daily home care oral hygiene regimen that does not include rinsing or irrigating, is one that is sorely lacking.11
If at-home rinsing strongly merits inclusion in a daily oral hygiene regimen, then at-home subgingival irrigation, perhaps, deserves an even more important role. WaterPik Corporation has conducted studies showing that with rinsing alone, the rinsing agent can reach to 21% of the depth of a 6mm pocket. By using an oral irrigator with a subgingival tip, the irrigant can reach to 90% of the depth of that same 6 mm pocket.12
We are now on the road to optimal oral health. We have identified accumulating bacterial plaque as the principal causative agent in both peri-implant disease and also in periodontal disease. We have also identified rinsing and subgingival irrigation as being critically important if our patients’ oral hygiene regimens are to be truly effective.9
Since rinsing and subgingival irrigation are so critically important in achieving effective oral hygiene, does it make any difference which rinse or irrigant our patients use? Inhibiting bacterial plaque buildup is best accomplished with brushing and rinsing with an effective antiseptic rinse or brushing and irrigating with an effective antiseptic irrigant. Recent testing of professional antiseptic rinses was done to determine the efficacy of each antiseptic rinse against key periodontal bacteria and the results may surprise you.
Table 3 shows the comparative efficacy of each of the tested antiseptic rinses against both Fusobacterium nucleatum and Prevotella intermedia at 30 seconds exposure time. These bacteria were chosen because of their extreme pathogenicity and because they play such an important role in the development of periodontal disease. To ensure that testing was done under realistic conditions, fresh, human, whole saliva was used as an organic challenge in testing each rinse because salivary proteins inactivate many antiseptic rinses.13 The tested rinses are arranged in descending order of efficacy. Two key points that can be gleaned from this table are that 1) There is a tremendous difference in efficacy amongst the tested antiseptic rinses, ranging from complete inactivation of both pathogenic bacteria by the molecular iodine rinse to no biocidal activity, at all by a stabilized chlorine dioxide rinse against Prevotella intermedia and 2) The molecular iodine rinse was the only rinse to completely inactivate the bacteria.14
Table 3
| Log reduction at 30 seconds | ||
| Antiseptic Rinse | Fusobacterium nucleatum | Prevotella intermedia |
| Molecular iodine 100 ppm | 6.0 complete inactivation | 6.0 complete inactivation |
| Chlorhexidine gluconate 0.12% | 4.8 28x less effective | 3.3 730x less effective |
| Cetylpyridinium chloride 0.07% | 0.2 820,000x less effective | 5.3 7x less effective |
| Chlorine dioxide | 0.71 361,000x less effective | 3.9 190x less effective |
| Povidone iodine 10% | 1.8 28,000x less effective | 1.3 73,000x less effective |
| Hydrogen peroxide | 0.4 640,000x less effective | 0.52 532,000x less effective |
| Stabilized chlorine dioxide | 0.04 964,000x less effective | 0 no biocidal activity |
The rinse found to be the most effective (100 ppm molecular iodine) was tested again to further validate its efficacy. The additional testing was also conducted with a human saliva challenge, but the testing was expanded to two other pathogenic periodontal bacteria, Porphyromonas gingivalis and Tannerella forsythia. The complete inactivation of these additional pathogens within 30 seconds further validated the unique efficacy of the molecular iodine rinse.15
Some Information in Table 3 may be confusing because it shows two different iodine rinses with vastly different levels of efficacy. The molecular iodine rinse was shown to be tens of thousands of times more effective than the povidone iodine rinse. Why is that? Because 10% Povidone iodine contains several different species of iodine each in abundant supply, but only one species of iodine is actually biocidal and it is present in only trace quantities (2-3 ppm) in povidone iodine. That biocidal species of iodine is molecular iodine (I2) and it accounts for all of the antiseptic activity of povidone iodine. Molecular iodine oral care products were developed and patented by ioTech International in 2017 and are available in Canada exclusively through Henry Schein Canada. They are stable solutions containing high levels of molecular iodine at levels 30-100 times greater than is present in povidone iodine and are available as a ready-to-use rinse or as a concentrated irrigant for use in a Water Flosser.16 Because iodine is an essential nutrient, required by humans in order to avoid iodine-deficiency diseases17 and because high level molecular iodine solutions contain almost none of the other abundant iodine species, they are non-staining and have wide margins of safety.
The test results shown in Table 3, comparing the biocidal efficacy of seven antiseptic rinses against two key periodontal pathogens, are arranged in descending order of efficacy. They make a compelling case for the use of molecular iodine for periodontal care since it is far more efficacious against perio pathogens than any of the other antiseptic rinses tested.
Cariogenic bacteria, along with periodontopathic bacteria are responsible for almost all dental disease. Indeed, 95% of adults have or will experience periodontal disease or dental carries in their lifetimes.18
Wouldn’t it be wonderful if just one antiseptic agent could be used both safely and effectively to combat periodontal disease and dental caries? Let’s now look at Table 4. It compares the biocidal efficacy of each of the antiseptic rinses shown in Table 3, but this time they are being tested for their effectiveness against Strep mutans, a principal cariogenic bacterium.
Table 4
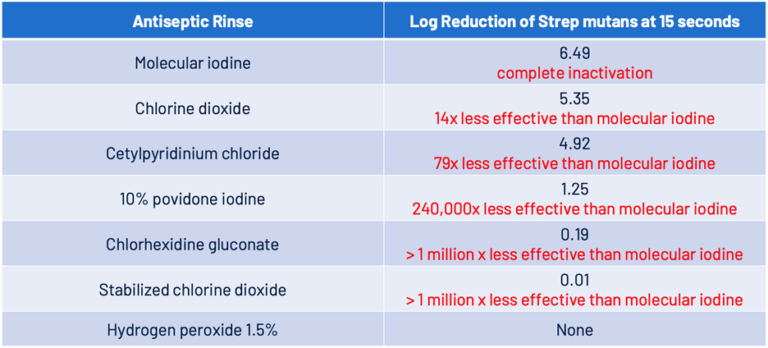
BioScience Laboratories, Bozeman, Montana
Again, molecular iodine proves far more effective than all the other tested rinses. It was the only rinse shown to be fully effective against Strep mutans at 15 seconds exposure time and was 14 times more effective than the next most effective rinse.
The superior biocidal efficacy demonstrated by molecular iodine against Strep mutans is especially significant because Strep mutans is a principal cariogenic bacterium. It is even more significant because studies have shown that carious dental lesions cannot form in the absence of cariogenic bacteria, even with a diet containing more than 50% sugar.19,20
Molecular iodine not only has an excellent safety profile, but it is also actually an essential nutrient, required by humans to synthesize thyroid hormones and to avoid iodine deficiency diseases.21 Several studies have shown that iodine is significantly effective in preventing dental caries.22,23
The evidence is clear. If you want to help your patients avoid the ravages of periodontal disease and achieve better treatment outcomes and higher levels of patient satisfaction, you’ll follow these 3 easy steps:
- Educate your patients to the importance of their role and of their responsibility in being meticulous in their daily home care.
- Ensure that your patients include rinsing and/or subgingival irrigation as part of an effective home care regimen.
- Ensure that the rinse or irrigant that your patients are using has evidence-based effectiveness.
Helping your patients to an effective daily oral hygiene regimen will also be helping your patients to better overall health. Let’s not lose sight of the fact that periodontal bacteremias are closely linked to Alzheimer’s disease, cardiovascular disease, certain cancers, and a myriad of other debilitating diseases.
Disclaimer: The author Dr. Herb Moskowitz is the Chairman and Co-Founder of ioTech International, a developer and manufacturer of molecular iodine oral care products.
References
- Analysis of 9 studies with 1,497 participants and 6,283 implants. Journal of Periodontology. Volume 84 #1: Nov 2013
- Definition and Prevalence of Peri-implant Diseases. Zitman et al. J Clin Periodontal 2008; 35: 288-291
- Analysis of 47 studies with at least 30 patients in each study. Journal of Dentistry 2017; July: 62 1-12
- Analysis of 57 studies between 2005 and 2021. What is the prevalence of peri-implantitis? Diaz et al. BMC Oral Health (2022) 22: 449
- Proceedings of the 1st Workshop on Periodontology. Quintessence 1999: 365-369
- Why Are Implants Failing? Christensen, Gordon J. DentalTown.com. Oct 2019; 68-72
- Global Prevalence of Periodontal Disease and Lack of Its Surveillance. Nazir, M. et al. Scientific World Journal. May 2020: 146-160
- Home Oral Care. American Dental Association website. Dec 2022
- Flossing vs Rinsing. Which is More Effective? Dentistry IQ March 6, 2002
- Journal of International Society of Preventative and Community Dentistry. Jan –June 2011
- How Can I Improve My Oral Hygiene. Cleveland Clinic website April 21, 2022
- Depth of penetration in periodontal pockets with oral irrigation. Eakle, W. et al. J Clin Periodontal. 1986 Jan; 13(1): 39-44
- Clinicians Report. Christensen, Gordon J. April 2021, Volume 14 Issue 3, pages 1-3
- Prime Analytical Laboratories, Concord CA. Fall, 2022
- Nelson Laboratories, Bozeman, MT. Feb, 2023
- Molecular Iodine – The World’s Most Perfect Antimicrobial Agent: Can It Control Periodontal Disease In Your Practice? Moskowitz, H. Fall, 2019
- Iodine Fact Sheet. National Institute of Health, Office of Dietary Supplements: May 1, 2024
About the authors

Dr. Herb Moskowitz is the Chairman and Co-Founder of ioTech International. He is the co-author of ioTech’s U.S. patent and global patent applications. He has also practiced clinical dentistry for more than 25 years and is a graduate of the University of Tennessee Dental School. He also has a financial interest in ioTech International, a developer and manufacturer of molecular iodine oral care products.

Dr. Janice Goodman is a member of the Oral Health Dental Journal Editorial Board. She graduated from UofT in 1979 and USC in 2015. She has practiced functional dentistry in Toronto for over 40 years. She has a financial interest in ioTech International, a developer and manufacturer of molecular iodine oral care products.












