Composite resins offer several advantages over dental amalgams beyond just esthetic benefits. Since composite resin restorations are retained through adhesion rather than mechanical retention, more conservative tooth preparation is encouraged – preserving natural tooth structure for future restorative margins, maintaining structural resistance of the remaining tooth, and decreasing the likelihood of damage to the pulp. Composite resins are not condensable, creating the challenge of achieving adequate adaption of the restorative material to the tooth preparation. Several methods to improve this adaptation have been proposed.
Some clinicians employ flowable composites as the first restorative layer. While flowable composites have improved since their introduction, they often create more shrinkage stress, and are more flexible than more highly filled composites.2 Another attempt to improve marginal adaptation is the “snow plough” technique (uncured flowable composite is dispersed by a more highly filled composite packed over it. This technique has not been extensively researched, but one clinical trial reported slightly worse marginal adaptation with “snow ploughing”.3
Another approach to better adapt composite resin to the tooth preparation is to pre-heat the composite in a warming device in order to reduce its viscosity. This objective is to reproduce the adaptation of flowable composites while maintaining the physical properties of a highly-filled resins. Several studies have reported that heating composite improves its physical and mechanical properties.3
Improvements in marginal adaptation
Heating composite reduces its viscosity.4 While flowable composites realize decreased viscosity through adjusted filler content, heated highly-filled composites attain flowability by thermal vibrations forcing monomers within the composite further apart, allowing them to more easily slide past each other.5
Laboratory studies have demonstrated better adaptation of heated composite. Heated composite restorations manifested less microleakage than room temperature or flowable restorations.5 Heated composites also generate less marginal gap formation at the tooth-restoration interface than room temperature composites.6,7
Improvements in degree of conversion
Degree of conversion is measured as the percentage of reacted C=C bonds, and represents the linking or crosslinking of resin monomers. Increasing the degree of conversion has been correlated to improved mechanical properties (strength, modulus)8 as well as decreased solubility9 of dental composites.
Light curing initiates resin photopolymerization. Monomers begin to form bonds, linking together to create crosslinked networks. As the polymer networks grow, the linking ability of individual monomers becomes restricted in the “thick soup” of the maturing polymer. The chemical reaction is now diffusion-controlled; additional bonds are limited by the frequency at which two monomer or polymers can collide together and bond, rather than the speed of the chemical reaction. Eventually, the resin vitrifies. The reactions (and double-bond conversions) cease due to a severely limited movement available within the polymer network.
Increasing the placement temperature of composite resin offers increased monomer mobility and increased segmental mobility of the polymer chains. With more movement of the monomers and flexibility of the polymer network, there is increased frequency of monomer/polymer collisions. A study of the polymerization kinetics of composite heated to 60°C determined that warming delayed the onset of diffusion-controlled propagation and increased the degree of conversion achieved prior to vitrification.10
One concern is that composite material temperature may decrease between the compule removal from the warmer and the application into the preparation. In fact, light polymerization of the composite resin should be initiated as soon as possible after removing the restorative from the warmer in order to optimize its properties.5 Another concern is that reduced filler flowable composites cool faster than more highly filled composites. Thus, conversion improvement is less likely when heating flowable composites.11
Effects on mechanical and physical properties
An increase in the degree of monomer conversion reduces the free volume within the polymer network, the space between polymer chains, and the number of hydrophilic sites within the polymer. As a direct result, preheated composites show lower sorption and solubility when compared to materials cured at room temperature.12,13
The higher double-bond conversion of heated composites may erroneously be considered to create a “tighter” polymer network and therefore increased volumetric shrinkage.14 Heating composites, in fact, increases monomer mobility and polymer chain segmental movement. This movement allows monomers to flow more easily and rearrange themselves to relieve polymerization contraction shrinkage stresses.15
Fortunately, repeated heating and cooling (up to 40 cycles) of composite resins have shown no detrimental effect on the strength of the composite. Therefore, an unused heated compule may be stored at room temperature, and reheated for use in a future procedure.16
Effects on pulpal temperature
Normal pulp temperature is between 34-35°C.17,18 Baldissara et al reported that pulpal temperature increases of 14.7°C showed no clinical or histological signs of necrosis in vital human teeth,17 and therefore, temperature increases up to this amount can be considered safe. Although composites are warmed to 68°C, a difference of 33°C to tooth temperature, the thermal experience of the pulp is significantly lower due to the insulation of remaining dentin. In a laboratory study, a thermocouple was attached to a 0.5mm thick dentin disc placed in a 37°C incubator. Composite resin warmed to 68°C was placed in contact with the other side of the dentin disc. The thermocouple temperature increase registered a mere 1-2°C.19 However, if the clinicians suspects a remaining dentin thickness less than 0.5mm, a cavity liner may be considered.
Heating and cooling rate of a composite compule
A thermocouple probe was placed inside a compule of composite resin (Phil Nano, Dental Savings Club, Montreal QC). (Fig. 1) The compule was placed inside:
- Pre-heated Calset Composite Warmer (Addent, Danbury CT)
- Compex HD Composite Gun (Addent, Danbury CT)) that was turned on once the compule was placed.
Fig. 1

The temperature of the composite compule was recorded every 30 seconds until the temperature plateaued. The compule was removed from the Calset Composite Warmer and the time required for the composite to return to room temperature was again recorded. The results indicate that it takes 3:30 minutes for the composite to heat from 23°C (room temperature) to 68°C in the Calset warmer. (Fig. 2) Once removed from the warmer, the compule cools to 43°C within 2 minutes and to 23°C (room temperature) after 6:30 minutes.
Fig. 2
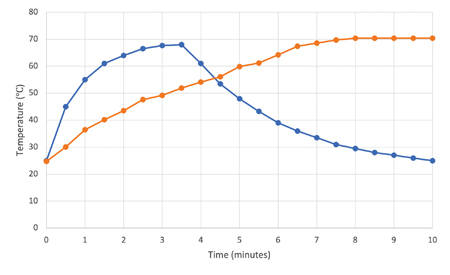
In the Compex HD Composite Gun, the composite reached its maximum temperature (70°C) in 1 minute. The composite heating occurred at the same rate whether the gun pre-heated or not. The advantage of the Compex HD gun is that there is no temperature loss in the transfer of the restorative material into the preparation.
Clinical Case
A shallow class II preparation (maximum depth 2mm) is isolated with a sectional matrix (Composi-tight 3D Fusion, Garrison, Spring Lake MI) and bonded (Phil Bond, Dental Savings Club, Montreal QC). (Fig. 3) A nanocomposite compule (Phil Nano, Dental Savings Club) is s placed into a Compex HD warming composite gun. (Fig. 4) After 1 minute of warming, the composite is placed in the cavity preparation, adapted to the floor of the preparation with the compule gun, (Fig. 5) and teased to the preparation walls with a dry Micro Scrub (Dental Savings Club, Montreal QC) applicator. (Fig. 6) The restorative material is sculpted and marginally adapted. (Fig. 7) The filling material was light cured immediately to take advantage of the warmed composite’s increased degree of conversion. (Fig. 8) The completed composite restoration. (Fig. 9)
Fig. 3.1

Fig. 3.2
Composi-tight 3D Fusion (Garrison Dental Solutions, Spring Lake MI).
Fig. 4

Fig. 5.1
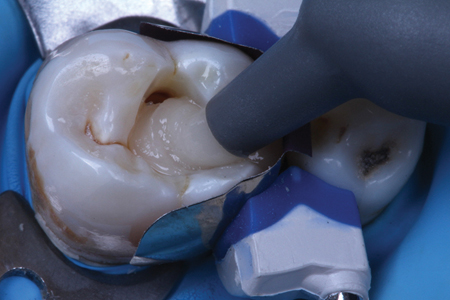
Fig. 5.2

Fig. 6.1
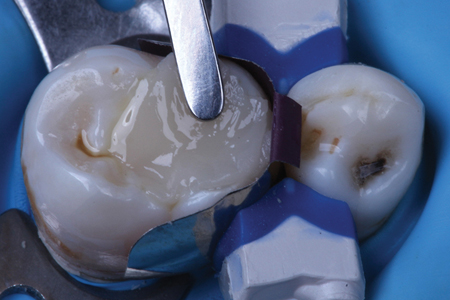
Fig. 6.2

Fig. 7

Fig. 8

Fig. 9
Summary
Heating composite resin in a warming device decreases its viscosity, allowing better adaptation of the composite to the tooth preparation. The increased monomer mobility caused by heating generates a higher degree of monomer conversion in the resin. The strength, shrinkage stress, and solubility of the composite are generally improved by composite heating. The pulpal temperature rise is minimal and is considered to be safe assuming a remaining dentin thickness of at least 0.5mm. Using a preheated composite warmer, a compule of composite takes approximately 3:30 minutes to reach 68°C. After removing the compule from the warmer, it will cool to 43°C after 2 minutes and back to room temperature within 6:30 minutes. The heated composite gun takes approximately 1 minute to reach a temperature of 68°C.
Oral Health welcomes this original article.
References
- l Sunbul H, Silikas N, Watts DC. Polymerization shrinkage kinetics and shrinkage-stress in dental resin-composites. Dent Mater. 2016 Aug;32(8):998-1006. doi: 10.1016/j.dental.2016.05.006. Epub 2016 May 28. PMID: 27240744.
- Ferracane JL, Lawson NC. Probing the hierarchy of evidence to identify the best strategy for placing class II dental composite restorations using current materials. J Esthet Restor Dent. 2021 Jan;33(1):39-50. doi: 10.1111/jerd.12686. Epub 2020 Nov 18. PMID: 33206440.
- Freedman G, Krejci I; Warming up to composites Compend Contin Educ Dent. 2004 May;25(5):371-4, 376
- Lucey S, Lynch CD, Ray NJ, Burke FM, Hannigan A. Effect of pre-heating on the viscosity and microhardness of a resin composite. J Oral Rehabil. 2010 Apr;37(4):278-82. doi: 10.1111/j.1365-2842.2009.02045.x. Epub 2009 Dec 29. PMID: 20050987.
- Wagner WC, Aksu MN, Neme AM, Linger JB, Pink FE, Walker S. Effect of pre-heating resin composite on restoration microleakage. Oper Dent. 2008 Jan-Feb;33(1):72-8. doi: 10.2341/07-41. Erratum in: Oper Dent. 2009 Mar-Apr;34(2):246. Asku, Mert N [corrected to Aksu, Mert N]. PMID: 18335736.
- Choudhary N, Kamat S, Mangala T, Thomas M. Effect of pre-heating composite resin on gap formation at three different temperatures. J Conserv Dent. 2011 Apr;14(2):191-5. doi: 10.4103/0972-0707.82618. PMID: 21814365; PMCID: PMC3146116.
- Fróes-Salgado NR, Silva LM, Kawano Y, Francci C, Reis A, Loguercio AD. Composite pre-heating: effects on marginal adaptation, degree of conversion and mechanical properties. Dent Mater. 2010 Sep;26(9):908-14. doi: 10.1016/j.dental.2010.03.023. Epub 2010 Jun 16. PMID: 20557926.
- Ferracane JL, Greener EH. The effect of resin formulation on the degree of conversion and mechanical properties of dental restorative resins. J Biomed Mater Res. 1986 Jan;20(1):121-31. doi: 10.1002/jbm.820200111. PMID: 3949822.
- da Silva EM, Almeida GS, Poskus LT, Guimarães JG. Relationship between the degree of conversion, solubility and salivary sorption of a hybrid and a nanofilled resin composite. J Appl Oral Sci. 2008 Mar-Apr;16(2):161-6. doi: 10.1590/s1678-77572008000200015.
- PMID: 19089210; PMCID: PMC4327638.
Fróes-Salgado NR, Silva LM, Kawano Y, Francci C, Reis A, Loguercio AD. Composite pre-heating: effects on marginal adaptation, degree of conversion and mechanical properties. Dent Mater. 2010 Sep;26(9):908-14. doi: 10.1016/j.dental.2010.03.023. Epub 2010 Jun 16. - Lempel E, Őri Z, Szalma J, Lovász BV, Kiss A, Tóth Á, Kunsági-Máté S. Effect of exposure time and pre-heating on the conversion degree of conventional, bulk-fill, fiber reinforced and polyacid-modified resin composites. Dent Mater. 2019 Feb;35(2):217-228. doi: 10.1016/j.dental.2018.11.017. Epub 2018 Nov 28. PMID: 30503020.
- Castro FL, Campos BB, Bruno KF, Reges RV. Temperature and curing time affect composite sorption and solubility. J Appl Oral Sci. 2013;21(2):157-162. doi:10.1590/1678-7757201302298.
- Ferracane JL. Hygroscopic and hydrolytic effects in dental polymer networks. Dent Mater. 2006 Mar;22(3):211-22. doi: 10.1016/j.dental.2005.05.005.
- Lohbauer U, Zinelis S, Rahiotis C, Petschelt A, Eliades G. The effect of resin composite pre-heating on monomer conversion and polymerization shrinkage. Dental Materials 2009;25:514-9
- Tauböck TT, Tarle Z, Marovic D, Attin T. Pre-heating of high-viscosity bulk-fill resin composites: effects on shrinkage force and monomer conversion. J Dent. 2015 Nov;43(11):1358-64. doi: 10.1016/j.jdent.2015.07.014. Epub 2015 Jul 30. PMID: 26232610.
- D’Amario M, De Angelis F, Vadini M, Marchili N, Mummolo S, D’Arcangelo C. Influence of a repeated preheating procedure on mechanical properties of three resin composites. Oper Dent. 2015 Mar-Apr;40(2):181-9. doi: 10.2341/13-238-L. Epub 2014 Aug 1. PMID: 25084104.
- Trowbridge HO, Franks M, Korostoff E, Emling R. Sensory response to thermal stimulation in human teeth. J Endod. 1980 Jan;6(1):405-12. doi: 10.1016/S0099-2399(80)80216-0.
- Baldissara P, Catapano S, Scotti R. Clinical and histological evaluation of thermal injury thresholds in human teeth: a preliminary study. J Oral Rehabil. 1997 Nov;24(11):791-801. doi: 10.1046/j.1365-2842.1997.00566.x.
- El-Deeb HA, Abd El-Aziz S, Mobarak EH. Effect of preheating of low shrinking resin composite on intrapulpal temperature and microtensile bond strength to dentin. J Adv Res. 2015 May;6(3):471-8. doi: 10.1016/j.jare.2014.11.013. Epub 2014 Dec 24. PMID: 26257945; PMCID: PMC4522590.
About the Author
 Preshtha Mangla is a 2nd year resident in the Biomaterials residency at UAB School of Dentistry.
Preshtha Mangla is a 2nd year resident in the Biomaterials residency at UAB School of Dentistry.
 Nate Lawson is the Director of the Division of Biomaterials and the Program Director of the Biomaterials Residency at the UAB School of Dentistry.
Nate Lawson is the Director of the Division of Biomaterials and the Program Director of the Biomaterials Residency at the UAB School of Dentistry.












