Introduction and Background
Cleft lip and palate is one of the most common craniofacial defects involving the face and jaws with a worldwide frequency of 1 in 700. 1 While cleft lip and palate rarely results in mortality, the associated morbidity is significant with aesthetic, functional and psychosocial challenges for the child as well as a social and financial burden for the family. 2 The cleft lip and palate defect arises from the failure of fusion of the facial processes during the first four to eight weeks post conception. 3,4 The failure of fusion of the median nasal and maxillary processes results in a cleft lip and for defects extending into the nostril, failure of fusion with the lateral nasal processes is also involved. 5 Clefts of the palate result from failure of fusion of the medial nasal segments and failure of elevation and fusion of the palatal shelves of the maxillary processes. 5,6 There can be large variation in the presentation of cleft lip and palate depending on which and to what extent the facial processes have been affected. Broadly they can be categorized into two main groups. One group includes clefts that involve the lip with or without the palate (CL/P) and these may be subdivided into either unilateral or bilateral. 1 The other group includes clefts which involve the palate only (CP). 1 Both of these groups can be further divided into syndromic cases for which the clefts are associated with other physical and developmental anomalies versus non syndromic cases where the cleft defect occurs in isolation. 7 The majority of cleft lip and palate cases are non syndromic in nature with multiple studies reporting that approximately 70% of CL/P and 50% of CP cases are isolated defects and not associated with a syndrome. 1,2,8,9
The distribution of cleft lip and palate is not uniform and there is considerable variation among different ethnicities and geographical origins with higher rates reported for American Indian and Asian populations at 1 in 500 or greater and lower rates reported for African populations at 1 in 2500, with Caucasian populations in between. 1,10 On the individual level, it is more common for clefts to be unilateral on the left as well as showing a higher predilection for males compared to females. 11
It is difficult to isolate the etiological factors that result in a cleft lip and palate and little is known about what causes the defect. Current evidence points to potential contributions from both genetic factors, environmental factors and the interaction between the two. 1-3
The diagnosis of cleft lip and palate is often made prenatally through the use of ultrasound, the first line imaging modality in obstetrics and gynecology. 12-14 Ultrasound has been shown to have a high specificity, i.e., there are little false positives but a low sensitivity and detection rate. 13,14 Maarse and colleagues in a systematic review found that prenatal detection rates varied from 0% to 73% for all types of cleft, 9% to 100% for CL/P and 0% to 22% for CP. 15 Prenatal diagnosis of cleft lip and palate enables the cleft and craniofacial team to prepare and support the parents by providing information and reviewing cleft treatment prior to the birth of their child. 14 For those cases not identified prenatally, the diagnosis of cleft lip and palate is made at birth, which can be emotionally distressing for the parents. 16
Treatment
The first milestone surgical intervention in the treatment of cleft lip with or without palate (CL/P) is the repair of the lip commonly performed around three to six months of age. For isolated cleft palate (CP) cases, the first milestone surgical intervention is the closure of the palate commonly performed at 12-18 months of age. Prior to the repair of the lip, some centers employ presurgical infant orthopedics (PSIO) to narrow the cleft defect and improve the alignment of the maxillary segments. 17 PSIO was first introduced in the 1950s by McNeil and since then many different types of orthopedic devices ranging from active to passive have been described in the literature. 17 Active appliances are designed to use springs and screws to deliver an active force to reposition the segments for example, the Latham appliance. 17,18 Semi-active appliances such as that originally proposed by McNeil use modifications to an acrylic plate to mold the segments into the desired position. 17,19 Passive appliances rely on the removal of definitive areas of the plate to induce development of the segments into the desired alignment such as the system proposed by Hotz. 17,20
The primary goal and benefit of PSIO is the reduction in the size of the cleft and approximation of the maxillary alveolar segments prior to the lip surgery. Despite it’s introduction over 50 years ago, PSIO continues to be a controversial topic and there is no long-term quality evidence to demonstrate whether the benefits seen in the short term prior to lip surgery have positive effects on long term treatment outcomes. Prahl and colleagues summarized the arguments used by those in favor of PSIO. 17,21 Proponents of PSIO argue that this approach allows for a more normalized pattern of deglutition, prevents twisting and dorsal position of the tongue in the cleft, reduces the cleft width, prevents crossbites, and improves feeding, nasal breathing, middle ear conditions and speech development. PSIO has also been claimed to improve the alignment of the arch form and position of the alar base as well as straightening the nasal septum and facilitating surgery by reducing tension on the repair. Moreover, the use of PSIO involves the parents in the treatment and provides a positive psychological effect. 17,21 Opponents of PSIO claim that the procedure is not evidence based and is complex, expensive and places an increased burden on the family in terms of travel and compliance. 17,21 The difficulty in acquiring quality evidence to evaluate the effectiveness of PSIO is in part due to the large variation in treatment protocols of the different teams. Shaw and colleagues reported that in the Eurocleft project, out of 201 centres registered with the network, 194 different protocols were being used. 22 As PSIO takes place very early in the child’s life, it is difficult to isolate the effect of PSIO from the effects of subsequent surgical procedures. Moreover existing studies are predominantly retrospective, with small samples sizes and poor definition of groups, cleft type and treatment. 21 With the lack of conclusive evidence available, the use of PSIO comes down to the preference of the cleft team and approximately 50% of European centres and more than 40% of centres in the United States utilize PSIO. 22,23 At The Hospital for Sick Children (SickKids) in Toronto, there is a strong preference for the use of PSIO in the form of Nasoalveolar Molding (NAM).
The SickKids Approach
Nasoalveolar Molding is a type of PSIO introduced by Grayson in 1993. 24 It consists of an acrylic plate, which encompasses the premaxilla and alveolar segments. The plate is progressively adjusted and areas ground away to facilitate movements of the maxillary segments. Once the cleft size is reduced stents fabricated from wire are added to the plate and coated in acrylic and soft denture liner to mold the lateral cartilages and nasal tip. The principle was based on the research of Matsuo, who determined that auricular cartilage and nasal cartilage could be molded early in the neonatal period due to temporary plasticity of the cartilage thought to arise from the increased level of estrogen circulating in the first few weeks postpartum. 25-27 The primary objective of NAM like all PSIO procedures it to decrease the severity of the initial cleft deformity with goals of; reduction in the width of the alveolar cleft segments, lip segments that are almost approximated at rest, symmetrical lower lateral alar cartilages and adequate nasal mucosal lining. 28 In summary, the goal is to restore the skeletal, cartilaginous and soft-tissue relationships prior to surgery.
The approach taken at SickKids involves the use of NAM. The initial appointment in the dental department occurs on referral from the plastic surgeon and cleft coordinator. The infant is examined to determine the type and extent of the cleft defect and a management plan is formulated based on the severity of the defect (Figs. 1 & 2). As alluded to earlier, isolated CP cases generally do not require NAM as the alveolar segments and lips are intact. For CL/P cases, the severity of the cleft determines if NAM will be utilized. Once the decision to proceed with NAM has been made, the treatment plan is discussed with the parents and consent obtained. An impression is taken with rapid set heavy body polyvinyl siloxane material and once set it is removed and the infant’s mouth immediately checked for any residual impression material (Fig. 3). The impression is poured up in dental stone and the acrylic molding plate fabricated on the dental cast (Fig. 4).
Fig. 1

Fig. 2

Fig. 3

Fig. 4

An insertion appointment is made one week later and the plate is tried in to ensure a good fit and correct extension. Care is taken to adjust the border of the plate to allow for adequate frenal relief and reduce potential areas of ulceration. 28 The parents are instructed on the wear and care of the plate, ensuring that it is worn full time and taking it out for cleaning a minimum of once per day. 28 The plate is retained utilizing orthodontic elastics to engage the retention arm and attached to the cheek with surgical tapes, which are changed once daily. A skin barrier base tape, such as DuoDerm® or Mepitac®, is placed on the cheek first to reduce the trauma to the skin from repeated tape changes. An example of a molding plate at insertion for an infant with a bilateral complete cleft lip and palate is illustrated above (Fig. 5). The surgical tapes and elastics serve to both retain the molding plate as well as provide a posteriorly directed force to help approximate the alveolar segments. The parents are then provided with feeding guidance and instruction from the occupational therapist.
At the subsequent appointment one to two weeks later, the soft tissue is checked to ensure no ulcerations have developed and the plate extensions trimmed to ensure there is no resistance and interferences as the alveolar segments move closer together. Lip taping is added to provide additional force to approximate the lip segments (Fig. 6). At this same appointment, soft denture liner may be added to the internal aspect of the plate to increase pressure and direct the alveolar segments into the desired position (Fig. 7). Appointments are scheduled every week or fortnight and adjustments made by trimming the plate and addition of soft denture liner to continue to move the segments together as necessary.
Fig. 5

Fig. 6
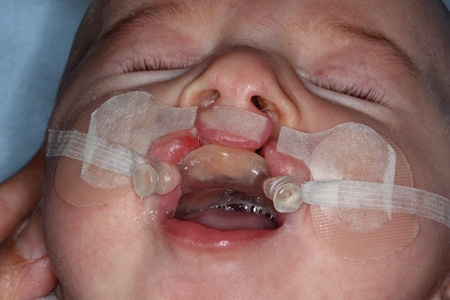
Fig. 7

Once the distance between the alveolar segments is less than 5 mm, preparations can be made for the addition of the nasal stent to elevate and direct the nasal rim and tip (Fig. 8). It is important to allow for the cleft size to be reduced prior to the addition of the nasal stent as it allows for laxity in the alar rim and the proper assessment of the nostril size and position. 28 If the stent is introduced prematurely an increased nostril circumference may result once the cleft segments are approximated. 28 The stent is fabricated from 0.032-inch (0.8mm) stainless steel wire and is attached to the plate medial to the retention arm and enters the nostril 3 to 4 mm past the nostril aperture. The end may take the form of a teardrop or kidney bean and is coated with hard acrylic and a final layer of soft denture liner. Bilateral cases require two nasal stents and provide the opportunity for columella lengthening if required utilizing soft denture liner and vertical taping of the lip (Fig. 9). At the nasal stent insertion appointment, the plastics team is notified that the stent has been placed so that they can plan for the lip repair surgery. The patient is continually reviewed weekly to fortnightly and adjustments made to the nasal stent and molding plate as required. Once the plastic surgeon is happy with the progress, the patient is given a final presurgical check and instructions. In the five days prior to the surgery, lip taping is reduced to ensure that soft tissue surrounding the lip is in pristine condition prior to the repair. The changes that can be achieved by NAM in these short few months can be quite dramatic and rewarding for both clinician and parents (Fig. 10).
Fig. 8

Fig. 9

Fig. 10

The question of whether these changes make a difference to the final outcome for the patient in the long-term still needs to be answered. The suggested main advantage of NAM over other forms of PSIO is the improvement in nasal aesthetics and symmetry. Uzel and Alparslan in their systematic review on the long term effects of PSIO found nine controlled clinical trials in the literature reporting on NAM, however only one of these studies contained a control group without a PSIO and a follow up of more than six years. 29 They concluded that while the studies on NAM show encouraging results for nasal symmetry, future randomized controlled trials are needed. In the absence of strong conclusive evidence supporting or refuting NAM, the continued use of NAM here at SickKids is driven by the positive results and clinical preference of the cleft team.
In our experience, we feel that NAM results in a more predictable surgical outcome allowing nasal symmetry to be more reliably achieved with a direct impact on the aesthetic result post surgery. Moreover, we have found that NAM has a positive effect on the parents as they are engaged in the treatment of their child and can witness the impact of their work on treatment progress. It is our opinion that the benefits of NAM outweigh the risks and that it has an overall positive effect on treatment outcome that is worth pursuing. OH
Oral Health welcomes this original article.
References
- Murray JC. Gene/environment causes of cleft lip and/or palate. Clin Genet. 2002 Apr;61(4):248-56.
- Dixon MJ, Marazita ML, Beaty TH, Murray JC. Cleft lip and palate: understanding genetic and environmental influences. Nat Rev Genet. 2011 Mar;12(3):167-78.
- Mossey PA, Little J, Munger RG, Dixon MJ, Shaw WC. Cleft lip and palate. Lancet. 2009 Nov 21;374(9703):1773-85.
- Proffit WR, Fields HW, Sarver DM. Contemporary orthodontics. 5th ed. St. Louis, Mo.: Elsevier/Mosby; 2013. p. p.
- Jiang R, Bush JO, Lidral AC. Development of the upper lip: morphogenetic and molecular mechanisms. Dev Dyn. 2006 May;235(5):1152-66.
- Ferguson MW. Palate development. Development. 1988;103 Suppl: 41-60.
- Prescott NJ, Winter RM, Malcolm S. Nonsyndromic cleft lip and palate: complex genetics and environmental effects. Ann Hum Genet. 2001 Nov;65(Pt 6):505-15.
- Calzolari E, Bianchi F, Rubini M, Ritvanen A, Neville AJ, Group EW. Epidemiology of cleft palate in Europe: implications for genetic research. Cleft Palate Craniofac J. 2004 May;41(3):244-9.
- Calzolari E, Pierini A, Astolfi G, Bianchi F, Neville AJ, Rivieri F. Associated anomalies in multi-malformed infants with cleft lip and palate: An epidemiologic study of nearly 6 million births in 23 EUROCAT registries. Am J Med Genet A. 2007 Mar 15;143A(6):528-37.
- Vanderas AP. Incidence of cleft lip, cleft palate, and cleft lip and palate among races: a review. Cleft Palate J. 1987 Jul;24(3):216-25.
- Hennekam RCM, Allanson JE, Krantz ID, Gorlin RJ. Gorlin’s syndromes of the head and neck. 5th ed. Oxford ; New York: Oxford University Press; 2010. p. lxi, 1452 p.
- Morgan S, Unipan A, Datta S. Ultrasound in obstetrics and gynaecology. Obstet Gynaecol Reprod Med. 2016;26(6):175-183.
- Steinberg JP, Gosain AK. Thirty Years of Prenatal Cleft Diagnosis: What Have We Learned? Plast Reconstr Surg. 2015 Sep;136(3):550-7.
- Johnson N, J RS. Prenatal diagnosis of cleft lip and palate. Cleft Palate Craniofac J. 2003 Mar;40(2):186-9.
- Maarse W, Berge SJ, Pistorius L, van Barneveld T, Kon M, Breugem C, et al. Diagnostic accuracy of transabdominal ultrasound in detecting prenatal cleft lip and palate: a systematic review. Ultrasound Obstet Gynecol. 2010 Apr;35(4):495-502.
- Davalbhakta A, Hall PN. The impact of antenatal diagnosis on the effectiveness and timing of counselling for cleft lip and palate. Br J Plast Surg. 2000 Jun;53(4):298-301.
- Berkowitz S. Cleft lip and palate : diagnosis and management. Third Edition. ed. New York: Springer; 2013. p. 982 pages.
- Latham RA, Kusy RP, Georgiade NG. An extraorally activated expansion appliance for cleft palate infants. Cleft Palate J. 1976 Jul;13:253-61.
- Mc NC. Orthodontic procedures in the treatment of congenital cleft palate. Dent Rec (London). 1950 May;70(5):126-32.
- Hotz MM. Pre- and early postoperative growth-guidance in cleft lip and palate cases by maxillary orthopedics (an alternative procedure to primary bone-grafting). Cleft Palate J. 1969 Oct;6:368-72.
- Prahl C, Kuijpers-Jagtman AM, van’t Hof MA, Prahl-Andersen B. A randomised prospective clinical trial into the effect of infant orthopaedics on maxillary arch dimensions in unilateral cleft lip and palate (Dutchcleft). Eur J Oral Sci. 2001 Oct;109(5):297-305.
- Shaw WC, Semb G, Nelson P, Brattstrom V, Molsted K, Prahl- Andersen B, et al. The Eurocleft project 1996-2000: overview. J Craniomaxillofac Surg. 2001 Jun;29(3):131-40; discussion 141-2.
- Kornbluth M, Campbell RE, Daskalogiannakis J, Ross EJ, Glick PH, Russell KA, et al. Active Presurgical Infant Orthopedics for Unilateral Cleft Lip and Palate: Intercenter Outcome Comparison of Latham, Modified McNeil, and Nasoalveolar Molding. Cleft Palate Craniofac J. 2018 May;55(5):639-648.
- Grayson BH, Cutting C, Wood R. Preoperative columella lengthening in bilateral cleft lip and palate. Plast Reconstr Surg. 1993 Dec;92(7):1422-3.
- Matsuo K, Hirose T. Nonsurgical correction of cleft lip nasal deformity in the early neonate. Ann Acad Med Singapore. 1988 Jul;17(3):358-65.
- Matsuo K, Hirose T, Tomono T, Iwasawa M, Katohda S, Takahashi N, et al. Nonsurgical correction of congenital auricular deformities in the early neonate: a preliminary report. Plast Reconstr Surg. 1984 Jan;73(1):38-51.
- Grayson BH, Cutting CB. Presurgical nasoalveolar orthopedic molding in primary correction of the nose, lip, and alveolus of infants born with unilateral and bilateral clefts. Cleft Palate
Craniofac J. 2001 May;38(3):193-8. - Grayson BH, Maull D. Nasoalveolar molding for infants born with clefts of the lip, alveolus, and palate. Semin Plast Surg. 2005;19(4):294-301.
- Uzel A, Alparslan ZN. Long-term effects of presurgical infant orthopedics in patients with cleft lip and palate: a systematic review. Cleft Palate Craniofac J. 2011 Sep;48(5):587-95.
About the Authors
 Dr. Richard Lee is a former Clinical Fellow in Orthodontics at the Hospital for Sick Children in Toronto. He is a graduate of the University of Western Australia where he undertook both his general dental and specialist training and is currently in private practice in Perth, Australia.
Dr. Richard Lee is a former Clinical Fellow in Orthodontics at the Hospital for Sick Children in Toronto. He is a graduate of the University of Western Australia where he undertook both his general dental and specialist training and is currently in private practice in Perth, Australia.

Dr. Bruno Vendittelli, DDS, D. ORTHO, FRCD (C) is a Toronto based orthodontist whose practice is Forest Hill Orthodontics. He is a Staff Orthodontist at the Hosptial for Sick Children and an Associate at the University of Toronto, Faculty of Dentistry.
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












