Introduction
The severely worn dentition often poses a challenge to the restorative clinician. Diagnosis and treatment planning involve multidisciplinary and in-depth evaluation of etiological, esthetic, occlusal, functional and preventive factors. Modern dentistry has made tremendous progress in areas of decay prevention, treatment of periodontitis and preservation of the natural dentition. Patients in general are more than ever informed and equipped to preserve their natural teeth and oral health, however, the prevalence of tooth wear from multi-factorial causes appears to be increasing in the dentate population. At the same time, global life expectancy has increased significantly. Hence, the profession is seeing an older population group presenting with severely worn teeth from normal day-to-day function seeking to maintain oral health quality of life. These older patients’ dentitions appear to have reached the “end” of their structural life span: a rather uncommon clinical presentation when life expectancy was merely 55 to 60 years. It is therefore important for dental professionals to recognize early signs that may indicate future long-term irreversible structural damage of the dentition which can initiate early prevention and adequate treatment. Severely worn dentition cases can unfortunately require comprehensive full mouth rehabilitation to restore compromised esthetics, occlusion and loss of vertical dimension in order to reach the goals of an ideal stable outcome. Financial constraints are a common barrier to comprehensive reconstructive treatment especially when segmentation of the rehabilitation over several years is not possible without accepting compromises in esthetics and occlusion. This article will review some common causes of severe tooth wear, some guidelines to identify and evaluate case difficulty, challenges presented by severe tooth wear and how it affects occlusal vertical dimension (OVD) and a systematic protocol to treatment plan incorporating the esthetics of the smile. The clinical images in this article are examples of patients referred and treated by the author in a contemporary specialty prosthodontics practice.
Prevalence of Tooth Wear
Extensive tooth wear seems to have been the norm in ancient civilizations and the main attributed cause was coarse diet related. This is well supported by anthropological studies. In today’s societies, it is extremely rare to find the severity of wear identified in historical remains. In the case of the contemporary elderly patient, a longer life span implies a higher likelihood of advanced tooth wear. This risk simply increased, as the elderly patient remains dentate for longer years. 1,2 Prevalence studies on tooth wear in older individuals is sparse. In addition, lack of consensus on methods of assessments can make comparisons of degree of wear unreliable. There is however some concerning data indicating that dental wear is on the increase in adolescents and young adults, mainly as a consequence of an erosive process. A recent consensus report indicates increased prevalence and concern for erosive tooth wear in younger populations. 3
The problems and challenges associated with severe tooth wear are likely to place greater demands on the dental profession for the next decades. In spite of advances in fully implant-supported prostheses, we can expect to continue to save and restore natural dentitions when indicated.
Etiology and Mechanisms of Tooth Wear
Tooth Wear is considered pathologic when the loss of tooth surface becomes excessive and affects the appearance or function of the dentition or causes discomfort. The clinical outcome and presentation of the dentition describe the multifactorial underlying causes. 1,2,4
The dental literature refers to Attrition, Abrasion and Erosion as terms to describe tooth wear, although these terms do not refer specifically to the descriptive process of tooth wear. The processes involved can include functional or para-functional patterns of movement, opposing restorative material (differential wear), diet (course, acidic), diseases (reflux or eating disorder), salivary factors, occupational environment, oral hygiene, lifestyle in general and bruxism. Generally, the diagnosis of bruxism is based on the dentist’s opinion and is seldom verified by an accurate/reliable diagnostic test (somnography, video/audio recordings). The most common clinical findings corroborated with bruxism is opposing matched wear facettes resulting from intense tooth grinding. 1
Clinical Case 1
Attrition
Attrition is the physiological wear of tooth structure as a result of tooth-to-tooth contact as in mastication with possible abrasive material intervention between the involved surfaces. It occurs primarily on the functional occlusal and incisal surfaces that come into contact during mastication.
Abrasion
Abrasion is the physical wear of tooth surfaces by an abnormal mechanical process independent of occlusion. The process involves a foreign object or substance repeatedly contacting the tooth. The site and pattern of the abrasive lesion can be diagnostic because different foreign bodies produce different patterns of abrasion.
Erosion
Erosion is the loss of tooth surface by a chemical process that does not involve bacterial action. It is basically caused by chronic exposure of teeth to acids from external and internal sources, resulting in characteristic patters and distributions of the lesions. Erosion typically presents as concave bilateral defects without the soft rough chalkiness associated with bacterial decay lesions. Early stages of erosion affect enamel, resulting a shallow, smooth, glazed surface without ridges or stain lines. Erosive lesions are typically free of plaque deposits and exhibit a “clean” surface. In advanced erosion cases, restorations can project above the occlusal surfaces and the cusps/convexities/incisal edges show concavities know as “cupping.” Intrinsic causes (gstric acid reflux) of erosion affect the palatal surfaces of the maxillary teeth showing concave depressions. Extrinsic causes (citric fruits, soda, etc.) is typically more evident on the labial surfaces of the maxillary teeth exhibiting scooped-out depressions. Erosive lesions located on the palatal surfaces of the maxillary teeth as a result of chronic vomiting have been termed as perimolysis or perimylolysis. It is believed that these lesions are caused by the tongue directing the vomitus forward during self-induced vomiting (anorexia and bulimia nervosa), while the lateral spread of the tongue protects the mandibular teeth along with the diluting capacity of the saliva from the mandibular salivary glands.
Fig. 1

Differential Diagnosis and Treatment Options
Clinically, it is often difficult to clearly differentiate among erosion, abrasion, and attrition. Tooth wear could originate from a combination of causes. Although there could be a dominant factor causing severe wear of a dentition, one can easily understand that a patient suffering from moderate gastric reflux in combination with para-functional bruxism would potentially suffer from a more rapid rate of wear than another patient that bruxes in the absence of any gastric reflux. A careful clinical examination in conjunction with a thorough case history (dental, medical and diet), high quality photographs and diagnostic models are imperative for diagnosis and treatment planning. Study casts and photographs appear to be the most reliable methods of monitoring the progression or severity of tooth wear over time.
There seems to be a general consensus among dental professionals that severe tooth wear appears to have a multifactorial etiology 1,2,4 in which extrinsic and intrinsic erosive acids, abrasion, and attrition may all contribute simultaneously or at different times to the manifestation of tooth wear. Early diagnosis, identification of the cause and regular monitoring enables initial prevention, management and timely initiation of adequate restorative treatment when required.
A systematic review 5 of treatment options for tooth wear reports that the present evidence is not strong enough to form conclusions. The clinician may therefore have difficulties deciding which treatment option to choose to resolve complex situations of advanced tooth wear. This review presents a few guidelines and clinical implications. The available evidence suggests the use of diagnostic waxing and diagnostic tooth arrangement. The use of centric relation is advised for the occlusal positioning for rehabilitation. Testing of the OVD increases with a removable appliance and the use of a provisional stage before definitive treatment is recommended. Both composite resins and glass ceramics are indicated, and a protective appliance with regular post-treatment evaluation is advised for follow-up.
Case Severity and Difficulty
The American College of Prosthodontists (ACP) has developed a classification system6 designed for use by dental professionals in the diagnosis and treatment of completely dentate patients. Four categories of a completely dentate situation are defined (Class I – IV), differentiated by specific diagnosis criteria, with Class I representing an uncomplicated situation and Class IV representing the most complex clinical situation. This classification can assist the dentist in assessment of case difficulty and decision to treat or refer for treatment. This system includes two broad diagnostic criteria relevant to the classification: tooth condition and occlusal scheme.
Class I (uncomplicated) classification level is characterized by an ideal or minimally compromised tooth condition and occlusal scheme:
- Ideal or minimally compromised tooth condition: No localized adjunctive therapy required. Pathology affecting the coronal morphology of three or fewer teeth in a sextant.
- Ideal or minimally compromised occlusal scheme: No pre-prosthetic therapy required. Contiguous, intact dental arches.
Class IV (most complex) classification level is characterized by severely compromised tooth conditions requiring extensive therapy and/or reestablishment of occlusal scheme with change in the occlusal vertical dimension:
- Severely compromised tooth condition: Tooth condition – insufficient tooth structure to retain or support intracoronal or extracoronal restorations – in three or more sextants. Pathology affecting the coronal morphology of four or more teeth in all sextants. Teeth require localized adjunctive therapy, i.e., periodontal, endodontic, or orthodontic procedure in three or more sextants.
- Severely compromised occlusal scheme: Major therapy required to reestablish the entire occlusal scheme including any necessary changes in the OVD.
Challenges in Treatment of the Severely Worn Dentition
A. Occlusal Vertical Dimension (OVD)
It is commonly assumed, without definitive evidence that extensive occlusal wear results in decreased OVD. However, it is also possible that gradual tooth wear can be compensated by continuous eruption of the affected teeth, maintaining OVD. On the other hand, occlusal wear may occur at a faster rate than continuous compensative eruption, resulting in a loss of OVD. 4 There are several methods to evaluate OVD (phonetics, interocclusal distance, facial appearance, etc.) as well described in a literature review. 7 Loss of posterior occlusion support is probably the most common cause of decreased OVD.
The major restorative challenge is often the lack of adequate restorative space. There are situations where restoration of a worn dentition can only be accomplished predictably by increasing the OVD.
A classic paper by Turner et al. categorizes severe wear patients in three categories:
- Category 1: Excessive wear with loss of OVD
- Category 2: Excessive wear without loss of OVD but with space available.
- Category 3: Excessive wear without loss of OVD but with limited space
Category 2 patients have maintained OVD by continuous eruption. Restorative space can be achieved by increasing the OVD as part of the final reconstruction. Analysis of articulated diagnostic casts in centric relation may reveal an anterior slide form Centric Relation (CR) to Maximum Intercuspation Position (MIP). In these cases, equilibration or restoration of the posterior teeth can provide occlusal stability in centric relation and favorably provide adequate restorative space for the anterior teeth.
Category 3 patients are the most difficult because vertical space must be obtained to accommodate restorative materials. Treatment sometimes requires an interdisciplinary approach including pre-prosthetic orthodontics, clinical crown lengthening, orthognathic surgery and programmed OVD increase.
Retention and resistance forms require minimal clinical crown heights for full coverage restorations. In the absence of adequate tooth preparations or sufficient crown heights, the long-term success of restorations can be compromised leading to loss of cement seal and failure of the restoration. The general rule for full coverage crowns, teeth should be prepared so that they exhibit the following characteristics: 10 to 20 degrees of total occlusal convergence, a minimal occlusocervical dimension of 4 mm for molars and 3 mm for other teeth, and an occlusocervical-to-faciolingual dimension ratio of 0.4 or greater. 8 These guidelines for minimal tooth dimensions may be used as a tool to initiate restorative treatment before tooth wear leads to less than ideal preparation heights or help avoid/prescribe crown lengthening procedures.
Clinical Case 2
B. Treatment Planning Challenges
Planning treatment for severely worn teeth is difficult because of all the different scenarios that can occur when teeth wear. In some patients, wear is isolated to few teeth, which means the vertical dimension has not changed, one can conclude that if the worn teeth are in occlusion, they must have erupted. Other patients have wear on all their teeth, which indicates the possibility of loss of OVD, but there is no certainty of loss of OVD as the teeth may have erupted at the same rate as they wore down. This dilemma is one of the major challenges in treating the worn dentition. Increasing the OVD to achieve space for restorative materials where there has been no apparent loss of OVD is seldom advisable; but if deemed necessary, the increase should be minimal to achieve the final restorative goals of occlusion. 9 As a general rule, it is advised to “test” the planned increase in OVD with an occlusal appliance or with fixed provisional restorations. There is no indication that permanent alteration in the OVD will produce long-lasting TMD symptoms. 10
When the entire dentition is severely worn requiring reconstruction of the occlusion with increased OVD in CR, a full mouth rehabilitation involving full coverage restorations would generally provide the most flexibility in achieving the predictable esthetics and function. Most often, the entire dentition must be treated comprehensively in a controlled and rather short period of time. Financial limitations of the patient may limit the clinician’s ability to treat severely worn dentitions comprehensively. Fortunately, advances in adhesive direct composite restorations can provide flexibility in select cases to restore part of the mouth to ideal occlusion, form and function while definitive ceramic restoration may be used to treat the rest of the dentition. The composite restorations can eventually be replaced with porcelain restorations over time to complete treatment in a “segmented” fashion without compromising the ideal plane of occlusion, esthetics and function.
Fig. 2

Clinical Case 3
C. Prosthodontic Treatment Planning
The goals of comprehensive prosthodontic rehabilitation should ideally include esthetic and functional outcomes while providing improved oral health related quality of life with restorations that are maintainable in the long-term. In the author’s experience, most dentate patients with severely worn dentitions present with little to no symptoms or impairment of their chewing ability. However, the majority of these patients express concerns about loss of tooth structure and esthetic issues. The esthetic concerns of patients are broad. They typically include short teeth, lack of tooth display at rest and smile, darkened areas of exposed dentin on mandibular teeth, thin eroded enamel showing the underlying dentin and less frequently, altered irregular gingival margins. Esthetic impediments are frequently evident at initial examination. Severely worn dentitions are often associated with healthy periodontiums with minimal to no attachment loss. Periodontal management may involve correction of gingival levels if they have been altered or if there is insufficient clinical crown height.
Traditional prosthodontics approaches the problem of the worn dentitions by evaluating changes in occlusion (Articulated models, CR and MIP) and the etiology of wear. This is critical for prognosis and when it comes to the actual reconstructive treatment. However, mounted models, occlusal evaluation and severity of wear, without references to the esthetics of the smile in the facial frame, are insufficient to develop a systematic and predictable comprehensive plan.
Contemporary prosthodontic protocols integrate esthetic features of the smile and the face. As in complete denture therapy 11 where there is total loss of the dentition and periodontium, a comprehensive evaluation and treatment plan should include the role of tooth position, dimension, shape in relation to the facial appearance integrating symmetry, harmony and occlusal function. Spear 12 describes an effective and systematic Facially Generated Treatment Planning approach for the worn dentition in eight steps that emphasized on both esthetic and occlusal goals of treatment. This approach has many similarities and parallels to complete denture tooth set up.
Fig. 3
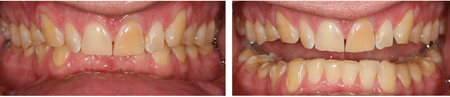
Fig. 4

Fig. 5

Fig. 6

Clinical Case 4
Facially Generated Treatment Plan
The eight steps, supported with articulated models, IO and EO photographs and wax-up, are carried out in the following order:
1. Maxillary Central Incisal Edge position: this is evaluated at rest and in a full smile
2. Maxillary Incisor Inclination: this relates to the labial/lingual inclination and affects overjet
3. Maxillary Occlusal Plane: this step evaluates the position of the remaining maxillary teeth with the desired position of the maxillary central incisor
4. Determine Ideal Gingival Levels: this step evaluates the required gingival alterations required based on the creation of ideal width/height of the worn and/or erupted teeth
5. Mandibular Incisor Incisal Edges: this step is also evaluated at rest and smile in relation to the face. It is fairly common to notice over-eruption of mandibular incisors in wear cases.
6. Mandibular Incisor Inclination: this step and the next two are carried out on mounted models. This considers the desired occlusal relationship and etiology of wear. The overjet is determined in this step
7. Mandibular Occlusal Plane: this step corrects and levels the mandibular plane as well as helps evaluate any correction required for over-erupted teeth if any.
8. Evaluate Mandibular Anterior Gingival Levels: As in step 4, this is where ideal tooth width/height based confirms if there was any over-eruption of the lower anterior sextant and the necessary gingival corrections that should be included on the treatment plan.
The facially generated treatment planning approach is used for treatment planning, interdisciplinary referrals (periodontist, oral surgeon, endodontist) and can significantly differ from the actual sequence of treatment when it is being rendered. It is beyond the scope of this article to discuss sequential planning between all the disciplines. However, it is important to highlight, that an essential part of the prosthodontics phase is the meticulous esthetic, occlusal and functional evaluation of the provisional restorations prior to finalization of the definitive restorations for predictable esthetic and functional success.
Fig. 7

Clinical Case 5
Role of Primary Care Provider
Patients are most likely being monitored regularly by their primary care provider at recall examinations and hygiene appointments. It is critical to identify patients that are at risk or already showing signs of wear to initiate a discussion about the possible etiologies. Palliative care, prevention (occlusal guard, topical fluoride), counseling (diet and lifestyle, physician referral (gastric reflux), possible restorative treatment or discussion of future restorative treatment can be presented to patients as they can be completely unaware of their present or likely future dental condition. Another important observation is the severity/rate of wear regardless of etiology. There is some sense of urgency for patients presenting with severe active erosive wear in their mid-twenties compared to an older patient with the same degree of wear in their late 60’s.
Fig. 8

Fig. 9

Fig. 10

Fig. 11

Fig. 12

Fig. 13

Fig. 14
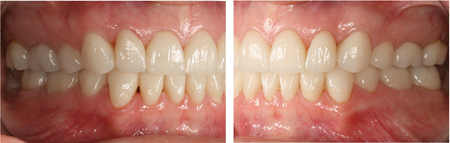
Fig. 15

Clinical Cases 6 & 7
Conclusion
Restoration of the extremely worn dentition presents a substantial challenge to the dental profession. Thorough and systematic evaluation of the etiology, history, and factors relative to OVD are essential to appropriate treatment planning. Various modalities, including direct or indirect techniques, can be successful in the treatment of patients with a worn dentition. A team approach that uses combined inter-disciplinary expertise will assure the longevity of the restoration for the patient while providing esthetic and functional outcomes. Comprehensive treatment planning should follow a well-sequenced approach that not only accounts for tooth wear but the overall esthetics and occlusion. In the absence of strong evidence-based guidelines regarding treatment protocols, the current literature provides some suggestions and clinical implications in patient management. As physical properties of restorative materials, adhesive technology and digital impressions and restoration fabrication continue to improve, the dental professional can hope to provide more conservative reconstructive treatment involving less “sound” tooth preparations in the future. OH
Fig. 16

diagnosed gastric reflux. Bruxism is a risk factor in addition to the erosive problem, so the absence of enamel on the functioning surfaces can lead to rapid wear even with treatment of the gastric reflux. This scenario presents with relative urgency for some form of restorative treatment followed with a preventive occlusal guard.
Fig. 17

Oral Health welcomes this original article.
References
- Hattab FN, Yassin OM. Etiology and diagnosis of tooth wear: a literature review and presentation of selected cases. Int J Prosthodont. 2000 Mar-Apr;13(2):101-7.
- Johansson A, Johansson AK, Omar R, Carlsson GE. Rehabilitation of the worn dentition. J Oral Rehabil. 2008 Jul;35(7):548-66.
- Carvalho TS, Colon P, Ganss C, Huysmans MC, Lussi A, Schlueter N, Schmalz G, Shellis RP, Tveit AB, Wiegand A. Consensus report of the European Federation of Conservative Dentistry: erosive tooth wear – diagnosis and management. Clin Oral Investig. 2015 Sep;19(7):1557-61.
- Turner KA, Missirlian DM. Restoration of the extremely worn dentition. J Prosthet Dent. 1984 Oct;52(4):467-74.
- Muts EJ, van Pelt H, Edelhoff D, Krejci I, Cune M. Tooth wear: a systematic review of treatment options. J Prosthet Dent. 2014 Oct;112(4):752-9.
- McGarry TJ, Nimmo A, Skiba JF, Ahlstrom RH, Smith CR, Koumjian JH, Guichet GN; American College of Prosthodontics. Classification system for the completely dentate patient. J Prosthodont. 2004 Jun;13(2):73-82.
- Fayz F, Eslami A. Determination of occlusal vertical dimension: a literature review. J Prosthet Dent. 1988 Mar;59(3):321-3.
- Goodacre CJ. Designing tooth preparations for optimal success. Dent Clin North Am. 2004 Apr;48(2):v, 359-85.
- Wiskott HW, Belser UC. A rationale for a simplified occlusal design in restorative dentistry: historical review and clinical guidelines. J Prosthet Dent. 1995 Feb;73(2):169-83.
- Moreno-Hay I, Okeson JP. Does altering the occlusal vertical dimension produce temporomandibular disorders? A literature review. J Oral Rehabil. 2015 Nov;42(11):875-82.
- Murrell GA. Complete denture esthetics. Dent Clin North Am. 1989 Apr;33(2):145-55.
- Spear FM. Interdisciplinary Management of Worn Anterior Teeth. Facially Generated Treatment Planning. Dent Today. 2016 May;35(5):104-7.
About the Author
 Dr. Oliver Pin-Harry earned his DDS from L’Université de Montpellier, France and his MS & Certificate in Prosthodontics from the University of North Carolina at Chapel Hill, where he serves as Adjunct Assistant Professor. He is a Diplomate of the American Board of Prosthodontics, Fellow and Research Award recipient of the American College of Prosthodontists, a published author and international speaker on implants and esthetics. He maintains a full-time prosthodontics specialty practice in Burlington, Ontario.
Dr. Oliver Pin-Harry earned his DDS from L’Université de Montpellier, France and his MS & Certificate in Prosthodontics from the University of North Carolina at Chapel Hill, where he serves as Adjunct Assistant Professor. He is a Diplomate of the American Board of Prosthodontics, Fellow and Research Award recipient of the American College of Prosthodontists, a published author and international speaker on implants and esthetics. He maintains a full-time prosthodontics specialty practice in Burlington, Ontario.
RELATED ARTICLE: Letter to the Editor: The Severely Worn Dentition
Follow the Oral Health Group on Facebook, Instagram, Twitter and LinkedIn for the latest updates on news, clinical articles, practice management and more!












