Dental Caries as a Disease
Oral diseases have negative consequences on the overall health and well-being of individuals. Concurrently, they form one of the major public health challenges globally.1 The Global Burden of Disease Study (2016) found dental caries in permanent teeth to be the most prevalent condition among the estimated 328 diseases affecting half of the world’s population.2 Despite the efforts of recent decades, untreated dental caries has maintained its leading position over the past 30 years, decreasing only minimally since the 1990s.3 Prevention of dental caries is simple and effective, but treatment is costly. Approximately 5% of total health expenditure and 20% of out-of-pocket health expenditure is for dental care in high-income countries; in low- and middle-income countries, dental care is beyond most of the population and health care systems and governments cannot address oral health care demands.4 Given the above, the choice of restoration manufacturing materials and techniques is very relevant to achieving positive long-term outcomes.
In recent decades, composite resin has replaced amalgam as the primary direct filling material in most developed countries.5,6 This shift has been accelerated by EU Regulation 2017/852: “use of amalgam should be phased down in accordance with the Convention and with national plans”.7 This transition is not without its problems, however. Large, high occlusal load restorations in posterior teeth are most challenging.8 Manual direct restorative methods require great care and diligence, making these procedures, time-consuming. Composite resin restorations, on the other hand, all too often require repetitive repair or replacement (every few years) due to fractures, wear, and secondary caries linked to volumetric shrinkage of the material during polymerization.9-12 Repetitive repair and replacement of old restorations make up a large part of adult oral health care treatment.9 Current composite materials have fewer side effects than their predecessors, but all consequences and risks of these materials are not completely understood.13,14 They may also enter marine and lake environments via dental waste.15
Fig. 1
Fig. 2

The Rayo 3DToothFill Concept
Computer-aided design and computer-aided manufacturing (CAD/CAM) have entered the profession alongside digitalization.16 Milling technology is well accepted for manufacturing high-quality chairside restorations. On the other hand, 3D printing technology is developing rapidly and provides a promising, and far less expensive alternative. Printing’s very high accuracy makes it suitable for dental manufacturing;16-20 in digital dentistry, 3D printing technology is expected to grow swiftly while milling technology is projected to decline in the coming years.21 3D printing technology is currently used in laboratories to manufacture models, drilling and cutting guides, duplicate crowns, partial denture frameworks, dental implants, occlusal splints and orthodontic aligners, among others.
Rayo 3DToothFill is a novel technique for fabricating tooth fillings and other dental restorations chairside. The process combines automated 3D printing and robotics to manufacture dental restorations. Rayo 3DToothFill software (SW) directs and operates the manufacturing processes. The system is compatible with any oral scanner CAD SW with an open STL-format (stereolithography). The technology itself is easy to adopt and use and fits within the tight confines of a dental operatory.
Unlike solid ceramic or composite blocks used in milling technology, Rayo 3DToothFill enables layering of the restoration to simulate the internal structure of natural tooth with a somewhat flexible inner core and hard outer shell. This unique feature provides optimal elasticity for the restoration to enhance durability and to promote aesthetics by providing a tooth-like translucency for the filling. Rayo 3DToothFill is designed to use the existing medically approved filling materials. In the current Phase 1, only polymer resin composites are included. Compatibility of the3DToothFill method with ceramics and metal alloys will be evaluated in the next development phase.
Fig. 3

Fig. 4
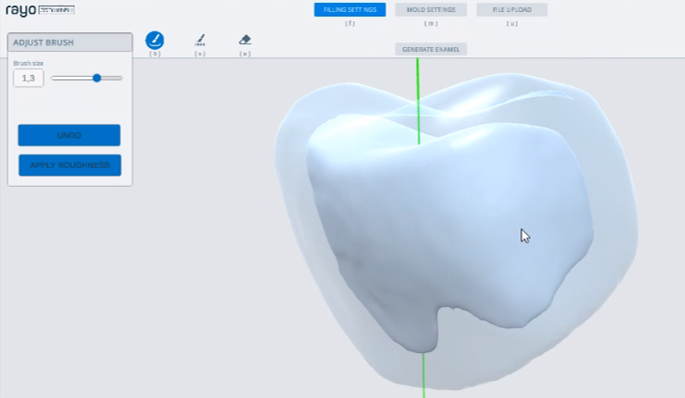
Rayo 3DToothFill Clinical Use
After preparation, the oral scanner images the cavity dimensions, the adjacent and opposing dentition, and the buccal occlusion. The dentist, utilizing the scanner’s CAD SW, designs the 3D restoration based on the tooth and cavity anatomies and the adjacent and opposing teeth. On completion, the design is imported from the scanner SW into the Rayo 3DToothFill SW to manufacture both the mould and the restoration. The process starts by printing the mould, which is then transferred to the Rayo robot which manufactures the restoration by casting filling material layers in the mould. The automated filling and curing procedures in the Rayo 3DToothFill robot are directed by Rayo 3DToothFill SW. After the manufacturing process is finished, the dentist cements the finished restoration into the cavity, completes polymerization, and verifies the occlusion. The restoration fits perfectly and is ready for functional use.
The digital imaging, 3D printing, and advanced software algorithms of Rayo 3DToothFill robotics enable a precision of a few tens of microns. Additionally, the process compensates for polymerization shrinkage. The excellent marginal and internal fit improve the restorative prognosis. A minimal marginal gap between tooth and restoration prevents plaque accumulation and cement dissolution, reducing the risk of secondary caries, endodontic inflammation, and periodontal disease.22 Benefits of 3D printing technology include higher restoration precision compared to subtractive manufacturing, where the accuracy is limited by the milling unit, machining tools, and low material loss.20,23 The Rayo 3DToothFill process is very efficient in its utilization of materials, energy, and water, leaving mininum residue or waste. Since the restorations are manufactured outside the mouth, the release of polymer particles in saliva and evacuation systems is minimal compared to conventional direct filling techniques. Further, it is possible to reuse or recycle even thermoset resin materials (moulds, cleaning residue). Hardened resin materials can be washed, ground, and re-used as is, or dissolved in solvents, and further processed by recycling for 3D printing or as components for composites.
For patients, the Rayo 3DToothFill solution provides quality care and durable restorations faster and more comfortably. The chairside fabrication process is convenient, minimizing dental visits with single appointment manufacturing of restorations. Mould printing takes 10-15 min and Rayo 3D robot filling manufacturing just a few minutes more. Furthermore, it is important to note that the 3D printer is capable of printing up to 10 moulds simultaneously, greatly increasing clinical efficiency. For dental professionals and health care organizations, the Rayo 3DToothFill solution increases productivity, reduces workload, and produces predictable, quality restorations. These benefits are amplified with increasing extent and complexity of treatment (large occlusal rehabilitation and/or under general anesthetics).
This innovation began as a collaborative research project between Finnish universities and researchers. Both dental and biomaterial science experts were involved. At present, Rayo 3DToothFill robot and software prototypes are completed and the in vivo study was started early in 2020 in Finland. One hundred adult patients requiring pairwise Class II, III or IV restorations are enrolled. Short fiber-reinforced composite24 material replaces the dentin layer and a flowable composite from the same manufacturer replaces the enamel. The two fillings in each patient are manufactured simultaneously; one is placed conventionally, directly into the cavity, and the other one utilizes the Rayo 3DToothFill method. The same dentist performs both the fillings for each patient. The restorations will be followed up for five years, reporting clinical evaluation results after six months, one year, two years and five years.
The first commercial versions of Rayo 3DToothFill robot and SW will be available in late 2020. Dentist end-user costs for Rayo 3DToothFill technology has not yet been determined but should be very competitive with milling technologies.
Oral Health welcomes this original article.
Corresponding author: Pirkko-Liisa Tarvonen Specialist in Dental Public Health, Dental Marketing Director. Rayo 3D-Toothfill Ltd., Kassivikintie 99-34 01180 Kalkkiranta, Finland. Email. pirkko-liisa.tarvonen@rayo3d.fi www.rayo3d.fi
References
- Dörfer C, Benz C, Aida J, Campard G. The relationship of oral health with general health and NCDd: a brief review. Int Dent J 2017; 67 Suppl2: 14-18.
- GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 2017; 390(10100): 1211-1259.
- Peres MA, Macpherson LMD, Weyant RJ, Daly B, Venturelli R, Mathur MR, Listl S, Celeste RK,
- Guarnizo-Herreño CC, Kearns C, Benzian H, Allison P, Watt RG. Oral diseases: a global public health challenge. Lancet 2019; 394(10194): 249-260.
- WHO Oral Health. Available at: https://www.who.int/news-room/fact-sheets/detail/oral-health
- Lynch CD, Opdam NJ, Hickel R, Brunton PA, Gurgan S, Kakaboura A, Shearer AC, Vanherle G, Wilson NH; Academy of Operative Dentistry European Section. Guidance on posterior resin composites: Academy of Operative Dentistry–European Section. J Dent. 2014; 42(4): 377-383.
- Opdam NJ, van de Sande FH, Bronkhorst E, Cenci MS, Bottenberg P, Pallesen U, Gaengler P, Lindberg A, Huysmans MC, van Dijken JW. Longevity of posterior composite restorations: a systematic review and meta-analysis. J Dent Res. 2014; 93(10): 943-949.
- EUR-Lex. Regulation (EU) 2017/852 of the European Parliament and of the Council of 17 May 2017 on mercury, and repealing Regulation (EC) No 1102/2008. Available at: https://eur-lex.europa.eu/eli/reg/2017/852/oj.
- Ahlholm P, Lappalainen R, Lappalainen J, Tarvonen PL, Sipilä K. Challenges of the Direct Filling Technique, Adoption of CAD/CAM Techniques, and Attitudes Toward 3D Printing for Restorative Treatments Among Finnish Dentists. Int J Prosthodont. 2019; 32(5): 402-410.
- Nihtilä A. Adult heavy and low users of dental services: treatment provided. Swed Dent J. 2016; 40(1): 21-32.
- Moraschini V, Fai CK, Alto RM, Dos Santos GO. Amalgam and resin composite longevity of posterior restorations: A systematic review and meta-analysis. J Dent. 2015; 43(9): 1043-1050.
- Ilie N, Hickel R. Resin composite restorative materials. Austr Dent J 2011; 56 (1 Suppl): 59–66.
- Garoushi S, Gargoum A, Vallittu PK, Lassila L. Short fiber-reinforced composite restorations: A review of the current literature. J Investig Clin Dent. 2018; 9(3): e12330.
- Gupta SK, Saxena P, Pant VA, Pant AB. Release and toxicity of dental resin composite. Toxicol Int. 2012; 19(3): 225-34.
- Cokic SM, Duca RC, Godderis L, Hoet PH, Seo JW, Van Meerbeek B, Van Landuyt KL. Release of monomers from composite dust. J Dent. 2017; 60: 56-62.
- Andrady AL. Microplastics in the marine environment. Mar Pollut Bull. 2011; 62(8): 1596-1605.
- Beuer F, Schweiger J, Edelhoff D. Digital dentistry: an overview of recent developments for CAD/CAM generated restorations. Br Dent J 2008; 204(9): 505-511.
- Dawood A, Marti Marti B, Sauret-Jackson V, Darwood A. 3D printing in dentistry. Br. Dent J 2015; 219: 521-529.
- Barazanchi A, Li KC, Al-Amleh B, Lyons K, Waddell JN. Additive Technology: Update on Current Materials and Applications in Dentistry. J Prosthodont. 2017; 26(2): 156-163.
- Mai HN, Lee KB, Lee DH. Fit of interim crowns fabricated using photopolymer-jetting 3D printing. J Prosthet Dent. 2017; 118(2): 208-215.
- Ahlholm P, Sipilä K, Vallittu P, Kotiranta U, Lappalainen R. Accuracy of inlay and onlay restorations based on 3D printing or milling technique – a pilot study. Eur J Prosthodont Restor Dent. 2019; 27(2): 56-64.
- Dental 3D Printing Market. Global Forecast to 2023. Markets and Markets. Available at: www.marketsandmarkets.com.
- Seo D, Yi Y, Roh B. The effect of preparation designs on the marginal and internal gaps in Cerec3 partial ceramic crowns. J Dent. 2009; 37: 374-382.
- Ebert J, Ozkol E, Zeichner A, Uibel K, Weiss O, Koops U, et al. Direct inkjet printing of dental prostheses made of zirconia. J Dent Res 2009; 88: 673-676.
- Garoushi S, Gargoum A, Vallittu PK, Lassila L. Short fiber-reinforced composite restorations: A review of the current literature. J Investig Clin Dent. 2018; 9(3): e12330.
About the Author
 Pirkko-Liisa Tarvonen DDS, PhD, University Lecturer, Department of Oral and Maxillofacial Diseases, Faculty of Medicine, University of Helsinki, Helsinki, Finland, Institute of Dentistry, University of Eastern Finland, Kuopio, Finland, Dental Marketing Director, Rayo 3D-Toothfill Ltd.
Pirkko-Liisa Tarvonen DDS, PhD, University Lecturer, Department of Oral and Maxillofacial Diseases, Faculty of Medicine, University of Helsinki, Helsinki, Finland, Institute of Dentistry, University of Eastern Finland, Kuopio, Finland, Dental Marketing Director, Rayo 3D-Toothfill Ltd.
 Kirsi Sipilä DDS, PhD, Professor, Research Unit of Oral Health Sciences, Faculty of Medicine, University of Oulu, Oulu, Finland, Oral and Maxillofacial Department, Medical Research Center Oulu, Oulu University, Hospital, Oulu, Finland, Research Director, Rayo 3D-Toothfill Ltd.
Kirsi Sipilä DDS, PhD, Professor, Research Unit of Oral Health Sciences, Faculty of Medicine, University of Oulu, Oulu, Finland, Oral and Maxillofacial Department, Medical Research Center Oulu, Oulu University, Hospital, Oulu, Finland, Research Director, Rayo 3D-Toothfill Ltd.
 Kenneth Tarvonen M.Sc. (Econ.), CEO, Rayo 3D-Toothfill Ltd.
Kenneth Tarvonen M.Sc. (Econ.), CEO, Rayo 3D-Toothfill Ltd.
 Reijo Lappalainen Professor, Biomaterials technology, Dept. of Applied Physics & SIB Labs, University of Eastern Finland, Kuopio, Finland, CTO, Rayo 3D-Toothfill Ltd. Rayo 3D-Toothfill Ltd. brings modern technology and techniques to chairside restorative care. This innovation aims to provide quality care for large patient groups around the globe.
Reijo Lappalainen Professor, Biomaterials technology, Dept. of Applied Physics & SIB Labs, University of Eastern Finland, Kuopio, Finland, CTO, Rayo 3D-Toothfill Ltd. Rayo 3D-Toothfill Ltd. brings modern technology and techniques to chairside restorative care. This innovation aims to provide quality care for large patient groups around the globe.












