The following article will illustrate a comprehensive full mouth reconstruction therapy with treatment objectives for Aesthetics and Biomechanics. Our patient (N.B.) presented to the office with the pre-existing dental treatment done from another country as illustrated in photos 1 and 2. After the initial consultation, our patient wished for fixed implants and prosthodontics to restore and replace her natural dentition. Comprehensive diagnostic records were gathered in order to formulate the treatment plan with options (Table #1). Based on the diagnostic records gathered, a list of diagnosis was made and summarized in Table #2. Case presentation was conducted reviewing several treatment options with risks, benefits and alternatives of each treatment plan. Full mouth diagnostic wax set up was completed with alterations from pre-existing mounted models. Alterations for aesthetics, tooth proportions, gingival displays, vertical dimension of occlusion, shade and biomechanical support confirmed. Pre-surgical implant provisionals fabricated accordingly in preparation for immediate implant provisionalization at time of implant placement. Phase 1 treatment involved full maxillary arch extractions of compromised dentition with immediate molar implant placement in upper molar 16 site, five additional anterior implants and lateral window sinus grafting to upper left posterior region. After confirmation of initial primary stability of all six maxillary anterior implants with an Osstell Implant Stability Quotient of greater than 60, immediate screw retained provisionals was inserted with soft diet instructions. Phase 2 of treatment included extraction of the lower right premolar with immediate implant placement into the 45 site and implant placement at the 47 site. The lower anterior 31 and 41 were extracted with single implant placement. The lower left pre-existing implant was integrated with the previous bridge sectioned and implants placed in 36 and 37 positions. Phase 3 involved staged additional two implant placements to upper left posterior quadrant after sinus graft maturation of six months.

Phase 4 was initiated after implant healing. A final open tray impression was taken using heavy and light-bodied polyvinylsiloxane capturing both implants and tooth preparations. Impression posts were splinted with old burs and flowable composite prior to impression making. The patient’s maxillary immediate load prosthesis was replaced with acrylic screw-retained provisionals that were adjusted and contoured chair side. These provisionals were used to evaluate esthetic, phonetics, and function. Soft tissue training was also done at this stage. Full-face photographs, in addition to video of the patient during speech, revealed that the incisal length were initially too long. After adjustments were made to meet the esthetic demand of the patient, alginate impressions were taken of the both maxillary and mandibular provisionals. A digital scan using 3Shape was done and a maxillary set of milled PMMA provisionals were fabricated. This was delivered to the patient to further improve esthetics and occlusion. After several weeks with these new provisionals, all functional and esthetics issues were addressed. A new set of intraoral and extraoral photographs were taken and sent to the ceramist. A PVS impression was taken of the milled PMMA provisionals and the cast was mounted on a semi-adjustable articulator using a facebow transfer. The PMMA provisionals were also used to cross mount the master casts onto the same articulator. A digital scan of the milled PMMA prosthesis was performed using the 3Shape scanner. This ensured that minimal adjustments were needed for the final prosthesis since the occlusal surfaces of the maxillary prosthesis was milled in zirconia. On the maxilla, the final restoration was a 13-unit implant screw-retained porcelain fused to zirconia prosthesis from 16-27. Porcelain was placed only onto the buccal surface with fewer cutbacks in the posterior regions. On the mandibular arch, a ceramometal screw-retained implant fixed partial denture was fabricated from 37-36. The existing implant between the 37 and 36 was retained and supported the distal half of the 36 using a cement-retained design. 31-41 and 45-46 were also restored with ceramometal screw-retained implant fixed partial dentures. 35, 34, 44 were restored with eMax single crowns and eMax veneers were placed on 33, 32, 42, 43. Screw access holes were filled with teflon tape and composite. A nightguard was fabricated for the patient to minimize risk of porcelain chipping and fracture. Frequent recalls and maintenance for this patient was crucial to prevent the recurrence of caries, periodontal disease and prosthetic complications.
Oral Health welcomes this original article.
Fig. 1
Full face photo of the patient of initial presentation.

Fig. 2
Initial panaoramic radiograph.

Fig. 3
Full face photo of the patient with acrylic provisionals.

Fig. 4
Smile photo of acrylic provisionals after shortening incisal length.

Fig. 5
Full face photo of acrylic provisionals after shortening incisal length.

Fig. 6
Smile photo of milled PMMA provisionals.

Fig. 7
Full face photo of milled PMMA provisionals.

Fig. 8
Occlusal view of 3Shape virtual planning.

Fig. 9
Frontal view of 3Shape virtual planning showing implant location.

Fig. 10
Frontal view of 3Shape virtual planning.

Fig. 11
Zirconia frame.

Fig. 12
Zirconia frame with first layer of porcelain.

Fig. 13
Maxillary prosthesis after first bake.

Fig. 14
Lateral view of final maxillary prosthesis.

Fig. 15
Frontal view of final maxillary prosthesis.

Fig. 16
Frontal view of maxillary and mandibular restorations (except mandibular veneers).

Fig. 17
Lateral view of maxillary and mandibular restorations.

Fig. 18
Frontal view of final restorations at delivery in maximum intercuspation.
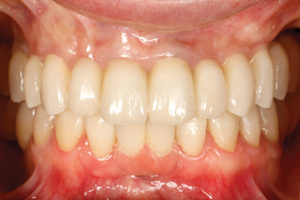
Fig. 19
Right view of final restorations.

Fig. 20
Left view of final restorations.

Fig. 21
Smile photo of patient with final restorations.

Fig. 22
Panoramic radiograph at final delivery.

Fig. 23
Final full face photo of patient.

Fig. 24
Final full face photo of patient.

About the Authors
Dr. Goth Siu completed his Doctor of Dental Medicine degree at the University of Pennsylvania in Philadelphia. He then completed a specialty residency program in Prosthodontics at the University of Illinois at Chicago. Dr. Siu is board certified in Prosthodontics in Canada and the US. He is practicing at Dr. Mark Lin Prosthodontic Centre, Markham Dental Group and Profiles Dental Specialists.
Dr. Mark H. E. Lin graduated from the University of Detroit Mercy for his dental program. He then completed a one-year General Practice Residency program at the Miami Valley Hospital in Dayton, Ohio. He practiced general dentistry for 13 years and then returned to complete his post-graduate training in the specialty of prosthodontics at the University of Toronto. He maintains a full-time private specialty practice as a prosthodontist at Dr. Mark Lin Prosthodontic Centre.












