Is This Vision Important for Dentistry?
Introduction
Breastfeeding has an important role in the development of the orofacial structures in babies. For this reason, we need to review our knowledge and the importance of the mouth in the success of breastfeeding and in the growth of the infants and, on the other hand, the role of laser systems in a minimally invasive management of oral disorders and pathologies.
In the first world countries of the 20th century, we observed a significant decrease in breastfeeding, which contributed to an increase in orofacial imbalances. Fortunately, from the end of the 20th century and continuing now, we are experiencing the resurgence of breastfeeding. In many cases, breastfeeding problems for mothers and babies are attributed to abnormal attachments of the tongue or the upper lip (such as tongue tie and lip-ties). Other problems like epulis, tumors, angiomas or natal teeth can be considered to be primary factors in creating breastfeeding difficulties, they alter the correct function of the mouth of the baby.
This means that pediatricians and breastfeeding experts, together with expert dentists in neonatology, must create multidisciplinary teams to study cases in which the mouth becomes an impediment to the proper development of breastfeeding.
We must carefully study each case and check for a restrictive pattern that is the cause of the difficulty in breastfeeding, as this is vital for the integral development of the newborn.
There is a strong belief or axiom that we must wait until the child has grown to perform a frenectomy, but sometimes when we do not do it, it may affect the future growth process itself and limit the infant’s own development.
Fig. 1

Disturbances caused by not being breastfed
We have to take into account that oral health is an important part of the breastfeeding experience 1,2,3,4,5,6,7 and breastfeeding is not only a lifestyle choice, but rather a basic health need. When we do not have proper type of nutrition, we can observe some problems in the development of babies. We associate the following problems with babies who were not breastfed: dental malocclusions, high palates, narrow dental arches, anterior & posterior dental crossbites, inadequate nasal respiration, alterations in the deglutition and in the management of the tongue, inadequate facial development, incorrect mastication pattern, parafunctions, thumb sucking or problems in the emotional sphere. 4,5,8 Newborns often present with ankyloglossia (tongue tie) or lip-tie which cause problems in breastfeeding. Ankyloglossia is associated with 25-60% of the incidence of difficulties during breastfeeding for mothers and babies. 9,10
Fig. 2

The importance of breastfeeding. The nipples as expanders of the palate.
Alterations in oral structures allow us to understand the importance of the breastfeeding experience, because the “Nipples are considered like Mother Nature’s palate-expanders”. As babies push the nipple behind the front teeth and push on the palate, they develop a wide and forward palate and enough room for the permanent teeth. On the other hand, peristaltic movements (in bottle feeding, piston movements) 11 produce the first physiological advance of the mandible, connecting the jaw, hyoid bone and cervical spine in a harmonic three-dimensional position.
The benefits of breastfeeding in the development of orofacial structures, allow infants to naturally breathe and swallow at the same time without learning a complicated protective mechanism.
Breastfeeding benefits to infants:
- it improves the infant’s immune system
- prevention of allergies
- no preservatives as it is always fresh
- emotional attachment to the mother
- it protects against gastroenteritis, constipation and other stomach illnesses
- it reduces the risk of SIDS (sudden infant death syndrome)
- promotes proper facial development
- reduces the risk of heart disease or obesity as teenagers and adults
- babies who are breastfed have fewer indicators of malocclusion problems, oral breathing or poor orofacial development. 8
In the future, adults with ankyloglossia will have more problems with snoring and nocturnal apneas, because the tongue goes backwards during sleep, closing more airway space.
Symptoms in babies
We can observe:
- Restricted tongue movement where the baby may be unable to poke his tongue out or lick his lips, and during crying the tongue may remain in the floor of the mouth or just the edges may curl up forming a ‘dish’ or a whale tail shape.
- Poor wave motion
- It is possible that baby is unable to open the mouths widely when attaching to the breast, resulting in a biting/grinding behavior and a tight labial frenulum which does not allow flanging of the lips
- Unsettled/fussy behavior when latching to the breast and during feeds
- Coughing on the milk flow
- Difficulty staying attached to the breast. The nipple slides off
- No latch or un-sustained latch
- Falling asleep at the breast before the end of feeding
- Frequent or very long feeds
- Excessive early weight loss/poor weight gain/faltering growth. Excessive weight loss in the first few days of life, or slow weight gain later on, despite constant feeding
- Clicking noises and/or dribbling during feeds
- Failure to thrive
- Colic, wind, hiccups
- Reflux (aerophagia)
- Gumming or chewing the nipple
- Unable to hold pacifier
There are many other symptoms and signs in the neonatal period and during childhood.
Diagnosis of frenulum disorders
For the diagnosis of frenulum and oral disorders in babies, we need to study the clinical history of baby and mother, type of delivery, maturity…etc. and a clinical exploration of all the structures of the child and mother which are involved in Breastfeeding. For example, checking the condition of the baby’s mouth by assessing: tongue, gums, jaws, lips, epiglottis and soft/hard palate. It is also important to take a look at the oral-nasal respiratory circuit and pattern.
We need the important information provided by the pediatrician about the baby. In addition, we need to carefully examine oral frenula, breathing and the neurological reflexes correlated with breastfeeding and with the maturity of babies. A child with neurological immaturity cannot perform adequate suction, even if we control his frenulum. 6
Fig. 3
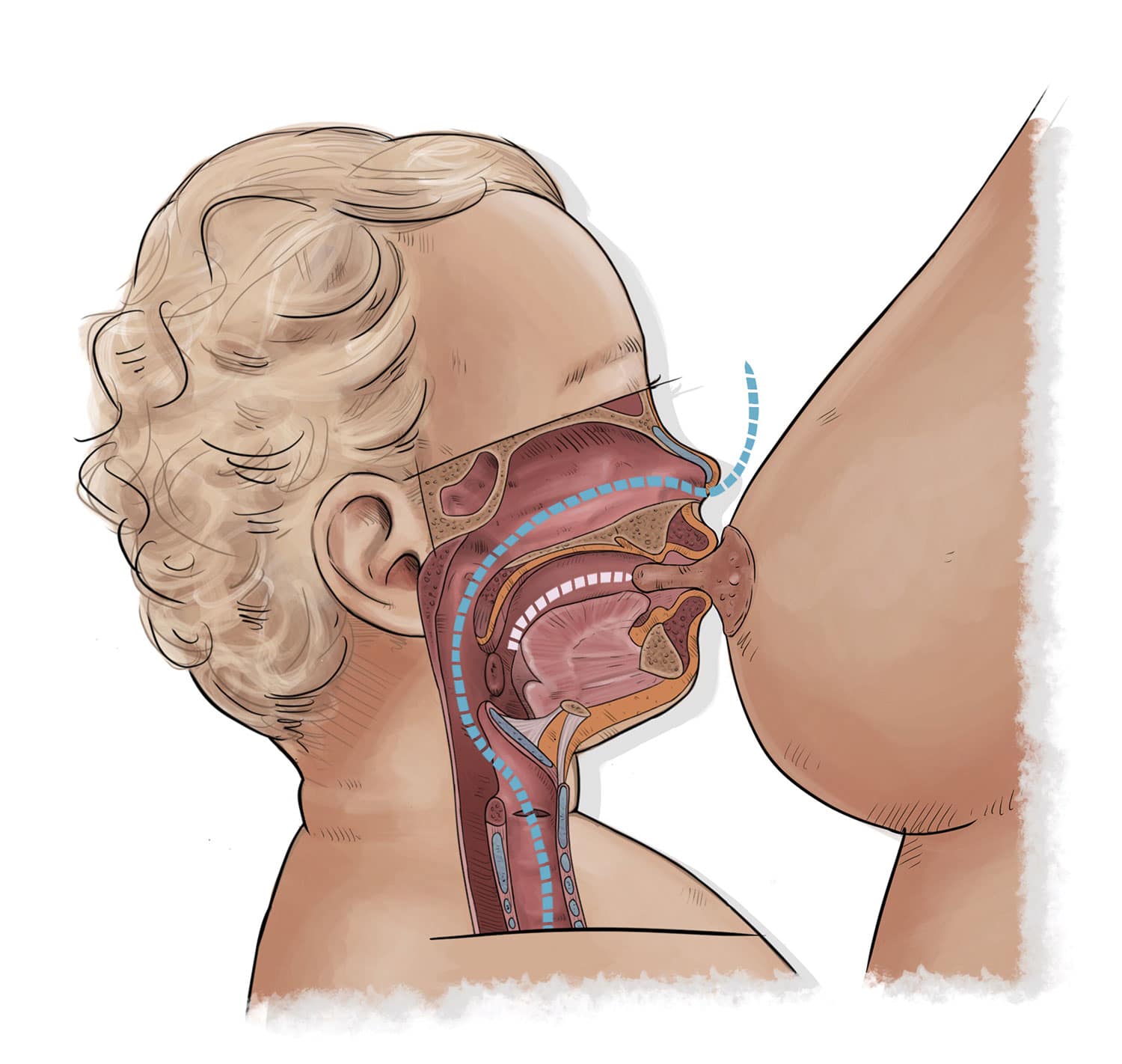
How to determine if your newborn infant is tongue-tied
Ankyloglossia or lip tie can be defined in different ways:
- Anatomic & clinical appearance.
- Restrictive movements and functional ability.
- Infant and mother symptoms: loss of weight, inability to breastfeed properly, pain in the nipple, mastitis… etc.
There is no universally agreed upon way to classify tongue or lip-ties, therefore, there are different frenula classifications. However, in our experience, we believe it is more appropriate to simplify everything and classify the presence of ankyloglossia in:
1. Normal:
- Normal appearance.
- Insertion of the frenulum well below the tip of the tongue and closer to the base than to the tip (approximately 1 cm) and inserted into the floor of the mouth close to the insertion of the genioglossus muscle.
- Correct mobility both to the front and in lateral movements.
- No symptoms of restriction.
2. Mild restriction:
- Normal appearance.
- Insertion of the frenulum under the tip of the tongue and towards the floor of the mouth, being able to have a “trident” that anchors it in the lingual part of the alveolar ridge.
- No important symptoms of restriction.
- The length of mobile tongue is 12-16 mm.
- The Restriction is between 0.22 – 0.39 with good mobility of the tongue.
3. Moderate restriction:
- The appearance of the tongue presents slight retraction of the tip or tendency to have a shape of the tail of a whale, and to position itself down when resting.
- The insertion of the frenulum is very close to the tip of the tongue and towards the floor of the mouth with a strong trident towards the alveolar ridge or in the alveolar ridge.
- Limited mobility both to the front and in lateral movements.
- When we provoke the suction introducing the finger in the mouth of the baby, we appreciate that the tongue has difficulties to surround and suck the finger, sometimes with a complete loss on the back of the finger, where there is a reverse movement (peristalsis), like a wave that is sailing backwards.
- Reversion of the sound or clicking occurs when the tongue loses contact with the finger and, therefore, loses the negative pressure.
- It is not very elastic.
- With symptoms of restriction.
- Length of mobile tongue 8-11 mm.
- The Restriction is between 0.14- 0.22 with limited mobility of the tongue.
4. Severe restriction:
- The appearance of the tongue presents strong retraction of the tip with complete hold of the tongue to the floor of the mouth or to the alveolar ridge.
- Heart-shaped, with the central part of the tongue very depressed, with tendency to place itself down in normal position.
- The insertion of the frenulum is at the tip of the tongue.
- Very limited mobility both to the front and in lateral movements.
- The tip of the tongue cannot ascend without closing the mouth and with a broad (heart-like) shape, with an important depression in the center of the tongue.
- The frenulum has less than 1 cm when the tongue is extended.
- There are signs of ischemia in the insertion of the tongue when we pull from it.
- It cannot be positioned on the lower lip.
- When we provoke the suction introducing the finger in the mouth of the baby, we appreciate that the tongue has serious difficulties to surround and suck the finger.
- It is very often seen the reversion of the sound or clicking that occurs when the tongue loses contact with the finger and, therefore, loses the negative pressure.
- It is relatively inelastic.
- With severe symptoms of restriction.
- Length of mobile tongue is smaller than 3 mm.
- The Restriction is close to and below 0.14 with very limited mobility of the tongue.
Fig. 4


Treatment options for lip and tongue-ties
- Myofunctional treatment.
- Frenotomy, Frenectomy or Z-plasty:
- With conventional surgery, these procedures are usually more aggressive and more uncomfortable after surgery. There is more bleeding and need for sutures. There is high incidence of recurrence/relapse.
- With laser systems, the treatment is minimally invasive, little to no bleeding, no sutures, quick recovery, low to no recurrence of the problem.
Frenotomy and Frenectomy Techniques with laser systems
- The child is swaddled with a blanket to control movements.
- Good control of patient’s airway.
- Safety glasses with elastic strap according to Laser Safety Standards: ANSI 136.1(USA) and EN207/EN208/EC60825 (Europe).
- Assistant holds and stabilizes head.
- Stabilize and elevate tongue.
- No anesthetics.
- Clip centre of frenum (~1 cm). Frenum is poorly vascularized and is poorly innervated
- Infant can breastfeed immediately.
- Completed in dental chair in 2-3 minutes.
It is very important for the infant’s safety and for a good visualization of the surgical area to have a well-trained staff to properly hold the infant and assist in maintaining a good airway. It is imperative to locate the mamelons where the holes of the outflow of the Wharton ducts are located, as they are excretors of the submaxillary salivary glands. We can use the fingers or the Lorenz tongue holder or groove director (Tongue lifter) to help position the tongue.
Differents laser systems, like the diodes or erbium lasers, can be used to perform this surgical procedure, as reported by several authors in recent publications on this subject. 12,13,14,15,16,17
In my opinion, Erbium laser is more comfortable for the babies. We don’t need anesthetic or sutures, we don’t have bleeding, we have precise control over the important surrounding structures, like the glands, and there is no recurrence.
- Diode Laser 940 nm: pre-initiated tip is used in direct contact with tissue at a power of 2.0W CW using a 400 µm fiber.
- Er,Cr:YSGG, 2780 nm: 2-3 Watts, 50 Hz, H/S Mode, 20% air, 20% water, tip MZ5 or MC3. Around 50-70 mJ/cm2 of fluence.
In most cases, 2-8 mm of freedom is adequate to allow an improved and comfortable nursing.
Fig. 5
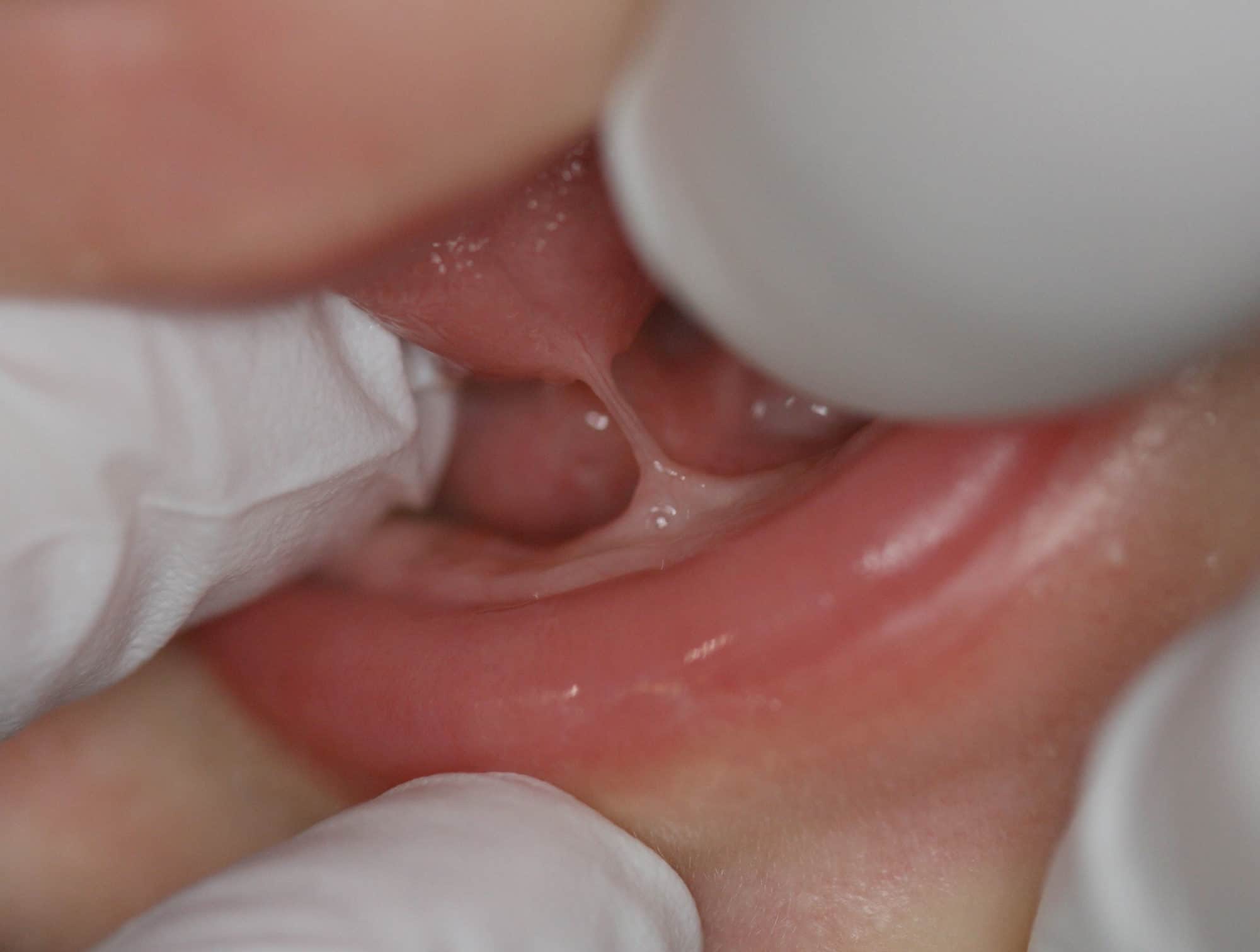



Post-operative care instructions
- 1 month after surgery, control by a myofunctional therapist expert in neonatology.
- Pull in the morning and at night. 2-3 times per day for 2 weeks.
- Rinsing the mouth with warm salt water.
- Hyaluronic gel.
- Auxin A+E, oil pearls.
- Cranial-Sacral therapy.
- Pediatric ibuprofen, if the baby has some discomfort.
Our mouths are very important for our lives! Dentists are in the unique position to help our youngest patients to start their lives on the right foot (or with the right mouth). Are we as a profession ready for this challenge?
A note from the editor
Performing baby frenectomies to help release tongue tie and lip tie is a very important service we can provide to young mothers and to give babies the right start in life. Many other laser systems, including Fotona or LiteTouch Er:YAG 2940nm, LightScalpel 10,600nm CO2, Solea 9300nm CO2, 1064nm Nd:YAG, 810nm diode Picasso, 980nm diode Zolar, Sirolase and Gemini, can safely and effectively perform this procedure. It is important to be properly trained by a certified and manufacturer approved trainer, as the machine settings and laser parameters vary among different laser systems and the parameters listed in this article cannot be applied to other laser systems. OH
Oral Health welcomes this original article.
References
- Palmer B. The Influence of Breastfeeding on the Development of the Oral Cavity: A Commentary. J Hum Lact. 1998;14: 93-98.
- Palmer B. For Better Health!!. Breastfeeding and frenulum presentation. En ponencia presentada en DDS Kansas City, Missouri. USA; 2003.
- Martín Santiago MP. Lactancia materna y desarrollo oclusopostural bajo una visión kinesiologica – Allattamento materno e sviluppo occlusoposturale da un punto di vista kinesiologico. En: ponencia presentada en Reunión Nacional de la SIKMO (Sociedad Italiana de Kinesiología Médica Odontológica). Nápoles. Italia; 2005.
- Kotlow LA. The influence of the maxillary frenum on the development and pattern of dental caries on anterior teeth in breastfeeding infants: prevention, diagnosis, and treatment. J Hum Lact. 2010 Aug; 26(3):304-8. doi: 10.1177/0890334410362520. Epub 2010 Mar 22. PubMed PMID: 20308621.
- Kotlow LA. The influence of the maxillary frenum on the development and pattern of dental caries on anterior teeth in breastfeeding infants: prevention, diagnosis, and treatment. Eur J Paediatr Dent. 2015 Dec;16(4):262. PubMed PMID: 26785517.
- Martín Santiago MP. Lactancia Materna y el papel de los láseres en la intervención de frenillos bucales en recién nacidos y niños. En: Charla dirigida a pediatras, matronas y especialistas en Lactancia materna. Santa Cruz de Tenerife. Departamento de Pediatría, Hospital Universitario de Canarias; 2016.
- Convissar R, Hazelbaker AK, Kaplan M, et al. Color Atlas of Infant Tongue-Tie and Lip-Tie Laser Frenectomy. Columbus, OH: PanSophia Press; 2017. ISBN: 978-0-9845445-3-0. Disponible en https://www.laserfrenectomybook.com/.
- Rondón R, Zambrano G, Guerra ME. Relación de la lactancia materna y el desarrollo Dento-Buco-Máxilo-Facial: Revisión de la literatura latinoamericana Revista Latinoamericana de Ortodoncia y Odontopediatría. 2012. Disponible en: https://www.ortodoncia.ws/publicaciones/2012/art-19/. Consultado el 06/03/2018.
- Walsh J, Tunkel D. Diagnosis and Treatment of Ankyloglossia in Newborns and Infants: A Review. JAMA Otolaryngol Head Neck Surg. 2017 Oct 1;143(10): 1032-1039. doi: 10.1001/jamaoto.2017.0948. Review. PubMed PMID: 28715533.
- Walsh J, Links A, Boss E, Tunkel D. Ankyloglossia and Lingual Frenotomy: National Trends in Inpatient Diagnosis and Management in the United States, 1997-2012. Otolaryngol Head Neck Surg. 2017 Apr;156(4): 735-740. doi: 10.1177/0194599817690135. Epub 2017 Feb 7. PubMed PMID: 28168891.
- Kotlow LA. Diagnosing and understanding the maxillary lip-tie (superior labial, the maxillary labial frenum) as it relates to breastfeeding. J Hum Lact. 2013 Nov;29(4):458-64. doi: 10.1177/0890334413491325. Epub 2013 Jul 2. PubMed PMID: 23821655.
- Kotlow L. Lasers and pediatric dental care. Gen Dent. 2008 Nov-Dec;56(7): 618-27. PubMed PMID: 19014020.
- Martín Santiago, MP. Estudio del Frenillo Labial Superior (FLS) y la cirugía láser con YSGG en la población metropolitana del norte de Tenerife. Master Europeo “Aplicaciones del Láser en Odontología” (European Master “Laser Applications in Dentistry”). Barcelona. EMDOLA. Facultad de Odontología. Universidad de Barcelona; 2010.
- Aras MH, Göregen M, Güngörmüş M, Akgül HM. Comparison of diode laser and Er:YAG lasers in the treatment of ankyloglossia. Photomed Laser Surg. 2010 Apr; 28(2):173-7. doi: 10.1089/pho.2009.2498. PubMed PMID: 19743963.
- Olivi G, Signore A, Olivi M, Genovese MD. Lingual frenectomy: functional evaluation and new therapeutical approach. Eur J Paediatr Dent. 2012 Jun;13(2): 101-6. PubMed PMID: 22762170.
- Lamba AK, Aggarwal K, Faraz F, Tandon S, Chawla K. Er, Cr:YSGG laser for the treatment of ankyloglossia. Indian J Dent. 2015 Jul-Sep;6(3):149-52. doi: 10.4103/0975-962X.163049. PubMed PMID: 26392733; PubMed Central PMCID: PMC4558751.
- Kumar G, Rehman F, Chaturvedy V. Soft Tissue Applications of Er,Cr:YSGG Laser in Pediatric Dentistry. Int J Clin Pediatr Dent. 2017 Apr-Jun;10(2):188-192. doi: 10.5005/jp-journals-10005-1432. Epub 2017 Jun 1. PubMed PMID: 28890621; PubMed Central PMCID: PMC5571390.
About the Author
 Dr. Pilar Martín graduated in 1987 from the Universities of La Laguna (Spain) and Universidad Odontológica Dominicana (Santo Domingo) with degrees in Medicine, Surgery and Dentistry. In 1996, Dr. Pilar completed her Post Graduate Course in Cosmetic Dentistry at the Baylor Collage of Dentistry in Texas. She has also been trained in the field of surgery with the Master in Implantology, Surgery, Periodontics and Prosthodontics in the University of Bern (Switzerland) in 2002.
Dr. Pilar Martín graduated in 1987 from the Universities of La Laguna (Spain) and Universidad Odontológica Dominicana (Santo Domingo) with degrees in Medicine, Surgery and Dentistry. In 1996, Dr. Pilar completed her Post Graduate Course in Cosmetic Dentistry at the Baylor Collage of Dentistry in Texas. She has also been trained in the field of surgery with the Master in Implantology, Surgery, Periodontics and Prosthodontics in the University of Bern (Switzerland) in 2002.
In 2010 she finished the European Master Degree in Oral Laser Applications in the University of Barcelona and EMDOLA. After that, she received her Master of Laser in Dermo-aesthetic Pathology in the University of Barcelona. She holds Master of Science degree in Laser Dentistry from RWHT University in Aachen, Germany, and is the Official Representative for AALZ (Aachen Dental Laser Center) in Latinamerica and Spain. Dr. Pilar is a member of WCLI (World Clinical Laser Institute) and recently, she has been named the Official Representative of WFLD (World Federation for Laser Dentistry) in Spain.












