Ten years ago, I took a weeklong survival class in the SE Utah high desert with my son. No food, water, tent, sleeping bag or phone, just you, your clothes, a knife and a compass. There were two guides and twelve of us. They trained us in the art and science of survival for the first few days then we were on our own and had to make our way back as a group and then as individuals. It was an awesome experience and full of lessons. They taught us you could go three weeks without food, three days without water, and three minutes without air. I did not realize at the time that they might have been developing a tagline for the American Academy of Physiologic Medicine in Dentistry (https://www.aapmd.org): Airway Trumps Everything.
Just as we have evolved in dentistry and medicine to this incredibly techno-savvy place with digital everything and pocket computer phones, so too has our perspective of medicine and dentistry and the complex interwoven architecture they share. Galen is most admired by modern medicine for being a brilliant anatomist who was way ahead of his time. Living so long ago, with so little previous knowledge to go on, it’s amazing what Galen figured out; in fact, he almost got it all right. Modern physiology has taught us form and function, cause and effect and disease management of the same “faculties” and “pneumas” that puzzled the ancient Greeks. Our own dental education has advanced as we discovered the bacterial etiology of decay, then periodontitis and on the neurophysiology of the stomatognathic system. These strides have indeed been remarkable yet there was a unification present all along that was so simple, it was easy to overlook. Just breathe! Without air for a few minutes, great restorations, TMD therapies and regenerative periodontal procedures lose their luster. Similarly, in medicine, my recent total knee replacement routine systemic treatments and the miracle of childbirth pale in importance to taking breath. Airway Trumps Everything!
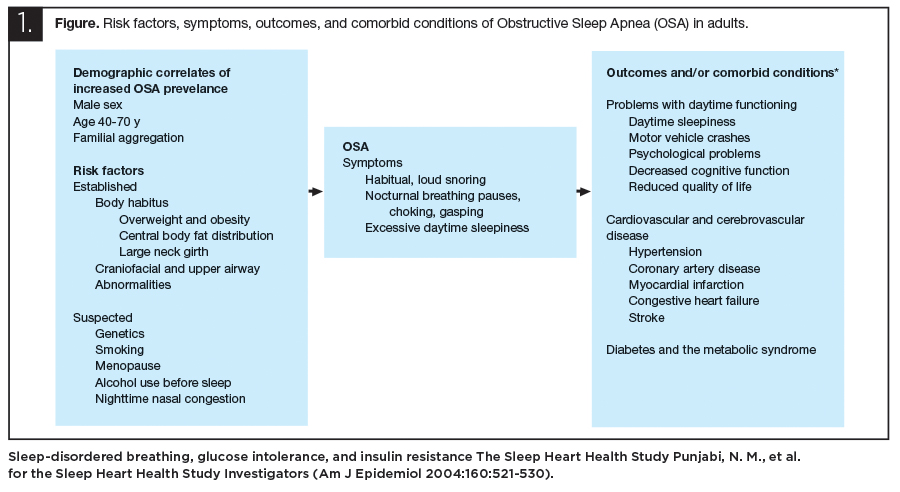
I know; it is so obvious that without breath we would die, but what about without good airways? What impact does compromise have? How do you measure good sleep and breathing? We are just recently coming to understand how important a contributor to health or disease states a patent functioning airway is, at night and while awake. The list of comorbidities caused by Upper Airway Resistance Syndrome and Obstructive Sleep Apnea is scary. In fact, sleep disturbances may be the most important consideration after genetics to the loss of health in medicine and dentistry today.
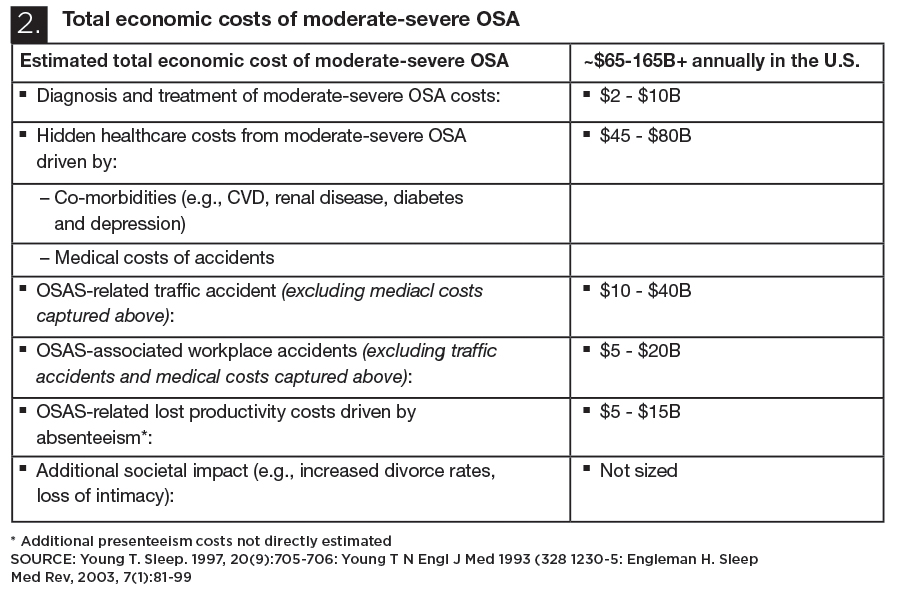
The cost to patients, their families and society is measurable and enormous. Harvard in 2010 published the Sleep Medicine study “The Price of Fatigue” for the medical school. The analysis below and the total cost data have only risen since this met analysis was completed.
- OSA attracts limited public attention (e.g., OSA related traffic accidents cost $35B versus well known public safety threats such as drunk driving ($60B) and not wearing seatbelts ($150B)
- Awareness, diagnosis, and treatment of OSA are limited by the economics and nature of the condition – OSA costs are highly fragmented and touch many disconnected stakeholders – Current technology, while effective at treating the disease, is cumbersome and uncomfortable for many – Low patient compliance limits the cost effectiveness of treatment for payors
- Opportunities to reduce the costs of sleep apnea include: – More holistic research to understand the current and projected costs of the disease (e.g. Prevalence, co-morbidities) – Building a cohesive community of stakeholders (e.g., physicians, patients, employers, public safety officials, etc.) to drive awareness – Improving the patient experience and comfort in treatment to drive adoption – Convincing payors and employers of the long-term economic benefits of screening and treatment.
So, what is the answer?
Dentistry is at the forefront of this story. Our frequent screening intervals allow us to take the point and drive treatment success. Oral appliance therapy (OAT) has been shown to be very successful in mild, moderate and even sever cases of OSA. Physicians and dentists have begun (they still have a way to go) working co-operatively. A recent New England Journal of Medicine articles discussed CPAP treatment’s lack of impact on cardiovascular prevention in OSA due to noncompliance. The American Academy of Sleep Medicine is now recommending OAT for patients who do not prefer CPAP or are noncompliant. Sadly, the state of undiagnosed OSA is still estimated at 85-90% of the disease and the noncompliance of CPAP still hovers around 60%. The improved compliance of OAT and very high success rates proves to make for better math that CPAP’s 40% utilization by patients of a 100% solution. Airway Trumps Everything!
The recent studies by the medical and dental community, advancements in European utilization of OAT and the slowly shifting winds of change are creating a tsunami of treatment needs and opportunities in dentistry. In the next few years we can help millions of patients breathe better, decrease their life threatening comorbidities and contribute to a safer work and life environment. It is NOT dentists practicing medicine. It is the dentist doing dentistry. Screening, referring and fulfilling prescriptions for oral appliances that fit into the mainstream of what we already do as clinicians. The shift to OAT continues to accelerate. Dentists and OAT manufacturers are going to need to scale up, and the good news is that dentistry is well positioned to do so. Dentists can easily add sleep screening to their dental exams. OAT manufacturers are already taking advantage of digital production technologies to enable significantly faster turnaround times and quality, without the problems of scalability that afflict traditional dental laboratories. We can make a difference. Airway Trumps Everything!
According to The Public Health Agency in Canada, one out of four Canadians had a high risk of OSA and almost one million have been diagnosed. Let’s do some math together. That leaves 7,750,000 undiagnosed and at risk. The Canadian Thoracic Society states that individuals with sleep apnea had other chronic conditions and were:
- 2.5 times more likely to report having diabetes;
- 1.8 times more likely to report hypertension;
- 2.2 times more likely to report heart disease; and,
- 2.2 times more likely to report a mood disorder such as depression, bipolar disorder, mania or dysthymia.
Airway Trumps Everything!
The non-profit AAMPD has advanced this co-operative effort among all health care providers and professional. Regardless of orientation towards treatment constructs, methodologies or dogmas, the need to keep the airway patent takes precedence over other design inputs. In dentistry, centric relation, neuromuscular, gnathological or OBI approaches to occlusion take a back seat to the three minutes we have to breath. At their seminal White Flag event in Tucson AZ last year, Howie Hindin and Michael Gelb brought health care professional together from across all components of medicine, dentistry and the allied health care realm. The all dismissed their differences and united behind this unifying theory of health care, they took a pledge to put airway first. The Mission of the American Academy of Physiologic Medicine in Dentistry’s Foundation for Airway Health is to help the public realize their maximum potential by championing the recognition, diagnosis and treatment of airway related disorders through collaboration, awareness, research, education and access to care. Join them, join dentistry’s role in helping improve the health and life of Canadians, because Airway Trumps Everything. OH
Oral Health welcomes this original article.
About the Author
 Mark Murphy is Lead Faculty for Clinical Education at ProSomnus Sleep Technologies, the Principal of FunktionalTracker.com, serves on the Guest Faculty at the University of Detroit Mercy School of Dentistry and is a Regular Presenter on Business Development, Practice Management and Leadership at the Pankey Institute. He has served on the Boards of Directors of the Pankey Institute, National Association of Dental Laboratories, the Identalloy Council, the Foundation for Dental Laboratory Technology, St. Vincent DePaul’s Dental Center and the Dental Advisor. He lectures internationally on Leadership, Practice Management, Communication, Case Acceptance, Planning, Occlusion, Sleep and TMD.
Mark Murphy is Lead Faculty for Clinical Education at ProSomnus Sleep Technologies, the Principal of FunktionalTracker.com, serves on the Guest Faculty at the University of Detroit Mercy School of Dentistry and is a Regular Presenter on Business Development, Practice Management and Leadership at the Pankey Institute. He has served on the Boards of Directors of the Pankey Institute, National Association of Dental Laboratories, the Identalloy Council, the Foundation for Dental Laboratory Technology, St. Vincent DePaul’s Dental Center and the Dental Advisor. He lectures internationally on Leadership, Practice Management, Communication, Case Acceptance, Planning, Occlusion, Sleep and TMD.
RELATED ARTICLE: Organized Dentistry Takes a Turn Toward the Airway












