Introduction
The single most controversial topic in dentistry is temporomandibular disorders (TMD). Because of the associated controversy and confusion most dentists are not prepared to deal with these patients when they appear in their practice. Proper diagnosis is the key. The goal of this article is to prepare you simply and succinctly to make straightforward evidenced based decisions when confronted with TMD patients. You will understand who can be treated simply with basic management and who should be referred. Case histories will be presented to illustrate these points.
It is important for the dentist to recognize that all TMD patients also require basic to complex dental treatment, aside from having their TMD issues managed. Many of these patients have occlusal changes from TMD, limited openings, and wear bitesplints. What is normally routine dental treatment can set off symptoms and alter the fit and adjustment of their splint. Many of these patients are taking medications for TMD that affect oral cavity (e.g. dry mouth). Awareness of these factors is essential for every dentist. The orofacial pain specialist can greatly assist in treatment of these patients. This article is not meant convey specific clinical skills, but rather to identify what TMD issues can be safely managed and what requires referral. It will also provide a framework for the interested dentist to further pursue continuing education to acquire hands-on knowledge.
Etiology of TMD
Before discussing diagnosis, it is important that we briefly discuss the etiology of TMD. TMDs are musculoskeletal orthopedic disorders of the TMJ joints and the muscles that move the joint. They are medical not dental conditions. Joints can get inflamed from excessive forces from injury (macrotrauma), or microtrauma (bruxism). Less often infection or autoimmune processes can affect the TMJs.
Muscles and tendons can also be inflamed or infected. Acute muscle pain can develop from overuse, trauma and infection.
A minority of TMD patients have chronic widespread muscle pain called myofascial pain dysfunction (MPD). The mechanism of this pain is poorly understood. It is evident that this is not a disorder of muscle overuse or hyperactivity, but is more related to other central nervous system disorders such as fibromyalgia. These patients are complex and extensive training is needed to manage these patients. Dentists should refer them to an orofacial pain dentist with advanced training who uses a team approach.
It needs to be made clear that many other factors can predispose a patient to TMD (Fig. 1).
Fig. 1

It also needs to be stressed that the common misconception that TMD is an “occlusal disease” is not evidenced based. 1,2 Much of the controversy and confusion about TMD revolves around this fallacious concept. There is no evidence that pre-existing occlusal conditions such as Angle classification, posterior interferences, “bite imbalance”, lack of anterior guidance, centric relation, bilateral crossbites in anyway cause TMD. 3 There is some weak evidence that large C.R-C.O slides, unilateral crossbites 4 are more prevalent in TMD patients.
There are however occlusal changes that can result from TMD, and certain factors that can predispose (but not in every instance), and perpetuate the disorder. A lack of posterior occlusal support overloading the joints when clenching may be one of these, however this remains to be proven. This lack of support can come from natural light contact of posterior teeth, lateral tongue thrust. It can also come from over equilibration, or leaving restorations (especially posterior implants) in “light occlusion”. These factors may be more a result of the TMD rather than a cause.
There is some evidence that patients with disc displacements with clicking joints also have a more posterior condylar position in the fossa. 4 Many dentists have postulated that this results from a deep anterior overbite and constriction of the envelope of function. This author also has a personal belief that this is possible, however there is no evidence to support this and further research is necessary.
It also important to realize that just as many patients with disc displacements have normal or anterior condylar positions. The practitioner should be cautioned to not determine diagnosis and management from imaging alone.
Diagnosis of TMD According to the Diagnostic Criteria for TMD (DC/TMD)
Unfortunately many dentists are unaware of the DC/TMD 5, even though they have been available since 1992. Dentists still misinform their patients that they have “TMJ” or a “bad bite” causing their problem.
These criteria have been carefully derived from 1000’s of TMD patients in both institutional and private practice settings. The criteria and the examiners have been subjected to careful statistical analysis from randomized clinical trials and prospective cohort studies, and are the accepted standard for diagnostic categories of TMD determined from subjective and objective examination protocols. Most TMDs are divided into three groups (Table 1):
Table 1

Patients with muscle pain without joint pain are rare. 6,7 Most patients with joint pain have related or referred muscle pain and spasm mediated through orthopedic laws.
Routine Examination for TMD According to the DC/TMD
Examination protocols for TMD can be rather complex, tedious and time consuming especially in more complex cases. For the basic cases that most dentists will choose to treat, a simple examination is presented here that is efficient, and will not be time consuming in most dental practices.
Rule #1 To keep things simple, always consider joint pathology first! Joint patients can be readily diagnosed and predictably treated by reducing load on the joints. This will be discussed later in the article.
Rule #2 Patients with chronic muscle pain and no apparent joint involvement are complex and present significant treatment challenges. They should be appropriately referred. In a later discussion, you will see that these patients are unmistakable and can be screened a straightforward manner (Fig. 2).
Fig. 2

Case Histories
The following case histories will be given for common TMD complaints that may present in your practice. The ones that should be referred will be indicated.
Case 1: New Painless Clicking and Popping
Subjective
A 16-year-old male has noticed increased clicking and popping in his right TMJ, increasing over the last six months. No pain or locking is reported. The patient reports he been chewing gum excessively.
Objective
No pain to palpation of joints or muscles. Opening is normal at 55 mm. (normal inter-incisal opening is 45-55 mm.) There is no wear on the teeth. No imaging necessary at this time. There are no occlusal factors. No MRI needed.
Diagnosis
Anterior disc displacement with reduction.
Treatment
Behavioral modification. Patient told to stop gum-chewing habit and not rest his head on his chin. There was no evidence of bruxism.
Discussion
Disc displacements are common, especially in the teen population. The etiology is still unknown. There have been many factors including joint laxity, change in viscosity of synovial fluid from inflammation, steepness of the articular eminence, lateral pterygoid hyperactivity, altered disc shape. 8
Unless the patient is symptomatic treatment is unnecessary. There is no need for referral. Reassurance from the dentist is all that is necessary.
- It is important especially for the orthodontist to screen all patients with clicking joints. It is essential that objective joint and muscle palpation for pain evaluation be done with initial records.
- If there is no pain or history of locking treatment may proceed. However if there is objective pain the patient should be advised and conservative splint therapy should be instituted until symptoms are controlled.
- In most cases this will avoid the patient already in orthodontic appliances from developing pain and a possible acute closed lock during treatment. If this happens consultation with an orofacial pain dentist to manage the patient would be advisable.
General Management Strategies for All TMD Patients with Joint Pain
- Reduce force to joint: soft diet, flat plane stabilization splint, behavioral modification (no gum chewing, strenuous impact exercise, no resting on the jaw, good posture)
- Anti-inflammatory medications
- Mild muscle relaxers to reduce spasm and aid sleep
- Physical therapy as needed: mobilization, massage, ultrasound, stretching etc.
All dentists should have these basic procedures in their armamentarium for TMD patients, and will be able to manage uncomplicated cases. It is not within the scope of this article to detail these. This is available in good evidenced based clinical courses.
Case 2: Joint Pain–Inflamed Joint
Subjective
A 42-year-old woman presents after having a blow to the left side of her chin causing pain in her right TMJ, referred ear and masseter pain. She reported limited opening, change in bite, and temporal headache, but no clicking or popping. She was already wearing a lower splint for bruxism but it was not helping.
Objective
There was severe pain to palpation of right TMJ and masseter muscle. There were no joint sounds. There was a midline shift of the occlusion to the left and a posterior open bite on the right side. Panorex was normal. MRI was not needed with this presentation. The patient’s lower splint was well made but had no contact on the right side.
Diagnosis
Acute TMJ capsulitis-synovitis with protective myospasm.
Treatment
Rest (soft diet), ice, ibuprofen 400 mg. TID for 10 days, and muscle relaxer prn (cyclobenzaprine 5 mg. QHS). Her present splint had lost contact on her right side die to the inflammatory occlusal changes present. If there is no sign of bruxism a splint is not necessary (Figs. 3-5).
Fig. 3
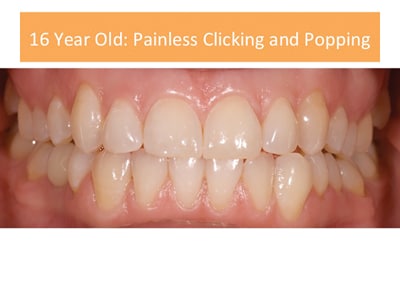
Fig. 4

A. Notice the midline shift and posterior open bite left side caused by inflammation and lateral pterygoid muscle spasm on the right (dashed lines).
B. Notice after 8 weeks of management the occlusal changes have resolved to normal.
Fig. 5

A. Retrodiscal tissue behind the joint is swollen with lateral pterygoid contraction bringing the condyle forward and downwards. This results in loss of posterior contact (molars) decreased overbite, and midline shift to the contralateral side.
B. After the inflammation has resolved (12 weeks) the determinants have returned to normal.
Discussion
This is a common occurrence of acute trauma occurring to the TMJ, and easily managed in every dental setting. There is no reason for referral of this patient.
The above protocol should be standard of care for inflammatory TMJ disorders.
The author wants to emphasize that the occlusal changes here were caused by TMD. There is a temporary constricted envelope of function caused by inflammation and ipsilateral lateral pterygoid spasm. Once the symptoms were reduced the occlusion returned to normal. There is no need for referral.
Case 3: Osteoarthritis Causing Sudden Bite Changes in An Elderly Patient
Subjective
An 82-year-old female presented with a chief complaint of pain in her left TMJ after biting on a hard food. She heard a loud “crunch” noticed that her bite had shifted and she has pain and difficulty chewing. The joint sounds remain.
Objective
The patient has severe pain to palpation of the left TMJ and masseter muscle. Her opening is 38 mm. There is rough crepitation in the left TMJ felt with both palpation and stethescopic auscultation. She has contact only on the left molars with an open bite. She has a midline shift to the left.
Imaging
CBCT shows severe flattening, atrophy, sclerosis of the left condyle.
Diagnosis
Advanced osteoarthritis left TMJ with collapse of cortical bone causing related bite changes.
Management
There is no difference in basic management as described with the previous patient in almost every case of joint inflammatory pain. Occlusal therapy after the patient is comfortable and the occlusion is stable to be managed conservatively with equilibration and restorative dentistry. The patient has to be informed that this bite change can reoccur. It would be prudent in this case allow for this with significant occlusal reduction on the preparations on the left so that there will be sufficient material for future equilibration. It might also be wise to cement the restorations provisionally to allow for laboratory adjustment (Figs. 6-8).
Fig. 6

The pictures denote the bite changes with contact only in the left posterior and midline shift. The white circle on the CBCT shows the flattened left condyle, ramus shortening and reduced joint space causing the shift. The right condyle retains its form.
Fig. 7

A. Lower bite splint to control symptoms and establish occlusal stability.
B. Bite splint adjusted to even bilateral contact.
C. Occlusal changes 3 months later showing joint instability.
Fig. 8

Patient was treatment planned for 5 crowns after condylar stability was established. Mounted models were taken and trial equilibration. After a wax up for the final restorations.
Discussion
This again is a patient that can be managed if the dentist realizes the TMD diagnosis.
This patient can be made comfortable with the same conservative treatment.
The etiology and pathogenesis of TMJ osteoarthritis is well established. 9 The difference here is that the bite changes are permanent and the patient has an unstable condylar position. It is necessary to establish condylar stability as best possible over at least one-year before proceeding with occlusal therapy. Even with this there is a possibility for further relapse. If this happens the only procedure to establish stability would be an alloplastic joint replacement. Most dentists can manage arthritic patients such as these. It would be helpful to refer to an orofacial pain dentist for initial diagnosis.
Case 4: Chronic Myofascial Pain Patient (Fig. 9)
Subjective
52-year-old woman, with the chief complaint of bilateral facial pain, dental pain, headache and neck pain for over 10 years. Her pain is located mainly in her posterior teeth with pain also in her cheeks and temples. The pain is severe more towards the end of her workday. She denies bruxism, has no pain to jaw function. She reports that her bite is “off ” and she cannot find a comfortable bite. All treatment to date has been ineffective including bite splints, occlusal equilibration, endodontics, extractions, botox. She has had orthodontics attempted twice but could not tolerate the appliances and they were removed. She was misdiagnosed with trigeminal neuralgia and failed medications from her neurologist. Her medical history is significant for IBS, fibromyalgia, depression. She is very anxious over her pain condition. The patient saw another dentist during treatment for a second opinion. He equilibrated her posterior teeth increasing her pain.
Fig. 9

A. Panorex (notice mostly posterior teeth involved)
B. Occlusion with Hawley bite plane in place
C. Hawley bite plane
Objective
The patient has a normal opening, no joint sounds, no joint pain to palpation. She has an Angle cl. I occlusion. Her teeth had been equilibrated numerous times, with loss of posterior contact. Palpation of the masseter muscles duplicates her chief complaint and refers pain to the molars. Palpation of the temporalis tendon is painful referring pain to the upper molars and anterior teeth. There was no TMJ pain to palpation during the initial examination.
Diagnosis
Chronic myofascial pain dysfunction.
The patient was counseled as to the nature and prognosis of her complaint. She was instructed that this was not a dental problem and that no further dental treatment should be done for her pain.
Injection of the masseter and temporalis muscle trigger points with Mepivicaine 3% eliminated all of the patient’s pain. She had benefit from this for over two weeks. A Hawley with an anterior bite plane was placed to reduce elevator muscle (masseter, temporalis and medial pterygoid) activity at night. This helped reduce 50% of the pain. The patient was counseled as to possible bite changes (anterior open bite) resulting from this appliance. The patient was given tricyclic medication (amitriptyline), muscle relaxer (baclofen), and low dose gabapentin. NSAIDS were of minimal help with her pain and she was told to take acetominophen as needed. She was referred to psychiatry for SSRI, cognitive behavioral therapy.
Discussion
This is a complex patient who should be referred to an orofacial pain dentist or clinic. The prognosis for this patient is guarded and this patient can be extremely time consuming and unproductive in a busy dental practice. Bite splints are often ineffective and may increase symptoms.
This type of patient will often respond with placebo to initial occlusal therapy and then have their pain return or be exacerbated. Occlusal therapy is contraindicated with this diagnosis. In this case the patient had excessive tooth structure removed from the posterior teeth creating the posterior open bite.
This patient has now been managed for over 10 years with still mild pain remaining.
Her splint has now been changed to an upper flat plane stabilization splint. She still has flares from time to time. When she had a posterior crown replaced two years ago her symptoms were exacerbated for six months.
Conclusions
TMD patients will inevitably appear in your practice. If you can diagnose this medical condition accurately there will be no indecision or confusion at how to manage them. It is important to realize that this is not a dental-occlusal disorder and occlusal therapy, whether equilibration, restorative dentistry, orthodontics, or orthognathic surgery is rarely indicated. Hopefully this author has provided knowledge that will assist in the reader acquiring basic skills in an evidenced based CE program. 10 This information is provided at the end of this article.
In Summation
- Diagnose accurately according to the DC/TMD.
- Minimal investment in instrumentation is necessary for basic diagnosis. Electronic equipment to diagnose occlusion, muscle activity, jaw tracking, joint sounds is unnecessary for most practitioners.
- CBCT is ideal imaging for initial diagnosis but panorex is acceptable. MRI may be needed for a minority of TMD patients.
- Refer patients with chronic muscle pain, headache, and psychological disorders especially is there is minimal joint pain to palpation.
- Most dentists should stick to basics: flat plane splint, anti-inflammatory medication, muscle relaxers, soft diet, physical therapy, home care
- No dental treatment (unless emergency) should be done until the patient has minimal pain, improved range of motion (opening), and stable occlusal markings on splint.
- In patients with unstable joints coordinate treatment with orofacial pain dentist to determine joint and occlusal stability.
- For hands-on training the American Academy of Orofacial Pain has resources for those interested in more training:
Oral Health welcomes this original article.
References
- Forssell H, Kalso E. Application of principles of evidence-based medicine to occlusal treatment of temporomandibular disorders: are there lessons to be learned? J Orofac Pain 2004;18:9-22.
- Gesch D, Bernhardt, Kirbshus A, Association of malocclusionand functional occlusion with temporomandibular disorders(TMD) in adults: a systematic review of population-basedstudies. Quintessence Int 2004;35:211-21
- Clark GT Sixty-eight years of experimental occlusal interference studies: What have we learned? (J Prosthet Dent 1999;82:704-13.)
- Pullinger AG et al Quantification and validation of predictive values of occlusal variables in temporomandibular disorders using a multifactorial analysis. JPD 2000;83(1):66-75
- Schiffman E, Ohrbach R, Truelove E et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: recommendations of the International RDC/TMD Consortium Network and Orofacial Pain Special Interest Group. J Orofac Pain Headache 2014;28:6-27.
- Raphael KG, Marbach JJ. Widespread pain and the effectiveness of oral splints in myofascial face pain. J Am Dent Assoc 2001;132:305–316.
- Manfredini D et al Age peaks of different RDC/TMD diagnoses in a patient population J. of Dentistry; January 38 (2010)392–399
- Manfredini D et al Etiopathogenesis of disk displacement of the temporomandibular joint: a review of the mechanisms Indian J Dent Res. 2009 Apr-Jun;20(2):212-21.
- Milam SB, Schmitz JP. Molecular biology of temporomandibular joint disorders. J Oral and Maxillofac Surg 1995;53:1448-54.
- Greene CS. Managing the care of patients with temporomandibular disorders: A new guideline for care. J Am Dent Assoc 2010;141;1086-1088.
About the Author
 Dr. Harold Menchel limits his practice to Orofacial pain in Coral Springs Florida. He is adjunct faculty in the Department of Prosthodontics at NOVA Southeastern School of Dental Medicine. His Orofacial Pain training was under Drs. Parker Mahan and Henry Gremillion at the University of Florida Facial Pain Center. He is an international speaker, educator, and has published articles in peer-reviewed journals including JADA. He reviews articles for JPD. Dr. Menchel is liaison to the American Medical Association for Orofacial pain coding and access to care. Dr. Menchel is a Diplomate of the American Board of Orofacial Pain.
Dr. Harold Menchel limits his practice to Orofacial pain in Coral Springs Florida. He is adjunct faculty in the Department of Prosthodontics at NOVA Southeastern School of Dental Medicine. His Orofacial Pain training was under Drs. Parker Mahan and Henry Gremillion at the University of Florida Facial Pain Center. He is an international speaker, educator, and has published articles in peer-reviewed journals including JADA. He reviews articles for JPD. Dr. Menchel is liaison to the American Medical Association for Orofacial pain coding and access to care. Dr. Menchel is a Diplomate of the American Board of Orofacial Pain.












