 This article is dedicated to Dr. Mervyn Gornitsky, a dear supervisor, mentor, and a friend who has served the dental community since 1953. I have had the pleasure of working with Dr. Gornitsky since 2015. Dr. Gornitsky served as JGH Chief of Dentistry from 1971 to 1998 and was given the title of Emeritus Chief of the department in 2002. His positive energy, contagious laugh and intellectual input will never be forgotten. Dr. Gornitsky always said, “The key is to stay interested, stay curious, and be open to new ideas; it’s what has made my many decades of work so fulfilling.” May his soul Rest In Peace.
This article is dedicated to Dr. Mervyn Gornitsky, a dear supervisor, mentor, and a friend who has served the dental community since 1953. I have had the pleasure of working with Dr. Gornitsky since 2015. Dr. Gornitsky served as JGH Chief of Dentistry from 1971 to 1998 and was given the title of Emeritus Chief of the department in 2002. His positive energy, contagious laugh and intellectual input will never be forgotten. Dr. Gornitsky always said, “The key is to stay interested, stay curious, and be open to new ideas; it’s what has made my many decades of work so fulfilling.” May his soul Rest In Peace.
Temporomandibular disorders (TMD) is a collective term used to describe musculoskeletal conditions characterized by pain in the muscles of mastication and temporomandibular joint or both, and/or associated structures.1 The common signs and symptoms include: tenderness in the muscles upon palpation, pain within the range of motion, or limitation of the jaw upon opening. This is followed by interference with vital functions such as eating, swallowing, and speaking.27
The prevalence of TMD-related pain ranges between 5% to 12%10,30 and the annual incidence is 3.9%.25 TMD-related pain is more common among females than males.30 Nevertheless, approximately 33% of TMD-related pain patients continue to suffer from moderate to severe levels of pain and disability, independent of treatment received.15,20 Many risks were identified to be associated with TMD-related pain. According to prospective studies, oral habits,12,14,16,28 psychological factors,3,6,28 and trauma9,11,23,28 are associated with TMDs risk. In addition, it has been suggested that pain (e.g., neck pain, back pain, headache, and fibromyalgia),13,18,29 and sleep comorbidities such as obstructive sleep apnea,17,24 fatigue,2,4,8 and insomnia17,26,31 are also associated with chronic TMD-related pain.
In many TMD-related pain patients, treatment options include the use of other interventions such as self-care, jaw exercises, physical therapy, and pharmacological treatments, which can improve the condition and preclude the need for an appliance.7 Splints, which are removable intraoral appliances are also considered as a treatment option for certain cases. They are provided to TMD-related pain patients to help ease pain in the mouth, face or jaws.
This short review will provide pertinent information about clinical considerations when selecting an intraoral appliance for TMD-related pain treatment. Existing evidence is of very low quality and did not demonstrate that splints reduced pain when compared with a minimal treatment (like jaw exercises, advice, or education) in patients with temporomandibular disorders.22 Certain patients may benefit more from appliance therapy than others. Thus, appliances can be considered as part of a broader rehabilitation treatment program to encourage healing, normal function, and restoration of normal activities.
There are many types of intraoral appliances. Four general types of intraoral appliances will be discussed: hard stabilization, anterior positioning, anterior bite planes, and posterior partial coverage.7
1. HARD STABILIZATION APPLIANCES
Fig. 1

These types of appliances are often called full coverage oral appliances since they typically cover all maxillary or mandibular teeth. In most studies, they have bilateral posterior tooth contacts, canine lateral guidance, and incisal anterior guidance. Other commonly used names for these appliances are splints, orthotic, bite guard, Michigan splint, and flat bite plane. There are no studies that suggest maxillary or mandibular appliances have efficacy over the other but rather depend on patient and clinician preference and comfort. The function of these appliances is to produce an orthopedically comfortable position for the jaw, reduce masticatory muscle activity and temporomandibular joint loading and increase awareness of oral parafunctional habits. Consequently,
this type of appliance intends to reduce temporomandibular joint disorders’ pain and dysfunction as well as prevent tooth wear and periodontal trauma. Soft resilient full coverage appliances may be less expensive than hard stabilization appliances but need to be adjusted similarly to hard appliances to allow comfort and efficacy.5,32 In most cases, these appliances need to be well adjusted to facilitate patient comfort, stability, and compliance. Patient compliance will most likely decrease if these appliances are too bulky, tight, or ill-fitting. Although the percentage of adverse events is not reported in the literature, patients should be monitored regularly for evidence of mucosal ulceration or inflammation, tooth pain, mouth odors, speech difficulties, dental caries, tooth mobility, and occlusal changes.
2. ANTERIOR POSITIONING APPLIANCES
Fig. 2

These appliances are intended to reposition the mandible and condyle anteriorly to improve the disc-condyle relationship and biomechanics of joint function. Common names for this type of appliance are mandibular orthopedic repositioning appliances, anterior positioning appliances, and disc-repositioning appliances. The primary indication for anterior positioning appliance therapy is TMJ disc displacement with reduction that is associated with painful clicking and/or intermittent locking. The appliance covers all teeth and provides occlusal indentations for the opposing posterior teeth. When the opposing teeth fully engage these occlusal guides, the condyle is held in a more anterior position during closing and opening movements, and the improved disc-condyle functional relationship results in a decrease in TMJ locking and noise with the associated joint or muscle symptoms. When this appliance is worn twenty-four hours per day for a prolonged period, it may cause a permanent anterior mandibular position and a posterior open bite. Thus, anterior positioning appliances are usually recommended to be worn part-time while sleeping. Anticipated open bite development should be discussed with the patient as part of the overall treatment plan. A referral to an orthodontist maybe warranted in case an open bite develops that the patient is unable to tolerate.
3. ANTERIOR BITE PLANES APPLIANCES
Fig. 3A

Fig. 3B

These are usually fabricated for the maxillary arch and adjusted to provide occlusal contacts with the mandibular anterior teeth and no posterior tooth contact. Common names for this type of appliance therapy are NTI splint, anterior bite splint, modified Hawley with an anterior bite plane, and anterior jig appliance. The NTI and anterior jig appliances differ from anterior bite planes appliances in that typically only the maxillary central incisors are covered, whereas the anterior bite plane usually covers all six maxillary anterior teeth with occlusal contacts with the six mandibular anterior teeth. The patient must be informed of potential adverse effects of full-time wear of partial coverage appliances as they may cause tooth movement, posterior open bite, and malocclusion.
4. POSTERIOR PARTIAL COVERAGE APPLIANCES
Fig. 4
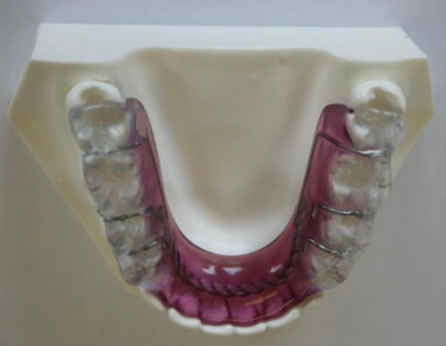
These have occlusal contact on the posterior teeth only and no contacts on the anterior teeth. Other variations of this appliance include the Gelb splint and pivotal, distraction, or localized occlusal interference splints. The posterior occlusal contacts are intended to change the biomechanics of the muscle and joints, as well as suppress muscle function and oral habits, thus decreasing pain due to repetitive strain. However, similar to anterior bite appliances, when partial coverage appliances are used full-time, adverse events such as tooth mobility, tooth movement, and an anterior open bite can occur.
SUMMARY AND CONCLUSIONS:
It has been suggested that the efficacy of intraoral appliance therapy may depend on appliance selection and patient selection. Some patients may benefit from appliance therapy more than others. For example, the results from Raphael and Marbach21 suggest that people with widespread pain are less likely to benefit from an appliance. A TMD-related pain patient reporting single comorbidity will be managed differently from a patient presenting with multiple comorbidities. The latter may require an interdisciplinary pain clinic setting that uses a team of clinicians to address different aspects of the problem in a concerted fashion. Failure to identify and to address the entire scope of the problem may lead to no improvement in pain or function, and further perpetuation of the problem. Patients with TMD-related pain presenting with multiple comorbid conditions such as fibromyalgia, neuropathic pain, migraine, depression, anxiety, bruxism, xerostomia, and other contributing factors can increase the risk for treatment failure.19 Single treatment strategies such as an appliance can also fail due to long-standing maladaptive behaviors, attitudes, and lifestyles that accompany a chronic condition. Patients with acute pain onset, limited treatment history, no comorbid conditions, and few behavioral and psychosocial contributing factors are easier to manage using single treatments. Patients with chronic pain presenting with comorbid conditions, persistent pain longer than 6 months, behavioral and psychosocial problems, frequent use of health-care services or medication, poor sleep, and work interference are more complex to manage and require a multi-disciplinary treatment approach with a number of healthcare professionals. Since these patients are more complex to treat, the clinician may require a team consisting of a physical therapist, psychologist, sleep physician, and dietitian, to improve the quality of life for the patient and to improve the likelihood of overall treatment success.
Oral Health welcomes this original article.
References
- ADA President’s Conference sets guidelines for examination, diagnosis and management of TM disorders. Journal (Canadian Dental Association) 1983;49(7):480-482.
- Aaron LA, Burke MM, Buchwald D. Overlapping conditions among patients with chronic fatigue syndrome, fibromyalgia, and temporomandibular disorder. Arch Intern Med 2000;160(2):221-227.
- Aggarwal VR, Macfarlane GJ, Farragher TM, McBeth J. Risk factors for onset of chronic oro-facial painresults of the North Cheshire orofacial pain prospective population study. Pain 2010;149(2):354-359.
- Chen H, Nackley A, Miller V, Diatchenko L, Maixner W. Multisystem dysregulation in painful temporomandibular disorders. J Pain 2013;14(9):983-996.
- Elsharkawy TM, Ali NM. Evaluation of acupuncture and occlusal splint therapy in the treatment of temporomandibular joint disorders. Egyptian dental journal 1995;41(3):1227-1232.
- Fillingim RB, Ohrbach R, Greenspan JD, Knott C, Diatchenko L, Dubner R, Bair E, Baraian C, Mack N, Slade GD, Maixner W. Psychological factors associated with development of TMD: the OPPERA prospective cohort study. J Pain 2013;14(12 Suppl):T75-90.
- Fricton J, Look JO, Wright E, Alencar FG, Jr., Chen H, Lang M, Ouyang W, Velly AM. Systematic review and meta-analysis of randomized controlled trials evaluating intraoral orthopedic appliances for temporomandibular disorders. J Orofac Pain 2010;24(3):237-254.
- Hoffmann RG, Kotchen JM, Kotchen TA, Cowley T, Dasgupta M, Cowley AW, Jr. Temporomandibular disorders and associated clinical comorbidities. Clin J Pain 2011;27(3):268-274.
- Huang GJ, Rue TC. Third-molar extraction as a risk factor for temporomandibular disorder. J Am Dent Assoc 2006;137(11):1547-1554.
- Isong U, Gansky SA, Plesh O. Temporomandibular joint and muscle disorder-type pain in U.S. adults: the National Health Interview Survey. J Orofac Pain 2008;22(4):317-322.
- Juhl GI, Jensen TS, Norholt SE, Svensson P. Incidence of symptoms and signs of TMD following third molar surgery: a controlled, prospective study. J Oral Rehabil 2009;36(3):199-209.
- Marpaung C, van Selms MKA, Lobbezoo F. Prevalence and risk indicators of pain-related temporomandibular disorders among Indonesian children and adolescents. Community Dent Oral Epidemiol 2018;46(4):400-406.
- Nilsson IM, List T, Drangsholt M. Headache and Co-morbid Pains Associated with TMD Pain in Adolescents. J Dent Res 2013.
- Ohrbach R, Bair E, Fillingim RB, Gonzalez Y, Gordon SM, Lim PF, Ribeiro-Dasilva M, Diatchenko L, Dubner R, Greenspan JD, Knott C, Maixner W, Smith SB, Slade GD. Clinical orofacial characteristics associated with risk of first-onset TMD: the OPPERA prospective cohort study. J Pain 2013;14(12 Suppl):T33-50.
- Ohrbach R, Dworkin SF. Five-year outcomes in TMD: relationship of changes in pain to changes in physical and psychological variables. Pain 1998;74(2-3):315-326.
- Ohrbach R, Fillingim RB, Mulkey F, Gonzalez Y, Gordon S, Gremillion H, Lim PF, Ribeiro-Dasilva M, Greenspan JD, Knott C, Maixner W, Slade G. Clinical findings and pain symptoms as potential risk factors for chronic TMD: descriptive data and empirically identified domains from the OPPERA case-control study. The journal of pain : official journal of the American Pain Society 2011;12(11 Suppl):T27-45.
- Olmos SR. Comorbidities of chronic facial pain and obstructive sleep apnea. Curr Opin Pulm Med 2016;22(6):570-575.
- Plesh O, Adams SH, Gansky SA. Temporomandibular joint and muscle disorder-type pain and comorbid pains in a national US sample. J Orofac Pain 2011;25(3):190-198.
- R dL. American Academy of Orofacial Pain Guidelines for Assessment, Diagnosis, and Management. Quintessence Publishing Co, Inc 2008(4th Ed).
- Rammelsberg P, LeResche L, Dworkin S, Mancl L. Longitudinal outcome of temporomandibular disorders: a 5-year epidemiologic study of muscle disorders defined by research diagnostic criteria for temporomandibular disorders. J Orofac Pain 2003;17(1):9-20.
- Raphael KG, Marbach JJ. Widespread pain and the effectiveness of oral splints in myofascial face pain. J Am Dent Assoc 2001;132(3): 305-316.
- Riley P, Glenny AM, Worthington HV, Jacobsen E, Robertson C, Durham J, Davies S, Petersen H, Boyers D. Oral splints for patients with temporomandibular disorders or bruxism: a systematic review and economic evaluation. Health Technol Assess 2020;24(7):1-224.
- Sale H, Bryndahl F, Isberg A. A 15-year follow-up of temporomandibular joint symptoms and magnetic resonance imaging findings in whiplash patients: a prospective, controlled study. Oral surgery, oral medicine, oral pathology and oral radiology 2014;117(4):522-532.
- 24. Sanders AE, Essick GK, Fillingim R, Knott C, Ohrbach R, Greenspan JD, Diatchenko L, Maixner W, Dubner R, Bair E, Miller VE, Slade GD. Sleep apnea symptoms and risk of temporomandibular disorder: OPPERA cohort. J Dent Res 2013;92 (7 Suppl):70s-77s.
- Slade GD, Bair E, Greenspan JD, Dubner R, Fillingim RB, Diatchenko L, Maixner W, Knott C, Ohrbach R. Signs and symptoms of first-onset TMD and sociodemographic predictors of its development: the OPPERA prospective cohort study. J Pain 2013;14(12 Suppl):T20-32. e21-23.
26. Smith MT, Wickwire EM, Grace EG, Edwards RR, Buenaver LF, Peterson S, Klick B, Haythornthwaite JA. Sleep disorders and their association with laboratory pain sensitivity in temporomandibular joint disorder. Sleep 2009;32(6):779-790. - Truelove EL, Sommers EE, LeResche L, Dworkin SF, Von Korff M. Clinical diagnostic criteria for TMD. New classification permits multiple diagnoses. J Am Dent Assoc 1992;123(4):47-54.
- Velly AM, Gornitsky M, Philippe P. Contributing factors to chronic myofascial pain: a case-control study. Pain 2003;104(3):491-499.
- Velly AM, List T, Lobbezoo F. Comorbid Pain and Psychological Conditions in Patients with Orofacial Pain. In: S B, editor. Orofacial Pain: Recent Advances in Assessment, Management, and Understanding of Mechanisms. Seattle IASP Press, 2014. pp. 53-74.
- Von Korff M, Dworkin SF, Le Resche L, Kruger A. An epidemiologic comparison of pain complaints. Pain 1988;32(2):173-183.
- Wickwire E, Bellinger K, Kronfli T, Grace E, Sarlani E, Wang K, Buenaver L, Smith M. (153) Relations between objective sleep data, sleep disorders, and signs and symptoms of temporomandibular joint disorder (TMD). The Journal of Pain The Journal of Pain 2008;9(4):14.
- Wright E, Anderson G, Schulte J. A randomized clinical trial of intraoral soft splints and palliative treatment for masticatory muscle pain. J Orofac Pain 1995;9(2): 192-199.
About the Author
 Dr. Sherif Elsaraj graduated from the University of Manitoba with a Doctor of Dental Medicine (DMD) in 2010. He holds a B.Sc. Honors in Biochemistry from Carleton University, an M.Sc. in Oral Biology from the University of Manitoba, and a Ph.D. in Craniofacial Pain and Health Sciences from McGill University. He completed a year of residency training at the Oral and Maxillofacial Radiology program at the University of Toronto. He is an active member of the Canadian Dental Association, Ontario Dental Association, Order des Dentists du Quebec and the Ottawa Dental Society. Dr. Elsaraj has limited his practice to seeing temporomandibular disorders, orofacial pain patients and obstructive sleep apnea management both in Ottawa and Montreal with the DOCS and JGH, respectively.
Dr. Sherif Elsaraj graduated from the University of Manitoba with a Doctor of Dental Medicine (DMD) in 2010. He holds a B.Sc. Honors in Biochemistry from Carleton University, an M.Sc. in Oral Biology from the University of Manitoba, and a Ph.D. in Craniofacial Pain and Health Sciences from McGill University. He completed a year of residency training at the Oral and Maxillofacial Radiology program at the University of Toronto. He is an active member of the Canadian Dental Association, Ontario Dental Association, Order des Dentists du Quebec and the Ottawa Dental Society. Dr. Elsaraj has limited his practice to seeing temporomandibular disorders, orofacial pain patients and obstructive sleep apnea management both in Ottawa and Montreal with the DOCS and JGH, respectively.












