Abstract
The patient treated in this report was not pleased with the appearance of his smile and his confidence to smile was affected. He desired ‘bigger’ and ‘whiter’ teeth. As with any elective cosmetic restorative procedure, a minimally-invasive approach providing the patient with a predictable, long-term result was indicated. The author utilized a combination of contemporary yet well-established, evidence-based techniques including a diagnostic wax up (Master Diagnostic Model MDM by Valley Dental Arts), analysis of preparation requirements for each individual tooth based on the desired outcome (as per MDM) and ultrathin bonded feldspathic Veneers to achieve the goals the patient desired.
Introduction
Contemporary cosmetic dentistry requires the dentist’s utmost consideration to maximize the preservation of healthy hard and soft oral tissues by applying minimally-invasive, evidence-based treatment techniques. Only by adhering to this core principle can the cosmetic dentist achieve predictable and long-term functioning restorations with high patient satisfaction and without compromising the immediate or long-term health of the tooth structure and gingival tissues. 1,2 Ultra-thin porcelain laminate veneers are in many cases elective restorations and are often placed in the absence of disease for purely esthetic reasons. A high degree of technical and scientific knowledge and skill is required by both the dentist and the laboratory technician and careful consideration of the available treatment options and techniques becomes critical to achieve the desired clinical outcome without compromising the patient’s health. 3,4 When it comes to bonded ceramic restorations it is well established that restorations bonded to intra-enamel tooth preparations demonstrate higher functional and esthetic survival rates. 5 Even a 0.5 mm chamfer commonly aimed for in traditional veneer preparations 6 will expose dentin in the gingival third of maxillary central incisor where the mean thickness of enamel is only 0.410mm. 7 Subgingival margin placement can lead to inflammation of the gingival tissues from the restorative procedures and materials. 3,8 Supra – or paragingival placement of a traditional margin can lead to a less than ideal esthetic result when dark tooth structure or a traditional margin are exposed even by naturally occurring recession in individuals with good oral hygiene. 9 Exposed margins can also be areas of increased plaque accumulation putting the patient at risk of developing gingival inflammation or secondary caries. 3,10 In this case report we describe the application of ultra-thin Veneers (0.1 mm-0.3 mm) that can be predictably placed and either completely or partially cover the facial surface of the involved teeth to create a beautiful smile. 11,12,13
Clinical Evaluation, Diagnosis and Treatment plan
Minimally invasive porcelain Veneers can be used to solve a variety of clinical situations. They are indicated any time a mostly additive approach is chosen to increase the volume of teeth by lengthening the incisal edge or adding facial bulk to teeth. Indications include diastema closures, increasing tooth size in undersized teeth or to expand the buccal corridor, restore tooth fractures as well as restoring canine guidance and the vertical dimension of occlusion.
In the case presented in this report the patient had undergone pre-restorative orthodontic treatment and maxillary orthognathic surgery with a mentoplasty to treat a class II malocclusion. After the treatment was completed, he was left with an adapted occlusion with heavily worn posterior teeth and an anterior open bite. He was unhappy with the appearance of his teeth and thought they were too small and dark (Figs. 1-4). He had been equilibrated and was asymptomatic at the time of the treatment and was seeking a minimally invasive treatment option to address his esthetic concerns without introducing any other changes to his occlusion at this point.
Fig. 1
Unretracted smile

Fig. 2
Retracted frontal view

Fig. 3
Retracted right lateral view

Fig. 4
Retracted left lateral view

Records including impressions for study models, clinical photographs and bite registrations were obtained and after review by the dentist and technician a Master Diagnostic Model (MDM) was fabricated by Valley Dental Arts laboratory (Stillwater, Minnesota, USA) involving 10 maxillary (#14 to #24) and 10 mandibular teeth (#34-#44) (Figs. 5-7).
Fig. 5
MDM frontal view

Fig. 6
MDM right lateral view

Fig. 7
MDM left lateral view

The goal for this model was to be able to establish realistic esthetic expectations with the patient and enable us to preview the treatment in the patient’s mouth by injecting a temporary restorative material in a mold created from this model. Functionally, the goal was to establish anterior coupling and canine guidance. Furthermore, the model was used to enable the analysis of the position of each individual tooth, before restoring it, in comparison to the desired post-restorative tooth dimension with the technician and identify areas where tooth preparation/modification is needed.
For some teeth this means they can be treated “prepless” and for others this approach facilitates a conservative, “prep less” tooth preparation only in areas where the natural shape of the tooth extends outside of the desired post-operative tooth dimension or an adequate path of insertion needs to be established. In some cases pre-restorative orthodontic alignment is indicated to facilitate maximum preservation of tooth structure.
Clinical and Laboratory Techniques
Tooth Preparation and Impression
After review of the MDM with the technician the selective tooth modifications were executed. In this case most of the teeth required no preparation and only some minor enamel recontouring was performed reducing some undercuts and particularly on #8 and #9 a slight intra-enamel facial reduction in the middle and incisal thirds of the labial surface of the teeth. Since we were going to increase the incisal length of the anterior teeth the incisal edge was flattened with polishing discs (Soflex, 3M) and all internal angles were rounded. This flat incisal was going to be utilized as a reference to verify correct and full seat of the Veneers during try in and bonding. No dentin was exposed and thus no temporary restorations were fabricated. In cases were temporary restorations are needed, they can be fabricated from chemical-cure bis-acryl resin using an impression of the MDM and a spot-etching bonding technique. An unretracted Vinyl Poly Siloxane (VPS) impression was taken to serve as a reference of the natural position of the gingiva for the technician. Retraction cord (Ultradent size #000 and Viscostat Clear) was then used for minimal gingival retraction. A second VPS impression was taken for the mastermodel and sent to the laboratory, along with a bite registration and pictures for shade matching, for the fabrication of the ultra-thin veneers.
Laboratory Techniques
In the laboratory the working models were fabricated from type IV dental stone and mounted in an articulator utilizing the provided bite registration (Figs. 8-12). The master model was left as a solid, uncut model to leave the soft tissues intact and was duplicated to fabricate a refractory model. On the refractory model the soft tissues were slightly trimmed to ensure full coverage of the teeth and develop a proper emergence profile. Silicone guides made from the diagnostic wax-up were used to verify that there was enough space for the ceramic restorations. Vita VM13 (A1 and Bleach shades) feldspathic porcelain was hand-stacked to create restorations that were 0.1mm – 0.3 mm in thickness. The Veneers were carefully divested and were then fit on the mastermodel and a sectioned, trimmed model (Fig. 13). In a final step they were etched with hydrofluoric acid and sent back for insertion.
Fig. 8
Frontal view of prepared teeth with retracted gingiva

Fig. 9
Right lateral view of prepared teeth with retracted gingiva

Fig. 10
Left lateral view of prepared teeth with retracted gingiva

Fig. 11
Occlusal view of prepared maxillary teeth

Fig. 12
Occlusal view of prepared mandibular teeth

Fig. 13
Mandibular sectioned model and utra-thin Veneers

Bonding Protocol for Porcelain Restorations
On the day of insertion the patient’s gingival tissues were retracted using a size #000 Ultradent braided cord again in combination with Viscostat Clear. The Veneers were carefully tried in to verify the fit and path of insertion for each individual restoration. The teeth were then cleaned with pumice and then one to two restorations were bonded at a time using the following protocol. The intaglio surfaces of the veneers were cleaned by scrubbing them with 35% phosphoric etchant and then treated with silane (Ultradent) for 60 seconds. In the meantime the teeth were etched with 35% phosphoric etchant. Then the adhesive of a two bottle system bonding agent (Kerr Optibond FL) was applied to the enamel and the veneer and the veneer was inserted using a nano-filled flowable composite (3M Filtek supreme flow B1). The Veneers were tag cured using a 3 mm wide light guide on 3M Elipar light and excess in the margin area was removed with a brush prior to fully curing the bonded restorations. Excess was then further removed with a #12 scalpel blade interproximately and along the facial aspect of the tooth and the lingual areas were cleaned and polished with rubber polishing cups (Enhance and PoGo by Dentsply). Additional interproximate polishing was performed with ultra-fine metal finishing strips (Brassler/USA). This process was repeated for all the restorations and in a final step the static and functional occlusal contacts were verified.
The patient was very happy with the result and has had no problems. He is wearing a flat plane splint at night time and has been asymptomatic. Figure 14 shows the result 12 months post-insertion.
Fig. 14
Unretracted post-operative smile*

Fig. 15
Retracted post-operative frontal view

Fig. 16
Retracted post-operative right lateral view

Fig. 17
Retracted post-operative left lateral view
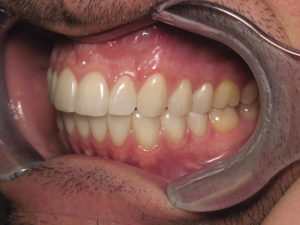
Fig. 18
Post-operative occlusal view of the maxillary arch

Fig. 19
Post-operative occlusal view of the mandibular arch

*(Porcelain Veneers by Jenny Wohlberg, AAACD, Valley Dental Arts, Stillwater, MN, USA)
Conclusion
Maximizing the preservation of enamel, especially in the gingival, is the primary key to long-term success when bonding porcelain veneers. Thus, ultra-thin veneers in combination with enamel recontouring, rather than conventional substractive preparation methods were dentin is unnecessarily exposed, should be the primary choice of today’s clinician. The recontouring should stay within the enamel layer, particularly in the gingival third, and should only be performed to establish a path of insertion or to create definitive incisal finish lines that help to facilitate proper seating of the restoration. Only in cases of subgingival margins should a gingival finish line be created. Close collaboration between the dentist and the laboratory technician is required to achieve maximum success. Detailed tooth-by-tooth analysis combined with the application of contemporary laboratory and bonding techniques make maximum preservation of tooth structure a possibility. Therefore, additive restorative techniques like the one described in this report should be the main choice for esthetic rehabilitations with bonded porcelain restorations.
References
1. Puri K, Puri N, Dodwad V, Masamatti SS. Restorative aspects of periodontal disease: an update part 1. Dent Update. 2014 Jul-Aug;41(6):545-8, 551-2.
2. Reeves J. Periodontal health–challenges in restorative dentistry. Prim Dent J. 2014 May;3(2):73-6.
3. Burnett RR, Diaz R, Waldrop TC, Hallmon WW. Clinical perspectives of periodontal and restorative interactions. Compendium. 1994 May;15(5):644, 646, 648-55.
4. Strassler HE. Minimally invasive porcelain Veneers: Indications ofr a conservative esthetic dentistry treatment modality. Gen Dent 2007; 55:686-694
5. Gurel G, Sesma N, Calamita MA, Coachman C, Morimoto S. Influence of enamel preservation on failure rates of porcelain laminate Veneers. Int J Periodontics Restorative Den 2013; 33:31-39.
6. Magne P, Belser U. Bonded Porcealin Restorations in the Anterior Dentition: A Biomimetic Approach: Quintessence Publisher Co, Inc: 2002.
7. Pahlevan A, MirazeeM, Yassine E, et al. Enamel thickness after preparation of tooth for porcelain laminate. J Dent 2014; 11:428-432.
8. Ferencz JL. Maintaining and enhancing gingival architecture in fixed prosthodontics. J Prosthet Dent 1991; 65:650-657.
9. Serino G, Wennstroem JL, Lidhe J, Eneroth L. The prevelance and distributon of gingival recession in subjects with a high standard of oral hygiene. J Clin Periodontol 1994; 21:57-63.
10. Silness J. Fixed prosthodontic and peridontal health. Dent Clin North Am 1980; 24:317-329.
11. Materdomini D, Friedman MJ. The contact lens effect: Enhancing porcelain veneer estetics. J Esthet Dent 1995; 7:99-103.
12. Horvath S, Schulz CP. Minimally invasive restoration of a maxiallary central incisor with a partial Veneer. Eur J Estetic dent 2012; 7:6-16.
13. Friedman M. Multiple potential of etched porcelain laminate veneers. J Am Dent Assoc 1987; 115:83E-87E.
About the Author
Dr. med.dent. Holger P. Meiser graduated from the Ruprecht-Karls University School of Dentistry in Heidelberg/Germany in 2002. He went on to complete residencies and fellowships in Advanced General Dentistry and Implant Dentistry at the University of Minnesota Dental School where he also earned a certificate in Contemporary Restorative and Esthetic Dentistry. He has fulfilled the requirements to achieve Mastership in the Academy of General Dentistry and Associate Fellowship in the American Academy of Implant Dentistry. Dr. Meiser is a member of the American Society for Dental Asthetics. He maintains a private practice in Minnetonka, MN, USA and serves as adjunct faculty in the Implant Program at the University of Minnesota and as an advisor to the Pankey Institute in Key Biscayne, FL, USA.
RELATED ARTICLE: The Beauty – And Logic – Of Minimal-Prep Veneers









